Linear Interstitial Keratitis
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Linear Interstitial Keratitis (LIK) is a rare, distinct clinical entity characterized by horizontal linear stromal infiltrates of the cornea. First described in the ophthalmic literature in 1923, this condition predominantly affects young adults and presents with a characteristic linear pattern that may extend from limbus to limbus.[1][2][3]
Etiology
The etiology of LIK remains idiopathic.[1][3][4] Syphilitic infection was historically proposed as a cause; however, serologic tests for syphilis have been negative in reported cases.[1][2] No consistent infectious etiology has been identified despite extensive workup including PCR for HSV and acanthamoeba, as well as bacterial and fungal cultures.
Several clinical features have led authors to suggest an autoimmune etiology, including recurrence inflammation, family history of autoimmune disease in some patients, panstromal involvement on confocal microscopy despite clinically localized disease, consistent response to corticosteroids, and absence of identifiable infectious agents. One case series detected elevated antinuclear antibodies (ANA) in 3 of 4 patients (titers 1:320 to 1:1280); however, rheumatology consultation found no underlying autoimmune disease, and the elevations were ultimately considered of unclear clinical significance.[5]
Epidemiology
LIK is an exceedingly rare condition with limited epidemiologic data available. The majority of reported cases occur in adolescents and young adults.[1][2][3][4] Coop reported the youngest patient at 8 years of age while Barrientos and Wildes reported the oldest patient diagnosed with LIK at 31 years of age.[4][6]
The condition appears to affect both males and females, with no clear gender predilection based on available case reports. The disease typically presents unilaterally, distinguishing it from bilateral forms of interstitial keratitis such as those associated with congenital syphilis.[1][2]
Pathophysiology
The pathophysiologic mechanisms underlying LIK remain poorly understood. Histopathologic examination from patients with LIK who have undergone penetrating keratoplasty or patch grafting has been unrevealing, with no specific diagnostic features identified.[1] One case report described histopathologic evaluation of a corneal button showing areas of bullous separation between the epithelium and Bowman layer with stromal scarring and thinning, but no findings specific to a particular etiology.[1]
Advanced imaging techniques have provided some insight into the inflammatory process. In vivo confocal microscopy (IVCM) reveals panstromal inflammation despite the appearance of localized anterior stromal involvement on anterior segment optical coherence tomography (AS-OCT).[4] This discrepancy suggests that the inflammatory process is more extensive than clinically apparent.
Clinical Features
Symptoms
Patients with LIK typically present with blurred vision, ocular pain, tearing, photophobia, and conjunctival injection.[1][2][3] The condition is characteristically recurrent, with episodes of inflammation alternating with periods of quiescence.[4][2]
Signs
The hallmark clinical finding is a horizontal/oblique linear stromal opacity often but not always extending from limbus to limbus.[1][2][3][4][5] The lesions are nonmigratory and located in the anterior stroma.[2] Additional clinical findings may include:
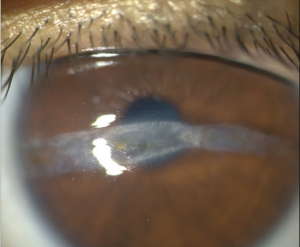
- Stromal edema
- Scarring
- Minimal vascularization[2]
- "Beaded" appearance of the linear infiltrate[4]
- Parallel linear stromal opacities (in some cases)[3]
- Conjunctival injection [5]
In severe cases, corneal perforation may occur, requiring urgent surgical intervention.[1]
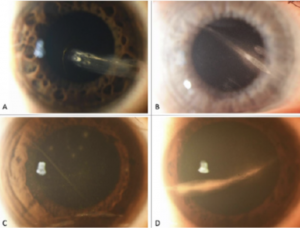
Diagnosis
Clinical Diagnosis
Diagnosis of LIK is primarily clinical, based on the characteristic linear appearance of the corneal opacity.[1][3][4] The horizontal orientation, limbus-to-limbus extension within the palpebral aperture, and recurrent nature of the condition are key diagnostic features.
Diagnostic Procedures
Laboratory Testing
While not necessary for diagnosis, serologic testing for syphilis and Lyme disease may be considered to exclude other etiologies. Cultures may be obtained if an epithelial defect is present, but should not demonstrate growth in true LIK.[1]
Imaging Studies
Anterior Segment Optical Coherence Tomography (AS-OCT)
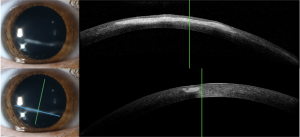
AS-OCT demonstrates anterior stromal hyperreflectivity with inflammation that appears confined to the anterior stroma.[3][4] The imaging shows a characteristic "beaded" appearance and may reveal corneal thinning in the area of involvement.[4]
In Vivo Confocal Microscopy (IVCM)
IVCM provides detailed microstructural findings including:
- Microcystic epithelial edema
- Dense fibrosis of the anterior stroma
- Highly reflective spiculated structures or hyperreflective needle-like structures[3][4]
- Disorganization of stromal architecture
- Panstromal inflammation [4]
IVCM demonstrates that inflammation extends throughout the full thickness of the stroma, despite the appearance of localized anterior involvement on clinical examination and AS-OCT.[4]
Differential diagnosis
The differential diagnosis of LIK includes:
- Classic interstitial keratitis (typically bilateral, associated with syphilis or other systemic infections)
- Herpes simplex disciform endotheliitis (central disc-shaped stromal edema with keratic precipitates)
- Herpes simplex necrotizing stromal keratitis (progressive stromal necrosis with ulceration)
- Bacterial keratitis (typically with epithelial defect and suppurative infiltrate)
- Fungal keratitis (feathery borders, satellite lesions)
- Acanthamoeba keratitis (ring infiltrate, severe pain)
- Neurotrophic keratitis (decreased corneal sensation, persistent epithelial defect)
- Linear endotheliitis (line of keratic precipitates on endothelium with peripheral stromal and epithelial edema)
Management
Medical Therapy
Topical corticosteroids represent the mainstay of therapy for LIK.[1][2][3][4] All reported cases have demonstrated responsiveness to topical steroid treatment. Response to topical steroids supports the diagnosis.[1]
Surgical Management
Surgical intervention is rarely required but may be necessary in cases of corneal perforation or visually significant scarring.[1]
Prognosis
The prognosis for visual recovery with appropriate steroid therapy appears to be generally favorable.[1][2][3] Lesions may heal spontaneously with some scarring and minimal vascularization but without loss of vision.[2] Patients may be left with residual scars outside of the visual axis.[3] However, LIK characteristically follows a relapsing and remitting course, and patients should be counseled accordingly.[2][4] In the one reported case requiring a penetrating keratoplasty, the patient achieved 20/20 best-corrected visual acuity at 6 months follow-up without evidence of LIK recurrence.[1]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 Calvo, C.M., et al., Linear interstitial keratitis: a distinct clinical entity revisited. Cornea, 2012. 31(12): p. 1500-3.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 Petrovic, A., et al., Characteristics of Linear Interstitial Keratitis by In Vivo Confocal Microscopy and Anterior Segment Optical Coherence Tomography. Cornea, 2018. 37(6): p. 785-788.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 Schwab IR, Grabner G, Ostler HB. Interstitial Linear Keratitis. American Journal of Ophthalmology. 1982;94(5):606-9.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 Barrientos LC, Wildes M. Linear Interstitial Keratitis: A Report of Two Cases and Review of Literature. Cureus. 2025;17(3):e80985.
- ↑ 5.0 5.1 5.2 5.3 Blaser F, Muth DR, Barthelmes D, Bajka A, Wiest MRJ, Zweifel SA, Said S. Linear Interstitial Keratitis - Assessment of a Poorly Explored Clinical Entity. JOJ Ophthalmol. 2024;10(4):555795. doi:10.19080/JOJO.2024.10.555795.
- ↑ Coop DH. Interstitial Linear Keratitis. Br J Ophthalmol. 1968;52(12):910-1
- ↑ Illinois Eye and Ear Infirmary, shared with patient guardian permission

