Sclerochoroidal Calcification
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Disease
Sclerochoroidal calcification (SCC) presents as flat or minimally elevated yellow placoid lesions, sometimes associated with gray lesions that are similar in appearance to senile scleral plaque.[1][2][3] SCC is rare and frequently misdiagnosed. The majority of cases are idiopathic and present with normal calcium-phosphorus metabolism and without associated ophthalmic or systemic conditions.[1]
Risk Factors
The majority of patients diagnosed with SCC are Caucasian and elderly.[1] There is a slight female predisposition (approximately 60% of cases).[4] Patients with previous systemic disorders that impact calcium-phosphorus metabolism are at higher risk of developing sclerochoroidal calcifications.[3] These include hyperparathyroidism, pseudohypoparathyroidism, parathyroid adenoma, chondrocalcinosis, sarcoidosis, Gitelman syndrome, Bartter syndrome, pseudo-gout, chronic renal disease, hypophosphatemia, hypervitaminosis, and metabolic imbalance after diuretic use.[1][3][5][6][7]
Etiology
Development of SCC can occur in 3 ways:
- Idiopathic,
- Dystrophic, and
- Metastatic.
Primarily, the pathogenesis of the disease is idiopathic.[1][3] Idiopathic presentation is seen in patients within the primary risk groups. Dystrophic calcification is seen following extensive tissue damage and/or chronic inflammation. Metastatic presentation is seen in patients with conditions that affect calcium-phosphorus metabolism.[1][3]
General Pathology
Calcium deposition begins in the sclera and expands to the choroid.[2] The white and yellow-colored calcium deposits manifest as yellow placoid lesions in diagnostic imaging. Lesions usually develop postequatorially and superotemporally; some have speculated that calcifications correspond to the insertion sites of the oblique extraocular muscles.[1][8] According to the literature, around half of the cases diagnosed are bilateral.[1][3] Lesions have been classified into 4 categories depending upon contour on optical coherence tomography:[6]
- Flat,
- Rolling,
- Rocky-rolling, and
- Table mountain.
Diagnosis
History
Because SCC often presents with minimal symptoms, it is often found during unrelated clinical exams.[6]
Symptoms
Patients are often asymptomatic and do not report ocular complaints.[2] Patients do not typically show a change in visual acuity. However, several case reports describe macular SCC associated with choroidal neovascularization or exudative retinal detachment, resulting in decreased visual acuity.[9][10][11] However, a large review of 179 eyes of 118 patients did not report hemorrhage, subretinal fluid, retinal pigment epithelial detachment, or choroidal neovascular membrane (CNVM) in any case.[3] A long follow-up (mean 4 years) of these cases did not show enlargement of the lesion, hemorrhage, subretinal fluid, CNVM, vision loss, or decalcification.[3] None of the cases needed treatment.[3]
Diagnostic Procedures
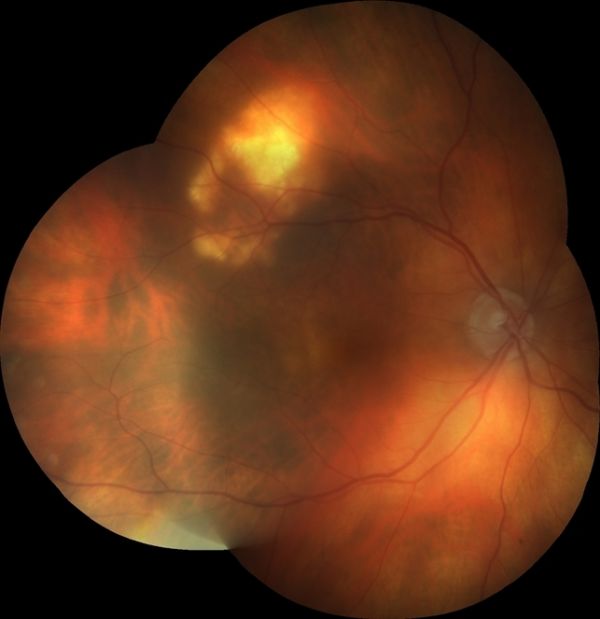
Ophthalmoscopy is sufficient for diagnosis. The fellow eye may also have a similar and symmetrical lesion. There may be multiple lesions, which, however, are typically localized near the superotemporal arcade or at the equator. There might be atrophy of the overlying choroid and/or retinal pigment epithelium.[3] The lesions may be arranged in a ring-like configuration. Calcifications can also be detected by B-scan ultrasonography, optical coherence tomography, orbital computed tomography, fundus autofluorescence, fluorescein angiography, and indocyanine green angiography.[4][6] Ophthalmoscopy can be unremarkable while ultrasound shows echogenic areas indicative of calcifications (hyperechoic lesion with acoustic shadow), due to deposition in the sclera not yet reaching the choroid.[2]
Laboratory Tests
Patients who are diagnosed with SCC should be screened for their calcium and phosphorus levels, complete blood count, and complete metabolic panel (paying attention to serum calcium and potassium) as well as magnesium, phosphorus, parathyroid hormone, blood pH, and urine calcium to distinguish from underlying systemic diagnoses.[1][5]
Differential Diagnosis
The differential diagnosis for SCC includes choroidal metastases, lymphoma, melanoma, nevus, choroidal hemangioma, choroidal osteoma, choroidal granuloma (tuberculosis, sarcoid), dysmorphic calcification, and chorioretinitis.[1][4][6][12] A distinguishing factor is that these lesions are choroidal, while SCC lesions are primarily scleral.[12] Choroidal osteoma is usually a solitary peripapillary lesion with sharp margins seen in young individuals, the ultrasonogram of which reveals calcification. There might be some areas of decalcification in longstanding choroidal osteomas. The risk of visual decline is higher, presumably due to the posterior location and association with the choroidal neovascular membrane.
Management
General Treatment
Parathyroid adenoma, Bartter, and Gitelman syndromes should be ruled out with testing due to complications associated with these diseases.[2] Patients should be advised to return annually for a dilated eye exam to monitor the progression of the lesions, although there is no treatment other than correcting any metabolic imbalances.
Prognosis
Calcifications are commonly misdiagnosed, leading to unnecessary testing and referrals to retinal specialists.[1][4] Lesions are typically located away from the macula and rarely encroach on the fovea. Therefore, visual prognosis in patients is good, and visual acuity usually remains unchanged.[2]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 Honavar SG, Shields CL, Demirci H, & Shields JA. Sclerochoroidal calcification: clinical manifestations and systemic associations. Arch Ophthalmol. 2001;119(6), 833-840. doi:10.1001/archopht.119.6.833.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Shields JA, Shields CL. CME Review: Sclerochoroidal calcification. Retina. 2002;22(3):251-261. doi:10.1097/00006982-200206000-00001.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 3.9 Shields CL, Hasanreisoglu M, Saktanasate J, Shields PW, Seibel I, Shields JA. Sclerochoroidal calcification. Retina. 2015;35(3):547-554. doi:10.1097/iae.0000000000000450.
- ↑ 4.0 4.1 4.2 4.3 Thomson AC, Brown GT, Dolores-Rodriguez A, Hunter AA. A case of extensive bilateral idiopathic sclerochoroidal calcification and review of the literature. Int Med Case Rep J. 2021; 14:749-755. doi:10.2147/imcrj.s336237.
- ↑ 5.0 5.1 Bourcier T, Blain P, Massin P, Grünfeld J-P, Gaudric A. Sclerochoroidal calcification associated with Gitelman syndrome. Am J Ophthalmol. 1999;128(6):767-768. doi:10.1016/s0002-9394(99)00277-9.
- ↑ 6.0 6.1 6.2 6.3 6.4 Hasanreisoglu M, Saktanasate J, Shields PW, Shields CL. Classification of sclerochoroidal calcification based on enhanced depth imaging optical coherence tomography “mountain-like” features. Retina. 2015;35(7):1407-1414. doi:10.1097/iae.0000000000000468.
- ↑ Sun H, Demirci H, Shields CL, Shields JA. Sclerochoroidal calcification in a patient with classic Bartter’s syndrome. Am J Ophthalmol. 2005;139(2):365-366. doi:10.1016/j.ajo.2004.07.054.
- ↑ Sivalingam A, Shields CL, Shields JA, Arch McNamara J, Jampol L, Wood W, Daubert G. Idiopathic sclerochoroidal calcification. J Ophthalmol. 1991;98(5):720-724. doi:10.1016/s0161-6420(91)32228-0.
- ↑ Lee H, Kumar P, Deane J. Sclerochoroidal calcification associated with Albright's hereditary osteodystrophy. BMJ Case Rep. 2012;2012:bcr0320126022. doi:10.1136/bcr-03-2012-6022.
- ↑ Cohen SY, Guyot-Sionnest M, Puech M. Choroidal neovascularization as a late complication of hyperparathyroidism. Am J Ophthalmol. 1998;126:320–2
- ↑ Leys A, Stalmans P, Blanckaert J. Sclerochoroidal calcification with choroidal neovascularization. Arch Ophthalmol. 2000;118:854–7.
- ↑ 12.0 12.1 Fung AT, Arias JD, Shields CL, Shields JA. Sclerochoroidal calcification is primarily a scleral condition, as shown by enhanced depth imaging optical coherence tomography. JAMA Ophthalmol. 2013;131(7):960. doi:10.1001/jamaophthalmol.2013.67.

