Laser Peripheral Iridotomy
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Introduction
Laser peripheral iridotomy (LPI) (also described as laser iridotomy or simply termed iridotomy) is a medical procedure that uses a laser device to create a hole in the iris, thereby allowing aqueous humor to traverse directly from the posterior to the anterior chamber and, consequently, relieve a pupillary block.[1][2][3] It is commonly used to treat a wide range of clinical conditions, encompassing primary angle‐closure glaucoma, primary angle closure (narrow angles and no signs of glaucomatous optic neuropathy), patients who are primary angle‐closure suspects (patients with reversible obstruction), and even eyes with secondary causes of iridocorneal angle closure.[1]
The first report of an effective surgical treatment for glaucoma was made in 1857 by the German ophthalmologist Albrecht von Graefe, who described the execution of a broad-sector surgical iridectomy through a corneal wound.[4]
However, since the emergence of laser technology in the field of ophthalmology, LPI has largely surpassed the former technique. In the mid-1970s, argon laser became the first to be routinely used to perform a noninvasive iridotomy.[5][6][7] Although the energy is well absorbed by iris pigment, argon laser (and Nd:YAG-KTP laser, which is often referred to as argon laser) iridotomy alone was associated with some complications and relatively high failure and subsequent closure rates.[5][8][9] Q-switched Nd:YAG laser (YAG laser 1064 nm) devices surfaced in the 1980s and were demonstrated to be effective in light-colored irides because the mechanism of action was independent of the melanin content of the iris. Furthermore, it required considerably less total energy than pure argon/Nd:YAG-KTP 532 nm laser iridotomy, achieved a superior rate of single-treatment success with lower risk of subsequent closure, and was less likely to cause damage to the cornea, lens, and retina.[3][5][10][11][12]
Indications
Laser peripheral iridotomy is indicated to prevent or overcome a suspected relative pupillary block by creating an alternative pathway for aqueous flow. Mainly used for patients in the primary angle-closure spectrum, it can also be useful in secondary angle-closure glaucoma and in the management of other types of glaucoma with associated pupillary block. The iridocorneal angle should be, in all cases, carefully examined after LPI to rule out other mechanisms of a closed angle requiring treatment.[13]
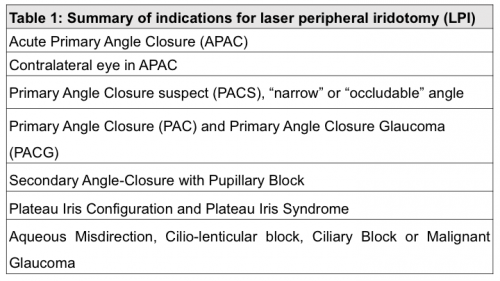
Indications for LPI include those in table 1 and are further described below.
Acute Primary Angle Closure
The benefit of LPI is well established to treat and prevent an acute angle-closure (AAC) crisis. The technique is usually performed soon after the diagnosis is made to prevent irreversible vision loss and prevent a recurrent AAC episode. It is essential to perform LPI in the fellow eye when indicated.[2][3] Before LPI is performed, however, patients experiencing acute primary angle closure (APAC) should receive aqueous suppressants to lower the intraocular pressure (IOP), relieve symptoms, and improve cooperation and visualization of the ocular media in order to safely and effectively apply the laser beam.[2][3][5] In conclusion, LPI associated with medical treatment is the preferred definitive treatment of acute angle-closure glaucoma with a pupillary block mechanism.[1]
Contralateral Eye in Acute Primary Angle Closure
The fellow eye of a patient with an AAC crisis should be evaluated because it is at high risk for a similar event, which can occur within days of the first episode.[2] LPI is indicated in gonioscopically proven occludable angles after an AAC episode as 50% of patients will experience a second attack in the fellow eye over a 5-year period.[1][2][14][15] The risk is significantly reduced if an iridotomy or iridectomy is performed in this eye.[2][16]
Primary Angle-Closure Suspect, “Narrow” or “Occludable” Angle
These eyes feature at least 2 quadrants of iridotrabecular contact (ITC) but normal IOP, no peripheral anterior synechiae (PAS), and no evidence of glaucomatous optic neuropathy or visual field defects. Observational studies suggest that the majority of these eyes will not develop either primary angle closure or primary angle-closure glaucoma.[2][17] All cases of primary angle-closure suspect (PACS) must be assessed individually. In general, the treatment complications are to be balanced against the perceived risk of angle closure.[1][2][5] The ZAP trial[18] demonstrated a small but significant prophylactic effect of LPI in these cases; however, the widespread use of prophylactic LPI for PACS or “occludable angles” is not recommended. Therefore, some authors defend that following such patients without treatment is a safe option.[2][19]
Primary Angle Closure and Primary Angle-Closure Glaucoma
Iridotomy is strongly recommended in eyes with primary angle closure (PAC) or primary angle-closure glaucoma (PACG).[1][2][20] PAC patients may have elevated IOP from chronic compromise of aqueous outflow. Chronic angle-closure glaucoma features permanent synechial closure of any extent as confirmed by indentation gonioscopy.[1] Medical treatment alone is contraindicated as all patients require relief of pupil block by iridotomy, iridectomy, or lens extraction. If the peripheral anterior synechiae occupy less than 50% of the circumference, iridectomy or iridotomy may suffice. Because complications of laser iridotomy are uncommon, its use as the initial procedure is justified in practically every case, as soon as the corneal transparency allows the LPI to be performed. If IOP remains uncontrolled after LPI, a filtering surgery should be considered as the next step.[1] However, in asymptomatic (chronic) angle closure, a high presenting pressure (>35 mm Hg), more than 6 clock hours of PAS, and/or established glaucomatous optic neuropathy are signs that the angle closure will not respond fully to LPI and surgical treatment may be needed to reach the IOP goal.[1]
Secondary Angle-Closure Mechanisms
Uveitis is a common cause of secondary pupillary block, and laser iridotomy may be required to prevent recurrence of pupillary block. Pupillary block can also develop slowly with a senile cataract or rapidly with dislocated or subluxated lenses, or with swollen post-trauma lenses. Iridotomy may not be curative but helps by relieving the pupillary block component, allowing for safer lensectomy. Pupillary block can occur in pseudophakic eyes, more often with anterior chamber lenses if an iridectomy is absent or occluded.[1][3][5]
Other Indications
Pigmentary Dispersion Syndrome, Pigmentary Ocular Hypertension, and Pigmentary Glaucoma
In pigmentary dispersion syndrome (PDS), the principle supporting LPI is to equalize the pressure between the anterior and posterior chamber so as to reduce the posterior concavity of the iris. This would allow for reduced friction between the iris and zonular fibers and reduce or eliminate pigment dispersion.[1][2][21][22] Nd:YAG LPI has been proposed as a means for eliminating a reverse pupillary block, although the benefit from LPI in patients with PDS, pigmentary ocular hypertension (POH), and pigmentary glaucoma (PG) is not yet established. However, LPI has been demonstrated to decrease the biomechanical factor of iris-zonule contact, which may prove to be beneficial to patients before the onset of trabecular dysfunction. There is insufficient high-quality evidence on the effectiveness of peripheral iridotomy for PG or PDS and, therefore, the long-term effects on visual function and other patient-important outcomes have not been established. In pigmentary glaucoma, this procedure is usually not recommended because there is already an optic neuropathy which can progress with IOP spikes after LPI.[21][22]
Plateau Iris Configuration and Plateau Iris Syndrome
Plateau iris configuration refers to a specific condition in which eyes have iridotrabecular contact after iridotomy, with close apposition of the peripheral iris to the angle on gonioscopy and a deep central anterior chamber.[1][2] On pupil dilation, these eyes do not experience a significant increase of IOP as opposed to eyes with plateau iris syndrome, which experience an IOP spike in this scenario and may require more extensive treatments. About one-third of eyes with primary angle closure treated with LPI have an angle that retains significant ITC.[2][23] LPI should be performed in every eye suspected of having a plateau iris configuration because it eliminates any pupillary block component.[1][2] These eyes present a thicker iris and an anteversion of the ciliary body, and these anatomical factors predict failure of a laser iridotomy to open an appositionally closed angle.[2][5] The long-term risk of PACG in eyes with plateau iris configuration does not appear to be higher than in eyes whose angles widen more after LPI.[2]
Aqueous Misdirection, Cilio-lenticular Block, Ciliary Block, or Malignant Glaucoma
Aqueous misdirection is a challenging form of secondary angle closure that presents with elevated IOP and shallowing of the central and peripheral anterior chamber caused by anterior rotation of the iris and ciliary body, occurring classically in the postoperative period. This clinical entity is a diagnosis of exclusion; therefore, LPI is important because it eliminates the possibility of a pupillary block mechanism in ciliary block glaucoma.[1]
Congenital Anomalies Potentially Associated With Secondary Glaucoma
The following conditions can be associated with secondary glaucoma: familial iris hypoplasia, anomalous superficial iris vessels, aniridia, Sturge-Weber syndrome, neurofibromatosis, Marfan syndrome, Pierre Robin syndrome, homocystinuria, goniodysgenesis, Lowe syndrome, microcornea, microspherophakia, rubella, broad thumb syndrome, and persistent hyperplastic primary vitreous. Laser iridotomy and surgical iridectomy are not effective.[1]
Systemic Drugs That Affect Iridocorneal Angle
A wide range of systemic drugs (eg, topiramate, methylphenidate, selective serotonin reuptake inhibitors, tricyclic antidepressants) have been implicated in case reports with angle closure; however, these eyes pose added difficulties in the decision-making process because the pretreatment gonioscopy findings alone are not enough to rule out such risk. It is sensible to repeat the gonioscopy in eyes with narrow angles whenever these drugs are initiated. The role of prophylactic LPI in this patient population should be weighed against the risk of angle closure or of withdrawal of these drugs.[1][2]
Postoperative reverse pupillary block
One of the indications for YAG iridotomy is the management of postoperative reverse pupillary block, a condition observed following cataract surgery, particularly in myopic patients with IOL fixation using the Yamane technique[24]. It has also been reported after uncomplicated surgery with a single-piece IOL in the bag[25]. Affected patients typically present with elevated IOP, ocular pain, decreased vision, with or without pigment dispersion[26][27][25], along with a widely open angle and significant iris-IOL contact. YAG iridotomy effectively treats this condition, leading to normalization of intraocular pressure and restoration of the iris position[24][25][27]
Contraindications
The following contraindications should be managed prior to performing LPI:[2][3][5]
- Ocular media opacities (eg, corneal edema, anterior chamber inflammation)
- High-risk eyes (eg, very shallow or flat anterior chambers, uveitis)
- Uncooperative patients
Preoperative Management
The following recommendations should be followed to safely and effectively perform LPI:[1][2][5][20]
- Apply pilocarpine 2%-4% to cause miosis, reduce iris thickness, and facilitate perforation.
- In the presence of corneal edema, use topical glycerin 10% if available, systemic acetazolamide, intravenous mannitol, or oral hyperosmotic agents.
- IOP-lowering drugs: To prevent IOP spikes after the procedure, use a topical alpha-2 agonist (brimonidine or apraclonidine) 1 hour prior to the procedure and immediately afterward. In the setting of AAC, IOP should be controlled beforehand with medical treatment.
- Apply topical anesthesia (eg, oxybuprocaine).
- Apply the iridotomy lens (eg, Abraham [+66 D], Wise [+103 D], or CGI LASAG CH lens) to the eye with coupling gel. The use of the lens keeps the eyelids open, minimizes eye movement, provides magnification, and improves visualization, reducing the risk of corneal burns and simultaneously increasing the power density by concentrating the laser energy.
- Focus: Set defocus to zero; focus first on the iris surface and then offset the YAG beam so that it converges slightly posteriorly in the stroma. A bubble of plasma travels toward the surgeon so it is safer to have the focal point within the iris stroma.
- Position of iridotomy: The hole should be created in the iris periphery, aiming for an iris crypt or area of iris thinning, at a site in the superior quadrants between 11 and 1 o’clock, which allows the lesion to be covered by the upper eyelid, avoiding the 12 o'clock position as air bubbles may occlude the iridotomy. Avoid iris vessels. If silicone oil (except high-molecular-weight silicone) or other tamponading fluids or gases present, perform an inferior LPI.
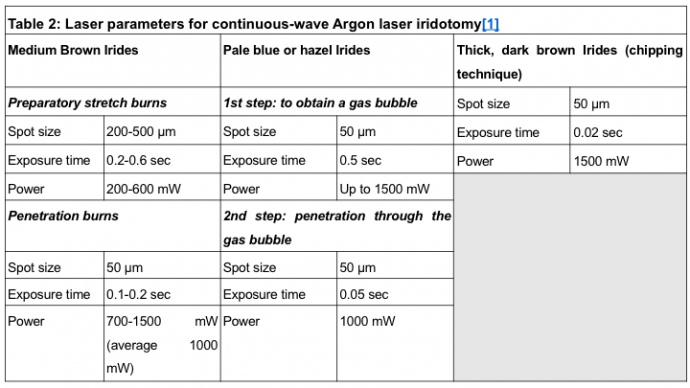
- Parameters: Consult tables 2 and 3.
- Endpoint: A small (150- to 200-micrometer), peripheral, and completely patent iridotomy is the ideal result. Whole-thickness perforation of the iris is assumed when pigment, mixed with aqueous, flows from the posterior into the anterior chamber. Once a full-thickness hole has been made, it should be enlarged horizontally to achieve an adequate size. Iridotomy size should be sufficient for patency in spite of iris edema, pigment epithelial proliferation, and pupil dilation. Transillumination through the iridotomy is not a reliable indicator of patency.
- Postoperative medication: Prescribe a topical corticosteroid 3 to 4 times a day for 4-7 days, as well as an IOP-lowering drug.
- Evaluate IOP in 30 minutes to 2 hours following LPI and anterior chamber depth 1 week later to confirm opening of the anterior chamber angle. If the patency is uncertain, check with gonioscopy, reconsider the mechanism, perform ultrasound biomicroscopy (UBM)/anterior segment optical coherence tomography (AS-OCT) if available, and/or repeat the iridotomy.
Types of Lasers for LPI
Iridotomy can be accomplished using the photodisruptive Q-switched Nd:YAG laser (Nd:YAG) or the photothermal Nd:YAG-KTP 532 nm (which is still often called argon laser) and solid-state lasers. The 2 laser types may also be used in sequential combination. Laser parameters should be individualized to each patient and adjusted appropriately during the procedure. Independently of the device used, some authors aim for an iridotomy of at least 200 micrometers in size and ideally 500 micrometers in diameter.[3][5]
Argon/Nd:YAG-KTP 532 nm or Solid-State Laser
Nd:YAG-KTP 532 nm and solid-state lasers produce thermal (coagulative) effects with lower energies at higher exposures or explosive effects (vaporization) if higher energies are used. Unlike Nd:YAG, these lasers require pigment for light energy absorption and therefore need more adjustments and greater variety in techniques and laser parameters to iris pigment density posterior to the stroma. Sequential Nd:YAG-KTP 532 nm/Nd:YAG LPI can be useful in patients with thick brown irides, particularly in East Asian and African populations. Nd:YAG-KTP 532 nm laser pretreatment to thin the iris results in lower energy needed with the Nd:YAG laser, which is then used to penetrate the iris and create an iridotomy. By using only a fraction of the power required for pure YAG laser iridotomy, it is more efficient and carries a lower risk of complications, namely anterior chamber hemorrhage.[3][5]
Nd:YAG Laser
The Q-switched Nd:YAG lasers rely on tissue photodisruption to create a rapidly expanding ionic plasma wave and thus are efficient in all iris colors. The subsequent shock wave and mainly cavitation bubble will, in turn, mechanically burst through the stromal tissue. The Nd:YAG laser is preferred by many surgeons because it perforates the iris easily, requiring lower energy than Nd:YAG-KTP 532 nm lasers. It is easier to penetrate dark brown irides with these devices because the former have a tendency to absorb too much energy during treatment, and pale irides absorb laser energy poorly. Moreover, Nd:YAG iridotomies may be less likely to close over time.[1][3][5][9][28]
Complications
Transient Increase in IOP
Acute-onset IOP elevation is the most common postoperative complication following LPI. It is usually transient, occurring most frequently in the first 4 hours after treatment. An increase of at least 8 mm Hg from baseline has been reported in 6% to 10% of patients and an IOP superior to 21 mm Hg in 2% to 72%.[1][29] Its occurrence as a primary event is thought to be caused by obstruction of the trabecular meshwork by released blood, iris pigment, and other debris.[5] Plateau iris syndrome or other nonpupillary block angle-closure mechanism, inflammation, extensive PAS, and prolonged corticosteroid therapy are possible secondary causes of IOP elevation postprocedure. Prophylaxis with pressure-lowering agents is an effective strategy to prevent IOP rise after the procedure.[1][12]
Anterior Chamber Bleeding
Anterior chamber bleeding, or hyphema, is a common complication after LPI. It refers to bleeding from the iridotomy site, is minor in most cases, and can usually be stopped by light pressure applied to the eye with the contact lens. The incidence and severity of anterior chamber bleeding has been reported to be similar whether the patient was on or off antithrombotic therapy (ie, aspirin, clopidogrel, warfarin) and between groups taking different antithrombotic medications. Therefore, antiaggregants and anticoagulants need not be discontinued before LPI, and specific patients may have a bleeding diathesis regardless of the medications taken.[29][30][31]
Visual Dysphotopsias
Visual symptoms are uncommon but known to occur after the procedure, including blurring, glares, halos, lines, spots, and shadows at a reported rate of 2% to 16%.[29] Symptom rates according to LPI location are mixed across large studies. The practice of placing LPI at the 10-2 o’clock position to prevent dysphotopsia illustrates how anatomical reasoning can lead us astray. While it seems logical that hiding the iridotomy behind the upper lid would reduce visual symptoms, systematic study of patient outcomes fails to support this assumption. A systematic review of 1,756 eyes from 878 patients compared the incidence of dysphotopsia based on LPI location (superior, inferior, or nasal/temporal). The analysis found no significant difference in the incidence of dysphotopsia among the location groups. Overall, the incidence of linear dysphotopsia was 2% to 3% regardless of LPI placement. Interestingly, the review also noted that LPI could resolve preexisting halos and glare, suggesting that the procedure may have some beneficial effects on visual symptoms.[32] Although Spaeth et al[33] report dysphotopsia symptoms after LPI in 9% of eyes with completely covered, 26% with partially covered, and 17.5% with fully exposed iridotomies, a large trial by Srinivasan et al reported no statistical difference of new visual symptoms according to LPI location (superior versus nasal or temporal) 2 weeks after LPI.[34] The same group also found that the majority of visual symptoms were likely to resolve after 6 months of follow-up, which may indicate that patients adapt or learn to ignore them.[35] Finally, temporal LPI has been reported to cause less visual symptoms than superior LPI.[29][36] Therefore, patients complaining of new-onset visual symptoms post-LPI can be reassured that improvement of symptoms may occur over time without active intervention. Tinted lenses have been used to relieve visual symptoms.[3]
Cataract Progression
The risk of a traumatic cataract has been reported to be increased in post-LPI subjects at follow-up periods ranging from 12 months to 6 years,[11][29][37][38] and case reports of posterior subcapsular cataracts after LPI may be found in the literature.[3] Postulated mechanisms include direct damage to the crystalline lens, altered aqueous fluid dynamics, and mild inflammatory changes to the iris which may induce metabolic changes that accelerate cataract formation.[5]
Iridotomy Closure and Need for Repeat LPI
Closure of the iridotomy has been reported to occur at a rate from 1% at 2 weeks to 20% within the first 6 months after the procedure, but the vast majority of iridotomies may remain patent years after the procedure.[29][39][40] Closure can occur due to accumulation of debris and pigment granules, although complete closure of the iridotomy is unusual with Nd:YAG lasers. Repeat LPI can be performed at the same site immediately after the first procedure or a few hours later if debris impedes the observation of the iridotomy or creating an iridotomy at another site.
Aqueous Misdirection Syndrome
In rare cases, aqueous misdirection can complicate the management of primary angle closure. This may occur following laser iridotomy and other surgical procedures. Forward movement of the lens iris diaphragm causes secondary angle closure resulting in IOP elevation. These cases typically have very small eyes (axial length <21 mm) and higher hypermetropic refraction (> +6 D). It is believed that the ciliary processes come into contact with the lens equator, and/or a firm zonule/posterior capsule diaphragm, causing misdirection of aqueous into the vitreous.[1] Malignant glaucoma is a rare complication of laser iridotomy and should be considered in eyes with progressive anterior chamber shallowing and myopia despite normal IOP.
Other Complications
A reduction in endothelial cell count after LPI has been reported in the literature.[12][29] Postoperative inflammation is usually transient and mild, rarely resulting in posterior synechiae. Rare complications include sterile hypopyon, macular hole formation, cystoid macular edema, and retinal hemorrhages.[10][30][41]
Outcomes
IOP Control
The effectiveness of the procedure in controlling the IOP varies according to the staging of the disease, with earlier stages of the angle-closure spectrum reporting the highest success rates, while the prognosis is less favorable after an AAC crisis and even more guarded if glaucomatous optic nerve damage can be demonstrated. In fact, several studies regarding the spectrum of primary angle closure report that 7.1%-28.0% of PACS eyes, 42.4%-80.0% of PAC eyes, and 83.3%-100% of PACG eyes required additional medical and/or surgical intervention after LPI.[5][42][43][44] On the other hand, the EAGLE trial, which included PAC and PACG patients, showed that initial treatment with clear lens extraction was superior to LPI with topical medical treatment for participants with an IOP over 30 mm Hg and primary angle closure or primary angle-closure glaucoma, with significantly fewer participants in the clear lens extraction group needing additional treatment to control IOP and fewer glaucoma medications than patients who received standard care. The benefit of clear lens extraction in patients with PAC and an IOP inferior to 30 mm Hg is unclear. Intraocular pressure was better with clear lens extraction than with standard care, with the mean pressure being around 1 mm Hg lower in the clear lens extraction group at 3 years.[29][45]
Anatomical Improvement
The effect of LPI on angle width has been evaluated across studies using a variety of quantitative and qualitative parameters. A large number of studies have demonstrated short-term increases in angle width across the PAC spectrum expressed as an increase in the Shaffer grade and an increase in quantitative angle-width parameters using UBM and AS-OCT.[29] However, 2 prospective studies have demonstrated a gradual and significant decrease in angle width after LPI was performed.[18][46] Baseline anatomical factors associated with persistent angle closure after LPI include the presence of PAS; increased IOP; UBM parameters such as shallower peripheral angle width, thicker iris, and more anteriorly positioned ciliary body; and AS-OCT parameters such as greater mean lens vault and thicker iris. These factors represent a narrower angle before LPI and nonpupillary block mechanisms of angle closure.[29] Indeed, LPI induces significant changes in the 3D anterior segment morphology in primary angle-closure suspect patients with an increase in central anterior chamber depth and anterior chamber volume and widening of the iridocorneal angle with no change in central corneal thickness, IOP, or pupil diameter.[47] LPI is more effective than pilocarpine in widening the iridocorneal angle without significant shallowing of the anterior chamber in eyes with anatomically narrow angles.[48]
Prevention of AAC Crisis
LPI has been shown in trials to prevent recurrent attacks of acute angle closure, with an effectiveness and safety equal to that of surgical iridectomy, and with better acceptability to patients.[49] Good effectiveness in preventing acute attacks in fellow eyes has also been reported.[16] Nonetheless, isolated reports do exist of eyes experiencing a recurrent acute attack after LPI.[3][50] In AAC, laser iridotomy relieves the attack in most cases. Superior outcomes have been reported in Caucasian eyes compared to Asian eyes.[3] In AAC attacks, a significant amount of PAS, higher presenting IOP, longer attack duration, poor initial response to therapy (<30% IOP), and larger cup-disc ratio have been associated with inadequate long-term IOP control after LPI. These findings are consistent with a more severe disease affecting the ITC and the trabecular meshwork.[2][3][29]
Disease Progression
Progression from PACS to PAC was based on the development of PAS or elevated IOP. Progression from PACS or PAC to PACG was defined using both structural (disc appearance) and functional (visual field) criteria in most studies.[2] In the EAGLE cohort, visual acuity outcomes in the clear lens extraction group were similar to those in the LPI group.[51] In the EAGLE trial, clear lens extraction was superior to LPI in improving visual function. This improvement (eg, contrast sensitivity) may have resulted from eliminating mild age-related changes in lens transparency, and by correction of refractive error, which caused an improvement in good visual acuity without the need for spectacles. While this magnitude of change is unlikely to be clinically important, it points to the overall improvement in visual function associated with clear lens extraction. A recent systematic review found insufficient evidence based on randomized controlled trials as to whether iridotomy slows progression of visual field loss at 1 year compared to no iridotomy.[52]
Summary
LPI is an integral component in the management of PAC. Although LPI has been available since the 1970s, its role in the treatment algorithm for PAC is still under debate; questions such as who should be treated with an iridotomy and whether iridotomy prevents disease progression continue to be relevant today.[2] After LPI, most PACS subjects can expect to receive no further treatment. On the other hand, many PAC and APAC eyes, and most PACG eyes, need additional treatment to control IOP. LPI has a favorable effect on IOP, especially when extensive synechial closure or glaucomatous nerve damage has not occurred. Factors predictive for IOP elevation, or the need for further treatment after LPI, were those reflective of worse disease at baseline, such as higher IOP, greater cup-disc ratio, and greater synechial closure at presentation.[2] The safety and effectiveness of LPI for PAC/PACG has promoted a gradual widening of the criteria for iridotomy during the past couple of decades. However, more inclusive criteria spurred the debate over treatment algorithms, as we still do not know which eyes will develop glaucomatous damage, despite early manifestations of narrow angles, and offering iridotomy too soon would expose healthier patients to complications without clear evidence of benefit.[5] More recently, the role of cataract extraction in the PAC disease spectrum has continued to fuel debate around LPI timing and its indications. In fact, the EAGLE trial recommends clear lens extraction as first-line treatment for the subset of PAC patients with an IOP over 30 mm Hg. Newer and more objective angle imaging devices are expected to contribute toward predicting the success of laser iridotomy in the future.[2][5][45]
In conclusion, LPI increases angle width in all stages of PAC and has a favorable effect on IOP in eyes without extensive angle or disc damage. Although there is a gradual decrease in angle width in PACS eyes after LPI, further treatment after LPI in this subgroup is infrequent. In contrast, additional treatment after LPI is more likely in PAC, APAC, and PACG eyes, and they should be monitored for IOP elevation and progression to glaucoma.[1][2][13]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 European Glaucoma Society terminology and guidelines for glaucoma, 4th edition---part 1: supported by the EGS Foundation. Br J Ophthalmol. 2017;101(4):1-72.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 2.23 2.24 Prum BE Jr, Herndon LW Jr, Moroi SE, et al. Primary Angle Closure Preferred Practice Pattern guidelines. Ophthalmology. 2016;123(1):P1-P40.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 Lam DSC, Tham CCY, Congdon NG, Baig N. Peripheral iridotomy for angle-closure glaucoma. In: Shaarawy TM, Sherwood MB, Hitchings RA, Crowston JC, eds. Glaucoma. Elsevier; 2015;708-715. doi:10.1016/B978-0-7020-5193-7.00072-8
- ↑ Gräfe A. Ueber die Iridectomie bei Glaucom und über den glaucomatösen Process. Albrecht von Graefes Archiv für Ophthalmologie. 1857;3:456-555. doi:10.1007/bf02720732
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 5.12 5.13 5.14 5.15 5.16 Cruz M. Laser iridotomy. In: Henriques J, Duarte A, Quintão T, eds. Laser Manual in Ophthalmology--Fundamentals and Laser Clinical Practice. Medical Laser Interdisciplinary Portuguese Society; 2017:115-122.
- ↑ Khuri CH. Argon laser iridectomies. Am J Ophthalmol. 1973;76:490-493.
- ↑ Palanker DV, Blumenkranz MS, Marmor MF. Fifty years of ophthalmic laser therapy. Arch Ophthalmol. 2011;129(12):1613-1619. doi:10.1001/archophthalmol.2011.293
- ↑ Quigley HA. Long-term follow-up of laser iridotomy. Ophthalmology. 1981;88:218-224.
- ↑ 9.0 9.1 Robin AL, Pollack IP. A comparison of neodymium:YAG and argon laser iridotomies. Ophthalmology. 1984;91:1011-1016.
- ↑ 10.0 10.1 Berger BB. Foveal photocoagulation from laser iridotomy. Ophthalmology. 1984;91:1029-1033.
- ↑ 11.0 11.1 Vijaya L, Asokan R, Panday M, George R. Is prophylactic laser peripheral iridotomy for primary angle closure suspects a risk factor for cataract progression? The Chennai Eye Disease Incidence Study. Br J Ophthalmol. 2017;101:665-670.
- ↑ 12.0 12.1 12.2 Kumar RS, Baskaran M, Friedman DS, et al. Effect of prophylactic laser iridotomy on corneal endothelial cell density over 3 years in primary angle closure suspects. Br J Ophthalmol. 2013;97:258-261.
- ↑ 13.0 13.1 Glaucoma. International Council of Ophthalmology. Accessed June 1, 2019. http://www.icoph.org/enhancing_eyecare/glaucoma.html
- ↑ Lowe RF. Acute angle-closure glaucoma: the second eye: an analysis of 200 cases. Br J Ophthalmol. 1962;46:641-650.
- ↑ Bain WE. The fellow eye in acute closed-angle glaucoma. Br J Ophthalmol. 1957;41:193-199.
- ↑ 16.0 16.1 Ang LP, Aung T, Chew PT. Acute primary angle closure in an Asian population: long-term outcome of the fellow eye after prophylactic laser peripheral iridotomy. Ophthalmology. 2000;107:2092-2096.
- ↑ Wilensky JT, Kaufman PL, Frohlichstein D, et al. Follow-up of angle-closure glaucoma suspects. Am J Ophthalmol. 1993;115:338-346.
- ↑ 18.0 18.1 Jiang Y, Chang DS, Zhu H, et al. Longitudinal changes of angle configuration in primary angle-closure suspects: the Zhongshan Angle-Closure Prevention Trial. Ophthalmology. 2014;121:1699-1705.
- ↑ Weinreb RN, Moghimi S. Prophylactic laser iridotomy in primary angle-closure suspects. Lancet. 2019;393:1572-1574.
- ↑ 20.0 20.1 Weinreb RN, Friedman DS, eds. Angle Closure and Angle Closure Glaucoma: Reports and Consensus Statements of the 3rd Global AIGS Consensus Meeting on Angle Closure Glaucoma. Kugler Publications; 2006.
- ↑ 21.0 21.1 Michelessi M, Lindsley K. Peripheral iridotomy for pigmentary glaucoma. Cochrane Database Syst Rev. 2016;2:CD005655.
- ↑ 22.0 22.1 Buffault J, Leray B, Bouillot A, Baudouin C, Labbé A. Role of laser peripheral iridotomy in pigmentary glaucoma and pigment dispersion syndrome: a review of the literature. J Fr Ophtalmol. 2017;40(9):e315-e321. doi:10.1016/j.jfo.2017.09.002
- ↑ Kumar RS, Tantisevi V, Wong MH, et al. Plateau iris in Asian subjects with primary angle closure glaucoma. Arch Ophthalmol. 2009;127:1269-1272.
- ↑ 24.0 24.1 Bharathi M, Balakrishnan D, Senthil S. “Pseudophakic reverse pupillary block” following yamane technique scleral-fixated intraocular lens. Journal of Glaucoma. 2020 Jul 1;29(7):e68-70.
- ↑ 25.0 25.1 25.2 Abushanab MM, Solyman O, Sakr AA, Serhan HA. Pseudophakic reverse pupillary block after implantation of a single-piece foldable intraocular lens in the capsular bag: Case report and literature review. Oman Journal of Ophthalmology. 2024 Jan 1;17(1):120-3.
- ↑ Itagaki H, Kunikata T, Hiratsuka K, Saito J, Oshika T. Reverse pupillary block associated with pigment dispersion syndrome after in-the-bag intraocular lens implantation. Journal of Cataract & Refractive Surgery. 2013 Dec 1;39(12):1925-8.
- ↑ 27.0 27.1 Bang SP, Joo CK, Jun JH. Reverse pupillary block after implantation of a scleral-sutured posterior chamber intraocular lens: a retrospective, open study. BMC ophthalmology. 2017 Mar 29;17(1):35.
- ↑ Pollack IP, Robin AL, Dragon DM, et al. Use of the neodymium:YAG laser to create iridotomies in monkeys and humans. Trans Am Ophthalmol Soc. 1984;82:307-328.
- ↑ 29.00 29.01 29.02 29.03 29.04 29.05 29.06 29.07 29.08 29.09 29.10 Radhakrishnan S, Chen PP, Junk AK, Nouri-Mahdavi K, Chen TC. Laser peripheral iridotomy in primary angle closure: a report by the American Academy of Ophthalmology. Ophthalmology. 2018;125:1110-1120.
- ↑ 30.0 30.1 Arunmongkol S, Suwan Y, Supakontanasan W, Nilphatanakorn S, Teekhasaenee C. Eight-ball hyphema after laser iridotomy in a patient with undiagnosed hypocellular myelodysplastic syndrome. Int Med Case Rep J. 2018;11:133-137.
- ↑ Golan S, Levkovitch-Verbin H, Shemesh G, Kurtz S. Anterior chamber bleeding after laser peripheral iridotomy. JAMA Ophthalmol. 2013;131:626-629.
- ↑ Balas M, Mathew DJ. Dysphotopsia and location of laser iridotomy: a systematic review. Eye (Lond). 2024;38(7):1240-1245. doi:10.1038/s41433-023-02913-1
- ↑ Spaeth GL, Idowu O, Seligsohn A, et al. The effects of iridotomy size and position on symptoms following laser peripheral iridotomy. J Glaucoma. 2005;14(5):364-367. doi:10.1097/01.ijg.0000177213.31620.02
- ↑ Srinivasan K, Zebardast N, Krishnamurthy P, et al. Comparison of new visual disturbances after superior versus nasal/temporal laser peripheral iridotomy: a prospective randomized trial. Ophthalmology. 2018;125:345-351.
- ↑ Kavitha S, Ramulu PY, Venkatesh R, et al. Resolution of visual dysphotopsias after laser iridotomy: six-month follow-up. Ophthalmology. 2019;126:469-471.e1.
- ↑ Vera V, Naqi A, Belovay GW, Varma DK, Ahmed IIK. Dysphotopsia after temporal versus superior laser peripheral iridotomy: a prospective randomized paired eye trial. Am J Ophthalmol. 2014;157:929-935.
- ↑ Tan AM, Loon SC, Chew PTK. Outcomes following acute primary angle closure in an Asian population. Clin Experiment Ophthalmol. 2009;37:467-472.
- ↑ Lim LS, Husain R, Gazzard G, Seah SKL, Aung T. Cataract progression after prophylactic laser peripheral iridotomy: potential implications for the prevention of glaucoma blindness. Ophthalmology. 2005;112:1355-1359.
- ↑ Waisbourd M, Shafa A, Delvadia R, et al. Bilateral same-day laser peripheral iridotomy in the Philadelphia Glaucoma Detection and Treatment Project. J Glaucoma. 2016;25:e821-e825.
- ↑ Jiang Y, Chang DS, Foster PJ, et al. Immediate changes in intraocular pressure after laser peripheral iridotomy in primary angle-closure suspects. Ophthalmology. 2012;119:283-288.
- ↑ Tsui JC, Marks SJ. Unilateral stage 1A macular hole secondary to low-energy Nd:YAG peripheral iridotomy. Cureus. 2021;13(1):e12603. doi:10.7759/cureus.12603
- ↑ Peng P-H, Nguyen H, Lin H-S, Nguyen N, Lin S. Long-term outcomes of laser iridotomy in Vietnamese patients with primary angle closure. Br J Ophthalmol. 2011;95:1207-1211.
- ↑ Rosman M, Aung T, Ang LPK, Chew PTK, Liebmann JM, Ritch R. Chronic angle-closure with glaucomatous damage: long-term clinical course in a North American population and comparison with an Asian population. Ophthalmology. 2002;109:2227-2231.
- ↑ Chen M-J, Cheng C-Y, Chou C-K, Liu CJL, Hsu W-M. The long-term effect of Nd:YAG laser iridotomy on intraocular pressure in Taiwanese eyes with primary angle-closure glaucoma. J Chin Med Assoc. 2008;71:300-304.
- ↑ 45.0 45.1 Azuara-Blanco A, Burr J, Ramsay C, et al. Effectiveness of early lens extraction for the treatment of primary angle-closure glaucoma (EAGLE): a randomised controlled trial. Lancet. 2016;388:1389-1397.
- ↑ Lee KS, Sung KR, Shon K, Sun JH, Lee JR. Longitudinal changes in anterior segment parameters after laser peripheral iridotomy assessed by anterior segment optical coherence tomography. Invest Ophthalmol Vis Sci. 2013;54:3166-3170.
- ↑ Mansoori T, Balakrishna N. Anterior segment morphology after laser iridotomy in primary angle closure suspects. Clin Exp Optom. 2018;101:333-338.
- ↑ Mogil RS, Khezri N, Ren R, et al. Changes in iridocorneal angle and anterior chamber structure in eyes with anatomically narrow angles: laser iridotomy versus pilocarpine. J Glaucoma. 2018;27:1073-1078.
- ↑ Schwenn O, Sell F, Pfeiffer N, Grehn F. Prophylactic Nd:YAG-laser iridotomy versus surgical iridectomy: a randomized, prospective study. Ger J Ophthalmol. 1995;4:374-379.
- ↑ Tanasescu I, Grehn F. Acute angle-closure glaucoma despite previous Nd: YAG laser iridotomy: a report on 13 cases. Ophthalmologe. 2003;100:832-835.
- ↑ Day AC, Cooper D, Burr J, et al. Clear lens extraction for the management of primary angle closure glaucoma: surgical technique and refractive outcomes in the EAGLE cohort. Br J Ophthalmol. 2018;102:1658-1662.
- ↑ Le JT, Rouse B, Gazzard G. Iridotomy to slow progression of visual field loss in angle-closure glaucoma. Cochrane Database Syst Rev. 2018;2018(6):CD012270.