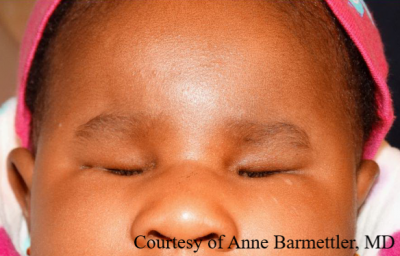
Anophthalmia
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Disease
Anophthalmia is a severe form of ocular malformation characterized by the complete absence of an eye (Figure 1) [1]. This differs from a similar appearing disorder, microphthalmia, in which the patient has a hypoplastic eye remnant or residual neuroectoderm in the eye socket [2]. Of note, the term “clinical anophthalmia” refers to what appears to be complete absence of the eye, however there actually is some residual tissue [3]. Anophthalmia can occur as either an isolated developmental abnormality or as part of a syndrome [2].
Etiology
Anophthalmia results from failed development of optic structures, which can occur due to a defect in neural tube induction, formation of the optic vesicle and/or cup, or by secondary breakdown of previously formed optic tissues [2].
Anophthalmia has a complex etiology that is not fully elucidated, but is thought to include both genetic and environmental components. The genetics of anophthalmia are discussed below. Possible contributing environmental factors include infections (such as several TORCH infections including CMV, rubella, Parvovirus B19, and toxoplasmosis), nutritional deficiencies (vitamin A), and in utero exposure to toxins (alcohol, thalidomide, warfarin) [2].
Genetics
Several genes are implicated in the development of anophthalmia. Mutations in SOX2, OTX2, PAX6, STRA6, ALDH1A3, RARB, VSX2, RAX, FOXE3, BMP4, BMP7, GDF3, GDF6, ABCB6, ATOH7, C12orf57, TENM3 (ODZ3), and VAX1 have all been implicated in abnormal ocular development and the pathogenesis of anophthalmia [4] [5].
SOX2: Mutations in SOX2 are the most common genetic cause of anophthalmia and are present in up to 40% of cases of anophthalmia [4]. These are most commonly de novo, loss of function mutations with a heterozygous genotype [5]. The SOX2 gene encodes a transcription factor that plays a central role in differentiation of lens tissue from surface ectoderm [6]. Cases of anophthalmia with identified SOX2 mutations are characteristically bilateral and may occur as part of SOX2 anophthalmia syndrome [4]. Extraocular manifestations of SOX2 anophthalmia syndrome include learning disabilities, growth and motor delays, seizures, and malformation of CNS structures such as the hippocampus, pituitary gland, and corpus callosum [4].
OTX2: Mutations in the OTX2 gene are also commonly implicated in a wide range of ocular malformations and occurs in 3% of patients with bilateral anophthalmia [5]. OTX2 encodes a transcription factor that is implicated in differentiation of the optic vesicle and formation of the retina and assists in the development of pigmentation [7]. OTX2 genes have considerable variable expressivity in phenotypic presentation. Extraocular manifestations associated with OTX2 mutations include learning disability, developmental delay, and structural abnormalities of brain structures [4].
PAX6: PAX6 is one of the main regulatory molecules in optic development [6]. PAX6 helps to control expression of other key genes in differentiation of structures of the eye and plays a direct role in the establishment of eye fields and formation of the lens [6]. PAX6 mutations have classically been implicated in aniridia, but there appear to be interactions between PAX6 and SOX2 mutations that contribute to the development of anophthalmia [5]. Extraocular manifestations associated with PAX6 mutations include growth, mental, and motor delay, seizures, ADHD, hypotonia, and microcephaly [4].
Pathophysiology
The eye is formed through a well-coordinated set of steps involving differentiation of tissues derived from neuroectoderm, neural crest, mesoderm, and surface ectoderm [7]. Development of optic tissues typically begins in the fourth week of development with closure of the rostral neuropore of the neural tube [6]. The optic vesicles form from neuroectoderm of the forebrain. The optic vesicles induce differentiation of surface ectoderm into lens tissue and the vesicles themselves invaginate to form optic cups. The optic cups grow around the developing lens to form structures of the mature globe, including the retina, iris, and ciliary body. The optic stalk, which connects the optic cup to the forebrain, develops into the optic nerve. Surrounding mesenchyme is induced to form structures of the choroid, cornea, and sclera [6]. Ocular malformations, such as anophthalmia, occur due to failure of these steps of development to occur properly. True anophthalmia, or complete absence of eye tissues, is classified in primary, secondary and consecutive anophthalmia, depending on the stage in which failure of development or secondary degeneration occurs. In primary anophthalmia, which is rare and usually bilateral, the primary optic vesicles fail to from from the cerebral vesicle. Secondary anophthalmia occurs secondary to gross abnormalities in the anterior neural tube, and is considered rare and lethal. Consecutive anophthalmia occurs from a secondary degeneration of the optic vesicles.
Epidemiology
True anophthalmia is a rare birth defect. Studies from California [8] and Italy [9] have reported the incidence as 0.18 cases per 10,000 births and 0.33 cases per 10,000 births, respectively. The majority of cases are bilateral with one source documenting 53-71% of cases as bilateral based on the etiology of the malformation (isolated vs syndromic vs chromosomal anomaly) [10].
Risk Factors
Risk factors for anophthalmia include older maternal age (greater than 40), multiple births, low birth weight, and prematurity [2]. In utero risk factors include infections, maternal vitamin A deficiency, hyperthermia, and exposure to toxins such as warfarin and alcohol [2]. Anophthalmia may also occur within the context of genetic syndromes, such as trisomy 13, trisomy 18, and mosaic trisomy 9 [2].
Diagnosis
Prenatal Assessment
Anophthalmia can be discovered prenatally via ultrasound [11]. Ocular malformations can be detected as early as the end of the first trimester by use of two- and three-dimensional ultrasound and diagnosis can be confirmed with fetal MRI [11][12]. However, anophthalmia is seldom detected by prenatal ultrasound unless other abnormalities are present as well [13]. Given the possible syndromic etiology of anophthalmia, identification of absence of the eye on ultrasound should prompt a further genetic workup via amniocentesis or chorionic villus sampling [13]. Other environmental causes (infection, toxin exposure, vitamin A deficiency) should be explored as well [13].
Postnatal Assessment
Neonatal features indicative of anophthalmia include collapsed structures of the lid with a shortened lid fissure and small conjunctival sac [14]. A thorough examination should be formed to identify any other abnormalities that may indicate the presence of a genetic syndrome [15]. Ophthalmic findings of the single eye in the case of unilateral anophthalmia may include coloboma, cataracts, retinal defects, or optic nerve hypoplasia [15]. Any concern for ocular malformation should prompt an assessment by a pediatric ophthalmologist as soon as possible. This assessment should consist of physical examination of structures of the eyes and orbits, as well as examination of the parents for any relevant family history, gestational exposure, or ocular abnormalities [15].
Imaging
If an ocular malformation is suspected, an ultrasound should be performed to assess for the presence of optic structures [15]. Electrodiagnostics, such as flash visual evoked potentials, can be used to determine if there is residual functioning retinal tissue [15]. CT and MR imaging can further characterize contents of the globe, the degree of involvement of central optic nervous tissue, and to screen for co-existing CNS abnormalities [2]. Figure 2 compares an MRI of a patient with normal optic structures within the socket and a patient with anophthalmia. CNS abnormalities that may occur in syndromic anophthalmia include pituitary hypoplasia, hippocampal malformation, hypothalamic abnormalities, and fusiform gyrus defects [2][16]. Renal ultrasound is also recommended in patients with anophthalmia due to the high co-occurrence of ocular and renal pathology [15].
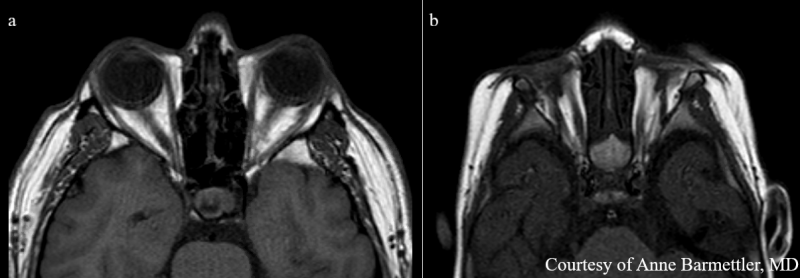
Figure 2: Axial T1 MRI of a patient with normal optic structures (2a) compared to MRI of a patient with anophthalmia (2b). Note the complete absence of globes and aplasia of optic nerves as compared to the normal image. Extraocular muscles can still be seen within the socket. Image courtesy of Anne Barmettler, MD.
Genetic Screening
Screening for genetic syndromes should begin with a history and examination of both the patient and family members to assess for both ocular and extraocular pathology [15]. A multi-disciplinary approach involving pediatricians, ophthalmologists, and clinical geneticists is recommended [2]. Any suspicion for underlying genetic syndromes should prompt an appropriate genetic workup. Chromosomal analysis and genetic screening can be performed in both syndromic and isolated cases to identify mutations with known implications in anophthalmia [15].
Management
Of note, if the anophthalmia is unilateral, excellent ophthalmic care of the remaining eye is crucial and monocular precautions (such as polycarbonate lenses with full time wear) should be employed.
Socket Expansion
Due to the severity of the potential impact of anophthalmia on the growth and development of facial structures, early intervention in the first year of life is recommended after anophthalmia is diagnosed [15]. If untreated, the socket will remain underdeveloped and compromise the ability to wear an ocular prosthesis later in life. In cases of unilateral anophthalmia, this will cause marked facial asymmetry. A non-surgical intervention of socket expanders can be used to facilitate proper development of the socket to minimize facial dysmorphia and maximize ability for implantation of future prosthesis [2]. These socket expanders look like an ocular prosthesis, but without any drawings, and are placed into the conjunctival fornices in the same location as a prosthesis. Antibiotic drops can be considered for infection prevention and the lids are closed until the patient is ready for a larger socket expander or an orbital implant [15]. Some people utilize hydrophilic expanders to allow for gradual expansion of the material following placement [17].
Orbital Implantation
Approximately two months after introduction of a socket expander, a surgery can be considered to place an orbital implant to permanently increase orbital volume and stimulate normal orbital socket development [17]. Implants can be autologous, like a dermis fat graft, or can be made from a variety of materials including both nonporous materials (acrylic) and porous materials (hydroxyapatite, polyethylene, aluminum oxide) [18]. Dermis fat grafts tend to grow with the child, decreasing the number of times the child has to undergo surgery. Man-made implants require progressively larger implants to be exchanged as the patient continues to grow and develop, allowing for continued expansion of the socket [17]. Once postoperative edema resolves, an ocular prosthesis can be worn over this.
Additional Surgical Considerations
After initial expansion and exchange of increasingly larger orbital implants, patients will require visits on an annual basis for examination and review of the implant [15]. Surgical correction of the lacrimal sac and eyelid may also be required for better overall cosmetic results [2].
References
- ↑ D.R. FitzPatrick, V.V. Heyningen. Developmental eye disorders. Curr. Opin. Genet. Dev., 15 (3) (2005), pp. 348-353.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 Verma AS, Fitzpatrick DR. Anophthalmia and microphthalmia. Orphanet J Rare Dis. 2007; 2:47. Published 2007 Nov 26. doi:10.1186/1750-1172-2-47.
- ↑ Plaisancié, J., Ceroni, F., Holt, R. et al. Genetics of anophthalmia and microphthalmia. Part 1: Non-syndromic anophthalmia/microphthalmia. Hum Genet 138, 799–830 (2019).
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 K.A. Williamson, D.R. FitzPatrick. The genetic architecture of microphthalmia, anophthalmia and coloboma. Eur. J. Med. Genet., 57 (2014), pp. 369-380.
- ↑ 5.0 5.1 5.2 5.3 L. Mauri, A. Franzoni, M. Scarcello, et al. SOX2, OTX2 and PAX6 analysis in subjects with anophthalmia and microphthalmia. Eur J Med Genet, 58 (2015), pp. 66-70.
- ↑ 6.0 6.1 6.2 6.3 6.4 Sadler, T. W., & Langman, J. (2012). Langman's medical embryology (12th ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins, pp. 329-336.
- ↑ 7.0 7.1 Fuhrmann S. Eye morphogenesis and patterning of the optic vesicle. Curr Top Dev Biol. 2010; 93:61-84. doi:10.1016/B978-0-12-385044-7.00003-5.
- ↑ Shaw GM, Carmichael SL, Yang W, Harris JA, Finnell RH & Lammer EJ (2005): Epidemiologic characteristics of anophthalmia and bilateral microphthalmia among 2.5 million births in California, 1989–1997. Am J Med Genet A 137: 36–40.
- ↑ Clementi M, Tenconi R, Bianchi F, Botto L, Calabro A, Calzolari E, Cianciulli D, Mammi I, Mastroiacovo P, Meli P, Spagnolo A, Turolla L, Volpato S. 1996. Congenital eye malformations: A descriptive epidemiologic study in about one million newborns in Italy. Birth Def Orig Art Series 30: 413–424.
- ↑ Kallen B, Robert E, Harris J. The Descriptive Epidemiology of Anophthalmia and Microphthalmia, International Journal of Epidemiology, Volume 25, Issue 5, October 1996, Pages 1009–1016.
- ↑ 11.0 11.1 Mashiach R, Vardimon D, Kaplan B, Shalev J, Meizner I. Early sonographic detection of recurrent fetal eye anomalies. Ultrasound Obstet Gynecol. 2004 Nov;24(6):640-3.
- ↑ Searle A, Shetty P, Melov SJ, Alahakoon TI. Prenatal diagnosis and implications of microphthalmia and anophthalmia with a review of current ultrasound guidelines: two case reports. J Med Case Rep. 2018;12(1):250. Published 2018 Aug 29.
- ↑ 13.0 13.1 13.2 Benacerraf BR, Bromley B, Jelin AC. Anophthalmia and Microphthalmia. Am J Obstet Gynecol. Volume 221, Issue 5. Nov 2019.
- ↑ Schittkowski, MP, Gundlach, KKH & Guthoff, RF Congenital clinical anophthalmos and functionless microphthalmos. Ophthalmologe 100 : 507-517 (2003).
- ↑ 15.00 15.01 15.02 15.03 15.04 15.05 15.06 15.07 15.08 15.09 15.10 Ragge, N., Subak-Sharpe, I. & Collin, J. A practical guide to the management of anophthalmia and microphthalmia. Eye 21, 1290–1300 (2007).
- ↑ Sisodiya SM, Ragge NK, Cavalleri GL, Hever A, Lorenz B, Schneider A, Williamson KA, Stevens JM, Free SL, Thompson PJ, van Heyningen V, Fitzpatrick DR. Role of SOX2 mutations in human hippocampal malformations and epilepsy. Epilepsia. 2006 Mar;47(3):534-42.
- ↑ 17.0 17.1 17.2 Helmuth Gundlach, Karsten Kurt M.D., D.D.S., M.S.D.; Guthoff, Rudolf Friedrich M.D.; Martin Hingst, Volker Hermann D.D.S.; Schittkowski, Michael Peter M.D.; Bier, Ulrich Christian M.D., D.D.S. Expansion of the Socket and Orbit for Congenital Clinical Anophthalmia, Plastic and Reconstructive Surgery: October 2005 - Volume 116 - Issue 5 - p 1214-1222.
- ↑ Quaranta-Leoni, Francesco M Treatment of the anophthalmic socket, Current Opinion in Ophthalmology: September 2008 - Volume 19 - Issue 5 - p 422-427.