Trichoepithelioma
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Trichoepithelioma
Disease
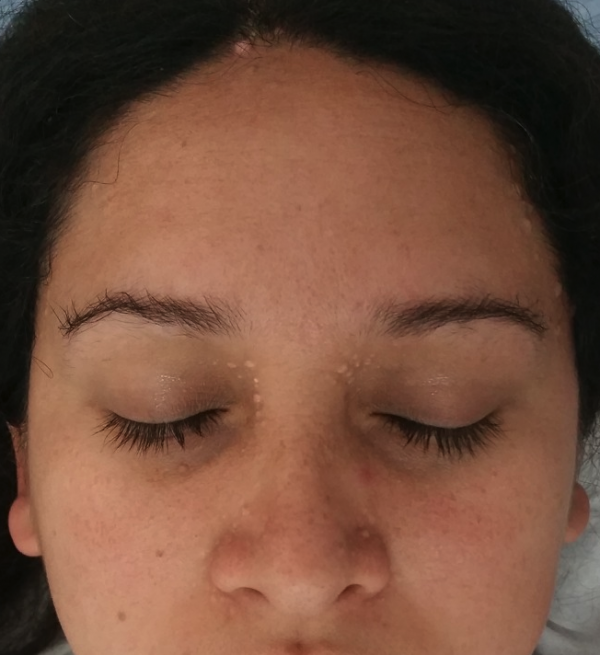
Trichoepithelioma is a rare benign adnexal neoplasm originating from basal cells of hair follicles. They may appear as solitary or multiple nodules most commonly on the face, though solitary lesion isolation to the eyelid is exceedingly rare[2][3][4]. There is potential, though uncommon, for malignant transformation most commonly to basal cell carcinoma, thus accurate diagnosis and treatment is necessary[2][5][6][7][8].
The disease was first recognized by Headington and French in 1962 as a “trichogenic adnexal tumor.” It has since then been known by a variety of names (Brooke-Fordyce trichoepitheliomas, EAC, epithelioma adenoids cysticum of Brooke, familial multiple trichoepitheliomata, multiple familial trichoepithelioma, hereditary multiple benign cystic epithelioma, MFT) with minimal reported cases due to its rare occurrence[9].
Etiology
Trichoepithelioma can be classified into three categories: solitary, multiple, and desmoplastic. In the United States, trichoepithelioma has been reported as approximately 2.75 cases per year in one dermatopathology laboratory[4].
Solitary nodules are least common, with eyelid involvement being exceedingly rare. They do not follow an inheritance pattern and tend to develop on the face of middle-aged individuals[2]. It has been suggested that mutations in human patched (PTCH) gene is involved in the pathogenesis. The PTCH gene normally functions as a tumor suppressor that provides regulatory feedback for the sonic hedgehog pathway[10].
Though extremely rare, solitary trichoepithelioma of the eyelid can occur. According to Simpson et al., who presented the largest study on eyelid trichoepitheliomas, 18 cases have been reported over thirty years. It was found that eyelid trichoepithelioma is twice as prevalent in males between the ages of 3-73 years (mean age 48.6 years). In addition, the upper eyelid was twice as likely to develop trichoepithelioma than the lower eyelid[11].
Multiple nodular trichoepitheliomas are the most common and often are part of systemic disease such as Multiple familial trichoepithelioma, Spiegler-Brookler syndrome, Rombo Syndrome and Cowden syndrome, with Multiple familial trichoepithelioma and Spiegler-Brookler syndrome being the most common[2][3][4][9]. Mutations in the cylindromatosis oncogene (CYLD) is responsible for Brooke-Spiegler syndrome and multiple familial trichoepithelioma in an autosomal dominant fashion. The CYLD gene normally functions as a tumor suppressor, producing a deubiquinating enzyme that negatively regulates NF-kappaB and c-Jun N-terminal kinase pathways[12]. Despite the autosomal dominant inheritance, there is decreased penetrance and expressivity in men[3]. Almost all CYLD gene mutations are located in exons 9 through 20, with missense and nonsense mutations having high and low phenotypic variation, respectively[13][14].
The desmoplastic variant has no known genetic loci.
Pathophysiology
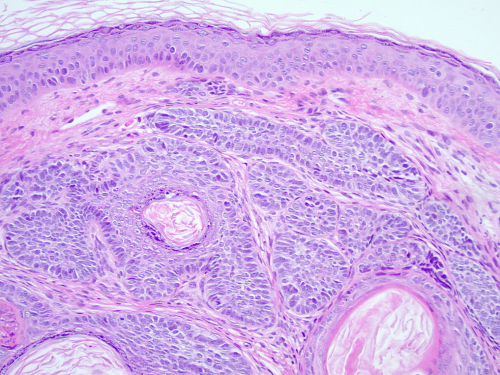
Trichoepithelioma originate from a benign proliferation of epithelial-mesenchymal origin cells (basal cells) of hair follicles[2][15]. On gross examination, the specimen is grayish-white to grayish-yellow without any areas of hemorrhage, necrosis or evidence of ulceration. Histologically, it is of dermal origin with numerous well-formed keratinous cysts, lacy cell pattern, dense fibromyxoid stroma, minimal inflammation in the absence of rupture, absence of abnormal hair follicles, absence of mitotic figures in basaloid cells[2]. The presence of a papillary-mesenchymal body are associated with benign follicular differentiation. Immunohistology with collagen IV and laminin reveals a continuous layer of basement membrane. Spindle cells surrounding trichoepithelioma cells stain strongly with CD34, while only the blood vessels within BCC do. Outer cells of trichoepithelioma islands stain strongly with bcl-2, while all cells in BCC stain[4][16]. Furthermore, CD10 has been demonstrated to be positive in trichoepithelioma stroma, while positive in basaloid cells of BCC[17]. The desmoplastic variant is differentiated by its desmoplastic stroma and surrounding dense fibrous tissue[18].
Due to potential of malignant transformation into basal cell carcinoma and its similar presentation, differentiating between the two is critical as biopsy and margin approach differences due to misdiagnosis can have prognostic and aesthetic implications[15]. On presentation, BCC presents as a shiny, neutral-colored, raised papule with telangiectasias and central ulcerations. The borders are often rolled with a crusted, ulcerated center. Conversely, trichoepithelioma is a benign, firm, non-tender, flesh colored nodule that is mobile. There is no presence of hemorrhage, telangiectasias, ulceration, or necrosis[2]. On histology, BCC originate from the epidermal basal cell layer with ulceration, fewer keratinous cysts, clefting, minmal stroma, dense inflammation, and adenoid and cystic tumor lobules[2]. Immunohistochemical differences are described above.
Diagnosis
Preliminary diagnosis may be made based on history and clinical appearance. Definitive diagnosis depends on histopathologic exam of a lesion after biopsy.
- Patients will present with a slow growing small (typically <1cm), painless, firm, mobile nodule or papule that do not ulcerate
- Depending on location, mass effect may cause dermatochalasis, ectropion, and compromised vision
- Trichoepitheliomas are most commonly found on scalp, nose, forehead, eyelids, but have been reported in the upper trunk, and buttocks[2][3][9][20]
- The desmoplastic variant presents as an isolated, firm, annular lesion with raised borders that do not ulcerate[21]
If multiple nodules are present, if the patient is very young, or if family history reveals multiple family members with nodules, genetic testing is indicated.
Differential diagnosis
- Basaloid Epithelioma
- Basal Cell Carcinoma
- Cylindroma
- Syringoma
- Epidermoid cyst
- Sebaceous hyperplasia
- Microcystic adnexal carcinoma
- Trichoadenoma
- Tumor of follicular infundibulum
- Basaloid follicular hamartoma
- Trichilemmoma
- Trichofolliculoma
- Trichilemmal Cyst (Pilar Cyst)
Management
Various management techniques have been proposed for trichoepithelioma. When feasible, all lesions should be removed through surgical excision with a 2mm margins (with 3-4mm margins if concerned for basal cell carcinoma), including subcutaneous tissue deep to the tumor. Due to its predilection for the face along with its similarity to BCC, Mohs micrographic surgery can be used to ensure surgical margins as well as optimal cosmetic outcome. Other proposed procedures include split-thickness skin grafting, dermabrasion, electro-surgery, and laser surgery, though the results of these procedures are inconsistent[22].
As trichoepithelioma can have rare but aggressive malignant transformation, adequate surgical excision and histopathological examination is necessary[23][20][4].
Non-surgical techniques such as argon laser ablation and cryotherapy have been reported in some cases of trichoepithelioma, but excision of the nodule is by far the more preferred procedure. With more extensive surgical excision (particularly in MFT or syndromic trichoepithelioma), skin grafting may be required for improved surgical and cosmetic results.[3]
Prognosis
Prognosis for trichoepithelioma is very good in most cases. For solitary nodules, recurrence after excision is very rare. However, there are reports of occasional transformation to high-grade carcinomas and mixed (epithelial or sarcomatous tumors). Inherited trichoepitheliomas such as Multiple familial trichoepithelioma can transform into an aggressive, recurrent carcinoma with ulcerations.[2][4]
Complications
Depending on the number of nodules and the location, removal may lead to disfigurement and scarring especially if involving the face. There have also been reports of facial lesions re-growing into elevated papules or nodules after surgical flattening with dermabrasion or laser therapy. In addition, partial removal of the tumor may also instigate persistence or recurrence.
References
- ↑ Kuo DS, Nyong'o OL. Congenital solitary eyelid trichoepithelioma. Journal of American Association for Pediatric Ophthalmology and Strabismus. 2010 Jun 1;14(3):277-9.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 Gupta A, Ali MJ, Mishra DK, Naik MN. (2015). Solitary Trichoepithelioma of the Eyelid: A Clinico-Pathological Correlation. International journal of trichology. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4502481/. Accessed July 24, 2019.
- ↑ 3.0 3.1 3.2 3.3 3.4 Mohammadi AA, Seyed Jafari SM. (2014). Trichoepithelioma: a rare but crucial dermatologic issue. World journal of plastic surgery. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4236999/. Accessed July 24, 2019.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Votruba M, Collins CM, Harrad RA. (1998). The management of solitary trichoepithelioma versus basal cell carcinoma. Eye (London, England). https://www.ncbi.nlm.nih.gov/pubmed/9614515. Accessed July 24, 2019.
- ↑ Samaka RM, Bakry OA, Seleit I, Abdelwahed MM, Hassan RA. Multiple familial trichoepithelioma with malignant transformation. Indian journal of dermatology. 2013 Sep;58(5):409.
- ↑ Martinez CA, Priolli DG, Piovesan H, Waisberg J. Nonsolitary giant perianal trichoepithelioma with malignant transformation into basal cell carcinoma: report of a case and review of the literature. Diseases of the colon & rectum. 2004 May 1;47(5):773-7.
- ↑ Pariser RJ. Multiple hereditary trichoepitheliomas and basal cell carcinomas. Journal of cutaneous pathology. 1986 Apr;13(2):111-7.
- ↑ Ayhan M, Adanali G, Senen D, Gorgu M, Erdogan B. Rarely seen cutaneous lesions in an elderly patient: malignant transformation of multiple trichoepithelioma. Annals of Plastic Surgery. 2001 Jul 1;47(1):98-9.
- ↑ 9.0 9.1 9.2 Multiple familial trichoepithelioma - Genetics Home Reference - NIH. U.S. National Library of Medicine. https://ghr.nlm.nih.gov/condition/multiple-familial-trichoepithelioma#genes. Accessed July 24, 2019.
- ↑ Matt D, Xin H, Vortmeyer AO, Zhuang Z, Burg G, Böni R. Sporadic trichoepithelioma demonstrates deletions at 9q22. 3. Archives of dermatology. 2000 May 1;136(5):657-60.
- ↑ Simpson W, Garner A, Collin JR. Benign hair-follicle derived tumours in the differential diagnosis of basal-cell carcinoma of the eyelids: a clinicopathological comparison. British journal of ophthalmology. 1989 May 1;73(5):347-53.
- ↑ Blake PW, Toro JR. Update of cylindromatosis gene (CYLD) mutations in Brooke‐Spiegler syndrome: novel insights into the role of deubiquitination in cell signaling. Human mutation. 2009 Jul;30(7):1025-36.
- ↑ Jia WX, Li WR, Wu YD, et al. A de novo missense mutation of the CYLD gene with multiple familial trichoepithelioma. Clin Exp Dermatol. 2021;46(4):792-794. doi:10.1111/ced.14515
- ↑ Parren, L.J.M.T., Giehl, K., van Geel, M. et al. Phenotype variability in tumor disorders of the skin appendages associated with mutations in the CYLD gene. Arch Dermatol Res310, 599–606 (2018). https://doi.org/10.1007/s00403-018-1848-2
- ↑ 15.0 15.1 Gray HR, Helwig EB. (1963). Epithelioma adenoides cysticum and solitary trichoepithelioma. Archives of dermatology. https://www.ncbi.nlm.nih.gov/pubmed/13949982?dopt=Abstract. Accessed July 24, 2019.
- ↑ 16.0 16.1 Kuo DS, Nyong'o OL. (2010). Congenital solitary eyelid trichoepithelioma. Journal of AAPOS: the official publication of the American Association for Pediatric Ophthalmology and Strabismus. https://www.ncbi.nlm.nih.gov/pubmed/20603064. Accessed July 24, 2019.
- ↑ Pham TT, Selim MA, Burchette Jr JL, Madden J, Turner J, Herman C. CD10 expression in trichoepithelioma and basal cell carcinoma. Journal of cutaneous pathology. 2006 Feb;33(2):123-8.
- ↑ Carter JJ, Kaur MR, Hargitai B, Brown R, Slator R, Abdullah A. Congenital desmoplastic trichoepithelioma. Clinical and Experimental Dermatology: Clinical dermatology. 2007 Sep;32(5):522-4.
- ↑ Kuo DS, Nyong'o OL. Congenital solitary eyelid trichoepithelioma. Journal of American Association for Pediatric Ophthalmology and Strabismus. 2010 Jun 1;14(3):277-9.
- ↑ 20.0 20.1 Lee KH, Kim JE, Cho BK, Kim YC, Park CJ. (2008). Malignant transformation of multiple familial trichoepithelioma: case report and literature review. Acta dermato-venereologica. https://www.ncbi.nlm.nih.gov/pubmed/18176750. Accessed July 24, 2019.
- ↑ Carter JJ, Kaur MR, Hargitai B, Brown R, Slator R, Abdullah A. Congenital desmoplastic trichoepithelioma. Clinical and Experimental Dermatology: Clinical dermatology. 2007 Sep;32(5):522-4.
- ↑ Raghuveer C, Murthy C, Siddalingappa K, Shivanand DR. Multiple trichoepitheliomas: Cosmetic improvement with dermabrasion. Journal of cutaneous and aesthetic surgery. 2011 Jan;4(1):68.
- ↑ Karikal A, Shetty P, Karikal A, Shetty SR. (2013). Multiple trichoepitheliomas: A rare occurrence. South Asian journal of cancer. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3876652/. Accessed July 24, 2019.

