Photokeratitis
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Photokeratitis, or Ultraviolet Keratitis, is a painful eye condition which can develop after unprotected exposure to Ultraviolet (UV) rays. Ultraviolet rays, from a variety of sources including welding arcs (arc eye, welder's eye) , reflections off snow (snow blindness), and germicidal UV lamps can damage the corneal epithelial cells and cause them to slough off after several hours. This is similar to having a "sunburn" of the eye. This leaves underlying corneal nerves exposed and damaged, causing symptoms of intense pain, photophobia, and foreign body sensation.
Disease Entity
ICD 10 Codes
- H16.131 right eye
- H16.132 left eye
- H16.133 bilateral
- H16.139 unspecified eye
Pathophysiology
The cornea is transparent and transmits light in the visible spectrum (400 nm to 700 nm), but will absorb light in the Ultraviolet spectrum (10 nm to 400 nm). Numerous animal studies have shown that the the corneal epithelium absorbs almost 100% of UV light below 290 nm (UV-C range). This epithelial UV absorption potentially serves a protective role for the underlying stroma and endothelium, but causes in the process damage and apoptosis which results in a delayed sloughing of the epithelium. [1]
Significant longer spectrum UV exposure has been shown to cause stromal and endothelial damage in animal models. [2]
The reason photokeratitis is painful is that the epithelium is preferentially damaged and sheds, leaving the underlying sub-epithelial nerve plexus exposed.[2]
Etiology and Risk Factors
Arc welding and light reflections from snow (particularly at high altitudes) remain the most classical examples of exposures for photokeratitis, but many other sources exist and have been reported. Below includes a list of potential sources of UV exposure in photokeratitis
- Arc welding
- Snow reflections
- Other recreational solar exposure
- Sun lamps
- Tanning beds
- Germicidal or laboratory UV lights
- Damaged metal halide lamps (can be found in gymnasiums) [3]
- Halogen lamp burst [4]
Exposure to UV at high altitude settings, such as mountain climbing in snow covered terrain, can be particularly intense and result in photokeratitis commonly known as snow blindness. This is due to a combination of factors. At higher altitudes, the atmosphere is thinner and there is less scattering of the UV rays. Snow terrain also has a increased albedo or reflection of radiation. Fresh fallen snow can carry a reflectance or albedo rate of up to 0.9 or 90% reflectance.[5]
Diagnosis
Signs and Symptoms
Delayed presentation from exposure is absolutely characteristic of photokeratitis. Anywhere from 30 minutes to 12 hours after an exposure to a source, patients will usually present with bilateral eye pain, photophobia, decreased vision, tearing, and will often have facial or eyelid erythema related to the UV exposure as well.
Physical Examination
Physical examination should reveal bilateral eye involvement. If unilateral, one could be suspicious of a corneal or tarsal foreign body or other causes of unilateral eye irritation and redness.
Typically, examination will reveal bulbar conjunctival injection and chemosis, with relatively sparing of the palpebral conjunctiva since UV exposure to those areas should be blocked by the eyelids. Epiphora (tearing), eyelid chemosis, and superficial facial burns may be apparent as well. Visual acuity can be normal to moderately decreased, and assessing visual acuity may be difficult without instillation of a topical anesthetic.
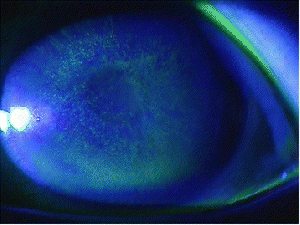
Instillation of fluoroscein dye will reveal punctate epithelial staining of the cornea, which in severe exposures may be coalescent. These areas of staining represent the corneal epithelium that has been damaged and sloughed off.
Differential Diagnosis
It is important to consider other conditions that can cause bilateral eye redness, irritation, and photophobia:
- Viral conjunctivitis - can be bilateral and cause similar findings, but typically one eye becomes involved first, and the conjunctival injection and chemosis would be prominent in the palpebral conjunctiva as well. With photokeratitis, you would expect a concurrent bilateral onset and relative sparing of the palpebral conjunctiva.
- Contact lens overwear - would expect contact lens history
- Dry eye - would see decreased tear lake, decreased tear breakup time, lack of UV exposure history
- Topical drug toxicity - consider sensitivity or toxicity to drops like brimonidine, neomycin, tobramycin, any topical medications with preservatives
- Chemical exposure - cleaning sprays, oven cleaners, other chemicals can cause similar symptoms and findings to photokeratitis
- Upper eyelid foreign body - usually unilateral, with vertical linear abrasions classically
Management
General Treatment
Treatment of photokeratitis is supportive, and similar to that of treatment of a corneal abrasion. The corneal epithelium should heal within 24-72 hours, and supportive measurements such as ointment, artificial tears, and oral analgesics can be used to treat symptoms until the cornea is re-epithelialized.
Topical antibiotic ointments such as erythromycin ointment can provide improved comfort and also may also prevent a bacterial super-infection. We recommend dosing erythromycin ointment 4 times a day for 2-3 days.
The use of topical NSAID drops such as ketorolac or diclofenac for pain relief remains controversial. A Cochrane systematic review in 2017 was unable to show clear benefit in topical NSAID use for traumatic corneal abrasions, and these drops are not as cost effective as oral analgesics. [7] Thus, we do not recommend the routine use of topical NSAIDs in most cases of photokeratitis.
Patching the eye has been shown to not be effective in the treatment of corneal abrasions, and can delay corneal healing, and is thus not recommended [8][9]
Usage of cycloplegics/mydriatics such as cyclopentolate or homatropine have not been shown to be effect in corneal abrasions, and are generally not recommended [10][11].
It is recommended that if the patient is a contact lens wearer, that they stay out of contact lenses until the cornea is healed.
Follow Up
Follow up should be arranged with an ophthalmologist within one to two days or initial diagnosis to ensure the resolution of signs and symptoms. Any new or worsening pain should be promptly re-evaluated.
There have been no long term follow up studies on photokeratitis, but it is known that prolonged or increased lifetime UV exposure can lead to other pathologies such as pterygium, erythema, malignant melanoma, and non-melanotic skin cancers.[12]
Prevention
Photokeratitis is a preventable disease with proper UV protection.
Patients with recreational UV exposure should wear proper fitting sunglasses that meet the American National Standards Institute (ANSI) sunglasses requirements and have appropriate UV blocking properties.[13]
Patients with occupational UV exposure such as welders should adhere to the standard protections outlined by the ANSI standards for Eye and Face Protectors and for Occupations and Educational Personal Eye and Face Protection Devices. For welders specifically, having a full face shield with adjustable shade levels is necessary for adequate protection.

Inuits from the artic region have classically fashioned snow goggles with thin slits in them, from materials such as caribou antler or driftwood, to help reduce the amount of UV exposure and prevent snow blindness.
References
- ↑ Podskochy, A. (2004). Protective role of corneal epithelium against ultraviolet radiation damage. Acta Ophthalmologica Scandinavica, 82(6), 714-717.
- ↑ 2.0 2.1 Bergmanson, J. P. (1990). Corneal damage in photokeratitis--why is it so painful?. Optometry and vision science: official publication of the American Academy of Optometry, 67(6), 407-413.
- ↑ Finn, L. E. (2016). Photokeratitis linked to metal halide bulbs in two gymnasiums—Philadelphia, Pennsylvania, 2011 and 2013. MMWR. Morbidity and mortality weekly report, 65.
- ↑ Mahadik, S., Mehta, M., & Saxena, M. (2014). Halogen lamp burst photokeratitis: a mass incidence. Journal of Evolution of Medical and Dental Sciences, 3(17), 4601-4605.
- ↑ Ambach, W., Blumthaler, M., & Schöpf, T. (1993). Increase of biologically effective ultraviolet radiation with altitude. Journal of Wilderness Medicine, 4(2), 189-197.
- ↑ Kwon, DH., Moon, JD., Park, WJ. et al. Ann of Occup and Environ Med (2016) 28: 3. https://doi.org/10.1186/s40557-015-0087-7
- ↑ Wakai, A., Lawrenson, J. G., Lawrenson, A. L., Wang, Y., Brown, M. D., Quirke, M., ... & Lang, E. (2017). Topical non‐steroidal anti‐inflammatory drugs for analgesia in traumatic corneal abrasions. Cochrane Database of Systematic Reviews, (5).
- ↑ Flynn CA, D'Amico F, Smith G. Should we patch corneal abrasions? A meta-analysis. J Fam Pract. 1998;47(4):264–270.
- ↑ Turner A, Rabiu M. Patching for corneal abrasion. Cochrane Database Syst Rev. 2006;(2):CD004764.
- ↑ Meek R, et al. Is homatropine 5% effective in reducing pain associated with corneal abrasion when compared with placebo? A randomized controlled trial. Emerg Med Australas. 2010;22(6):507–513.
- ↑ Carley F, Carley S. Towards evidence based emergency medicine: best BETs from the Manchester Royal Infirmary. Mydriatics in corneal abrasion. Emerg Med J. 2001;18(4):273.
- ↑ Tenkate, T. D. (1999). Occupational exposure to ultraviolet radiation: a health risk assessment. Reviews on environmental health, 14(4), 187-210.
- ↑ ANSI.Ophthalmics - Nonprescription Sunglass And Fashion Eyewear Requirements. ANSI.org. https://webstore.ansi.org/Standards/VC%20(ASC%20Z80)/ANSIZ802018?source=blog. Accessed December 2nd, 2019

