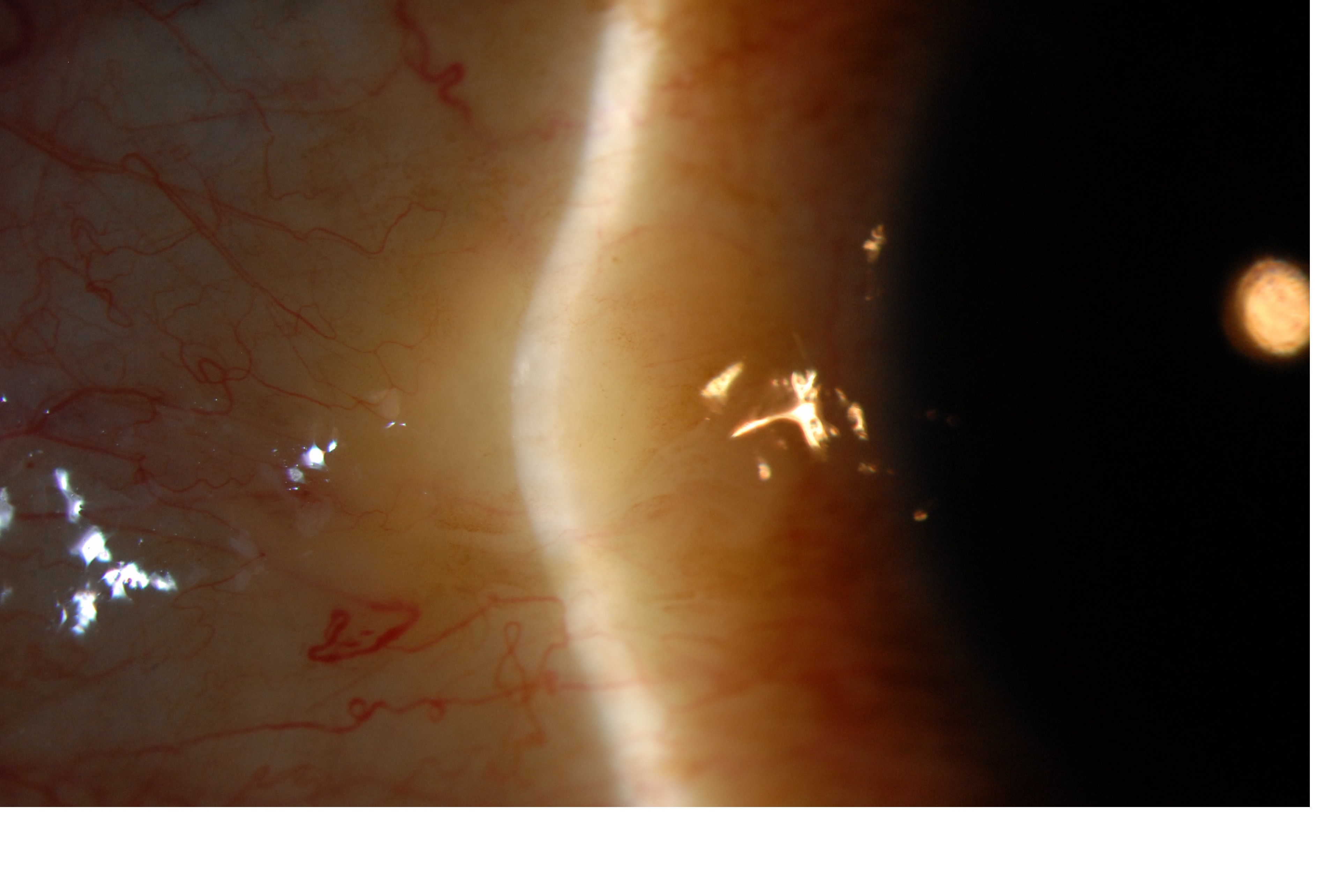
Pinguecula
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Pinguecula, plural pingueculae
Derived from the Latin word "pinguis" which means fat or grease[1]
ICD-9 Code 372.51
Disease Entity
A relatively common non-malignant, raised yellow-white lesion of the interpalpebral bulbar conjunctiva that does not involve the cornea and represents elastoic degeneration of subepithelial collagen with hyalinized connective tissue.[2] These fleshy lesions are typically found bilaterally and adjacent to the limbus of the nasal bulbar conjunctiva although they can be present temporally as well.
Etiology
Pingueculae are thought to arise as a result of the effects of environmental irritants such as wind and dust and are associated with UV-light exposure and aging, however the evidence of the association between UV-light exposure and pingueculae remains limited. [3] It is thought that both pteryigia and pingueculae arise more commonly on the nasal side because light passing medially through the cornea focuses on the area of the nasal limbus while the shadow of the nose reduces the intensity of light transmitted to the area of the temporal limbus.[2]
Risk Factors
UV-light exposure, wind, dust, outdoor lifestyle and proximity to the equator. age, male gender, smoking, working outdoors, diabetes mellitus [4]
General Histopathology
The finding of increased nuclear p53 in the limbal epithelium of pterygia, limbal tumors, and most pingueculae indicates the probable existence of p53 mutations in these cells as an early event in their development, which is consistent with their causation by UV radiation exposure[5]. Verhoeff elastic stain demonstrates degeneration of the elastoic tissue (stains for elastin but is not broken down by elastase) of subepithelial stromal collagen with hyalinized connective tissue.[2][6] The overlying epithelium is often thinned but may be hyperplastic or dysplastic.
Primary Prevention
Avoidance of UV-light exposure may decrease the incidence.[7]
Diagnosis
The diagnosis is usually made clinically by slit-lamp biomicroscopy. The classic growth is raised and yellow-white in color, found in the interpalpebral fissure and is more common nasally than temporally. The lesion may be highly vascularized and injected or associated with punctuate epithelial erosions or dellen (thinning of adjacent cornea due to drying).[8]
Physical Examination
See diagnosis
Signs
See diagnosis
Symptoms
Most pingueculae are asymptomatic but may cause ocular surface irritation including foreign body sensation, tearing, burning or itching. Some may find these lesions cosmetically unacceptable.
Diagnostic Procedures
Biopsy with histopathologic confirmation is not usually necessary but may be indicated for atypical cases where the diagnosis remains questionable. The thickness of the lesion can be monitored with anterior segment OCT.
Laboratory test
Not indicated
Differential diagnosis
- Conjunctival intraepithelial neoplasia (CIN)
- Limbal dermoid
- Conjunctival tumor (e.g., papilloma, nevus, melanoma)
Management
Lubrication with artificial tears and ointment can help with ocular surface irritation. Excision is indicated only when pingueculae are cosmetically unacceptable or when they become chronically inflamed or interfere with successful contact lens wear. Long-term use of topical steroid therapy should be discouraged due to adverse side-effects but can but used judiciously in patients with inflamed pingeuculae termed “pingueculitis”. Topical indomethicin has also been demonstrated at reducing symptoms of inflammation.[9]
Surgery
Laser photocoagulation and surgical excision of pingueculae have both been used successfully with similar cosmetic outcomes.[10]
A study of 30 patients showed surgical excision of symptomatic pinguecula with conjunctival autograft secured with fibrin glue improved not only cosmesis but also improved dry eye syndrome.[11]
Prognosis
Pingculae may grow slowly over time but are associated with minimal ocular morbidity.
One study showed that nasal corneal epithelial damage in inflamed pinguecula patients may be a stimulus for exaggerated wound repair causing the release of growth factors leading to growth of conjunctival epithelium onto the cornea. Inflamed pinguecula patients with impaired ocular surface lubrication and nasal corneal epithelial defects may be a subgroup of pinguecula patients who have a propensity to progress to pterygium.[12]
Additional Resources
- Boyd K, Lipsky SN. Pinguecula and Pterygium. American Academy of Ophthalmology. EyeSmart/Eye health. https://www.aao.org/eye-health/diseases/pinguecula-pterygium-list. Accessed March 21, 2019.
References
- ↑ http://medical-dictionary.thefreedictionary.com/pinguecula .
- ↑ 2.0 2.1 2.2 2.Weisenthal, Robert W, Afshari, Natalie A, Bouchard, Charles S, Colby, Kathyrn A, Rootman, David S, Tu, Elmer Y, 2013, External Disease and Cornea, AAO, BCSC, Chapter 12, Depositions and Degenerations.
- ↑ Yam JC, Kwok AK. Ultraviolet light and ocular diseases. Int Ophthalmol. 2013 May: 14(2)187-94
- ↑ 4.Mimura T, Obata H, Usui T, Mori M, Yamagami S, Funatsu H, Noma H, Amano S, Pinguecula and diabetes mellitus. Cornea. 2012 Mar;31(3):264-8.
- ↑ Dushku N, Reid TW, P53 expression in altered limbal basal cells of pingueculae, pterygia, and limbal tumors. Curr Eye Res. 1997 Dec;16(12):1179-92
- ↑ Machemer, Robert. Pterygium, Atlas of ophthalmology.com
- ↑ 9.Bergmanson JP, Söderberg PG, The significance of ultraviolet radiation for eye diseases. A review with comments on the efficacy of UV-blocking contact lenses. Ophthalmic Physiol Opt. 1995 Mar;15(2):83-91
- ↑ Ehlers, J.P, Shah, C.P, The Wills eye manual: office and emergency room diagnosis and treatment of eye disease. Lippincott Williams & Wilkins. 2008: (4.9) 66-67.
- ↑ Frucht-Pery J, Solomon A, Siganos CS, Shvartzenberg T, Richard C, Trinquand C. Treatment of inflamed pterygium and pinguecula with topical indomethacin 0.1% solution. Cornea. 1997 Jan;16(1):42-7
- ↑ Ahn SJ, Shin KH, Kim MK, Wee WR, Kwon JW, One-year outcome of argon laser photocoagulation of pinguecula. Cornea. 2013 Jul;32(7):971-5
- ↑ Jeong J, Rand GM, Kwon T, Kwon JW. The Improvement of Dry Eye Symptoms after Pinguecula Excision and Conjunctival Autograft with Fibrin Glue. J Ophthalmol. 2019;2019:6438157. Published 2019 Jun 9. doi:10.1155/2019/6438157
- ↑ Küçük E, Yılmaz U, Zor KR. Corneal Epithelial Damage and Impaired Tear Functions in Patients with Inflamed Pinguecula. J Ophthalmol. 2018;2018:2474173. Published 2018 Oct 31. doi:10.1155/2018/2474173