Sagging Eye Syndrome
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Disease
Sagging eye syndrome (SES) was first described by Rutar and Demer in 2009, as a potential leading cause of strabismus in older adult population as a combination of horizontal and vertical strabismus in addition to bilateral blepharoptosis (ptosis with high lid creases) and deepening of the sulcus.[1]SES should be differentiated from heavy eye syndrome (HES) which is an association of axial high myopia, esotropia, and hypotropia.[2]
In a recent study by Goseki et.al.[3] from 945 patients complaining of diplopia, most of them where between 60 and 80 years old, approx 31% had SES with ~60% female predominance. Interestingly, they found that the relative proportion of SES was just 4.7% in patients younger than 50 years but it increased to 60.9% in patients older than 90 years old. The cyclotorsion component of SES was present in 65% of patients.
Anatomy of pulleys system
Extraocular muscles (EOM) are surrounded by connective tissue that serve as a functional support and a mechanical pulley. The mechanical properties of pulleys are critical for the support and rotational properties of the eye. Histologic studies showed that each rectus pulley consists of an encircling ring of collagen located near the globe equator in tenon fascia, coupled to the orbital wall, adjacent EOMs, and equatorial Tenon fascia by bands containing densely woven collagen, elastin, and smooth muscle.[4]The pulleys inflect rectus and inferior oblique paths by the exact same way that the trochlea inflects the path of the superior oblique (SO) tendon. The global layer of each rectus EOM, passes through the pulley and becomes contiguous with the tendon to insert on the globe. The orbital layer, inserts on the pulley, not on the globe.[4]A dense band is present from the medial rectus to the inferior pulleys (MR–IR band) and from the medial rectus to the superior rectus pulleys (MR–SR band). Similarly, another dense band is found from the Superior rectus to the lateral rectus pulleys (LR–SR band).
Pathophysiology
The LR-SR band vertically supports the LR pulley against the downward force of the inferior oblique muscle to maintain the LR pulley’s vertical position. However, age-associated degeneration of the ligaments interconnecting the EOM pulleys permits inferior sag of the LR pulley, causing esotropia, cyclovertical strabismus, or both.[5]
| Age Related Distance Esotropia (ARDE)[6] | Cyclovertical Strabismus (CVS)[6] |
|---|---|
|
|
Diagnosis
History
There has been an increased awareness and diagnosis of these degenerative strabismic disorders after 2000.[7] The typical presentation in an older individual is one of gradual or subacute onset of diplopia. Per some observations, its is more common in Caucasian females.[5] Initially, most patients only notice intermittent binocular diplopia at long distances, such as in the theater or while driving. Over a period of several months, the diplopia becomes more constant and is noticed while driving, watching television, and in other long-distance vision situations. Typically, patients note that they do not have any diplopia at near. The remainder of the neurological examination should be normal, without any cranial neuropathies. Patients may also present with ductional deficits depending on the grade of muscle displacement.[5] In addition, patients may have had eyelid surgery, face lifting,[6] or even apparently uncomplicated refractive or cataract surgery.[6][8]
Physical Examination
External features
Adnexal signs such as: retraction of the upper eyelid into the superior orbit (superior sulcus deepening), aponeurotic blepharoptosis, floppy lower lids, and high upper eyelid crease.[1][5][8] The patients may also present with bilateral ptosis.
Sensorimotor exam[5]
- ARDE only: incomitant esotropia worse in distance and in side gaze with no strabismus or small phoria for near and no vertical deviation
- ARDE and CVS: incomitant esotropia with a small hypotropia in one side
- CVS only: hypotropia with no horizontal deviation
- Supdraduction deficit
- Normal horizontal duction range, and normal horizontal saccadic velocities
Magnetic Resonance Imaging (MRI)
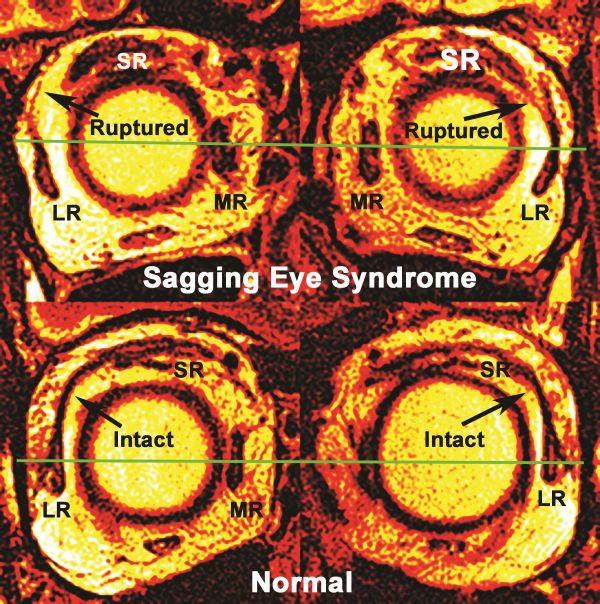
The use of MRI imaging is confirmatory rather than "required" to make the diagnosis, since diagnosis is mainly clinical. Chaudhuri and Demer used MRI to evaluate rectus EOMs, pulleys, and the LR-superior rectus (SR) band ligament in SES. Magnetic resonance imaging resolution showed superotemporal bowing of the LR-SR band in milder cases and abrupt termination of an attenuated band remnant in the superolateral orbit in more severe cases.[5] The ligament was ruptured in 64% of orbits with DPE and 91% of orbits with CVS. Also found significant displacement of all four rectus pulleys away from the orbital center, lateral displacement of the inferior rectus pulley and obliquely angulated lateral rectus pulley.[5]
MRI measurements of horizontal EOM lengths in SES were approximately 40%, or 14 mm, longer than the EOMs of nonstrabismic younger and older controls.[5]
In recent imaging studies, Patel et al. enlisted 100 patients without strabismus, and readers graded the LR-SR band visible in 95% of orbits on non-fat-suppressed coronal T1-weighted sequences, 68% on coronal STIR sequences. Typically, the band appears as an uninterrupted, arc-like structure extending from the lateral rectus to the superior rectus/levator palpebrae complex. Of note among this cohort of patients without strabismus, noncontinuous LR-SR bands were found in 5% of cases, and superotemporal bowing in 24% of cases. Results from this study also supported previously published evidence of normal age-related connective tissue degeneration as there was a positive age effect in correlation to supero-temporal bowing of the LR-SR band.[9]
Differential diagnosis
Differentiating sagging eye syndrome (SES) from other causes of strabismus is not always a straight forward task given that patients with SES may have risk factors for strokes or tumors. Usually the sensorimotor exam is helpful, as in SES the misalignment does not map similar to cranial nerve palsies or skew deviation. In addition, patients with SES usually have normal horizontal saccades and normal horizontal ductions. The differential includes:
- Cranial nerve palsy (Third, Fourth or Sixth nerves)
- Skew deviation
- Thyroid eye disease
- Myasthenia gravis
- Decompensated phoria
- Heavy Eye Syndrome
It can be difficult to adjudicate small angle deviations such as HES and SES from mild myasthenia gravis, incompletely resolved sixth nerve palsy, thyroid eye disease, and decompensated prior phorias. Depending on the clinical circumstances, the imaging, and the course, clinicians should consider evaluating for other etiologies prior to making the diagnosis of HES or SES.
Management
Observation
Since most of the patients have good fusional capacities they do not experience double vision for near with that said these patient can likely manage without the need for intervention.
Prism
Sagging eye syndrome rarely gives a deviation of more than 10 PD (Prisms Deviation) [5]. In spectacle-dependent patients, a temporary Fresnel prism or permanent ground in prism are usually helpful in managing the double vision for distance without inducing diplopia for near given their strong near fusional capacities as mentioned before. When patients are spectacle independent and want to remain independent, surgical approach could be offered.
Surgery
Patients with sagging eye syndrome can be treated surgically if they do not respond to or do not desire prism therapy. Different surgical approaches exist when dealing with the components of sagging eye syndrome including divergence insufficiency esotropia and cyclovertical strabismus.
A review in January 2020 supported the evidence that when the symptoms of diplopia are burdensome to the patient, surgery is the only treatment that can eliminate the misalignment almost 100%. In that study, strabismus surgery was performed in 50% of all SES cases. It was found that the mean distance-esotropia deviation in Prism was 6.9 ± 0.7 and it resolved to 0.3 ± 0.3 after surgery, while mean vertical deviation went from 3.0 ± 0.3 to 0.7 ± 0.2.
Some of the surgical techniques used for improvement on diplpia include: medial rectus recession (>4 mm ) if esotropia, vertical rectus surgery if comitant hypertropia, and inferior oblique recession for incomitant hypertropia plus excyclotorsion[10]. For more details, below.
Age Related Distance Esotropia (ARDE)
- Lateral Rectus Resection
In 2005 Thacker NM et al. published a case series of long-term follow up for 29 patients with divergence insufficiency esotropia underwent lateral rectus resection. Their patients all had satisfactory results, with no patients initially over-corrected or requiring additional prisms. However, they had a recurrence rate of almost 7% over their mean follow-up period of 39 months.[11] In 2013, Stager et al. reported a series of 57 patients underwent unilateral lateral rectus resection for distance esotropia deviations of 5–30Δ with 96.5 % did not require further surgery.[12]
- Medial Rectus Recession
Bothun and Archer reported a series of 8 patients who underwent bilateral medial rectus recessions for distance esotropias of 12–35Δ; 5 patients had satisfactory results with collapse of the distance-near deviation from 15Δ pre-operatively to 5Δ postoperatively.[13]Later Chaudhuri and Demer reported 24 patients and compared the results of those undergoing lateral rectus resection (n = 8) to those undergoing medial rectus recession (n = 16). They concluded that medial rectus recession is as effective as lateral rectus resection and suggested that double the distance angle of esotropia should be used as the surgical target.[14]In their case series patients with lateral incomitance, the adjustable suture was generally placed on the MR opposite the horizontal direction of the greatest ET.
Cyclovertical Strabismus (CVS)
- Selective tenotomy and plication
Chang MY et al. reported a case series of 9 patients with vertical strabismus incomitant in horizontal gaze positions and cyclotorsion who underwent Adjustable small-incision selective tenotomy and plication. 8 (89%) had successful with postoperative vertical alignment and 4 (50%) were successfully corrected, with <5° of cyclotorsion postoperatively. They concluded that these surgeries are less effective for correcting cyclotorsion in patients with restriction or prior strabismus surgery.[15]
- Graded Vertical Rectus Tenotomy (GVRT)
In 2015 Chaudhuri and Demer published a retrospective observational study about utilizing Graded Vertical Rectus Tenotomy (GVRT) for treating incomitant vertical misalignment. The procedure is performed under topical anesthesia in the presence of an anesthesiologist. Initial tenotomy 30% of tendon width was performed to avoid intraoperative overcorrection. Surgical effect was assessed immediately by sitting the patient up and repeating the measurements at near and distance. If hypertropia persisted, further 5%–10% increments of GVRT up to a maximum of 90% were added with monitoring of alignment. The inferior rectus (IR) was chosen when hypertropia was vertically concomitant or greatest in infraversion. The SR was chosen when hypertropia was greatest in sursumversion or absent in infraversion. Temporal GVRT was chosen for the IR and nasal GVRT for the SR. They concluded that GVRT performed with intraoperative monitoring under topical anaesthesia, precise correction of hypertropia up to 10Δ can be achievable.[16]Linear regression analysis of hypertropia correction with tenotomy showed that for a 3–6Δ hypertropia, a 30–90% tenotomy is recommended. In this study, they reiterate that a topical anesthesia with intra-operative re-assessment of deviation[16].
Due to the degenerative etiology of this syndrome, the connective tissue involution may progress after surgery, up to 20% of patients[16], therefore is important to inform the patient of this possibility prior to surgery.
Additional Resources
- American Academy of Ophthalmology. Committee on Aging. Heavy Eye vs. Sagging Eye Syndrome. https://www.aao.org/interview/heavy-eye-vs-sagging-eye-syndrome San Francisco: American Academy of Ophthalmology, 2020. Accessed May 05, 2020. -- Available for American Academy of Ophthalmology members
- American Academy of Ophthalmology. Committee on Aging. Sagging Eye Syndrome. https://www.aao.org/audio/sagging-eye-syndrome San Francisco: American Academy of Ophthalmology, 2022. Accessed January 24, 2022.
- American Academy of Ophthalmology. Clinical Update. Diplopia at Distance in Older Patients: Is It Sagging Eye Syndrome?, 2022. Accessed March 11,2026.https://www.aao.org/eyenet/article/diplopia-at-distance-in-older-patients- Available for American Academy of Ophthalmology members
- Neuro-Ophthalmology with Dr Andrew G. Lee, Sagging Eye Syndrome, https://www.youtube.com/watch?v=fgBb0TE1t4A and https://youtu.be/w5UKiYj3AC8.
References
- ↑ 1.0 1.1 Rutar T, Demer JL. “Heavy Eye” Syndrome in the Absence of High Myopia: A Connective Tissue Degeneration in Elderly Strabismic Patients. Journal of AAPOS : the official publication of the American Association for Pediatric Ophthalmology and Strabismus / American Association for Pediatric Ophthalmology and Strabismus. 2009;13(1):36-44. doi:10.1016/j.jaapos.2008.07.008.
- ↑ Demer JL et al. Heavy eye syndrome versus sagging eye syndrome in high myopia. Journal of American Association for Pediatric Ophthalmology and Strabismus {JAAPOS} , Volume 19 , Issue 6 , 500 - 506
- ↑ Goseki T, Suh SY, Robbins L, Pineles SL, Velez FG, Demer JL "Prevalence of Sagging Eye Syndrome in Adults with Binocular Diplopia." American Journal of Ophthalmology, Volume 209, January 2020, Pages 55-61. DOI: https://doi.org/10.1016/j.ajo.2019.09.006
- ↑ 4.0 4.1 Demer JL. More respect for connective tissues. J AAPOS. 2008;12(1):5–6.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 Chaudhuri Z, Demer JL. Sagging Eye Syndrome: Connective Tissue Involution as a Cause of Horizontal and Vertical Strabismus in Older Patients. JAMA ophthalmology. 2013;131(5):619-625. doi:10.1001/jamaophthalmol.2013.783.
- ↑ 6.0 6.1 6.2 6.3 Bradley J. Katz, MD; Joseph L. Demer, MD, PhD; Robert A. Clark, MD: Sagging Eye Syndrome. Audio blog post. American Academy of Ophthalmology. 2016.
- ↑ Repka MX and Eric Downing E. Characteristics and surgical results in patients with age-related divergence insufficiency esotropia. J AAPOS 2014;18:370-373
- ↑ 8.0 8.1 Demer JL. The Apt Lecture. Connective tissues reflect different mechanisms of strabismus over the life span. J AAPOS. 2014;18(4):309-15.
- ↑ Patel SH, Cunnane ME, Juliano AF, Vangel MG, Kazlas MA, Moonis G. Imaging appearance of the lateral rectus-superior rectus band in 100 consecutive patients without strabismus. AJNR Am J Neuroradiol. 2014;35(9):1830-5.
- ↑ Richards, Alan B. et al. Surgical techniques for sagging eye syndrome: avoiding lateral rectus surgeryJournal of the American Association for Pediatric Ophthalmology and Strabismus (JAAPOS), Volume 26, Issue 4, e29
- ↑ Thacker NM, Velez FG, Bhola R, Britt MT, Rosenbaum AL. Lateral rectus resections in divergence palsy: Results of long-term follow-up. J AAPOS. 2005;9:7–11.
- ↑ Stager DR, Sr, Black T, Felius J. Unilateral lateral rectus resection for horizontal diplopia in adults with divergence insufficiency. Graefes Arch Clin Exp Ophthalmol. 2013;251:1641–1644.
- ↑ Bothun ED, Archer SM. Bilateral medial rectus muscle recession for divergence insufficiency pattern esotropia. J AAPOS. 2005;9:3–6.
- ↑ Chaudhuri Z, Demer JL. Medial rectus recession is as effective as lateral rectus resection in divergence paralysis esotropia. Arch Ophthalmol. 2012;130:1280–1284
- ↑ Chang MY, Pineles SL, Velez FG. Adjustable small-incision selective tenotomy and plication for correction of incomitant vertical strabismus and torsion. Journal of AAPOS : the official publication of the American Association for Pediatric Ophthalmology and Strabismus / American Association for Pediatric Ophthalmology and Strabismus. 2015;19(5):410-416. doi:10.1016/j.jaapos.2015.07.290.
- ↑ 16.0 16.1 16.2 Chaudhuri Z, Demer JL. Graded Vertical Rectus Tenotomy For Small Angle Cyclovertical Strabismus in Sagging Eye Syndrome. Br J Ophthalmol. 2016 May ; 100(5): 648–651. doi:10.1136/bjophthalmol-2015-306783
- Chaudhuri Z, Demer JL. Long-term Surgical Outcomes in the Sagging Eye Syndrome. Strabismus. 2018 Jan 3:1-5. doi: 10.1080/09273972.2017.1421676. [Epub ahead of print] https://doi.org/10.1080/09273972.2017.1421676

