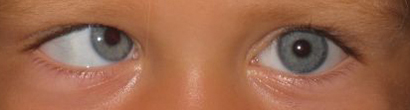
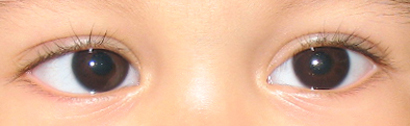
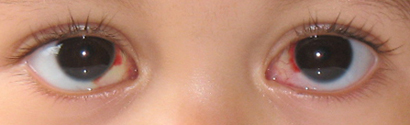
Infantile Esotropia
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Strabismus/Eye misalignment
Disease
Esotropia is a form of ocular motility disorder in which there is an inward turning of one or both eyes, commonly referred to as "crossed eyes".[1] By definition, infantile esotropia onsets during the first 6 months of life. The term "congenital esotropia" has been used synonymously but the condition is rarely present at birth. The deviation is typically constant, comitant, and large (≥30 PD). It may be accompanied by dissociated vertical deviation (DVD) (50%-90%), overelevation in adduction (70%), fusion maldevelopment nystagmus syndrome (latent nystagmus) (40%), and optokinetic asymmetry. These associated findings may develop over time, usually after 1-2 years of age.
Ocular instability of infancy describes transient misalignment of the eyes that is common up to the age of 3 months, and possibly longer in premature infants; this should not be confused with infantile esotropia. A constant esotropia of ≥40 PD after 10 weeks of age is unlikely to resolve spontaneously.[2]
Etiology
The etiology of infantile esotropia is unknown. Many theories have been postulated regarding the pathogenesis of the disease. The Worth[3] theory suggests that there is an irreparable congenital defect in the infant's visual system and that surgery can be carried out at leisure mostly for cosmetic purposes. On the other hand, Chavasse[4] suggested a primary motor dysfunction, where the associated poor fusion and lack of high-grade stereopsis is probably a sensory adaptation to abnormal visual stimulation during early binocular development caused by the motor misalignment. Thus, surgical correction should be performed early during infancy. This second view was largely accepted afterwards by Costenbader and Parks and is the basis for early procedural intervention. David Guyton found on scleral search coil recordings of patients with dissociated vertical deviation that these patients have a convergence damping of the horizontal component of fusion maldevelopment nystagmus with chronic convergence that he proposed leads to shortening of the medial rectus over time. [5] Michael Brodsky has proposed that infantile esotropia is caused by disruption of the development of binocularity in the striate cortex, leading to immature subcortical motor pathways to decompensate nasalward in the direction of innate or convergent biases.[6][7]
There can be a hereditary component with other family members having a history of strabismus. Infantile esotropia is more common in children with a history of prematurity, developmental delay, cerebral palsy, and hydrocephalus.
Diagnosis
History
Detailed history taking regarding gestational age at birth, birth weight, complications of birth, the health of the child and developmental milestones may help in the management of the case. A history of first presentation aided by photographs of the child in the first few months of life can assist in documenting the onset, detecting the stability of the condition and confirming the diagnosis. Family history may elicit the presence of a genetic factor/ familial inheritance.
Physical Examination
Appropriate diagnosis and management require a full ophthalmologic evaluation with cycloplegia and dilation to examine for other causes of esotropia in young children, including media opacities, refractive error, cranial nerve palsy, etc.
Detailed examination of motility and alignment is needed and can be challenging in young children. The exam should be quick and performed in a fun atmosphere. Try to engage the child’s attention with the use of colorful toys, whistling and making noises.
Visual acuity
Amblyopia occurs in approximately 40% - 50% of children with congenital esotropia.[8] This can be determined by observing the child for a fixation preference for one eye. Detection of fixation preference for one eye can be performed by the use of vertical prism test[9]. Many infants may freely alternate their fixation. Others may cross fixate using alternate eyes in the opposite field of gaze, (i.e. looking to the left with the right eye and looking to the right with the left) and do not develop amblyopia. Optokinetic response to detect smooth pursuit and saccade eye movements can aid in the diagnosis of amblyopia in young children.
Understanding visual milestones and anatomic development is needed for visual assessment of the child. On average, by 2 months of age, the optic nerve completes myelination. At 3 to 4 months, the fovea develops, and by 6 months iris pigmentation is approximately 90% complete. Methods to evaluate vision in infants include observing fixation and following visual behaviors, Visual evoked potential (VEP) testing, optokinetic response, preferential looking and optotype visual acuity depending on the child’s age and level of cooperation.[10]
Refractive errors
A cycloplegic refraction should be performed. Correction of hyperopia of ≥+2.00 D should be tried to evaluate for a possible accommodative component to the esotropia.
Sensorimotor
The deviation in infantile esotropia is typically constant, comitant, and ≥30 PD. Corneal light reflex tests (Hirschberg and Krimsky) can be helpful for estimating the angle of deviation but cover testing should be used when possible.
Horizontal ductions are typically full, but full abduction may be difficult to elicit due to cross-fixation (using the left eye to look toward the right and vice versa). Methods to assess abduction include: 1) patching or covering the opposite eye during evaluation of ductions 2) use of the doll’s head maneuver, 3) spinning the child. In the doll’s head maneuver, the child is given an interesting fixation target to look at and the head it gently rotated away from the target. Spinning stimulates a vestibular movement to the opposite direction of the spin and a refixation saccade in the same direction. The child can be gently spun on an office stool in a parent’s lap away from a fixation target to elicit abduction. Long-standing esotropia may lead to a small abduction deficit from restriction; however, CN VI palsy should still be ruled out.
Infants up to age 6 months are expected to have superior development of smooth pursuits in the temporal-to nasal direction compared to the nasal-to temporal direction. This asymmetry may persist in patients with infantile esotropia.
Associated conditions
Associated overelevation in adduction/ inferior oblique overaction occurs in around 70% of cases
Dissociated vertical deviation (DVD) occurs in 50-90% of cases. DVD is elevation of the non-fixing eye when covered or with visual inattention.
Fusion maldevelopment nystagmus syndrome (latent nystagmus) occurs in 40% of infantile esotropia cases. It is a predominantly horizontal jerk nystagmus elicited by occluding either eye. The fast phase is toward the uncovered eye.[11]
These associated findings typically do not manifest until after age 1 year.
Differential diagnosis
- Pseudoesotropia
- Sensory esotropia
- Congenital sixth nerve palsy
- Nystagmus blockage syndrome
- Type I Duane’s syndrome
- Ciancia syndrome
- Congenital fibrosis syndrome
- Mobius syndrome
- Infantile Myasthenia Gravis
- Esotropia associated with neurologic diseases e.g. cerebral palsy, periventricular luekomalacia
Management
Evaluation for an underlying disease process should be made when symptoms and signs lead in that direction. Most cases of infantile esotropia will require procedural intervention.[12] Children with esotropia that presents after 6-9 months of age and those who show limited abduction may require imaging.
General treatment
Associated amblyopia therapy
The timing of amblyopia treatment in relation to eye muscle realignment surgery is debatable. Some surgeons treat amblyopia before performing surgery to create a stronger visual drive to maintain alignment. However, it has been found that those with mild to moderate amblyopia are as likely to maintain alignment as those who had amblyopia treated prior to surgery. Surgical realignment may improve amblyopia in some cases.[13] Surgery does not need to be deferred until amblyopia is fully treated.
Surgery
Some studies have shown early strabismus surgery provides more potential for development of binocular function.[14] [15]In North America, surgery is frequently performed before age 2 years, with some reports finding improved fusion and stereopsis with very early surgery even before 6 months [16]. Strabismus surgery is more technically challenging earlier in infancy because of the small size of an infant’s eye and orbit, in addition to the lack of stability of the deviation and difficulties in measuring the alignment.[12] Parents should be aware that the goal of treatment is to get the eyes aligned and encourage the best sensory development possible, which might take more than one surgical procedure. The standard approach for treatment is bilateral medial rectus recessions which weaken the medial recti (the muscles pulling the eyes inward). Alternatively, a medial rectus recession with an ipsilateral lateral rectus resection can achieve the same effect and may be preferred if the visual acuity is unequal.
If overelevation in adduction is noted, surgical weakening of the inferior oblique muscles can be performed simultaneously. The other associated conditions of DVD and fusion maldevelopment nystagmus usually appear later in life and may be addressed surgically at that point.
Surgical follow up
After surgical realignment, patients are usually advised to return within a few weeks following surgery to assess eye alignment and the ocular healing process. Intraocular infection is rare following strabismus surgery. Patients should be followed closely for amblyopia, even if they achieve good motor alignment. Patient should continue to be monitored for recurrent strabismus and development of amblyopia.[17][18]
Complications
Undercorrection (persistent crossing) and overcorrection (wandering of an eye) are the most commonly noted complications of surgery. Many of these are transient. Other less common complications include perforation of the sclera, lost or slipped muscles, infection, anterior segment ischemia, postoperative diplopia, conjunctival granulomas and cysts.
Botulinum Toxin
Botulinum toxin can be injected into the medial recti to weaken them and bring eyes back into alignment. While the action of Botulinum toxin is limited to around 2-3 months, allowing for binocular fusion can lead to long-term improvement in alignment, although reports of the longevity of improved alignment are variable[19][20][21][22][23]. Patients may require multiple injections. Botulinum may be more effective in infantile esotropia when the angle of deviation is <30-35 PD.[23][24][25]
Prognosis
Untreated, children with infantile esotropia can develop good vision in each eye, but bifoveal fixation with full binocular function will not be achieved. Therefore, they will have poor depth perception and atypical appearance. Amblyopia can reduce visual acuity. When infants undergo early surgical intervention, they have a chance of better alignment and stereopsis outcomes. Multiple surgeries may be needed to correct large angle esotropia. The number of children requiring a second operation is between 15-30%.[17] Alignment within 10 prism diopters usually leads to a monofixation syndrome with central suppression but peripheral fusion, leading to improved depth perception. Amblyopia, residual esotropia or consecutive persistent exotropia may develop and should be addressed early to get the best possible visual and fusion potential.
Additional Resources
References
- ↑ Costenbader FD. Infantile esotropia. Trans Am Ophthalmol Soc 1961;59:397-429.
- ↑ Pediatric Eye Disease Investigator Group. Spontaneous resolution of early-onset esotropia: experience of the Congenital Esotropia Observational Study. Am J Ophthalmol. 2002 Jan;133(1):109-18. doi: 10.1016/s0002-9394(01)01316-2. PMID: 11755846.
- ↑ Worth C. squint, its causes and treatment. London: Bailliere, Tindall, and Cox, 1903.
- ↑ Chavasse FB. Worth’s squint on the binocular reflexes and the treatment of strabismus, 7th ed. Philadelphia: P.Blakiston’s Son & Co, 1939.
- ↑ Guyton, DL. Reaching for the Holy Grail in strabismus: the mechanism underlying infantile esotropia. J AAPOS. 2022 26(4):e1. https://doi.org/10.1016/j.jaapos.2022.08.006.
- ↑ Brodsky MC. Monocular nasotemporal optokinetic asymmetry-unraveling the mystery. J AAPOS. 2019 Oct;23(5):249-251. doi: 10.1016/j.jaapos.2019.07.001. Epub 2019 Sep 12. PMID: 31521846.
- ↑ Brodsky MC. Essential Infantile Esotropia: Potential Pathogenetic Role of Extended Subcortical Neuroplasticity. Invest Ophthalmol Vis Sci. 2018 Apr 1;59(5):1964-1968. doi: 10.1167/iovs.18-23780. PMID: 29677359.
- ↑ Wright KW. Esotropia. In: Wright KW. Pediatric ophthalmology and strabismus. St. Louis, MO: CV Mosby;1995.p.179-94.
- ↑ Wright KW, Walonker F, Edelman PM, , 10-diopter fixation test for amblyopia. Arch Ophthalmol 1981;99:1242-6.
- ↑ Robbins SL et al, Vision testing in the pediatric population, Ophthalmol Clin N Am 16 (2003) 253-267.
- ↑ Hiles DA, Watson A, Biglan AW. Characteristics of infantile esotropia following early bimedial rectus recession. Arch ophthalmol 1980;98:697-703.
- ↑ 12.0 12.1 Pediatric Eye Disease Investigator Group. Spontaneous resolution of early-onset esotropia: experience of the Congenital Esotropia Observational Study. Am J Ophthalmol 2002;133:109-18.
- ↑ Lam GC, Repka MX, Guyton DL. Timing of amblyopia therapy relative to strabismus surgery. Ophthalmology. 1993 Dec;100(12):1751-6. doi: 10.1016/s0161-6420(13)31403-1. PMID: 8259271.
- ↑ Ing M, Costenbader FD, Parks MM, et al. Early surgery for congenital esotropia. Am J Ophthalmol 1966;62:1419-1427.
- ↑ Taylor DM. How early is early surgery in the management of strabismus? Arch Ophthalmol 1963;70:752-6.
- ↑ Bhate M, Flaherty M, Martin FJ. Timing of surgery in essential infantile esotropia - What more do we know since the turn of the century? Indian J Ophthalmol. 2022 Feb;70(2):386-395. doi: 10.4103/ijo.IJO_1129_21. PMID: 35086202; PMCID: PMC9023972.
- ↑ 17.0 17.1 Elston J. Concomitant strabismus. In: Taylor D. Pediatric ophthalmology. 2nd ed. London: Blackwell science; 1997. p. 925-36.
- ↑ Raab EL. Comitant esotropia. In: Wilson ME, Saunders RA, Trivedi RH. Pediatric ophthalmology: current thoughts and practicle guide. Leipzig. Springer;2009. p. 85-112.
- ↑ AlShamlan FT, Alghazal F. Comparison of Dose Increments of Botulinum Toxin A with Surgery as Primary Treatment for Infantile Esotropia and Partially Accommodative Esotropia. Clin Ophthalmol. 2022 Aug 27;16:2843-2849. doi: 10.2147/OPTH.S382499. PMID: 36061630; PMCID: PMC9432566.
- ↑ Issaho DC, Carvalho FRS, Tabuse MKU, Carrijo-Carvalho LC, de Freitas D. The Use of Botulinum Toxin to Treat Infantile Esotropia: A Systematic Review With Meta-Analysis. Invest Ophthalmol Vis Sci. 2017 Oct 1;58(12):5468-5476. doi: 10.1167/iovs.17-22576. PMID: 29059315.
- ↑ Song D, Qian J, Chen Z. Efficacy of botulinum toxin injection versus bilateral medial rectus recession for comitant esotropia: a meta-analysis. Graefes Arch Clin Exp Ophthalmol. 2023 May;261(5):1247-1256. doi: 10.1007/s00417-022-05882-5. Epub 2022 Nov 2. PMID: 36322214.
- ↑ Niyaz L, Yeter V, Beldagli C. Success rates of botulinum toxin in different types of strabismus and dose effect. Can J Ophthalmol. 2023 Jun;58(3):239-244. doi: 10.1016/j.jcjo.2021.12.002. Epub 2022 Jan 14. PMID: 35038409.
- ↑ 23.0 23.1 de Alba Campomanes AG, Binenbaum G, Campomanes Eguiarte G. Comparison of botulinum toxin with surgery as primary treatment for infantile esotropia. J AAPOS. 2010 Apr;14(2):111-6. doi: 10.1016/j.jaapos.2009.12.162. PMID: 20451851.
- ↑ Mayet I, Ally N, Alli HD, Tikly M, Williams S. Botulinum neurotoxin injections in essential infantile esotropia-a comparative study with surgery in large-angle deviations. Eye (Lond). 2021 Nov;35(11):3071-3076. doi: 10.1038/s41433-020-01300-4. Epub 2021 Jan 11. PMID: 33432167; PMCID: PMC8526699.
- ↑ Gallo FG, Plaitano C, Esposito Veneruso P, Magli A. Long-Term Effects of Botulinum Toxin in Large-Angle Infantile Esotropia. Clin Ophthalmol. 2020 Oct 19;14:3399-3402. doi: 10.2147/OPTH.S266652. PMID: 33116391; PMCID: PMC7584504.