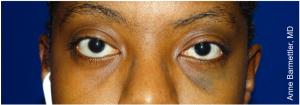
Oculodermal Melanocytosis (Nevus of Ota)
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Definition: Oculodermal melanosis (Nevus of Ota, melanosis oculi), also known as oculodermal melanocytosis, oculomucodermal melanocytosis, or congenital melanosis bulbi, is a benign mesodermal melanosis involving the distributions of the ophthalmic and maxillary trigeminal nerve with associated hyperpigmentation of the eye and its adnexa.[1][2] Entrapment of melanocytes in the upper third of the dermis leads to gray-blue macular hyperpigmentation of the conjunctiva and sclera and ipsilateral facial skin, usually occurring unilaterally.[3] Scleral involvement occurs in greater than two-thirds of cases and is associated with an increased risk of developing glaucoma.[4][5] Rarely, there can also be intraoral involvement with similar pigmented lesions seen on the palate.[6]
Etiology/Prevalence
Nevus of Ota typically presents at birth but can also appear in puberty or during pregnancy.[5] Nevus of Ota presents more commonly in females than males, with a 5:1 ratio.[5] It also occurs predominantly in people of Asian and African descent.[1] Although white individuals are least likely to develop Nevus of Ota, they are the most likely to develop malignant melanoma associated with this condition.[7]
Risk Factors
There are no known risk factors for Nevus of Ota. It is most commonly seen in the Japanese population[8] but can rarely present in the Indian and White populations.[6][8] Patients with Nevus of Ota are at risk for glaucoma and melanoma.[5] Those with Nevus of Ota extending into the eye have an increased risk of developing glaucoma (10% of patients) as invasion of melanocytes can block drainage of aqueous, leading to elevated intraocular pressures.[9] Malignant cutaneous or ocular melanoma may develop in these patients. 1/400 patients can develop uveal (typically choroidal) melanoma in the affected eye, and risk factors for malignant transformation include: related cutaneous or palatal melanocytosis (especially in the temple); scleral involvement of the superior, nasal, or temporal quadrants; choroidal melanocytosis; and diffuse iris melanocytosis .[10] [11]
General Pathology
Nevus of Ota is a form of dermal melanocytosis that produces hyperpigmentation of the eye and the surrounding adnexa along the V1/V2 trigeminal nerve distribution. The hyperpigmentation is seen as a bluish or brownish pigmentation of the eyes and/or on the face’s skin and lids.[5] On histopathology, excessive dendritic melanocytes can be found in affected tissues. These melanocytes can give rise to malignant melanoma.) [12] Cutaneous melanocytosis is a form of a blue nevus, most of which are thicker and more irregular than the lesions seen in melanocytosis. The common form of blue nevi lacks potential for malignant transformation, whereas the cellular type has low potential for evolution to melanoma. [13] [14]
Pathophysiology
Currently, there is no definitive cause of Nevus of Ota. Several hypotheses have been suggested:
- One hypothesis is that it is caused by failure of migration of melanocytes from neural crest cells to their normal location within the basal layer of the epidermis.[7] Genetic mutations have been noted, including receptor tyrosine kinase (c-KIT) positive, guanin nucleotide-binding protein G(q) subunit alpha (GNAQ) mutations, as well as activating GTpase RAS pathway mutations. Ubiquitin carboxyl-terminal hydrolase (BAP1) and tumor protein p53 (TP53) mutations have also been demonstrated on whole genome sequencing of the nevi during tumor evolution.[15]
- Additional hypothesized causes include previous radiation exposure and hormonal factors.[9]
Primary Prevention
There are no established preventative treatments for Nevus of Ota.
Diagnosis
Nevus of Ota is diagnosed clinically by physical exam that typically reveals unilateral hyperpigmented lesions within the V1/V2 trigeminal nerve distribution along the sclera, iris, eyelids, nose, forehead, cheeks, areas around the eye, or side of face.[9]
Diagnostic procedures
A complete ophthalmic examination including visual acuity testing and anterior and posterior segment examinations with measurement of intraocular pressures should be performed.
- Slit lamp biomicroscopy distinguishes between conjunctival and episcleral pigmentation and should be used to evaluate heterochromic irides and the eyelids. Gonioscopy may reveal hyperpigmentation of the angle structures.[10]
- Dilated ophthalmoscopy will demonstrate asymmetric hyperpigmentation of the choroidal vasculature and can show glaucomatous optic nerve cupping.[10]
- Ophthalmic ultrasound may reveal thickening of the vascular uveal layer.[10]
Dermoscopy, a noninvasive method that allows the in vivo evaluation of colors and microstructures of the epidermis, the dermoepidermal junction, and the papillary dermis not visible to the naked eye, allows closer examination of the involved epidermis.
Oral examination looking for palatal involvement should also be performed.[5]
Differential diagnosis
Ocular melanosis is a condition differentiated from Nevus of Ota by the absence of eyelid involvement.[9]
Nevus of Ito is a condition differentiated by involvement of hyperpigmentation of the neck, shoulders, axilla, and upper extremity.[9]
Nevus of Hori is a condition almost identical to Nevus of Ota, but this condition is bilateral on presentation, as opposed to the unilateral Nevus of Ota.[9]
Management
Disease processes associated with Nevus of Ota include glaucoma, malignant melanoma, and destruction of the dermis from dermatologic interventions.
General treatment
Ophthalmologic
Determination of the extent of ocular involvement requires vision screening, slit lamp exam, intraocular pressure, and gonioscopy for measurement and grading of the anterior chamber angle. Intraocular pressure and confrontational visual field testing should be monitored as some patients may develop open angle glaucoma even in the absence of elevated intraocular pressures.[16]
Surgical resection of melanocytosis lesions is not advised, however screening every 6 months for the development of malignant melanoma should also be done, using slit lamp biomicroscopy, and pupillary dilation for ophthalmoscopy. Melanoma treatment options include surgical resection based on the location, radiation therapy, enucleation, or transpupillary thermotherapy.[17] Consideration of tumor location, size, and patient comorbidities is necessary when deciding treatment. Iris melanomas have a good outcome, with a 5-year survival rate of greater than 95%. It is unclear if treatment of small choroidal melanomas prevents metastasis.[17]
Dermatologic
Treatment is usually not required unless for management of malignant transformation of periocular skin lesions or for cosmetic reasons.
If malignant transformation of the skin surrounding the eye occurs, a Mohs surgeon or an oculoplastic surgeon should be consulted to remove the lesions and reconstruct the periocular tissues. For more extensive lesions or metastatic disease, the combination of complete excision, adjuvant radiation therapy, or chemotherapy may be used.
The most effective approach for cosmetic treatment of skin lesions associated with Nevus of Ota is via laser therapy. This therapy’s mechanism of action is thought to work by destroying the melanocytes that mediate the bluish hyperpigmented sections on the skin. A study involving Q-switch alexandrite laser therapy (755 nm, 100 ns) with energy densities ranging from 4.75 - 7.0 J/cm2 at 8-12-week intervals was conducted. Results revealed that an average of only 2 laser treatments were required to see a 50% clinical improvement in participants. In addition, 5 out of the 7 participants showed a 100% lesional clearance after an average of 5 treatments.[18] There were also no recurrences of lesion, postinflammatory hyper/hypopigmentation, textural changes or scarring experienced in this patient group.[18] Dermatologic use of cosmetic products such as camouflaging creams, foundation, and concealers can mask discolorations, while some patients may opt for the use of chemical peels, dermabrasion with carbon dioxide, cryotherapy, or electrodissection.
Prognosis
Nevus of Ota is typically benign with an excellent ophthalmic and dermatologic prognosis with or without treatment. Yearly screening for glaucoma and malignant melanoma by an ophthalmologist and dermatologist is recommended.[5] However Shields et al found that patients with uveal melanoma associated with oculodermal melanocytosis have a twice as likely risk for metastasis compared to those without melanocytosis. [19]
Conclusion
Oculomucodermal melanocytosis (Nevus of Ota) is a benign dermal melanocytosis, that results in hyperpigmentation of the sclera and ipsilateral face. Presenting at birth or by adolescence, these lesions tend to remain unchanged throughout life but can darken overtime due to sun exposure. Although Nevus of Ota is a benign condition, patients do carry the risk of developing glaucoma and malignant cutaneous and/or ocular melanoma, and regular follow-up with ophthalmology and dermatology is recommended. While treatment is not typically required for the cutaneous lesions, it can be performed for cosmetic reasons, and patients should be aware of the treatment complications that can occur.
References
- ↑ 1.0 1.1 Rapini RP, Bolognia JL, Jorizzo JL. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. pp. 1720 22.
- ↑ Bhattacharya, S. K., Girgla, H. S., & Singh, G. (1973). Nevus of Ota. International Journal of Dermatology, 12(6), 344-347
- ↑ Kopf, A. W., & Weidman, A. I. (1962). Nevus of ota. Archives of Dermatology, 85(2), 195-208.
- ↑ Hori, Y., & Takayama, O. (1988). Circumscribed dermal melanoses: classification and histologic features. Dermatologic Clinics, 6(2), 315-326.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 Cronemberger, S., Calixto, N., & Freitas, H. L. (2011). Nevus of Ota: clinical-ophthalmological findings. Revista Brasileira de Oftalmologia, 70(5), 278-283.
- ↑ 6.0 6.1 Shetty SR, Subhash BG, Rao KA, Castellino R. Nevus of Ota with buccal mucosal pigmentation. Dent Resj (Isfahan) 2011 Winter, 8 (11) 52-5.
- ↑ 7.0 7.1 Shaffer, D., Walker, K., & Weiss, G. R. (1992). Malignant melanoma in a Hispanic male with nevus of Ota. Dermatology, 185(2), 146-150.
- ↑ 8.0 8.1 Redkar, N. N., Rawat, K. J., Warrier, S., & Jena, A. (2016). Nevus of Ota. Journal of the Association of Physicians of India, 64, 70.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 Hannan, C. (2018). Nevus of Ota: Treatment, Eye, Removal, Glaucoma, and More. Healthline. Retrieved at: https://www.healthline.com/health/nevus-of-ota
- ↑ 10.0 10.1 10.2 10.3 Finger, P. (2018). The Nevus of Ota. New York Eye Cancer Center. Retrieved at: https://eyecancer.com/eye-cancer/conditions/choroidal-tumors/nevus-of-ota/
- ↑ Shields CL, Qureshi A, Mashayekhi A, et al. Sector (partial) oculo(dermal) melanocytosis in 89 eyes. Ophthalmology 2011;118:2474-2479
- ↑ Shields JA, Shields CL, eds. Intraocular Tumors: An Atlas and Textbook. 2nd ed. Philadelphia,: Lippincott Williams and Wilkins, 2008:6-7
- ↑ Shields JA, Shields CL, eds. Eyelid, Conjunctival, and Orbital Tumors: An Atlas and Textbook. 2nd ed. Philadelphia: Lippincott Williams and Wilkins, 2008:100-8.
- ↑ Eagle, RC. Eye Pathology: An Atlas and Text. 2nd ed. Philadelphia: Lippincott Williams and Wilkins, 2011:251.
- ↑ Vivancos, A., Caratú, G., Matito, J., Muñoz, E., Ferrer, B., Hernández‐Losa, J., ... & Recio, J. A. (2016). Genetic evolution of nevus of Ota reveals clonal heterogeneity acquiring BAP 1 and TP 53 mutations. Pigment cell & melanoma research, 29(2), 247-253.
- ↑ Zeitz, O., Matthiessen, E.T., Reusss, J., Wiermann, A., Wagenfeld, L., Galambos, P., Richard, G., and Klemm, M. (2005) Effects of glaucoma drugs on ocular hemodynamics in normal tension glaucoma: a randomized trial comparing bimatoprost and latanoprost with dorzolamide. BMC Ophthalmology 5:6.
- ↑ 17.0 17.1 Shields CL, Shields JA, Perez N, et al.: Primary transpupillary thermotherapy for small choroidal melanoma in 256 consecutive cases: outcomes and limitations. Ophthalmology 109(2): 225-34, 2002.
- ↑ 18.0 18.1 Alster, T. S., & Williams, C. M. (1995). Treatment of nevus of Ota by the Q‐switched alexandrite laser. Dermatologic Surgery, 21(7), 592-596.
- ↑ Shields CL, Kaliki S, Livesey M, et al. Association of ocular and oculodermal melanocytosis with the rate of uveal melanoma metastasis: analysis of 7872 consecutive eyes. JAMA Ophthalmol 2013 Aug;131(8):993-1003.