Anterior Segment Optical Coherence Tomography
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Technology
Optical coherence tomography (OCT) is a high resolution cross-sectional imaging modality initially developed for retinal imaging. Anterior segment OCT (ASOCT) imaging was first described in 1994 by Izatt et al [1] using the same wavelength of light as retinal OCT, namely 830nm. This wavelength is suboptimal for imaging the angle due to limited penetration through scattering tissue such as the sclera. OCT imaging of the anterior segment with a longer wavelength of 1310nm was developed later on and had the advantages of better penetration through sclera as well as real-time imaging at 8 frames per second [2]. Currently, there are two commercially produced dedicated anterior segment devices, the SL-OCT (Heidelberg Engineering) and the Visante (Carl Zeiss Meditec, Inc.), of which only the latter is available in the United States. With the development of fourier domain OCT (FDOCT) technology, real-time imaging of the posterior segment has also become feasible. Several retinal FDOCT devices allow imaging of the anterior segment, however they still use the shorter wavelength of 830-870nm with its inherent disadvantages in imaging the AC angle. The higher resolution provided by FD retinal OCT devices does have advantages in imaging other structures in the anterior segment such as the cornea and conjunctiva. Fourier domain OCT devices operating at the longer wavelength suited for AC angle imaging have also been described [3][4], but these are not yet commercially available in the United States.
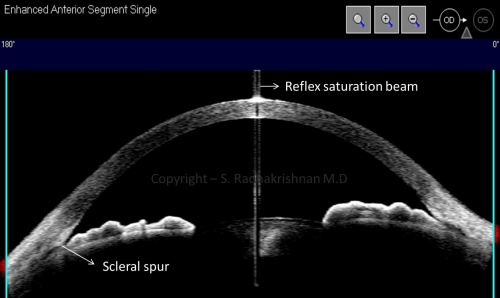
The Visante OCT has several scanning protocols of which the Enhanced Anterior Segment Single Scan and the High Resolution Raw scan are most useful for angle assessment. Figure 1 is an example of a good-quality Enhanced Anterior Segment Scan. The important features include good horizontal and vertical centration of the image within the frame, the presence of a reflex saturation beam indicating perpendicularity of the eye to the scanning beam and minimal tilting of the image. The scan dimensions are 16 x 6 mm and 4 image frames are averaged in order to increase the signal to noise ratio. In this scan protocol, the image is automatically corrected for the effects of refraction of the scanning beam. The High Resolution Raw Scan samples 512 A scans/image (as opposed to 256 A scans/image for the Enhanced scan), there is no image averaging or refraction correction.
Qualitative assessment
An important landmark to identify when interpreting ASOCT images is the scleral spur. This is visible as an inward projection of the sclera (see Figure 1) at the junction between the inner scleral and corneal curvatures. Apposition between the iris and the inner corneo-scleral wall has been used in several studies [5][6] as a qualitative method of detecting angle closure, however it must be noted that the degree of apposition may be variable and does not correlate exactly with appositional closure as defined by gonioscopy. In addition, several studies have shown that the when using the Anterior Segment Scan protocol which does not utilize image averaging, the scleral spur is not visible in about 25% of cases [7] – in this situation, it is still possible to qualitatively assess irido-corneal apposition in most images.
Quantitative assessment
Quantitative measurement of the AC angle is possible with in-built software in most of the anterior segment devices and also requires identification of the scleral spur. Several parameters have been described [8] and studies have shown good reproducibility [9][10]. Limitations in visibility of scleral spur and the wide natural variation in angle anatomy within the same eye as well as between eyes are limiting factors in the routine use of quantitative measurement for angle assessment.
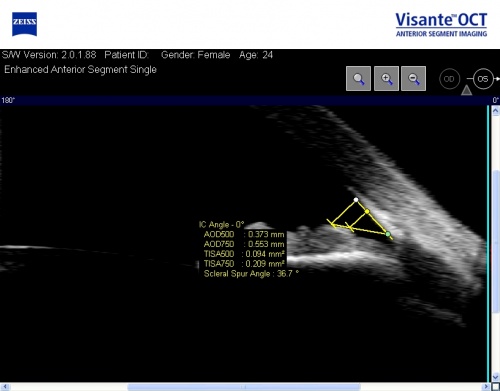
The commonly used quantitative parameters are as follows (Figure 3):
- Angle opening distance (in mm): Perpendicular distance between a point 500µm (AOD 500) or 750 µm (AOD750) anterior to the scleral spur and the opposing iris.
- Angle recess area (in mm2): The triangular area (ARA 500 or 750) bounded by the AOD 500 or 750, the anterior iris surface and the inner corneo-scleral wall
- Trabecular space area (in mm2): Trapezoidal area (TISA 500 or 750) bounded by the AOD 500 or 750, the anterior iris surface, the inner corneo-scleral wall and the perpendicular distance between the scleral spur and the opposing iris.
Several other quantitative parameters such as iris thickness [11], anterior chamber width [12] and lens vault [13] have also been described.
ASOCT versus UBM
Besides ASOCT, ultrasound biomicroscopy (UBM) may also be used for cross-sectional imaging of the anterior segment and the AC angle. When compared to ASOCT, UBM has the unique advantage of enabling visualization of structures posterior to the iris such as the ciliary body, zonules and the peripheral lens. However UBM is relatively more uncomfortable, requires a highly skilled operator in order to obtain good quality images and has a limited scan width (5 x 5 mm with the traditional UBM devices).
| ASOCT | UBM | |
|---|---|---|
| Technology | Optical | Ultrasound |
| Resolution | 15 µm | 50µm |
| Longest scan dimensions | 16 x 6 mm | 5 x 5 mm |
| Contact with eye | No | Ultrasound probe does not contact the eye directly but requires immersion bath |
| Real-time imaging | Yes | Yes |
| Imaging posterior to iris | No | Yes |
| Quantitative measurement | Yes | Yes |
Clinical use in glaucoma
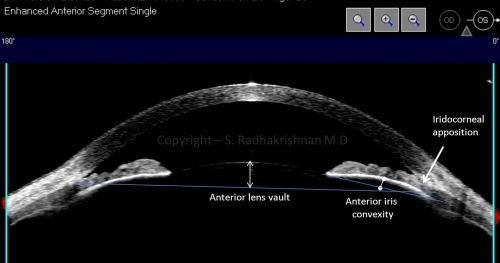
In clinical glaucoma practice, ASOCT is useful as an adjunct to gonioscopy as well as a substitute when gonioscopy is not feasible due to corneal pathology or lack of patient co-operation. In addition, it is extremely useful as a patient education tool, especially when laser peripheral iridotomy is being recommended. When compared to gonioscopy, OCT has the advantages of being non-contact and can be performed under dark conditions allowing angle assessment during physiological mydriasis. Based on the iris profile and position of the lens with respect to anterior segment structures, mechanisms of angle closure such as pupillary block and anterior lens vault can be discerned (Figure 2). It is important to note that structures behind the iris cannot be visualized with OCT, hence diagnosis of posterior mechanisms of angle closure such as iridociliary lesions and plateau iris must be confirmed with ultrasound biomicroscopy. ASOCT is also more useful than UBM for serial monitoring of the angle since approximate alignment with ocular landmarks (such as iridotomies, iris nevi, conjunctival blood vessels etc.) can be performed with ASOCT by utilizing the video image during OCT scan acquisition. It is important to keep in mind that not all scan types are corrected for errors due to refraction of the OCT scanning beam and comparisons must only be made between similar scan types. OCT may also be used to visualize trabeculectomy blebs and anterior segment implants such as drainage devices and keratoprosthesis – however, the clinical value in these situations appears to be limited.
Future directions
Fourier domain anterior segment OCT devices operating at 1310nm wavelength have been developed and these allow rapid 3-dimensional cube scanning of the anterior segment. Due to the large volume of data captured, 360 degree assessment of the anterior chamber angle and measurement of parameters such as iris volume and anterior chamber volume may be possible with these devices.
Angle assessment with ASOCT has thus far been mainly focused on measurement of static factors such as the AC angle width. Recently there has been increasing interest in assessing dynamic factors such as change in iris area or volume [14][15] that may identify eyes that are at a risk of acute primary angle closure.
Additional Resources
References
- ↑ Izatt JA, Hee MR, Swanson EA, et al. Micrometer-scale resolution imaging of the anterior eye in vivo with optical coherence tomography. Arch Ophthalmol. 1994;112:1584–1589
- ↑ Radhakrishnan S, Rollins AM, Roth JE, et al. Real-time optical coherence tomography of the anterior segment at 1310 nm. Arch Ophthalmol 2001;119:1179–85.
- ↑ Asrani S, Sarunic M, Santiago C, et al. Detailed visualization of the anterior segment using fourier domain optical coherence tomography. Arch Ophthalmol 2008;126:765-71.
- ↑ Fukuda S, Kawana K, Yasuno Y, et al. Repeatability and reproducibility of anterior ocular biometric measurements with 2-D and 3-D optical coherence tomography. J Cataract Refract Surg 2010;36:1867-73.
- ↑ Nolan WP, See JL, Chew PT, et al. Detection of primary angle closure using anterior segment OCT in Asian eyes. Ophthalmology 2007;114:33-9.
- ↑ Lavanya R, Foster PJ, Sakata LM, et al. Screening for narrow angle s in the Singapore population: evaluation of new non-contact screening methods. Ophthalmology 2008;115:1720-7
- ↑ Sakata LM, Lavanya R, Friedman DS, et al. Assessment of the scleral spur in anterior segment optical coherence tomography images. Arch Ophthalmol 2008;126:181-5.
- ↑ Radhakrishnan S, Goldsmith J, Westphal V, et al. Comparison of coherence tomography and ultrasound biomicroscopy for detection of narrow anterior chamber angles. Arch Ophthalmol. 2005;128:1053–1059.
- ↑ Fukuda S, Kawana K, Yasuno Y, et al. Repeatability and reproducibility of anterior ocular biometric measurements with 2-D and 3-D optical coherence tomography. J Cataract Refract Surg 2010;36:1867-73.
- ↑ Tan AN, Sauren LD, de Brabander J, et al. Reproducibility of anterior chamber angle measurements with anterior segment OCT. Invest Ophthalmol Vis Sci 2011;52:2095-9.
- ↑ Wang B, Sakata LM, Friedman DS et al. Quantitative iris parameters and association with narrow angles. Ophthalmology 2010;117:11-7.
- ↑ Nongpiur ME, Sakata LM, Friedman DS et al.Novel association of smaller anterior chamber width with angle closure in Singaporeans. Ophthalmology 2010;117:1967-73.
- ↑ Tan GS, He M, Zhao, W et al. Determinants of lens vault and association with narrow angles in patients from Singapore. Am J Ophthalmol 2012;154:39-46.
- ↑ Quigley HA, Silver DM, Friedman DS et al. Iris cross-sectional area decreases with pupil dilation and its dynamic behavior is a risk factor in angle closure. J Glaucoma 2009;18:173-9.
- ↑ Aptel F, Denis P. Optical coherence tomography quantitative analysis of iris volume changes after pharmacological mydriasis. Ophthalmology 2010;117:3-10.