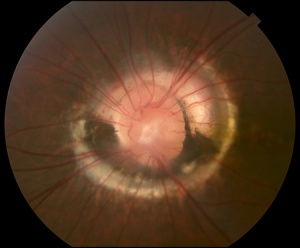
Ocular Manifestations of Moyamoya Disease
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Moyamoya disease (MMD) is a chronic occlusive cerebrovascular disorder affecting the terminal portions of the bilateral internal carotid arteries or proximal portions of the anterior and middle cerebral arteries[1][2]. The progressive ischemia results in the formation of a collateral vascular network in the base of the brain. The term “moya moya” is a Japanese word which means a hazy puff of smoke, used to describe the abnormal appearance of the vascular network seen in angiograms of patients with MMD[3].
Epidemiology
The incidence of MMD is highest among Japanese and Koreans, and much lower in Caucasians[3]. In 2003, the incidence of MMD was reported to be 0.54 per 100,000 in Japanese populations[4], which is ten times the incidence in North America and Europe[5]. The male to female ratio was 1:1.8, and the peak of prevalence was in the second decade in males age in the third decade for females[4]. There are rare cases presented Familial cases of MMD were reported to be 12.1%[4], while other case reports in North America were found to be isolated and ~ 4% familial [6] In a National inpatient sample at USA (2002-2008) incidence was 0.57 per 100 000 people per year. The prevalence and incidence where highest in the ones with Asian origin (mainly Japanese) in a similar rate than reported in Japanese studies[7] Furthermore, MMD is associated with Trisomy 21, with some sources reporting a 26-fold increase in the prevalence of MMD among patients with Trisomy 21.[8]
Etiology
The etiology of MMD is largely unknown, but due to the higher incidence of this disease in Japanese populations and the presence of familial cases, it is thought that MMD could be a multifactorial disease[3][9]. Some genetic studies of familial MMD propose that responsible genetic loci are located on chromosomes 3, 6, and 17[10][11][12]. Additionally, many cytokines such as VEGF, bFGF, and TGF-β1 have been found in MMD patients. These cytokines are associated with causing vessel narrowing and occlusion by promoting smooth muscle proliferation into the tunica intima, but it is still unknown if they are the cause of MMD[9]. It is likely that multiple factors are linked that underlie the pathophysiology of MMD. The estimated prevalence of MMD in Japan almost doubled between 1994 to 2003, probably due to advances in neuroradiological diagnostic techniques, which helped identify new cases[4].
A gene associated to MMD (and atherosclerosis intracranially) is RING finger protein (RNF213)
Ocular Manifestations
The two main types of symptoms in MMD are cerebral ischemia and hemorrhage. The main symptoms in children are transient ischemic attacks (TIA), which can occur repeatedly and on alternating sides because the occlusions are bilateral[3]. Headaches, involuntary motor disturbances, and seizures can also occur. In adults, intracerebral, intraventricular, or subarachnoid hemorrhages occur more frequently than ischemic symptoms[1][7].
Ocular manifestations in MMD are uncommon, but several case reports have described varying ocular manifestations including:[13][14][15][16][17]
- Amaurosis fugax
- Central retinal artery occlusion
- Morning glory disc anomaly
- Ocular ischemic syndrome
- Transient visual symptoms such as blurry vision[13][18].
- Visual field defects including homonymous hemianopsia have also been reported in patients with MMD[13][18].
Although the vascular occlusion seen in MMD is primarily associated with the anterior and middle cerebral arteries, these visual symptoms are associated with delayed stenosis of the posterior cerebral artery[18]. Visual disturbances are more likely to occur in cases with juvenile onset of MMD[19]. Importantly, when evaluating patients with concurrent MMD and Trisomy 21, visual disturbances may not be reported subjectively depending on the degree of intellectual disability impacting the patient. In this case, objective signs on physical examination and imaging may provide clinical information that patients are not able to provide.
Amaurosis Fugax
Several case reports document cases of amaurosis fugax in patients with MMD[2][15][17]. Amaurosis fugax is described as recurrent episodes of painless and transient loss of vision. Amaurosis fugax results from the occlusion of the internal carotid artery circulation. Thromboembolism that results from the carotid circulation in addition to hypoperfusion caused by the occlusion of the internal carotid artery are the underlying mechanisms that lead to transient vision loss[20].
Central retinal artery occlusion
Several case reports have described cases of central retinal artery occlusion (CRAO) in patients with MMD[13][21]. The central retinal artery is a branch off of the ophthalmic artery, and it supplies blood to the surface of the optic disc[22]. The artery can become obstructed due to an embolus or thrombus, vasculitis causing retinal vasculature inflammation, traumatic vessel wall damage, or spasm. The lack of oxygen to the retina often results in severe vision loss. CRAO is characterized by a cherry red spot in the center of the macula with the surrounding retina pale in color due to lack of blood flow[2]. In addition to a fundus examination, Fundus Fluorescein Angiography (FFA) can be used to diagnose CRAO by showing a delay in retinal arterial filling[13].
Despite the proximity of the central retinal artery to the ophthalmic artery, retinal vascular abnormalities rarely occur in cases of MMD as its slow progression allows for a collateral circulation to the eye to develop via the external carotid artery[21]. The disease is also more common in younger individuals whose vasculature has a greater ability to make hemodynamic adjustments to prevent arterial occlusion complications compared to older individuals. Additionally, vessel occlusion in MMD could occur distal to the bifurcation of the ophthalmic artery and thus may spare the eye[21].
Morning glory disc anomaly
Morning glory disc anomaly is a congenital deformity of the optic nerve associated with poor vision[5][14]. A fundoscopic examination shows three primary features including an enlarged, funnel-shaped excavation of the optic disc, chorioretinal pigment changes surrounding the optic disc, and a central glial tuft overlying the optic disc[14]. A distinguishing factor of morning glory disc anomaly from other congenital disc anomalies is the presence of abnormal retinal vasculature. This suggests that abnormal vascular development in utero may underlie the association between morning glory disc anomaly and MMD[5]. The association of morning glory disc anomaly with intracranial vascular disorders such as MMD may be under-recognized as carotid angiography might not be performed in individuals with morning glory disc anomaly[23]. Careful history taking of patients with morning glory disc anomaly can reveal presence of neurological symptoms that may necessitate the use of magnetic resonance angiography (MRA) to exclude abnormal intracranial vascular development whenever MMD is suspected[5].
Ocular ischemic syndrome
Ocular ischemic syndrome (OIS) is a condition associated with carotid artery occlusion that leads to ocular hypoperfusion. A consequence of chronic retinal and choroidal ischemia is the excessive production of vascular endothelial growth factor (VEGF)[24]. VEGF acts on epithelial cells to result in new blood vessel growth. This neovascularization occurs in the iris and at the irido-corneal angle in the anterior segment[24]. The new blood vessels are accompanied by the proliferation of a fibrovascular membrane that consists of myofibroblast cells. Myofibroblast cells contract the fibrovascular membrane which results in angle closure glaucoma. Chronic hypoperfusion to the ciliary body leads to a decrease in aqueous humor production, which can lead to a relative decrease in intraocular pressure in the anterior segment[25]. In addition to neovascular glaucoma and low intraocular pressure in the anterior segment, OIS can also result in complications such as anterior uveitis[15]. Patients with MMD are at risk of OIS due to the progressive occlusive nature of the disorder resulting in hypoperfusion of the eye[15][16].
Other
Case reports have shown increased in superficial vascular complex(SVC) of eyes with shunts secondary to Moyamoya disease(ophthalmic artery from internal carotid artery to middle meningeal and facial), as seen with OCT angiography. The increased SVC resolved after bypass from the superficial temporal artery to the middle cerebral artery [26].
Other studies have compared fundus photo of patients with Moyamoya with control patients patients in order to design a deep learning algorithm that can use retinal photographs as biomarkers of Moyamoya.[27]
Diagnosis
The clinical diagnostic criteria for MMD is based on the following angiographic findings:
1- Stenosis or occlusion of the terminal portion of the internal carotid artery or proximal portions of the anterior and/or middle cerebral artery
2- Abnormal vascular networks near the stenotic lesions in the arterial phase
3- Bilateral lesion[3]
When occlusions are unilateral, it is categorized as probable disease and these usually progress to involve the other side within couple of years on disease onset. Diagnosis of MMD is also possible using noninvasive modalities like MRA as opposed to conventional angiography.
Of note, in Japan, the guidelines were modified to include MMD diagnosis even when unilateral involvement due to the high incidence of progression from unilateral to bilateral.[28]
Management
Currently intracranial stenosis seen in MMD cannot be reversed.
Revascularization currently is the only effective way for ischemic MMD. Medical and surgical treatment options are directed towards alleviating symptoms and preventing strokes and TIAs[29]. Direct and indirect revascularization surgeries can be performed to improve blood flow to the brain. Direct bypass surgery involves making an anastomosis between the superficial temporal artery to the middle cerebral artery, while indirect bypass surgery consists of placing a vascularized soft-tissue flap on the surface of the brain to promote angiogenesis[3].
Non-surgical therapies focus on using antiplatelet agents, vasodilators, and antifibrinolytic agents to improve blood flow and prevent embolism in patients[29]. Additionally, recent studies have applied remote ischemic conditioning (RIC) to treat manifestation of MMD like transient ischemic attack, hemorrhagic or ischemic stroke, headache and seizure by inflating arm cuffs in both arms for 5min and off for 5min with a pressure of 50 mmHg over systolic blood pressure for a total of five cycles. The study showed reduced ischemic events, symptom relief and cerebral perfusion improvement[30]
Summary
Although MMD is a rare condition, it is important for the ophthalmologist to be aware of the ocular manifestations as they can lead to severe vision loss. The ophthalmologist plays an important role in the diagnosis of MMD because signs of the disease may first be observed in the fundus (posterior part of the eye) before they lead to other life-threatening CNS events. Appropriate management of the disease requires collaboration between the ophthalmologist, neurologist, vascular surgeon, and primary care physician[16].
References
- ↑ 1.0 1.1 Hishikawa, T., Sugiu, K. & Date, I. Moyamoya Disease: A Review of Clinical Research. Acta Med. Okayama 70, 229–236 (2016).
- ↑ 2.0 2.1 2.2 Das, D. et al. Moyamoya disease with neuro-ophthalmic manifestations: a rare case report. Eye Brain 2, 63–65 (2010).
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Fukui, M., Kono, S., Sueishi, K. & Ikezaki, K. Moyamoya disease. Neuropathol. Off. J. Jpn. Soc. Neuropathol. 20 Suppl, S61-64 (2000).
- ↑ 4.0 4.1 4.2 4.3 Kuriyama, S. et al. Prevalence and clinicoepidemiological features of moyamoya disease in Japan: findings from a nationwide epidemiological survey. Stroke 39, 42–47 (2008).
- ↑ 5.0 5.1 5.2 5.3 Williams, M., Adas, A., Sharma, N. & Gibson, M. Moyamoya disease presenting to the ophthalmology clinic. Can. J. Ophthalmol. J. Can. Ophtalmol. 41, 633–634 (2006).
- ↑ Gaillard J, Klein J, Duran D, Storey A, Scott RM, Kahle K, Smith ER. Incidence, clinical features, and treatment of familial moyamoya in pediatric patients: a single-institution series. J Neurosurg Pediatr. 2017 May;19(5):553-559. doi: 10.3171/2016.12.PEDS16468. Epub 2017 Mar 10. PMID: 28291427
- ↑ 7.0 7.1 Gonzalez NR, Amin-Hanjani S, Bang OY, et al. Adult Moyamoya Disease and Syndrome: Current Perspectives and Future Directions: A Scientific Statement From the American Heart Association/American Stroke Association. Stroke. 2023;54(10):e465-e479. doi:10.1161/STR.0000000000000443
- ↑ See AP, Ropper AE, Underberg DL, Robertson RL, Scott RM, Smith ER. Down syndrome and moyamoya: clinical presentation and surgical management. J Neurosurg Pediatr. 2015;16(1):58-63. doi:10.3171/2014.12.PEDS14563
- ↑ 9.0 9.1 Huang, S., Guo, Z.-N., Shi, M., Yang, Y. & Rao, M. Etiology and pathogenesis of Moyamoya Disease: An update on disease prevalence. Int. J. Stroke Off. J. Int. Stroke Soc. 12, 246–253 (2017).
- ↑ Inoue, T. K., Ikezaki, K., Sasazuki, T., Matsushima, T. & Fukui, M. Linkage analysis of moyamoya disease on chromosome 6. J. Child Neurol. 15, 179–182 (2000).
- ↑ Ikeda, H., Sasaki, T., Yoshimoto, T., Fukui, M. & Arinami, T. Mapping of a familial moyamoya disease gene to chromosome 3p24.2-p26. Am. J. Hum. Genet. 64, 533–537 (1999).
- ↑ Mineharu, Y. et al. Autosomal dominant moyamoya disease maps to chromosome 17q25.3. Neurology 70, 2357–2363 (2008).
- ↑ 13.0 13.1 13.2 13.3 13.4 Kumar M, A. & Ganesh B, A. CRAO in Moyamoya Disease. J. Clin. Diagn. Res. JCDR 7, 545–547 (2013).
- ↑ 14.0 14.1 14.2 Ponnatapura, J. Morning glory syndrome with Moyamoya disease: A rare association with role of imaging. Indian J. Radiol. Imaging 28, 165–168 (2018).
- ↑ 15.0 15.1 15.2 15.3 Chen, C. S., Lee, A. W., Kelman, S. & Wityk, R. Anterior ischemic optic neuropathy in moyamoya disease: a first case report. Eur. J. Neurol. 14, 823–825 (2007).
- ↑ 16.0 16.1 16.2 Papavasileiou, E., Sobrin, L. & Papaliodis, G. N. Ocular ischemic syndrome presenting as retinal vasculitis in a patient with moyamoya syndrome. Retin. Cases Brief Rep. 9, 170–172 (2015).
- ↑ 17.0 17.1 Borah, P. et al. Varied presentations of moyamoya disease in a tertiary care hospital of north-east India. Ann. Indian Acad. Neurol. 17, 317–320 (2014).
- ↑ 18.0 18.1 18.2 Lee, J. Y. et al. Delayed posterior circulation insufficiency in pediatric moyamoya disease. J. Neurol. 261, 2305–2313 (2014).
- ↑ Miyamoto, S. et al. Study of the posterior circulation in moyamoya disease. Part 2: Visual disturbances and surgical treatment. J. Neurosurg. 65, 454–460 (1986).
- ↑ Najem, K. & Margolin, E. Amaurosis Fugax. in StatPearls (StatPearls Publishing, 2018).
- ↑ 21.0 21.1 21.2 Chace, R. & Hedges, T. R. Retinal artery occlusion due to moyamoya disease. J. Clin. Neuroophthalmol. 4, 31–34 (1984).
- ↑ Varma, D. D., Cugati, S., Lee, A. W. & Chen, C. S. A review of central retinal artery occlusion: clinical presentation and management. Eye Lond. Engl. 27, 688–697 (2013).
- ↑ Sathyan, S. & Chackochan, M. Morning glory disc anomaly and facial hemangiomas in a girl with moyamoya syndrome. Indian J. Ophthalmol. 66, 1644–1646 (2018).
- ↑ 24.0 24.1 Terelak-Borys, B., Skonieczna, K. & Grabska-Liberek, I. Ocular ischemic syndrome - a systematic review. Med. Sci. Monit. Int. Med. J. Exp. Clin. Res. 18, RA138-144 (2012).
- ↑ Furino, C. et al. In vivo evidence of hypotrophic ciliary body in ocular ischemic syndrome by ultrasound biomicroscopy. Ophthalmic Surg. Lasers Imaging Off. J. Int. Soc. Imaging Eye 38, 505–507 (2007).
- ↑ cite Lo KJ, Wang AG, Cheng HC. Retinal Vasculature Changes after Bypass Surgery for Moyamoya Disease. Ophthalmology. 2021 Jan;128(1):120. doi: 10.1016/j.ophtha.2020.08.014. Erratum in: Ophthalmology. 2021 Mar;128(3):483. PMID: 33349336.
- ↑ Hong JS, Yoon S, Shim KW. Screening of Moyamoya Disease From Retinal Photographs: Development and Validation of Deep Learning Algorithms. Stroke.Volume 55, Issue 3, March 2024; Pages 715-724. DOI:https://doi.org/10.1161/STROKEAHA.123.044026
- ↑ Uchiyama S, Fujimura M. Adult Moyamoya Disease and Moyamoya Syndrome: What Is New?. Cerebrovasc Dis Extra. 2024;14(1):86-94. doi:10.1159/000540254
- ↑ 29.0 29.1 Kronenburg, A., Braun, K. P. J., van der Zwan, A. & Klijn, C. J. M. Recent advances in moyamoya disease: pathophysiology and treatment. Curr. Neurol. Neurosci. Rep. 14, 423 (2014).
- ↑ Ding JY, Shang SL, Sun ZS, et al. Remote ischemic conditioning for the treatment of ischemic moyamoya disease. CNS Neurosci Ther. 2020;26(5):549-557. doi:10.1111/cns.13279