Ocular Graft Versus Host Disease
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Disease
In the United States, over 20,000 patients per year receive allogenic hematopoietic stem cell transplantation (AHSCT) as a cure for hematological disorders.[1] The efficacy of AHST derives from activation of the immune system against malignant cells. Graft-versus- host disease (GVHD) is the result of an overactive systemic inflammatory response, which can lead to the destruction of normal host tissues. Chronic GVHD (cGVHD) is the most common cause of non-relapsing morbidity and mortality in patients greater than 2 years from transplant, occurring in 30% to 70% of patients.[2][3]
Historically, GVHD had been classified as either acute or chronic based on the time elapsed between the transplantation and symptoms. Acute GVHD was defined as the onset of symptoms within 100 days of transplant.[4] Chronic GVHD referred to patients with ongoing symptoms after 100 days of transplant. Currently, acute and chronic GVHD diagnoses are based on specific tissue involvement instead of temporal relationship to AHSCT. Acute GVHD affects the skin, oral and gastrointestinal mucous membranes, lungs, and liver. [4] Chronic GVHD not only affects the organs that can be damaged in acute GVHD, but more frequently involves the eyes, musculoskeletal systems, lymphohematopoietic systems, hair and nails, and genitals.[4][3]
Approximately 40% to 90% of patients with chronic GVHD will develop ocular symptoms.[2] Ocular manifestations include moderate to severe keratoconjunctivitis sicca, bilateral marginal keratitis, anterior uveitis, corneal ulceration and neovascularization, and conjunctival scarring. Ocular GVHD (oGVHD) can be debilitating and severely impact patients' quality of life. It is often difficult to diagnosis and treat due to limited understanding of its pathophysiology and somewhat confusing diagnostic and scoring systems.
Risk Factors
Stem cell transplantation is "allogenic" if the stem cells are derived from a human leukocyte antigen (HLA)- matched donor rather than from the patient's own tissue. Patients who have undergone allogenic stem cell transplantation can develop chronic GVHD, which commonly can present with ocular findings.[4] Reported risk factors for developing cGVHD include older donor and recipient age, mismatched HLA, prior episodes of acute GVHD, and diagnosis of chronic myeloid leukemia.[3]
General Pathology
Histology can show decreased conjunctival goblet cell density, increased conjunctival squamous metaplasia, and infiltration of tissues with inflammatory cells. Often a lymphocytic infiltration with epithelial cell necrosis and lymphocytic exocytosis can be seen.
Pathophysiology
The pathogenesis of GVHD remains poorly understood, although donor- derived alloreactive T lymphocytes are thought to play a pivotal role. Thymic injury sustained during conditioning regimens and/or acute GVHD may lead to central tolerance, aberrant proliferation of autoreactive T (predominantly CD4+ Th2) and B cells, and autoantibody formation.[5] Ocular GVHD involves both cell- mediated and humoral immunity that leads to infiltration and inflammation of the lacrimal gland, conjunctiva and ocular surface.[5] The inflammation can eventually cause a decrease in the density of conjunctival goblet cells as well as scarring of the lacrimal gland and conjunctiva.
Diagnosis
History
A history of allogenic bone marrow transplant is present in all patients with this disease. Affected patients often will complain of dry eye symptoms, such as chronic redness, eye pain, photophobia, foreign body sensation, and decreased vision.
Physical Examination
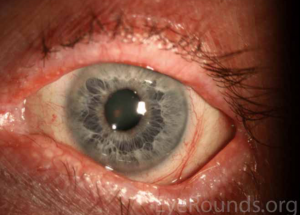
A complete ophthalmologic examination is required including visual acuity testing, refraction, slit lamp examination with the use of fluorescein, lissamine, or rose bengal stains, tear breakup time, tear film osmolarity, and corneal sensitivity testing. A Schirmer tests can be done to determine aqueous tear production, and evaluation of tear break-up time can be used to determine the quality of tears. Infectious etiologies must always be ruled out, especially in the presence of corneal ulceration. The degree of hyperemia, presence of conjunctival scarring, symblepharon, meibomian gland dysfunction, conjunctival and corneal staining, cataracts, and keratinization of the eyelid margins should all be detailed and followed closely in affected patients. Whether GVHD directly causes posterior pole findings such as microvascular retinopathy, central serous chorioretinopathy, and serous retinal detachments is controversial, as these reported associations may be the result of treatment.[4]
Signs
Ocular GVHD is associated with meibomian gland obstruction, anterior and posterior blepharitis. There is often associated scaring of the lacrimal gland leading to decreased tear production. Conjunctival hyperemia with pseudomembrane and membrane formation can also be seen. Chronic inflammation can lead to conjunctival necrosis and cicatricial scarring and fibrosis. Patients often have corneal manifestations including punctate epithelial keratopathy and filamentary keratitis. Severe disease can lead to corneal erosions, thinning, ulcerations, and possible perforations.
Symptoms
Ocular GVHD mimics other immunologically mediated ocular inflammatory diseases. Symptoms that are not unique to this disease entity can include dry eye, foreign body sensation, redness, epiphora, photophobia, blurred vision, eye irritation. Keratoconjunctivitis sicca (KCS) is the most common manifestation of cGVHD and can be exacerbated by concomitant radiation and chemotherapy. Furthermore, KCS can last years after the resolution of other systemic manifestations of cGVHD.
Children with a history of bone marrow transplantation can also develop ocular symptoms but do not complain of the same symptoms as adults. Often children are noted to have excessive eye rubbing, and they complain of light sensitivity as their predominant symptom.
Clinical diagnosis
In 2015, the NIH published an updated consensus for the diagnosis and scoring of cGVHD.[6] To meet the diagnostic criteria, patients may have either one diagnostic manifestation of cGVHD or one distinctive clinical feature with a diagnostic biopsy, laboratory, or other relevant test per affected organ, or evaluation by a specialist. Eye manifestations, such as acute onset "dry" eyes, photophobia, periorbital hyperpigmentation, diffuse punctate keratopathy are still considered a "distinct sign" of cGVHD, and thus cannot establish the diagnosis of cGHVD alone without additional supporting findings.[6] In addition, the diagnosis of ocular cGVHD is made if patients have acute onset dry eye symptoms with corresponding low Schirmer's test (< or = 5mm at 5 min) or a new onset keratoconjunctivitis sicca seen on exam with mean Schirmer's test between 6 to 10mm.[6] The NIH severity scoring removed the Schirmer’s test after reports of poor correlation with physician and patient- reported changes in signs and symptoms, but incorporates the number of times patients use artificial tears.[6]
Another grading criteria for ocular manifestations of chronic GVHD was introduced in 2004 by Robinson et al. See table below.[7]
| Grading criteria for chronic GVHD | |
|---|---|
| Grade | Manifestation |
| Grade 1 | Conjunctival hyperemia of the bulbar or palpebral conjunctiva |
| Grade 2 | Fibrovascular changes of the palpebral conjunctiva involving <25% of the total surface are of at least 1 eyelid |
| Grade 3 | Fibrovascular changes of the palpebral conjunctiva involving 25-75% of at least 1 eyelid. |
| Grade 4 | Involves >75% of the conjunctival with or without cicatricial entropion in at least 1 eyelid. |
In 2013, the International chronic oGVHD consensus group (ICOCG) proposed new diagnostic and severity guidelines for oGVHD based on the Ocular Surface Disease Index (OSDI), Schirmer’s test score without anesthesia, corneal fluorescein staining, and conjunctival injection.[8] Each ocular parameter is assigned a severity score (0-3), and the diagnosis of oGVHD is then determined from the aggregate score and the presence or absence of systemic cGVHD. These new guidelines incorporate several objective dry eye measures. This diagnostic criterion was validated by a study published in 2017.[9]
Diagnostic procedures
- Schirmer's test
- Tear breakup time
- Tear osmolarity
- Corneal sensitivity
- Tear film microscopy
- Confocal microscopy
- Impression cytology
- Conjunctival biopsy
Management
Systemic treatment of the GVHD is important, but often ocular symptoms do not respond well to with systemic treatments alone.
Localized treatment includes topical lubricants such as preservative free artificial tears, autologous serum tears, and topical immunosuppressive treatments. Punctal plugs or punctual cautery are often helpful in increasing lubrication, although there is controversy regarding whether they may concentrate inflammatory mediators on the ocular surface.[4] Systemic steroids have been found to be helpful. Topical anti-inflammatories are now a mainstay of treatment. These include topical corticosteroids, topical tacrolimus, topical cyclosporine A, and serum tears. Cyclosporine A is a T-cell inhibitor that helps to downregulate inflammatory cytokines in the conjunctiva. Malta et al. advocated initiation of topical cyclosporine 0.5% 1 month prior to bone marrow transplantation to reduce the severity of ocular symptoms associated with GVHD.[10] However, these recommendations have not been validated by a large double-blinded, placebo controlled trial. Bandage contact lenses and scleral lenses may be considered to protect the ocular surface and improve comfort levels. Amniotic membrane and tarsorrhaphy may be necessary if the ocular surface deteriorates despite aggressive conservative measures.
See Management of Ocular Graft vs Host page
General treatment
See Management of Ocular Graft vs Host page
Complications
If untreated, cicatricial scarring of the lacrimal gland and conjunctiva can occur. Additionally, severe corneal disease can lead to epithelial breakdown, thinning, infection, and possible perforation. Scarring and neovascularization can also cause decreased vision in these patients.
References
- ↑ Current use and outcome of hematopoietic stem cell transplantation: CIBMTR Summary Slides. 2015. Available at: http://cibmtr.org.
- ↑ 2.0 2.1 Global and organ-specific chronic graft-versus-host disease severity according to the 2005 NIH Consensus Criteria. Blood 2011;118:4242–4249.
- ↑ 3.0 3.1 3.2 Zeiser R, Blazar BR. Pathophysiology of Chronic Graft-versus-Host Disease and Therapeutic Targets. N Engl J Med 2017;377:2565-79.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Balasubramaniam SC, Raja H, Nau CB, Shen JF, Schornack MM. Ocular Graft-Versus-Host Disease: A Review. Eye Contact Lens 2015;41:256-61.
- ↑ 5.0 5.1 Kim SK. Ocular Graft vs. Host Disease. Ocular Surface 2011;3:S–177–S–179.
- ↑ 6.0 6.1 6.2 6.3 Jagasia MH, Greinix HT, Arora M, et al. National Institutes of Health Consensus Development Project on Criteria for Clinical Trials in Chronic Graft-versus-Host Disease: I. The 2014 Diagnosis and Staging Working Group report. Biol Blood Marrow Transplant 2015;21:389-401 e1.
- ↑ Robinson MR, Lee SS, Rubin BI, et al. Topical corticosteroid therapy for cicatricial conjunctivitis associated with chronic graft-versus-host disease. Bone Marrow Transplant 2004;33:1031-5.
- ↑ Ogawa Y, Kim SK, Dana R, et al. International Chronic Ocular Graft-vs-Host-Disease (GVHD) Consensus Group: proposed diagnostic criteria for chronic GVHD (Part I). Sci Rep 2013;3:3419.
- ↑ Rapoport Y, Freeman T, Koyama T, et al. Validation of International Chronic Ocular Graft-Versus-Host Disease (GVHD) Group Diagnostic Criteria as a Chronic Ocular GVHD-Specific Metric. Cornea 2017;36:258-63.
- ↑ Malta JB, Soong HK, Shtein RM, et al. Treatment of ocular graft-versus-host disease with topical cyclosporine 0.05%. Cornea 2010;29:1392-6.

