All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
MRD1
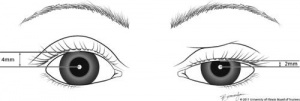
Margin reflex distance 1 or MRD1 is determined by the examiner and patient aligning at the same level. A light is directed at the patient’s eyes and the patient is directed to look at the light. The MRD1 is the measurement in millimeters from the light reflex on the patient’s cornea to the upperbeyelid margin, with the patient gazing in the primary position. MRD1 is used to indicate degree of ptosis or retraction. See below image.
MRD2
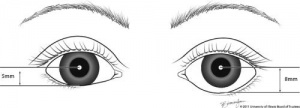
Margin reflex distance 2 or MRD2 measures from the corneal light reflex to the lower eyelid margin, with the patient’s eyes in the primary gaze.
MRD2 is useful for calculations involving reverse ptosis (such as seen in Horner syndrome), or lower eyelid retraction.
Amount of unilateral retraction: MRD2 normal – MRD2 abnormal eyelid
Amount of bilateral retraction: 5.5 – MRD2 either eyelid.
Palpebral fissure = MRD1 plus MRD2 [1]
MRD3
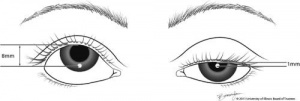
Margin reflex distance 3 or MRD3 is an entity described by Putterman, which is the distance from the ocular, not corneal, light reflex to the central upper-eyelid margin when the patient looks in extreme up gaze.[1] MRD3 is used to determine how much levator to resect in patients with congenital ptosis, who have a vertical strabismus associated with ptosis and in whom strabismus surgery is not indicated. MRD3 is less frequently used when compared to MRD 1 or 2.
In unilateral blepharoptosis: (Normal - Abnormal MRD3)*3= gives a value that determines the approximate amount of levator muscle resection.[1] In bilateral blepharoptosis: [Normal MRD3 (7mm) - MRD3 abnormal]*3 = approximate number of millimeters of levator muscle to resect in congenital ptosis.[1]
MLD
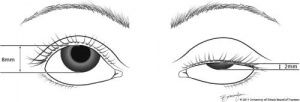
Margin limbal distance or MLD is used by some surgeons to measure levator function to determine the amount of levator muscle to resect. The MLD is the distance from the inferior limbus to the central upper-eyelid margin when the patient looks in extreme up gaze. In unilateral blepharoptosis, the difference in the MLD between the normal side and the abnormal side indicates the difference in levator function. In bilateral blepharoptosis, the examiner’s finger elevates the upper eyelid of the eye not being measured to prevent frontalis muscle action and to allow the patient to see the light.
If there is vertical strabismus associated with blepharoptosis (i.e. double elevator palsy), it has been determined that the MLD is not valid because the 6-o’clock limbal level in up gaze is abnormal given vertical restriction.[2][3][4]
References
- ↑ 1.0 1.1 1.2 1.3 Putterman AM. Margin reflex distance (MRD) 1, 2, and 3. Ophthal Plast Reconstr Surg. 2012;28(4):308-11.
- ↑ Callahan MA. Surgically mismanaged ptosis associated with double elevator palsy. Arch Ophthalmol. 1981;99(1):108-12.
- ↑ Struck MC, Larson JC. Surgery for Supranuclear Monocular Elevation Deficiency. Strabismus. 2015;23(4):176-81.
- ↑ Yurdakul NS, Ugurlu S, Maden A. Surgical treatment in patients with double elevator palsy. Eur J Ophthalmol. 2009;19(5):697-701.