Ocular Manifestations of Pityriasis Rubra Pilaris
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
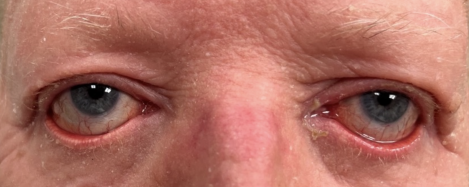
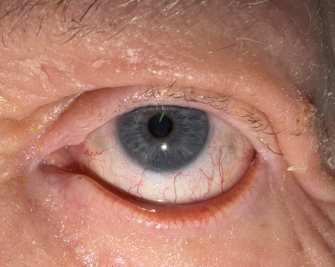
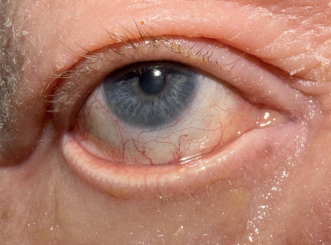
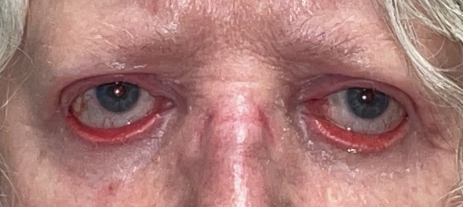
Pityriasis rubra pilaris (PRP) is a rare, inflammatory, papulosquamous disorder that has a variable onset, course, and prognosis. It is characterized by follicular hyperkeratotic papules, waxy palmar-plantar keratoderma, and erythematous plaques with islands of spared skin.[1],[2] PRP may present with ocular manifestations, as prolonged facial involvement can precipitate scarring leading to cicatricial ectropion. Cicatricial ectropion is associated with ocular surface dryness, discomfort, and potential progression to exposure keratitis, ulceration, infection, eyelid retraction, and vision loss.[1],[3],[4]
Disease Entity
ICD code: L44.0
Epidemiology and Risk Factors
Pityriasis rubra pilaris (PRP) is a spectrum of rare skin disorders with variable incidence, estimated between 1 in 5,000 to 50,000 persons who present as new patients to dermatology clinics.[5] Key clinical features of PRP include: follicular hyperkeratotic papules which are small scaly bumps caused by keratin build up in the hair follicles, waxy palmar-plantar keratoderma described as thickened red scale on the palms and soles, and orange-red erythematous plaques with islands of spared skin.[2],[6] PRP can present at any age, but it most commonly affects patients in their 6th and 7th decades of life.[7] The etiology of PRP is yet to be fully understood, though it is thought to involve autoimmune disease, viral infections, and malignancy. Fewer than 5% of patients with a diagnosis of PRP demonstrate familial manifestation of the disease; there is an association with autosomal dominant mutations in the CARD14 gene.[1] Isolated cases of drug-induced PRP have been identified, with tyrosine kinase inhibitors as the most frequently reported offender.[8] Infection by the COVID-19 virus and vaccination against COVID-19 have been reported as potential identifiable triggers.[6]
Non-cutaneous complications of the PRP spectrum include ectropion, hearing loss due to buildup in auditory canals, arthralgias, hair loss, edema, and difficult body temperature regulation.[1],[5] Additionally, patients with PRP often experience severe pruritus, burning sensations, painful palmoplantar fissures, and many physiologic and psychological sequelae of cutaneous and non-cutaneous symptoms.[5]
General Pathology, Pathophysiology and Histopathology
The pathophysiology of PRP has not yet been fully defined, and classification is dependent on clinical subtype. Inherited PRP is associated with a mutation of the CARD14 gene. This cascade causes aberrant immunological activation, similar to a pathway of psoriasis.[9]
Common histopathologic features of PRP include acantholysis (a loss of desmosomal connection between keratinocytes, causing skin detachment); alternating orthokeratosis (thickened skin secondary to normal cellular maturation) and parakeratosis (thickened skin secondary to abnormal, rapid maturation of cells); follicular plugging (by dead skin cells and keratin); lymphocytic inflammatory infiltrate; mitotic figures; a normal or thickened granular layer; and psoriasiform hyperplasia (skin thickening secondary to chronic epidermal inflammation).[1]
There are distinct histopathologic findings of PRP that can be divided into early evolving, fully developed, and late lesions. Early lesions have a “normal” basket-weave cornified layer, hypergranulosis, thick suprapapillary plates, dilation of blood vessels of the superficial plexus, and a sparse lymphohistiocytic infiltrate around superficial vessels.[10] Fully developed lesions displayed alternating foci of parakeratosis and orthokeratosis in both vertical and horizontal directions, arranged in columns, differing from psoriasis, which is arranged in mounds. The cornified layer is often thinned or entirely lost, while the granular layer is intact or thickened.[10] Late lesions showed prominent hypergranulosis instead of spongiosis, another differentiating factor from psoriasis, and a laminated or compactly orthokeratotic cornified layer.[10]
Ophthalmic Pathophysiologic and Clinical Manifestations
Cicatricial ectropion (CE) is a common ophthalmic finding in patients with PRP, secondary to tight, thickened skin formation following chronic, severe, periocular inflammation.[3] Patients may present with periocular erythema, hyperkeratotic scaling around the upper and lower lids, photophobia, foreign body sensation, epiphora and conjunctival injection.[11]
Cicatricial ectropion occurs during wound healing when normal skin is replaced with fibrous tissue following mechanical, thermal, chemical, or inflammatory insult. Soft tissue contracture occurs, causing loss of eyelid elasticity and vertical shortening of the anterior lamella, everting the punctum and rotating the eyelid away from the globe. This disturbs the ocular surface and may precipitate punctate epithelial erosions, ulceration, infection, and visual impairment.[11],[12] The severity of cicatricial ectropion correlates with the extent, chronicity, and location of the epidermal inflammation.[13] Patients with severe cicatricial ectropion have the potential to develop serious corneal sequelae, including keratitis, as well as functional and cosmetic deformity.[4]
Differential Diagnosis
When considering a differential diagnosis for PRP with ocular involvement, it is important to first rule out trauma, infection, or other potential emergencies. Other keratinizing disorders should be included in the differential diagnosis. Lamellar ichthyosis, an inherited, rare keratinization disorder, presents with keratin scales and subsequent contracture of the eyelids, a picture similar to PRP with cicatricial ectropion. Lamellar ichthyosis is present at birth and has large scaling, whereas PRP presents in childhood or adulthood with a fine scale.[14] Keratosis follicularis, another inherited, keratinizing dermatologic disease, can present with occasional ocular manifestations such as blepharitis, conjunctival hyperemia, and short tear film break-up time.[15] Despite eyelid inflammation, cicatricial ectropion has not been reported in the literature, differentiating keratosis follicularis with ocular involvement from PRP with ocular involvement.
Inflammatory dermatoses should also be considered when patients present with cicatricial ectropion. Psoriasis presents with well-demarcated plaques that can involve the eyelids, leading to chronic inflammation and secondary cicatricial ectropion similar to PRP.[14] The pattern of large silvery plaques and absence of fine scale with follicular papules helps differentiate psoriasis from PRP. Additionally, chronic cutaneous lupus erythematosus can rarely affect the eyes with manifestations such as periocular edema, blepharoconjunctivitis, and erythematous plaques leading to scarring and cicatricial ectropion.[14] Like psoriasis, cutaneous lupus has discrete plaques (though erythematous, unlike psoriasis) that differentiate it from the fine scaling of PRP.
Management
Conservative management includes the use of topical emollients and lubricants as well as topical corticosteroids, which help maintain the eyelid and ocular surface integrity. These are used mostly in addition to systemic therapy.[16]
Systemic therapy should be determined on a patient-to-patient basis, as adults should be started on systemic treatment more readily, while children are often managed more conservatively.[16] Initial systemic therapy options include the use of oral retinoids and methotrexate, which were reported by patients to be among the most helpful treatments in relieving their PRP symptoms, though the report is not specific to ocular symptoms.[7] One case report detailed the complete resolution of PRP-induced cicatricial ectropion in a patient who was placed on methotrexate to stabilize her cutaneous disease.[17] However, due to the side effect profile of methotrexate and oral retinoids, injectable biologics such as IL-17 or IL-23 inhibitors are the preferred initial therapies. If the disease is refractory to one of the above options, biologics can be used in conjunction with methotrexate or oral retinoids. Other therapies, such as TNF-alpha inhibitors, IL-1 inhibitors, JAK inhibitors, phototherapy, and immunosuppressants such as cyclosporine, have been reported as beneficial in patients with PRP, not specific to ocular manifestations.[16] Of note, oral dexamethasone has been reported to resolve one patient’s PRP-induced cicatricial ectropion.[18]
Surgical intervention may be necessary in cases of morbid PRP-induced cicatricial ectropion that are refractory to conservative and systemic treatment. It is important to optimize medical management with a dermatologist to stabilize cutaneous disease before proceeding with surgical intervention.[12] Ensuring adequate counseling prior to surgery is also important for tempering patient expectations. The likelihood of recurrence and the need for subsequent procedures are high. The use of oversized skin grafting has been described to correct eyelid malpositioning in patients with PRP-induced cicatricial ectropion.[3],[12]
Prevention
Prevention efforts should be directed at early detection, diagnosis, and treatment of PRP. Systemic treatment, such as oral retinoids, methotrexate, or biologics, should be initiated to prevent severe disease and potential facial and lid involvement. Diligent periocular skincare with emollients and topical corticosteroids in patients diagnosed with PRP can help prevent contracture.[7],[16]
Prognosis
The prognosis of PRP is variable from patient to patient and even between subtypes of PRP. Spontaneous resolution can occur within months to years, though some courses are chronic.[3],[16]
For patients with PRP-induced cicatricial ectropion, some experience spontaneous resolution with systemic disease resolution, while others have had success in the use of systemic treatment such as methotrexate and dexamethasone.[17],[18] In patients with PRP-induced cicatricial ectropion refractory to systemic treatment, surgical intervention with skin grafting may be required. This can be a prolonged course for patients, as many need multiple procedures to manage recurrence.[3],[12]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 Greiling TM. Pityriasis Rubra Pilaris: Pathogenesis, clinical manifestations, and diagnosis. UpToDate.com. Updated April 14, 2023. Accessed February 23, 2026. https://www.uptodate.com/contents/pityriasis-rubra-pilaris-pathogenesis-clinical-manifestations-and-diagnosis
- ↑ 2.0 2.1 National Organization for Rare Disorders (NORD). Pityriasis Rubra Pilaris. RareDiseases.org. Last updated February 2, 2021. Accessed February 24, 2026. https://rarediseases.org/rare-diseases/pityriasis-rubra-pilaris/
- ↑ 3.0 3.1 3.2 3.3 3.4 Moledina M, Davison S, Malik A. Ophthalmic complication of pityriasis rubra pilaris. BMJ Case Rep. 2024;17(5):e256445. Published 2024 May 28. doi:10.1136/bcr-2023-256445 https://pubmed.ncbi.nlm.nih.gov/38806396/
- ↑ 4.0 4.1 Paranjothy B, Shunmugam M, MacKenzie J, Azuara-Blanco A. Peripheral ulcerative keratitis in pityriasis rubra pilaris. Eye (Lond). 2007;21(7):1001-1002. doi:10.1038/sj.eye.6702797 https://pubmed.ncbi.nlm.nih.gov/17401317/
- ↑ 5.0 5.1 5.2 Greiling TM, Brown F, Syed HA. Pityriasis Rubra Pilaris. [Updated 2024 Apr 30]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482436/
- ↑ 6.0 6.1 Zhou T, Al Muqrin A, Abu-Hilal M. Updates on Pityriasis Rubra Pilaris: A Scoping Review. J Cutan Med Surg. 2024;28(2):158-166. doi:10.1177/12034754231223159 https://pubmed.ncbi.nlm.nih.gov/38174859/
- ↑ 7.0 7.1 7.2 Ross NA, Chung HJ, Li Q, Andrews JP, Keller MS, Uitto J. Epidemiologic, Clinicopathologic, Diagnostic, and Management Challenges of Pityriasis Rubra Pilaris: A Case Series of 100 Patients. JAMA Dermatol. 2016;152(6):670-675. doi:10.1001/jamadermatol.2016.0091 https://pmc.ncbi.nlm.nih.gov/articles/PMC6262840/
- ↑ Mufti A, Lytvyn Y, Maliyar K, Sachdeva M, Yeung J. Drugs associated with development of pityriasis rubra pilaris: A systematic review. J Am Acad Dermatol. 2021;84(4):1071-1081. doi:10.1016/j.jaad.2020.07.052 https://pubmed.ncbi.nlm.nih.gov/32687965/
- ↑ Fuchs-Telem D, Sarig O, van Steensel MA, et al. Familial pityriasis rubra pilaris is caused by mutations in CARD14. Am J Hum Genet. 2012;91(1):163-170. doi:10.1016/j.ajhg.2012.05.010 https://pmc.ncbi.nlm.nih.gov/articles/PMC3397268/
- ↑ 10.0 10.1 10.2 Soeprono FF. Histologic criteria for the diagnosis of pityriasis rubra pilaris. Am J Dermatopathol. 1986;8(4):277-283. doi:10.1097/00000372-198608000-00001 https://pubmed.ncbi.nlm.nih.gov/3766917/
- ↑ 11.0 11.1 EyeWiki. Cicatricial Ectropion. American Academy of Ophthalmology. Available at: https://eyewiki.org/Cicatricial_Ectropion Accessed March 9, 2026.
- ↑ 12.0 12.1 12.2 12.3 Cohen PR, Prystowsky JH. Pityriasis rubra pilaris: a review of diagnosis and treatment. J Am Acad Dermatol. 1989;20(5 Pt 1):801-807. doi:10.1016/s0190-9622(89)70093-1 https://pubmed.ncbi.nlm.nih.gov/2654219/
- ↑ Haridas AS, Sullivan TJ. Surgical Management of Cicatricial Ectropion in Pityriasis Rubra Pilaris. Ophthalmic Plast Reconstr Surg. 2016;32(1):e12-e15. doi:10.1097/IOP.0000000000000385 https://pubmed.ncbi.nlm.nih.gov/25794020/
- ↑ 14.0 14.1 14.2 Rossetto JD, Gracitelli CPB, Osaki TH, Osaki MH. Diseases, conditions, and drugs associated with cicatricial ectropion. Arq Bras Oftalmol. 2019;82(4):345-353. Published 2019 May 20. doi:10.5935/0004-2749.20190068 https://pubmed.ncbi.nlm.nih.gov/31116320/
- ↑ Hammad H, Adler E, Yeshurun A, et al. Ophthalmic Assessment in Patients With Darier Disease. Am J Ophthalmol. 2021;227:139-142. doi:10.1016/j.ajo.2021.03.011 https://pubmed.ncbi.nlm.nih.gov/33737033/
- ↑ 16.0 16.1 16.2 16.3 16.4 Greiling TM. Pityriasis Rubra Pilaris: Prognosis and management. UpToDate.com. Updated January 15, 2026. Accessed February 23, 2026. https://www.uptodate.com/contents/pityriasis-rubra-pilaris-prognosis-and-management
- ↑ 17.0 17.1 Durairaj VD, Horsley MB. Resolution of pityriasis rubra pilaris-induced cicatricial ectropion with systemic low-dose methotrexate. Am J Ophthalmol. 2007;143(4):709-710. doi:10.1016/j.ajo.2006.11.038 https://pubmed.ncbi.nlm.nih.gov/17386290/
- ↑ 18.0 18.1 Fydanaki O, Rezq H, Sepetis AE, Joganathan V. Resolution of Pityriasis rubra pilaris induced ectropion with oral dexamethasone. A case report. Orbit. 2025;44(1):87-89. doi:10.1080/01676830.2024.2311657 https://pubmed.ncbi.nlm.nih.gov/38319642/