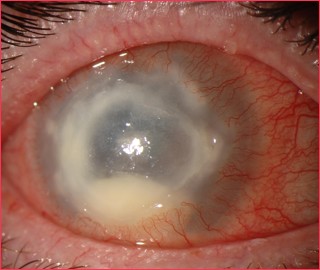
Acanthamoeba Keratitis
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Acanthamoeba keratitis.
Disease
Acanthamoeba keratitis, first recognized in 1973, is a rare, vision-threatening, parasitic infection seen most often in contact lens wearers. It is often characterized by pain out of proportion to findings and the late clinical appearance of a stromal ring-shaped infiltrate. It is both difficult to diagnose and difficult to treat.
Etiology and Incidence
Two of the 8 known species of Acanthamoeba, A. castellanii and A polyphaga, are responsible for most infections. Acanthamoeba are commonly found, free-living amoebae that have been located in various environments including pools, hot tubs, tap water, shower water, and contact lens solution. In May 2007, the US Food and Drug Administration (FDA) announced an outbreak of Acanthamoeba keratitis that was associated with Complete MoisturePlus Multi Purpose Solution, manufactured by Advanced Medical Optics. A systematic review and meta-analysis found that eyes with Acanthamoeba keratitis constitute 1.5% of the eyes with microbial keratitis, and it estimated the ratio of eyes with Acanthamoeba keratitis to the entire population to be 0.0002% or 2.3 eyes per 1 million people.[1]
Risk Factors
Risk factors include contact lens wear, exposure to organism (often through contaminated water), and corneal trauma. Low levels of anti-Acanthamoeba IgA in tears has also been shown to be a risk factor. It is thought that over 80% of Acanthamoeba keratitis appears in contact lens wearers. In 1 study, 75% of the patients were contact lens wearers; 40% wore daily soft lenses, 22% wore rigid gas-permeable lenses, and 38% wore extended wear or other lenses. In another case control study of 83 Acanthamoeba keratitis cases and 122 controls, daily-wear reusable lens users were at a three-fold higher risk of developing Acanthamoeba keratitis as daily disposable lens users.[2] Orthokeratology and cosmetic contact lenses wear may carry a high risk of Acanthamoeba keratitis.[3]
General Pathology and Pathophysiology
Acanthamoeba is ubiquitous. Corneal trauma, followed by exposure to the parasite (often through a water supply or contact lens solution) in a patient with low tear levels of anti-Acanthamoeba IgA leads to infection. Acanthamoeba exist in 2 forms: trophozoites and cysts. The trophozoites are mobile and consume bacteria (which allows for the diagnosis on E. coli plates). The trophozoites form double-walled cysts, which are incredibly resistant to methods of eradication (including freezing, heating, and irradiation).
The American Academy of Ophthalmology's Pathology Atlas contains a virtual microscopy image of Acanthamoeba keratitis.
Primary Prevention
Since treatment is toxic, lengthy, and not necessarily effective, prevention is essential. Contact lens wearers should be taught how to clean their contact lenses properly. They should be instructed never to use tap water or even saline to clean their lenses. They should also be instructed to visit an ophthalmologist at the earliest sign of problems.
Diagnosis
Diagnosis of Acanthamoeba keratitis is difficult and often delayed. Because the currently available treatments for Acanthamoeba are both toxic and lengthy, accurate diagnosis is essential. Diagnostic procedures usually begin with culture. The involved area of cornea can be scraped with a sterile instrument (blade, spatula, needle, calcium alginate swab, or cotton-tip applicator) under topical anesthesia at the slit lamp. The culture specimen can then be inoculated into a dish of E. coli plated over non-nutrient agar. Since the clinical picture is often nonspecific and coinfections are not uncommon,[4] cultures should be taken for bacterial, fungal, and viral infections as well. Acanthamoeba trophozoites and cysts can also be identified with the help of Gram, Giemsa-Wright, hematoxylin and eosin, periodic acid-Schiff, calcofluor white, KOH wet mount, or other stains. If available, confocal microscopy or polymerase chain reaction (PCR) are testing modalities that may be performed.[5][6] If culture or PCR results are negative or if the lesion is primarily intrastromal and epithelialized, a small corneal biopsy may be considered.
History
Patients should be asked about contact lens wear and hygiene, contact lens solutions, recent corneal trauma, and recent exposure to water sources.
Physical Examination
A comprehensive eye examination should be performed, with careful attention to the signs and symptoms described below.
Signs
Early signs may be mild and nonspecific. Possible findings include epithelial irregularities, epithelial or anterior stromal infiltrates, and pseudodendrites. Later signs include deep stromal infiltrates (ring-shaped, disciform, or nummular), corneal perforation, satellite lesions, persistent epithelial defects, radial keratoneuritis, scleritis, and anterior uveitis with hypopyon, peripheral anterior synechiae and iris atrophy and secondary glaucoma. Advanced signs include stromal thinning and corneal perforation.
Symptoms
Acanthamoeba keratitis is usually characterized by pain out of proportion to findings. Patients may also complain of decreased vision, redness, foreign body sensation, photophobia, tearing, and discharge. Symptoms may wax and wane; they may be quite severe at times.
Differential diagnosis
The differential diagnosis for Acanthamoeba in its early clinical stages includes herpes simplex keratitis, recurrent corneal erosion, staphylococcal marginal keratitis, and contact lens-associated keratitis. The differential diagnosis of later clinical stages includes viral, bacterial, fungal, and sterile (such as from topical anesthetic abuse) keratitis. Polymicrobial infection may also occur.
Management
Medical therapy
Medical treatment for Acanthamoeba keratitis is still evolving. Success has been reported with various combinations of antibiotic, antiviral, antifungal, and antiparasitic drugs. Different regimens include combinations of diamidines, biguanides, antibiotics, and antifungals, but the most frequently used drugs are biguanides as monotherapy or in combination with a diamidine. Some topical preparations of diamidines are propamidine-isethionate, hexamidine-diisethionate, and dibromopropamidine. Biguanides include polyhexamethylene biguanide (PHMB) and chlorhexidine. Neomycin-polymyxin B-gramicidin is thought to kill bacteria, which provides a food source for the Acanthamoeba. Antifungals include topical and oral preparations of voriconazole as well as ketoconazole, miconazole, clotrimazole and posaconazole . Voriconazole 1% was shown to be effective in a small study (n=18).[7] Oral miltefosine has been used more recently in refractory cases of Acanthamoeba keratitis[8] with resolution of disease. Severe inflammatory responses following adjuvant therapy with miltefosine have been reported.[8][9][10] Monotherapy with PHMB 0.08% was found to be as effective as dual therapy with PHMB 0.02% and propamidine 0.1% with cure rates of 86% in a RCCT.[11] Benzalkonium chloride (BAK) is an ophthalmic preservative and quaternary ammonium surfactant with antimicrobial properties including efficacy against Acanthamoeba. As such, Kaufman and Tu suggest adding a BAK-containing antibiotic ophthalmic drop such as fluoroquinolones (ciprofloxacin, ofloxacin, and gatifloxacin but not BAK-free moxifloxacin) to the treatment regimen of Acanthamoeba keratitis.[3] Steroids are controversial and may worsen the condition by inhibiting the host immune response; they are unnecessary in most cases of Acanthamoeba keratitis. However, steroid drops can have a beneficial role in selected cases with persisting inflammation. In such cases, topical steroids can be used only if started after anti-amoebic treatment has completed at least 2-3 weeks, and anti-amoebic therapy needs to be maintained throughout and continued after steroids have been withdrawn.[11][12] Pain should be addressed. Kaufman and Tu provide an intelligible management algorithm in their 2022 literature review linked here.[3] A study published in 2025, showed better outcomes in Acanthamoeba keratitis when an evidence based treatment protocol was used compared to an individualised treatment.[13]
Medical follow-up
Patients should be followed very closely (daily or almost daily) initially, until clinical response is seen or progression of the disease is blunted. Since recurrences can occur and Acanthamoeba cysts are so resistant to treatment, medical treatments should be tapered very slowly and, if necessary, continued for many months.
Surgery
Cases of corneal perforation may need to be managed with surgical interventions. Conjunctival flap and amniotic membrane have been used with varying success.[14] The use of collagen crosslinking in the treatment of Acanthamoeba keratitis has demonstrated variable outcomes.[15][16] If possible, penetrating keratoplasty should be reserved for cases of visually significant corneal scarring in quiet eyes. If there are still signs of active infection, medical therapy for Acanthamoeba should resume after keratoplasty, as cysts may linger in the cornea and cause recurrent infection in the graft.
Surgical follow-up
Patients should be followed closely at first to monitor for signs of recurrent infection.
Complications
Postoperative complications after penetrating keratoplasty include recurrence of Acanthamoeba infection. Other possible complications include infection, glaucoma, cataract, wound leak, rejection, and astigmatism.
Prognosis
The prognosis for Acanthamoeba is worse than for many other types of infectious keratitis, and prevention is therefore very important. However, especially if caught early before the onset of stromal disease, satisfactory outcomes can certainly be achieved.
Additional Resources
- Turbert D, Huffman JM. What Is a Corneal Ulcer (Keratitis)? American Academy of Ophthalmology. EyeSmart/Eye health. https://www.aao.org/eye-health/diseases/corneal-ulcer. Accessed February 5, 2026.
- Ocular Pathology Atlas. American Academy of Ophthalmology Web site. https://www.aao.org/resident-course/pathology-atlas. Published 2016. Accessed January 4, 2017.
- Krachmer J, Mannis M, Holland E: Cornea, 2nd ed. Elsevier Mosby, 2005, 1115-1122.
Reference
- ↑ Aiello F, Gallo Afflitto G, Ceccarelli F, Turco MV, Han Y, Amescua G, Dart JK, Nucci C. Perspectives on the Incidence of Acanthamoeba Keratitis: A Systematic Review and Meta-Analysis. Ophthalmology. 2025 Feb;132(2):206-218. doi: 10.1016/j.ophtha.2024.08.003. Epub 2024 Aug 9. PMID: 39127408.
- ↑ Carnt N, Minassian DC, Dart JKG. Acanthamoeba Keratitis Risk Factors for Daily Wear Contact Lens Users: A Case-Control Study. Ophthalmology. 2023 Jan;130(1):48-55. doi: 10.1016/j.ophtha.2022.08.002. Epub 2022 Aug 8. PMID: 35952937.
- ↑ 3.0 3.1 3.2 Kaufman AR, Tu EY. Advances in the management of Acanthamoeba keratitis: A review of the literature and synthesized algorithmic approach. Ocul Surf. 2022 Jul;25:26-36. doi: 10.1016/j.jtos.2022.04.003. Epub 2022 Apr 22. PMID: 35462076.
- ↑ Raghavan A, Baidwal S, Venkatapathy N, Rammohan R. The Acanthamoeba-Fungal Keratitis Study. Am J Ophthalmol. 2019 May;201:31-36. doi: 10.1016/j.ajo.2019.01.024. Epub 2019 Feb 2. PMID: 30721687.
- ↑ Parmar DN, Awwad ST, Petroll WM, Bowman RW, McCulley JP, Cavanagh HD. Tandem scanning confocal corneal microscopy in the diagnosis of suspected acanthamoeba keratitis. Ophthalmology. 2006 Apr;113(4):538-47. doi: 10.1016/j.ophtha.2005.12.022. PMID: 16581415.
- ↑ Biology 2023, 12(12), 1489; https://doi.org/10.3390/biology12121489
- ↑ Bagga B, Sharma S, Gour RPS, Mohamed A, Joseph J, M Rathi V, Garg P. A randomized masked pilot clinical trial to compare the efficacy of topical 1% voriconazole ophthalmic solution as monotherapy with combination therapy of topical 0.02% polyhexamethylene biguanide and 0.02% chlorhexidine in the treatment of Acanthamoeba keratitis. Eye (Lond). 2021 May;35(5):1326-1333. doi: 10.1038/s41433-020-1109-4. Epub 2020 Jul 27. PMID: 32719525; PMCID: PMC8182824.
- ↑ 8.0 8.1 Thulasi P, Saeed HN, Rapuano CJ, Hou JH, Appenheimer AB, Chodosh J, Kang JJ, Morrill AM, Vyas N, Zegans ME, Zuckerman R, Tu EY. Oral Miltefosine as Salvage Therapy for Refractory Acanthamoeba Keratitis. Am J Ophthalmol. 2021 Mar;223:75-82. doi: 10.1016/j.ajo.2020.09.048. Epub 2020 Oct 10. PMID: 33045218.
- ↑ Si Z, Veldman PB, Reidy JJ, Farooq AV. Severe Inflammatory Response in a Patient on Oral Miltefosine for Acanthamoeba Keratitis. Ocul Immunol Inflamm. 2022 May 19;30(4):1027-1028. doi: 10.1080/09273948.2020.1854315. Epub 2021 Feb 9. PMID: 33560165.
- ↑ de la Presa M, Ibach M, Berdahl J, Holland EJ. Anterior Scleral and Limbal Inflammatory Necrosis After Adjuvant Miltefosine for Recalcitrant Acanthamoeba Keratitis. Cornea. 2022 Jun 1;41(6):775-778. doi: 10.1097/ICO.0000000000002849. Epub 2021 Sep 3. PMID: 34483272.
- ↑ 11.0 11.1 Dart JKG, Papa V, Rama P, Knutsson KA, Ahmad S, Hau S, Sanchez S, Franch A, Birattari F, Leon P, Fasolo A, Kominek EM, Jadczyk-Sorek K, Carley F, Hossain P, Minassian DC. The Orphan Drug for Acanthamoeba Keratitis (ODAK) Trial: PHMB 0.08% (Polihexanide) and Placebo versus PHMB 0.02% and Propamidine 0.1. Ophthalmology. 2024 Mar;131(3):277-287. doi: 10.1016/j.ophtha.2023.09.031. Epub 2023 Oct 5. PMID: 37802392.
- ↑ Dart JK, Saw VP, Kilvington S. Acanthamoeba keratitis: diagnosis and treatment update 2009. Am J Ophthalmol. 2009 Oct;148(4):487-499.e2. doi: 10.1016/j.ajo.2009.06.009. Epub 2009 Aug 5. PMID: 19660733.
- ↑ Dart JKG, Papa V, Rama P, Knutsson KA, Ahmad S, Hau S, Sanchez S, Franch A, Birattari F, Leon P, Fasolo A, Mrukwa-Kominek E, Jadczyk-Sorek K, Carley F, Parwez H, Minassian DC. Acanthamoeba keratitis treatment outcomes compared for drug delivery by protocol versus physician's individualised treatment. Ocul Surf. 2025 Oct;38:132-141. doi: 10.1016/j.jtos.2025.03.008. Epub 2025 Apr 7. PMID: 40204130.
- ↑ Abdulhalim BE, Wagih MM, Gad AA, Boghdadi G, Nagy RR. Amniotic membrane graft to conjunctival flap in treatment of non-viral resistant infectious keratitis: a randomised clinical study. Br J Ophthalmol. 2015 Jan;99(1):59-63. doi: 10.1136/bjophthalmol-2014-305224. Epub 2014 Jul 22. PMID: 25053758.
- ↑ Papaioannou L, Miligkos M, Papathanassiou M. Corneal Collagen Cross-Linking for Infectious Keratitis: A Systematic Review and Meta-Analysis. Cornea. 2016 Jan;35(1):62-71. doi: 10.1097/ICO.0000000000000644. PMID: 26509768.
- ↑ Ting DSJ, Henein C, Said DG, Dua HS. Photoactivated chromophore for infectious keratitis - Corneal cross-linking (PACK-CXL): A systematic review and meta-analysis. Ocul Surf. 2019 Oct;17(4):624-634. doi: 10.1016/j.jtos.2019.08.006. Epub 2019 Aug 8. PMID: 31401338.