Argyrosis of the Conjunctiva
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
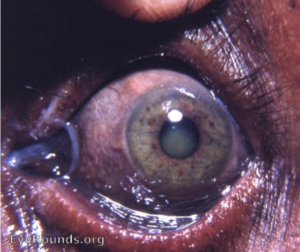
Argyrosis, derived from the Greek word for silver (argyros), is a condition caused by chronic exposure to chemical forms of the element silver. The most recognized symptom is the dramatic blue or bluish-grey colored skin.
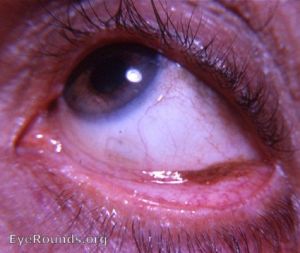
Disease Entity
Ocular discoloration caused by the local or systemic absorption of silver is known as ocular argyrosis. Argyrosis, any bodily discoloration caused by silver, may be the visible manifestation of generalized argyrosis.[1] Large doses of silver were used medicinally since the 17th century in the treatment of disorders such as epilepsy. Some records exist of silver nitrate being used therapeutically in 69 BC. Therapeutic argyria is now rarely seen but occurs infrequently in the patient receiving silver-containing ocular medications such as argyrol.
Ocular argyrosis has been reported after repeated exposure to silver-containing compounds, usually from topical silver-containing medicinal solutions [2] or occupational exposures. [1][3][4] [5] Case reports exist of argyria in studio photographers and dentists. Argyrosis should be considered in the differential diagnosis of focal pigmented conjunctival lesions. Aside from the discoloration of the eye, few ocular pathologic alterations occur with argyrosis with the most common being difficulties adapting to dark environments. Rare involvement of the lacrimal sac, lens, and cornea have also been reported.
Etiology
As stated above, ocular argyrosis is commonly reported after repeated exposure to silver-containing compounds. After prolonged exposure, silver is deposited into the tissues causing argyrosis.
Risk Factors
Ocular argyrosis typically occurs in individuals with long- term exposure to silver due to occupational hazards, silver- containing cosmetics, silver- containing medications, or acute exposure due to ocular injury from chemical explosions.[6] One article demonstrated a direct relationship between the levels of ocular pigmentation and duration of employment.[1] Another case report showed ocular argyrosis after long-term application of eyelash tint.[2] Subconjunctival ocular argyrosis has been described after treatment with Ruthenium-106 (Ru-106) brachytherapy, which consists of a radioactive core of Ru-106 surrounding by pure silver, for choroidal melanoma.[7]
General Pathology
Histologic examination has demonstrated silver deposition in the conjunctival epithelium, basement membrane and superficial substantia propria of the conjunctiva, Descemet's membrane, lens, and Bruch's membrane.[2][8]
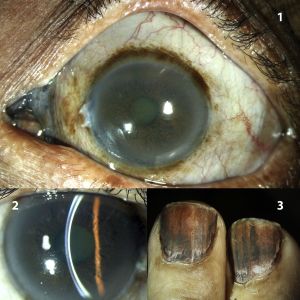
Diagnosis
Clinical evaluation may reveal various degrees of silver deposition/hyperpigmentation on the upper eyelid, lid margin, caruncle, conjunctiva, and/or diffuse Descemet’s membrane deposits.
Diagnostic Procedures
Clinical evaluation may reveal various degrees of silver deposition on the upper eyelid, lid margin, caruncle and conjunctiva, and/or diffuse Descemet’s membrane deposits. Hyperreflectivity seen in Bowman's layer and Descemet's membrane due to presumed silver deposition in ocular argyrosis has been described on anterior segment ocular coherence tomography (AS-OCT) imaging.[8] In vivo confocal microscopy has also been used to describe reflective deposits in Descemet's membrane, Bowman's layer, and corneal stroma in patients with suspected ocular argyrosis.[6]
Management
Management of this condition primarily involves prevention. Individuals with occupations that place them at risk should be protected with protective goggles.
Prognosis
Although a significant functional deficit related to ocular silver deposition has not been clearly documented, the possibility of subtle visual changes or future deficits cannot be ruled out. Of note, a recent case report outlined a 66-year-old jeweler with bilateral corneal deposits due to occupational silver exposure[9]. Notably, the patient exhibited impaired contrast sensitivity under scotopic conditions, suggesting potential retinal involvement[9]. This potential visual consequence creates a potential utility of regular comprehensive eye examinations, including contrast sensitivity measurements, in patients who have been exposed to an external source of silver.
References
- ↑ 1.0 1.1 1.2 Moss AP, Sugar A, Hargett NA, Atkin A, Wolkstein M, Rosenman KD. The ocular manifestations and functional effects of occupational argyrosis. Arch Ophthalmol. 1979 May;97(5):906-8. PubMed PMID: 312638.
- ↑ 2.0 2.1 2.2 Gallardo MJ, Randleman JB, Price KM, Johnson DA, Acosta S, Grossniklaus HE, Stulting RD. Ocular argyrosis after long-term self-application of eyelash tint. Am J Ophthalmol. 2006 Jan;141(1):198-200. PubMed PMID: 16387002.
- ↑ Hanna C, Fraunfelder FT, Sanchez J. Ultrastructural study of argyrosis of the cornea and conjunctiva. Arch Ophthalmol. 1974 Jul;92(1):18-22. PubMed PMID: 4835972.
- ↑ Yanoff M, Scheie HG. Argyrosis of the conjunctiva and lacrimal sac. Arch Ophthalmol. 1964 Jul;72:57-8. PubMed PMID: 14149749.
- ↑ Wilkes Jw. Argyrosis of the cornea and conjunctiva. J Tn State Med Assoc. 1953 Jan;46(1):11-13. PubMed PMID: 13011834.
- ↑ 6.0 6.1 Wu M, Wang X, Shao T, Wang Y. Case Report: In Vivo Confocal Microscopic Appearance of Corneal Argyrosis. Optom Vis Sci. Nov 2017;94(11):1066-1069. doi:10.1097/OPX.0000000000001133
- ↑ Khasati A, Thaung C, Mudhar HS, et al. Subconjunctival Ocular Argyrosis following Treatment with Ruthenium 106 Brachytherapy for Choroidal Melanoma. Ocul Oncol Pathol. Sep 2023;9(3-4):101-106. doi:10.1159/000531385
- ↑ 8.0 8.1 He X, Simmons NL, Wozniak RAF. Anterior Segment Optical Coherence Tomography in Ocular Argyrosis.Cornea. Nov 2020;39(11):1433-1435. doi:10.1097/ICO.0000000000002323
- ↑ 9.0 9.1 Mora NF, Bueis ABL. Ocular argyrosis. Oman J Ophthalmol. 2023 Jun 27;16(2):373-376. doi: 10.4103/ojo.ojo_337_22. PMID: 37602163; PMCID: PMC10433047.
- Calvery HO, Lightbody HD, Rones B: Effectof some silver salts on the eye. Arch Ophthalmol25:839-847, 1941.

