Descemet Stripping Endothelial Keratoplasty
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Surgical Therapy
Descemet Stripping Endothelial Keratoplasty (DSEK) and Descemet Membrane Endothelial Keratoplasty (DMEK)
Background
Corneal transplantation is a widely practiced surgical procedure. Over the past decade, lamellar techniques have been developed to replace penetrating keratoplasty (PK) [1] . Endothelial Keratoplasty (EK) has been adapted as an alternative in the treatment of corneal endothelial disorders. [2] In the various forms of endokeratoplasty, Descemet membrane and the endothelium are replaced, with or without a varying amount of corneal stroma. [3][4][5]
In Descemet stripping endothelial keratoplasty (DSEK), the patient’s Descemet membrane is peeled off, using specially designed strippers [4] and replaced with a partial thickness graft: a transplanted disc of Posterior Stroma, Descemet and Endothelium (10-30 % of the inner donor cornea). Both donor and host cornea are manually dissected. Differently, in Descemet’s stripping automated endothelial keratoplasty (DSAEK) the donor dissection is carried out using a mechanical microkeratome.[5] In Descemet membrane endothelial keratoplasty (DMEK) ,[5] the donor tissue placed (after stripping of the patient's Descemet membrane and endothelium) consists of only Descemet membrane and endothelium (no stroma).[5][6] In Descemet membrane automated endothelial keratoplasty (DMAEK), the donor dissection is carried out mechanically, not manually.[7]
Goal
Endothelial keratoplasty is intended to transplant a healthy endothelial cell layer that will pump the fluid out of the cornea. It’s expected to restore corneal clarity and improve vision. [5] This procedure corrects corneal endothelium failure, but is not able to correct corneal scarring, thinning or surface irregularity.
Patient Selection
Indications
Not all patients with corneal pathology are candidates for EK. The indication depends on decreased vision related to corneal swelling from poorly functioning endothelium. The main indications are:
- Acquired Pseudophakic or Aphakic bullous keratopathy, Failed previous graft.
- Inherited Fuchs' Endothelial Dystrophy
The ideal time to perform EK to prevent permanent change is unclear. However, early DSEK has been shown to influence visual outcomes in pseudophakic corneal edema [8] There is a significant relationship between Cataract Extraction to DSEK time and Best Spectacle Corrected Visual Acuity. Performing earlier (<6 M) DSEK for pseudophakic corneal edema appears to be associated with improved visual outcomes. [8]
Surgical Technique
Endothelial keratoplasty (surgical times vary depending on technique and experience) is done under local or general anesthesia. [5] Donor tissue preparation varies depending on the technique of endothelial keratoplasty surgery planned (DSEK, DSAEK, DMEK, DMAEK).
There have been major developments in the surgical techniques of endothelial keratoplasty as well as in donor preparation over the last few decades.[9][10][11][12][13]
After the surgery, the patient lies in a supine position, flat, facing the ceiling, to allow the retained air bubble to further stabilize the graft position, and evaluated prior to discharge to ensure there is no sign of pupillary block related to the air bubble and to confirm that the donor tissue is in good position. [12]
Postoperative care includes broad-spectrum topical antibiotics to prevent infection and topical steroids to treat inflammation and prevent rejection. [10] The patient is instructed to lay supine so that the air bubble helps keep the graft in position during the post-operative period (with intermittent breaks until the air bubble is reabsorbed to avoid pupillary block). The patient is also advised to avoid rubbing their eye (which could dislodge the donor graft). [12]
Advantages and Challenges
DSEK Procedure Advantages
Over PK:
- Less Invasive, smaller surgical incisions
- No corneal-graft sutures
- Faster visual recovery
- Less risk of sight threating complications and less induced astigmatism
- Post-surgery stronger eye (less prone to injury)
- Less risk of immune rejection of the transplanted corneal tissue
- Shorter post-operative care
DSEK itself:
- Increase overall donor tissue availability [2], using the posterior layer of the donor cornea in one patient and the anterior lamellar graft in another patient.
- Faster to learn. DMEK Surgical technique may require more training, technically more challenging. [2]
DSEK Procedure Challenges
Compared with DMEK:
- Final Best Corrected Visual Acuity (BCVA) may be suboptimal . [2][14] Optical irregularities due to stromal layers being transplanted in DSEK. For nano-thin DSEK, final BCVA was comparable to DMEK, demonstrating the significance of thinner donor graft preparation. [15]
- Slower visual rehabilitation compared to DMEK. [2] However, visual recovery is expedited with use of thinner corneal grafts. [11]
- Interface problems, folds in the donor disk from maladaptation to the recipient stroma, hyperopic shift, decentration of the donor disk, and excess donor corneal thickness. [16]
- DSEK grafts are less likely to require rebubbling procedures. [14]
DSEK itself:
- Limited accessibility (investments in equipment)
- Drop in Donor endothelial cell density in the early post-operative phase. [2]
Complications
- Graft Dislocation: graft moves from its intended position. Dislocation can sometimes be managed with rebubbling in the clinic setting, but may require a return to the operating room. [4] [12]
- Early graft failure: rates differ depending on surgical technique and experience and also technique of donor tissue preparation. A study in the US which looked records from 6 major eye banks in the US from Jan 1, 2013 to Dec 31, 208, reported the total percentage of early graft failure for DMEK at 1.18% and for DSAEK was 0.86%. They found that the early failure rate for DMEK was lower for cases in 2018 (0.68%) than in 2013 (7.69%), and suggesting that surgical learning curve may explain the decrease over time.[17]
- Graft Rejection: Rejection can develop months or years after the transplant. Against PK, initial rejection symptoms after DSEK procedure are usually subtle. Patients can be asymptomatic. When patients show redness, blurry vision and light sensitivity the rejection is severe. To prevent rejection patients should be under a closed follow-up care and kept on a prophylactic tapering down eye drop steroids regimen.
- Cell loss: Assessing endothelial cell density (ECD) after DSEK, an expected a median cell loss of 32% in the perioperative period, has been reported, and then the ECD declines at a linear rate of approximately 110 cells/mm2 per year between 6 months and 10 years after DSEK [18]. Gradual reduction in endothelial cell density over time can lead to loss of clarity and require repeating the procedure.
Follow up care
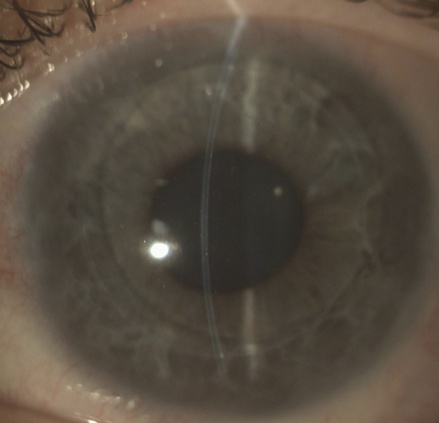
- Slit lamp biomicroscopy: to ensure that the graft is fully attached and to look for signs of rejection (scattered keratic precipitates, edema or conjunctival hyperemia). Fig. 1.
- Check IOP: monitor for steroid-induced pressure spikes.
- Check refraction after first month.
- Check central corneal thickness: a graft that is getting thicker over time may be failing and a graft that gets thicker suddenly signals rejection.
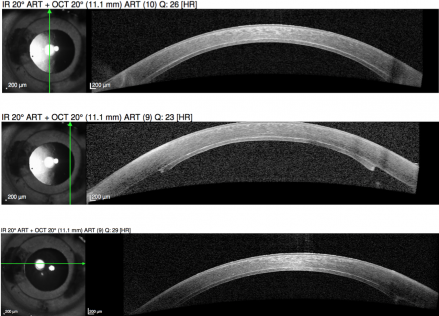
- Graft detachment: Anterior segment OCT can assess for graft detachments. Fig. 2. If the graft is detached, it will need to be reattached by rebubbling the anterior chamber. Since the graft has been in aqueous fluid, it often works well after reattachment. [19]
Conclusion
Endothelial keratoplasty procedures and donor tissue preparations techniques have seen major advancements over the last few decades. A metaanalysis published in 2018 [20] which looked at descemet stripping automated endothelial keratoplasty versus descemet membrane endothelial keratoplasty concluded that while the procedures were similar in safety, visual outcomes were better with DMEK compared to DSAEK. A Cochrane Review published in 2018 found that it was difficult to draw any conclusion regarding endothelial cell loss as two trials demonstrated no difference and two studies reported that DMEK had higher cell counts at one year. [14] However, a more recent study has demonstrated lower endothelial cell loss or secondary graft failure with DMEK compared to DSEK or PK.[21]
Additional Resources
- Boyd K, DeAngelis KD. Iridocorneal Endothelial Syndrome . American Academy of Ophthalmology. EyeSmart/Eye health. https://www.aao.org/eye-health/diseases/iridocorneal-endothelial-syndrome-5. Accessed March 14, 2019.
References
- ↑ Tan DT, Dart JK, Holland EJ, Kinoshita S. Corneal transplantation. Lancet. 2012;379:1749–61.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Dapena I, Ham L, Melles GR. Endothelial keratoplasty: DSEK/DSAEK or DMEK – the thinner the better? Curr Opin Ophthalmol. 2009 Jul;20(4):299-307.
- ↑ Coster DJ, Lowe MT, Keane MC, Williams KA. A comparision of lamellar and penetrating keratoplasty outcomes. Ophthalmology. 2014 May;121(5):979-87.
- ↑ 4.0 4.1 4.2 Bahar I, Kaiserman I, McAllum P, Slomovic A, Rootman D. Comparison of posterior lamellar keratoplasty techniques to penetrating keratoplasty. Ophthalmology. 2008 Sep;115(9):1525-33.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 Stuart AJ, Virgili G, Shortt AJ. Descemet’s membrane endothelial keratoplasty versus Descemet’s stripping automated endothelial keratoplasty for corneal endothelial failure (Protocol). Cochrane Database of Systematic Reviews 2016, Issue 3. Art. No.: CD012097.
- ↑ Kiel M, Bu JB, Gericke A, Vossmerbaeumer U, Schuster AK, Pfeiffer N, Wasielica-Poslednik J. Comparison of DMEK and DSAEK in Eyes With Endothelial Decompensation After Previous Penetrating Keratoplasty. Cornea. 2021 Sep 1;40(9):1218-1224. doi: 10.1097/ICO.0000000000002786. PMID: 34116539.
- ↑ Birbal RS, Sikder S, Lie JT, Groeneveld-van Beek EA, Oellerich S, Melles GRJ. Donor Tissue Preparation for Descemet Membrane Endothelial Keratoplasty: An Updated Review. Cornea. 2018 Jan;37(1):128-135. doi: 10.1097/ICO.0000000000001368. PMID: 28990995.
- ↑ 8.0 8.1 Weissbart SB, Hammersmith KM, Ayres BD, Rapuano CJ, Nagra PK, Raber IM, Azari AA. Influence of Early Descemet Stripping Endothelial Keratoplasty on Visual Outcomes in Pseudophakic Corneal Edema. Am J Ophthalmol. 2016 Dec;172:58-63.
- ↑ Maghsoudlou P, Sood G, Gurnani B, Akhondi H. Cornea Transplantation. 2024 Feb 24. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan–. PMID: 30969512.
- ↑ 10.0 10.1 Liarakos VS, Ham L, Dapena I, Tong CM, Quilendrino R, Yeh RY, Melles GR. Endothelial keratoplasty for bullous keratopathy in eyes with an anterior chamber intraocular lens. J Cataract Refract Surg. 2013 Dec;39(12):1835-45.
- ↑ 11.0 11.1 Tourabaly M, Chetrit Y, Provost J, Georgeon C, Kallel S, Temstet C, Bouheraoua N, Borderie V. Influence of graft thickness and regularity on vision recovery after endothelial keratoplasty. Br J Ophthalmol. 2020 Sep;104(9):1317-1323. doi: 10.1136/bjophthalmol-2019-315180. Epub 2019 Dec 17. PMID: 31848210
- ↑ 12.0 12.1 12.2 12.3 Lindstrom RL, Jhon T. Corneal Endothelial Transplant. First Edition. New Delhi, India. Jaypee Brothers Medical Publishers (P) Ltd. 2010
- ↑ Bethke W. Getting the Most from DSEK and DSAEK. Review of ophthalmology. https://www.reviewofophthalmology.com/article/getting-the-most-from-dsek-and-dsaek. Accessed May 20, 2017
- ↑ 14.0 14.1 14.2 Stuart AJ, Romano V, Virgili G, Shortt AJ. Descemet's membrane endothelial keratoplasty (DMEK) versus Descemet's stripping automated endothelial keratoplasty (DSAEK) for corneal endothelial failure. Cochrane Database Syst Rev. 2018 Jun 25;6(6):CD012097. doi: 10.1002/14651858.CD012097.pub2. PMID: 29940078; PMCID: PMC6513431.
- ↑ Kurji KH, Cheung AY, Eslani M, Rolfes EJ, Chachare DY, Auteri NJ, Nordlund ML, Holland EJ. Comparison of Visual Acuity Outcomes Between Nanothin Descemet Stripping Automated Endothelial Keratoplasty and Descemet Membrane Endothelial Keratoplasty. Cornea. 2018 Oct;37(10):1226-1231. doi: 10.1097/ICO.0000000000001697. PMID: 30028748.
- ↑ Villarrubia A, Cano-Ortiz A. Development of a nomogram to achieve ultrathin donor corneal disks for Descemet-stripping automated endothelial keratoplasty. J Cataract Refract Surg. 2015 Jan;41(1):146-51.
- ↑ Fliotsos MJ, Campbell JA, Li X, Engstrom MB, Stoeger CG, McClory C, Titus MS, Johnson P, Johnston KB, Fischer T, Brooks LK, Montoya MM, Glasser DB, Akpek EK, Srikumaran D. Trends in Early Graft Failure Leading to Regrafting After Endothelial Keratoplasty in the United States. Cornea. 2022 Jul 1;41(7):833-839. doi: 10.1097/ICO.0000000000002831. Epub 2021 Aug 5. PMID: 34369391; PMCID: PMC8818059.
- ↑ Price MO, Calhoun P, Kollman C, Price FW Jr, Lass JH. Descemet Stripping Endothelial Keratoplasty: Ten-Year Endothelial Cell Loss Compared with penetrating Keratoplasty. Ophthalmology. 2016 Jul;123(7):1421-7.
- ↑ Karmel M. Postop DSEK: Comprehensive Ophthalmologists Take the Wheel. EyeNet Magazine.https://www.aao.org/eyenet/article/postop-dsek-comprehensive-ophthalmologists-take-wh. Accessed May 20, 2017.
- ↑ Zhu L, Zha Y, Cai J, Zhang Y. Descemet stripping automated endothelial keratoplasty versus descemet membrane endothelial keratoplasty: a meta-analysis. Int Ophthalmol. 2018 Apr;38(2):897-905. doi: 10.1007/s10792-017-0533-3. Epub 2017 Apr 17. PMID: 28417337.
- ↑ Price MO, Kanapka L, Kollman C, Lass JH, Price FW Jr. Descemet Membrane Endothelial Keratoplasty: 10-Year Cell Loss and Failure Rate Compared With Descemet Stripping Endothelial Keratoplasty and Penetrating Keratoplasty. Cornea. 2024 Nov 1;43(11):1403-1409. doi: 10.1097/ICO.0000000000003446. Epub 2023 Dec 20. PMID: 38128100.