Childhood Glaucoma Research Network Classification and Epidemiology of Childhood Glaucoma
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Background
Pediatric glaucoma is a group of disorders that result in ocular hypertension with subsequent optic nerve damage and vision loss if left untreated. It accounts for 5% of blindness in the pediatric population[1] and affects more than 300,000 children in the world.[2] A diagnosis of glaucoma in childhood carries a tremendous economic burden on caregivers, and the quality of life for these children is lower compared to children without glaucoma. Because pediatric glaucoma is a heterogeneous disease, the Childhood Glaucoma Research Network (CGRN) classification system was developed to provide an organized and unified classification system of childhood glaucoma into seven subsets (glaucoma suspects plus 6 groups of childhood glaucoma).[3]
Childhood Glaucoma Research Network (CGRN) Classification
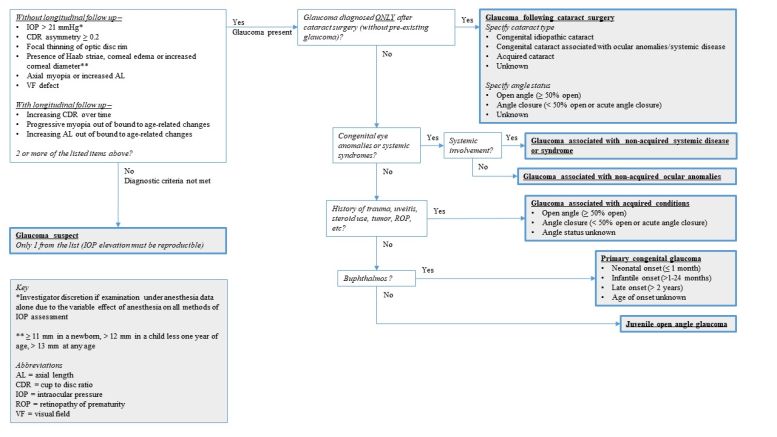
Childhood glaucoma is diagnosed based on the presence of ≥2 of the following criteria: 1) Intraocular pressure (IOP) of 21 mmHg or more, 2) optic nerve glaucomatous damage such as increased cupping, focal notching, or cup to disc asymmetry of 0.2 or more between both eyes, 3) Corneal changes such as increased corneal diameter or Haab striae, or 4) visual field defects consistent with optic nerve glaucomatous damage. Under the CGRN classification system, childhood glaucoma has been classified as primary or secondary (Figure).[3]
Primary glaucoma can be further subdivided into primary congenital glaucoma (PCG) and juvenile open-angle glaucoma (JOAG). PCG is defined as glaucoma that occurs in the absence of any acquired or non-acquired conditions, with associated isolated angle anomalies with or without iris anomalies. It is usually associated with ocular enlargement. JOAG is defined as open-angle glaucoma that occurs in isolation from any acquired or non-acquired ocular conditions or syndromes, without signs of ocular enlargement (e.g., buphthalmos) and with a normal-appearing angle.
Secondary glaucoma can be further subdivided into four categories: associated with non-acquired ocular anomalies (glaucoma develops without prior cataract surgery, in the setting of a non-acquired condition that is predominately ocular present at birth e.g. Aniridia, Axenfeld-Rieger anomaly, and microcornea); associated with non-acquired systemic disease or syndrome (glaucoma develops without prior cataract surgery, in the setting of a non-acquired condition that is present at birth and predominately systemic with or without ocular manifestations e.g. Marfan syndrome, Stickler syndrome); associated with acquired conditions (glaucoma that develops due to a condition that is not present at birth e.g. uveitis and trauma); or following cataract surgery (GFCS).
The CGRN also allows classification for children in which the diagnosis of glaucoma may be suspected but not proven. Glaucoma suspect is diagnosed based on the presence of ocular hypertension (IOP > 21 mmHg) on 2 separate occasions, visual field abnormalities suspicious of glaucoma, optic nerve appearance suspicious of glaucoma, or signs of ocular enlargement (e.g., increased corneal diameter or axial length) with normal IOP. This results in a total of seven categories in the CGRN system. One advantage of the CGRN system is its ease of use, unambiguity, and global applicability.[3]
Epidemiology:
Table 1. Summary of the published studies categorizing the childhood glaucoma patients according to the CGRN classification.
| Study | Country | Number of patients | PCG | JOAG | GFCS | Glaucoma associated with
acquired conditions |
Glaucoma associated with
non-acquired systemic anomalies |
Glaucoma associated with
non-acquired ocular anomalies |
Glaucoma suspects |
|---|---|---|---|---|---|---|---|---|---|
| Bouhenni et al.[4] | US (Akron OH) | 108 | 3 | 17 | 1 | 22 | 12 | 3 | 50 |
| Tam et al.[5] | US (Boston, MA) | 246 | 54 | 11 | 73 | 17 | 20 | 17 | N/A |
| Mokbel et al.[6] | Dakahelia, Egypt | 207 | 114 | 2 | 15 | 61 | 4 | 11 | N/A |
| Hoguet et al.[7] | US (Miami, FL) | 205 | 39 | 9 | 22 | 28 | 14 | 10 | 79 |
| Lopes et al.[8] | Sao Paulo, Brazil | 496 | 218 | 2 | 63 | 50 | 38 | 59 | 66 |
| Senthil et al.[9] | Hyderabad, India | 275 | 97 | 38 | 22 | 44 | 16 | 48 | N/A |
| Knight et al.[10] | Australian and New Zealand Registry of Advanced Glaucoma | 290 | 167 | 56 | 5 | 3 | 6 | 49 | N/A |
| El Sayed et al.[11] | Cairo, Egypt | 652 | 445 | 2 | 55 | 13 | 38 | 31 | 68 |
| Surukrattanaskul et al.[12] | Thailand | 423 | 88 | 8 | 33 | 80 | 32 | 97 | 85 |
| Total | 2902 | 1225 | 145 | 289 | 318 | 180 | 325 | 348 |
Several studies have used the CGRN classification for the categorization of childhood glaucoma. Bouhenni et al.[4] conducted a study in Akron, Ohio. The study included 108 patients diagnosed with childhood glaucoma or glaucoma suspects from 2008 through 2018. Males represented 64% of the whole cohort. The authors found that glaucoma suspect was the most prevalent category in their study (46%). The authors surmise that this is likely because the study was conducted at a tertiary care pediatric glaucoma center, where a significant number of glaucoma suspects are referred to. PCG was diagnosed in only 3% in this study, which the authors attribute to the fact that most patients with PCG were referred to other, larger ophthalmology clinics in the area.
Another study conducted by Mokbel et al.[6] in Mansoura Ophthalmic Center in Dakahelia, Egypt. They included 207 glaucoma patients (305 eyes) who have been seen at their institute over the period of 4 years. They reported that males represented 63.8% and that PCG was the predominant glaucoma category (55.1%). The authors attribute this to the high rate of consanguineous marriages in this population. In addition, the second most common category in this study was acquired glaucoma, with the majority of these cases being due to a traumatic hyphema.
Lopes et al.[8] conducted a retrospective study in Sao Paulo, Brazil including all patients seen in childhood glaucoma clinic from 2010 through 2018. They found that the majority of patients with childhood glaucoma were males (56.6%) similar to other studies. PCG was the most prevalent category (43.95%) and the JOAG was the least common category being diagnosed in only 2 cases. Glaucoma suspects represented only 13.3% of the whole cohort.
Senthil et al.[9] conducted a study in Hyderabad, India including 275 patients (449 eyes). These authors also found that PCG was the most common category in their patient population representing 37.64%. These authors noted that PCG in Asian children tends to present earlier than in other ethnicities. These authors also found that steroid-induced and traumatic glaucoma were the most common causes of secondary glaucoma.
Whereas Surukrattana et al.[12] conducted a study in Thailand including 423 patients (691 eyes) and found that glaucoma associated with non-acquired ocular anomalies was the most common subtype (22.9%) followed by PCG (20.8%). The condition mostly affected boys, with the majority being bilateral cases.
On the other hand, a retrospective study conducted by Tam et al.[5] evaluated the etiology of childhood glaucoma in 246 patients (373 eyes) referred to a tertiary care center in Boston, MA. They reported that GFCS was the most common subtype of childhood glaucoma (36.5%), followed by PCG (29%).
Conclusion:
The CGRN system was developed as an international consensus classification for childhood glaucoma. It allows for consistent treatment guidelines to be instituted, which can provide streamlined and consistent care for children with glaucoma. Developing a classification system can also enable the acquisition of data for multicenter research studies. Classifying patients into one of the 7 categories ensures that each patient meets one and only one classification, without overlap.
References:
- ↑ Marchini G, Toscani M, Chemello F. Pediatric glaucoma: current perspectives. Pediatric Health Med Ther. 2014;5:15-27
- ↑ Gilbert C, Foster A. Childhood blindness in the context of VISION 2020--the right to sight. Bull World Health Organ 2001;79(3):227-32.
- ↑ 3.0 3.1 3.2 Thau A, Lloyd M, Freedman S, et al. New classification system for pediatric glaucoma: implications for clinical care and a research registry. Curr Opin Ophthalmol 2018;29(5):385-94
- ↑ 4.0 4.1 Bouhenni RA, Ricker I, Hertle RW. Prevalence and Clinical Characteristics of Childhood Glaucoma at a Tertiary Care Children's Hospital. J Glaucoma 2019;28(7):655-9
- ↑ 5.0 5.1 Tam EK, Elhusseiny AM, Shah AS, et al. Etiology and outcomes of childhood glaucoma at a tertiary referral center. Journal of American Association for Pediatric Ophthalmology and Strabismus 2022
- ↑ 6.0 6.1 Mokbel TH, El Hefney EM, Hagras SM, et al. Childhood glaucoma profile in Dakahelia, Egypt: a retrospective study. Int J Ophthalmol 2018;11(4):674-80
- ↑ Hoguet A, Grajewski A, Hodapp E, Chang TC. A retrospective survey of childhood glaucoma prevalence according to Childhood Glaucoma Research Network classification. Indian J Ophthalmol 2016;64(2):118-23
- ↑ 8.0 8.1 Lopes NL, Gracitelli CPB, Rolim-de-Moura C. Childhood Glaucoma Profile in a Brazilian Tertiary Care Center Using Childhood Glaucoma Research Network Classification. J Glaucoma 2021;30(2):129-33
- ↑ 9.0 9.1 Senthil S, Badakere S, Ganesh J, et al. Profile of childhood glaucoma at a tertiary center in South India. Indian J Ophthalmol 2019;67(3):358-65.
- ↑ Knight LSW, Ruddle JB, Taranath DA, et al. Childhood and Early Onset Glaucoma Classification and Genetic Profile in a Large Australasian Disease Registry. Ophthalmology. 2021;128(11):1549-1560.
- ↑ El Sayed YM, Elhusseiny AM, Esmael AF, Gawdat GI, Elhilali HM. Childhood glaucoma profile in a tertiary centre in Egypt according to the childhood glaucoma research network classification. Annual meeting of American Association of Pediatric Ophthalmology and Strabimus (AAPOS) 2022, Scottsdale, AZ.
- ↑ 12.0 12.1 Surukrattanaskul S, Suvannachart P, Chansangpetch S, Manassakorn A, Tantisevi V, Rojanapongpun P. Characteristics and long-term outcomes of childhood glaucoma: a retrospective-cohort study. F1000Research. 2022. Vol 10 165. DOI:10.12688/f1000research.51256.2