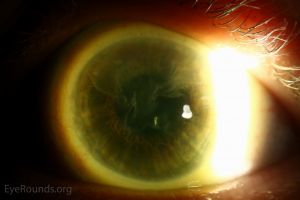
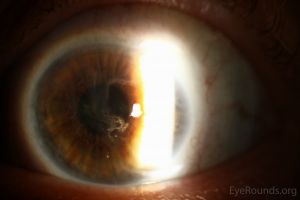
Contact Lens-Induced Limbal Stem Cell Deficiency
Disease Entity
Disease
Limbal stem cells (LSCs) are a vital set of cells that reside in the basal limbal region, serving as both a source of progenitor cells that differentiate to replenish corneal epithelium and as part of the limbal barrier between the conjunctiva and cornea.[1][2] Loss or dysfunction of these cells can lead to the inability to repair and renew corneal epithelium, a pathology known as Limbal Stem Cell Deficiency (LSCD). This can ultimately result in pathologic changes such as persistent epithelial defects, corneal conjunctivalization, neovascularization, and scarring.[2] Among the variety of etiologies that can cause LSCD is contact lens (CL)-induced LSCD, an often asymptomatic cause of LSCD.[3]
Epidemiology
An estimated 45 million people in the United States wear contact lenses (CL), among which two-thirds are female.[4] Of these 45 million people, it is estimated that 2.4-5%[5][6] of CL wearers may develop LSCD ranging from subclinical signs to symptomatic disease. It has also been reported that 15% of all cases of LSCD can be attributed to CL use.[7] The vast majority of studies focus on exclusive soft CL use induced LSCD[3][6][8] but LSCD can also develop in patients in rigid gas permeable (RGP) lenses[9] and poorly fitted scleral lenses.[10]
The duration of CL use has been demonstrated to have a positive correlation with LSCD.[3] In a review article, Rossen et al report that the mean duration of CL use associated with LSCD is 14.2-17.6 years with daily use of 12.5-16.25 hours.[3] Given that CL use is most commonly bilateral, disease presentation is also generally bilateral. However, asymmetry is often present and the fellow eye may have subclinical disease.[8][11][12] Early diagnosis is important as patients are often asymptomatic initially and can benefit from early medical management; soft CL wearers would benefit from annual screening examinations.[11]
While female wearers represent the majority of CL wearers in the US, there is a disproportionately higher rate of CL-induced LSCD among women, with studies estimating 67-93% of CL-induced LSCD cases being in women.[6][8][11] It is possible that this may have correlation with the higher prevalence of dry eye secondary to differences in hormonal factors in women, however this still requires further investigation.[8][11]
Pathogenesis
Mechanical Trauma
Contact lenses can induce mechanical trauma on the ocular surface as even properly fitted lenses may move 0.1-0.4mm with blinking.[13] The movement of the lens against the eyes during blinking can induce friction as tears are dispelled from the interface between the lens and ocular surface.[14] The superior limbus can become a site of chronic trauma because of the higher pressure experienced during blinking.[6][11][15] Conversely, the reduced eyelid pressure in the inferior limbus leads to less trauma and this may be an explanation for why CL-induced LSCD is less often inferiorly located.[6] Differences in eye and eyelid anatomy such as physiologically dryer eyes and narrower palpebral apertures which are more often found in Asian populations may also contribute to increased mechanical trauma from contact lens use.[13][16][17]
Dry Eye
Tear film stability is susceptible to disruption by CLs via multiple mechanisms including the lipid layer thinning, delayed tear film spread, osmolarity changes, and compositional changes (e.g. amounts of antioxidants, glycocalyx, mucin, protein, lipids, neutrophils).[18] While it is difficult to elucidate how the characteristics of different CLs (e.g. lens fit, lens design, material, etc.) affect specific elements of the tear film, it is clear that these changes in the tear film further enable the adverse effects of mechanical trauma induced by CL wear.[3]
Lens Disinfecting Solutions/Preservatives
Though phased out in the 1980s, the use of the preservative thimerosal in lens cleaning solution has been documented to cause a range of corneal pathology such as superior limbic/diffuse keratoconjunctivitis, keratitis, and pseudodendritic lesions.[9][19][20] More recently, studies comparing solutions with polyhexamethylene biguanide (PHMB) preservatives to hydrogen peroxide-based solutions have detected more corneal staining in the solutions that contain preservative.[21] However, despite using the same solution for both CLs, patients often present with asymmetric LSCD which suggests that factors beyond the preservatives such as underlying differences in the ocular surface, contact lens material and other ingredients in the lens disinfecting solutions may play a contributory role in LSCD pathogenesis.[21][22]
Hypoxia
The avascular corneal tissue receives part of its oxygen supply from the atmosphere and the use of CLs sets up a hypoxic environment that impedes corneal oxygenation.[23] This is evidenced by the increase in lactate dehydrogenase levels found in the tear film of CL wearers.[23] As with the increased pressures experienced in the superior limbus during blinking, there is a relative increase in hypoxia in this region as well, further exacerbating the detrimental effects of mechanical trauma from CL wear.[5][11][15]
Multifactorial Pathogenesis
Given the broad range of disease severity and asymmetric presentation in bilateral CL wearers, it is likely that the aforementioned issues work in tandem as part of a multifactorial pathway in the pathogenesis of CL-induced LSCD. Rossen et al. proposed a three part mechanism in which 1) the loss of lubrication from the tear film leads to increased friction and limbal trauma, 2) the ocular surface subsequently experiences prolonged exposure to disinfecting solutions and preservatives because of less irrigation from the tear film, and 3) increased inflammation from desiccation, hyperosmolar changes and hypoxia.[3] These factors may also contribute to different degrees in individual patients as some patients have localized disease to the superior cornea which may be attributable to mechanical trauma while others have 360-degree disease that may more likely point towards solution toxicity.[3] It is also possible that some of the epidemiological differences in underlying risk factors described earlier may be contribute a “first hit” in a two-hit hypothesis proposed by Chan and Holland.[8]
Diagnosis
History
Patients are commonly asymptomatic at initial presentation (71.4% in a retrospective study of CL-induced LSCD with corneal conjunctivalization)[6] but symptomatic individuals may experience nonspecific symptoms including decreased vision, tearing, irritation, pain, photophobia, blepharospasm, redness, dryness.[6][8][9][11]
Impression cytology, anterior segment ocular coherence tomography (AS-OCT), and OCT- angiography (OCT-A) have all been utilized in the diagnosis of LSCD.[24]
In a study by Shen et al., clinical and imaging features were used to classify CL-induced LSCD severity[25]:
· Mild cases showed localized late fluorescein staining at the superior limbus, minimal epithelial thinning on anterior segment OCT (AS-OCT), and slightly decreased basal epithelial cell density on confocal microscopy[25].
· Moderate cases exhibited more extensive late fluorescein staining across the limbus and peripheral cornea, noticeable epithelial thinning, and moderate loss of basal epithelial cells and nerve fibers[25].
· Severe cases presented with diffuse and dense late fluorescein staining, marked epithelial thinning or loss on AS-OCT, severe reduction in basal epithelial cells, and significant nerve damage on confocal imaging[25].
Differential Diagnosis
Superior Limbic Keratoconjunctivitis (SLK)
SLK shares much overlap with LSCD as both conditions demonstrate limbal inflammation and superficial punctate keratitis, specifically in the region of the superior limbus.[3] Moreover, trauma and dry eye both play a contributory role in the pathogenesis of both conditions.[19] However, SLK more consistently presents bilaterally and is associated with thyroid dysfunction rather than contact lens usage.[3] Medical treatment with large diameter bandage CL or surgical treatment with superior perilimbal conjunctival resection with or without cauterization can lead to resolution of SLK.[3][26]
CL-induced peripheral neovascularization
Peripheral neovascularization of up to 1-2mm of the cornea in the absence of changes in the corneal epithelium can be considered normal in CL wearers.[27][28] Although this neovascularization occurs from hypoxia, inflammation and subsequent edema, there should not be changes in the epithelium without co-existing LSCD.[28][29]
Conjunctival/corneal intraepithelial neoplasia (CIN)
Neovascularization can also be seen in CIN which commonly presents as a raised, circumscribed vascularized growth.[3] It can be distinguished from CL-LSCD with exfoliative or impression cytology which will demonstrate hyperplastic, dysplastic or anaplastic cells.[30]
Other causes of neovascularization
Causes of neovascularization that are not related to CL use include infections, inflammatory conditions, congenital disease (i.e. aniridia), degenerative disease and trauma.[27]
Management
Conservative Management
Contact Lens Discontinuation/Change
The most immediate treatment available for CL-induced LSCD is the complete discontinuation of contact lens use. Studies report widely varying outcomes with CL use cessation, with Jeng et al reporting that 11 of 18 eyes stabilized or improved with this treatment while 12 of 12 patients with severe disease failed conservative management in another study.[8][11] Therefore, it is likely that cessation alone is not always sufficient to treat LSCD, particularly in those suffering from severe disease.
After resolution of the CL-induced LSCD, it may be permissible to return to soft CL use. Consideration should be given to the possible contributing factor(s) of the lens (e.g., lens type, fit, cleaning solution, etc.) and changes should be made accordingly. Scleral lenses that can vault the limbus help to avoid limbal trauma and can play a therapeutic role in managing CL-induced LSCD.[3] In a recent study of 31 eyes fitted with Prosthetic Replacement of the Ocular Surface Ecosystem (PROSE) scleral devices, Kim et al noted improvement in best-corrected distance visual acuity (BCVA) and in corneal epithelial defects but did not note any significant differences in other corneal findings such as conjunctivalization or neovascularization.[31]
Dry Eye Treatment
As discussed earlier, CL use can disrupt the tear film and lead to dry eye which further exacerbates the CL-induced LSCD. Concomitant dry eye in CL-induced LSCD should be treated with preservative-free lubrication aggressively to allow the epithelium to heal.[8][9][11][32] More advanced therapies also exist, such as topical vitamin A (0.01%) and autologous serum tears.[8][11][32] Kim et al also reported on treating tear film deficiencies in patients with CL-induced LSCD with vitamin A ointment and punctal/cautery occlusion in addition to artificial tears and lid hygiene.[32] Autologous serum tears produced under sterile conditions from the patient’s own blood may also be used to treat dry eye by providing various epitheliotrophic growth factors and nutrients for the ocular surface.[33] In a case series of 20 eyes with severe CL-induced LSCD (median BCVA 20/100, persistent epithelial defects, >2 quadrants of corneal vascularization), Yeh et al reported regression of epithelial disease and VA improvement by 5 lines or more in 65% of eyes after aggressive treatment with serum tears for 8 weeks.[33]
Anti-inflammatory Treatment
Topical corticosteroids and cyclosporine can also be used to combat the inflammatory component of the disease process. These topical therapies have been used successfully in 13 patients and 2 patients who had comorbid rosacea demonstrated tear film improvement following lid hygiene and oral doxycycline in a study by Kim et al.[32]
Surgical Management
Mechanical Debridement
Surgical management can be considered in patients who fail conservative therapy and mechanical debridement (superficial keratectomy) can be performed in office, with some patients demonstrating immediate symptomatic improvement.[11][34] However, recurrence is frequent[11][34] and this surgical intervention may be augmented with concurrent medical management such as topical steroids and lubrication.[3]
Amniotic Membrane Transplantation
While the exact mechanism is yet to elucidated, amniotic membranes provide a nourishing environment for the repair of the limbal niche and growth of LSCs. It is also demonstrates anti-inflammatory properties and has a reduced risk of rejection.[35][36] However, this approach cannot be used alone to treat complete LSCD as it requires that at least some LSCs are present.[35][36] The membrane is draped over the conjunctiva and denuded cornea and sutured following conjunctival peritomy and scraping of the abnormal corneal epithelium.[36] Multiple studies have demonstrated improvement in LSCD, long-term symptomatic relief and improved visual acuity in patients who received amniotic membrane therapy, and in some cases with the other surgical interventions discussed in this section.[11][35][36]
LSC Transplantation
Allograft transplantation is a viable surgical option for LSCD that requires limbal tissue from either a cadaver (keratolimbal allograft, KLAL) or a living relative of the patient (HLA-matched living-related conjunctival limbal allograft, lr-CLAL).[37][38][39] Outcomes have been relatively positive with this technique, with 33-86% of eyes demonstrating improvised visual acuity in a variety of studies that looked at both types of source tissue.[8][12][38] By harvesting the allograft from a cadaver, there is no risk of complications to the donor eye. However, systemic immunosuppressive therapy is required and this surgical approach can be complicated by acute or chronic rejection, adverse effects from immunosuppressive therapy as well as ocular hypertension.[37][38][40] Limbal tissue grafting can be used in conjunction with amniotic membrane transplantation for cases of complete LSCD to help reconstitute the limbal niche before application of the membrane.[35][39][41]
It should be noted that autologous LSC transplantation is not recommended as this involves harvesting donor tissue from the contralateral eye. As most patients are bilateral contact lens wearers, it is not uncommon for the contralateral donor eye to have subclinical disease and this likely contributes to the post-surgical complications seen in these donor eyes.[3] Studies by Jenkins and Tan noted initial improvement in disease which were later complicated by conjunctivalization of the recipient eye and epithelial abnormalities in the donor eye respectively.[37][38] Ultimately, the autologous approach should be reserved for the rare case of unilateral contact lens use where one can be confident that the contralateral eye does not have LSCD.
Phototherapeutic Keratectomy
Laser therapy with an excimer laser can be directed to help treat superficial stromal scarring from LSCD. This has been used to successfully remove anterior corneal scars but it is recommended that this be used after treatment of LSCD because stromal scarring can often regress following restoration of a stable corneal epithelium.[3][42]
Keratoplasty
It is important to note that corneal transplantation alone is not considered a treatment for this condition as it is insufficient in the absence of LSCs. Keratoplasty can only provide a temporary intervention that is at high risk of failure from recurrent conjunctivalization because of the inability to heal.[8] Therefore, this technique should be considered as adjuvant therapy following reconstitution of the LSC function (e.g. via LSC transplantation).[19][35][41] Results vary with one patient who had total LSC failure achieving 20/30 BCVA in a case report by Nguyen et all while another patient with severe LSCD was treated with AMT, allograft limbal transplantation and PK but ultimately suffered PK rejection.[20][35] Rossen et al suggest performing deep anterior lamellar keratoplasty following limbal transplantation to manage the scarring, provided that the endothelium is normal, as is generally the case in CL-induced LSCD.[3]
References
- ↑ Schermer A, Galvin S, Sun TT. Differentiation-related expression of a major 64K corneal keratin in vivo and in culture suggests limbal location of corneal epithelial stem cells. J Cell Biol. 1986;103(1):49-62. doi:10.1083/jcb.103.1.49
- ↑ 2.0 2.1 Sangwan VS. Limbal stem cells in health and disease. Biosci Rep. 2001;21(4):385-405. doi:10.1023/a:1017935624867
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 Rossen J, Amram A, Milani B, et al. Contact Lens-induced Limbal Stem Cell Deficiency. Ocul Surf. 2016;14(4):419-434. doi:10.1016/j.jtos.2016.06.003
- ↑ Cope JR. Risk Behaviors for Contact Lens–Related Eye Infections Among Adults and Adolescents — United States, 2016. MMWR Morb Mortal Wkly Rep. 2017;66. doi:10.15585/mmwr.mm6632a2
- ↑ 5.0 5.1 Bhatia RP, Srivastava R, Ghosh A. Limbal stem cell study in contact lens wearers. Ann Ophthalmol Skokie Ill. 2009;41(2):87-92.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 Martin R. Corneal conjunctivalisation in long‐standing contact lens wearers. Clin Exp Optom. 2007;90(1):26-30. doi:10.1111/j.1444-0938.2006.00083.x
- ↑ Donisi PM, Rama P, Fasolo A, Ponzin D. Analysis of limbal stem cell deficiency by corneal impression cytology. Cornea. 2003;22(6):533-538. doi:10.1097/00003226-200308000-00009
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 Chan CC, Holland EJ. Severe limbal stem cell deficiency from contact lens wear: patient clinical features. Am J Ophthalmol. 2013;155(3):544-549.e2. doi:10.1016/j.ajo.2012.09.013
- ↑ 9.0 9.1 9.2 9.3 Sendele DD, Kenyon KR, Mobilia EF, Rosenthal P, Steinert R, Hanninen LA. Superior limbic keratoconjunctivitis in contact lens wearers. Ophthalmology. 1983;90(6):616-622. doi:10.1016/s0161-6420(83)34507-3
- ↑ Fadel D. Scleral Lens Issues and Complications Related to a Non-optimal Fitting Relationship Between the Lens and Ocular Surface. Eye Contact Lens. 2019;45(3):152-163. doi:10.1097/ICL.0000000000000523
- ↑ 11.00 11.01 11.02 11.03 11.04 11.05 11.06 11.07 11.08 11.09 11.10 11.11 11.12 Jeng BH, Halfpenny CP, Meisler DM, Stock EL. Management of focal limbal stem cell deficiency associated with soft contact lens wear. Cornea. 2011;30(1):18-23. doi:10.1097/ICO.0b013e3181e2d0f5
- ↑ 12.0 12.1 Shen C, Chan CC, Holland EJ. Limbal Stem Cell Transplantation for Soft Contact Lens Wear-Related Limbal Stem Cell Deficiency. Am J Ophthalmol. 2015;160(6):1142-1149.e1. doi:10.1016/j.ajo.2015.07.038
- ↑ 13.0 13.1 Truong TN, Graham AD, Lin MC. Factors in contact lens symptoms: evidence from a multistudy database. Optom Vis Sci Off Publ Am Acad Optom. 2014;91(2):133-141. doi:10.1097/OPX.0000000000000138
- ↑ Holden BA, Stephenson A, Stretton S, et al. Superior epithelial arcuate lesions with soft contact lens wear. Optom Vis Sci Off Publ Am Acad Optom. 2001;78(1):9-12. doi:10.1097/00006324-200101010-00008
- ↑ 15.0 15.1 Holland EJ, Schwartz GS. Iatrogenic limbal stem cell deficiency. Trans Am Ophthalmol Soc. 1997;95:95-107; discussion 107-110. doi:10.1007/0-387-21570-0_10
- ↑ Craig JP, Wang MTM, Kim D, Lee JM. Exploring the Predisposition of the Asian Eye to Development of Dry Eye. Ocul Surf. 2016;14(3):385-392. doi:10.1016/j.jtos.2016.03.002
- ↑ Tran N, Graham AD, Lin MC. Ethnic differences in dry eye symptoms: effects of corneal staining and length of contact lens wear. Contact Lens Anterior Eye J Br Contact Lens Assoc. 2013;36(6):281-288. doi:10.1016/j.clae.2013.06.001
- ↑ Craig JP, Willcox MDP, Argüeso P, et al. The TFOS International Workshop on Contact Lens Discomfort: report of the contact lens interactions with the tear film subcommittee. Invest Ophthalmol Vis Sci. 2013;54(11):TFOS123-156. doi:10.1167/iovs.13-13235
- ↑ 19.0 19.1 19.2 Bloomfield SE, Jakobiec FA, Theodore FH. Contact lens induced keratopathy: a severe complication extending the spectrum of keratoconjunctivitis in contact lens wearers. Ophthalmology. 1984;91(3):290-294. doi:10.1016/s0161-6420(84)34308-1
- ↑ 20.0 20.1 Nguyen DQ, Srinivasan S, Hiscott P, Kaye SB. Thimerosal-induced limbal stem cell failure: report of a case and review of the literature. Eye Contact Lens. 2007;33(4):196-198. doi:10.1097/01.icl.0000247636.10720.19
- ↑ 21.0 21.1 Garofalo RJ, Dassanayake N, Carey C, Stein J, Stone R, David R. Corneal staining and subjective symptoms with multipurpose solutions as a function of time. Eye Contact Lens. 2005;31(4):166-174. doi:10.1097/01.icl.0000152489.99455.db
- ↑ Lebow KA, Schachet JL. Evaluation of corneal staining and patient preference with use of three multi-purpose solutions and two brands of soft contact lenses. Eye Contact Lens. 2003;29(4):213-220. doi:10.1097/01.icl.0000081601.75812.03
- ↑ 23.0 23.1 Papas EB. The significance of oxygen during contact lens wear. Contact Lens Anterior Eye J Br Contact Lens Assoc. 2014;37(6):394-404. doi:10.1016/j.clae.2014.07.012
- ↑ Lee YF, Yong DWW, Manotosh R. A Review of Contact Lens-Induced Limbal Stem Cell Deficiency. Biology (Basel). Dec 5 2023;12(12)doi:10.3390/biology12121490
- ↑ 25.0 25.1 25.2 25.3 Shen Y, Xu JJ, Le QH. [The diagnosis and treatment of contact lens-induced limbal stem cell deficiency]. Zhonghua Yan Ke Za Zhi. 2023 Jun 11;59(6):467-475. Chinese. doi: 10.3760/cma.j.cn112142-20220627-00312. PMID: 37264577.
- ↑ Zoroquiain P, Sanft D-M, Esposito E, Cheema D, Dias AB, Burnier MN. High Inflammatory Infiltrate Correlates With Poor Symptomatic Improvement After Surgical Treatment for Superior Limbic Keratoconjunctivitis. Cornea. 2018;37(4):495-500. doi:10.1097/ICO.0000000000001508
- ↑ 27.0 27.1 Abdelfattah NS, Amgad M, Zayed AA, et al. Clinical correlates of common corneal neovascular diseases: a literature review. Int J Ophthalmol. 2015;8(1):182-193. doi:10.3980/j.issn.2222-3959.2015.01.32
- ↑ 28.0 28.1 Arentsen JJ. Corneal neovascularization in contact lens wearers. Int Ophthalmol Clin. 1986;26(1):15-23. doi:10.1097/00004397-198602610-00005
- ↑ Chan WK, Weissman BA. Corneal pannus associated with contact lens wear. Am J Ophthalmol. 1996;121(5):540-546. doi:10.1016/s0002-9394(14)75428-5
- ↑ Hamam R, Bhat P, Foster CS. Conjunctival/corneal intraepithelial neoplasia. Int Ophthalmol Clin. 2009;49(1):63-70. doi:10.1097/IIO.0b013e3181924ec3
- ↑ Kim KH, Deloss KS, Hood CT. Prosthetic Replacement of the Ocular Surface Ecosystem (PROSE) for Visual Rehabilitation in Limbal Stem Cell Deficiency. Eye Contact Lens. 2020;46(6):359-363. doi:10.1097/ICL.0000000000000685
- ↑ 32.0 32.1 32.2 32.3 Kim BY, Riaz KM, Bakhtiari P, et al. Medically reversible limbal stem cell disease: clinical features and management strategies. Ophthalmology. 2014;121(10):2053-2058. doi:10.1016/j.ophtha.2014.04.025
- ↑ 33.0 33.1 Yeh S-I, Chu T-W, Cheng H-C, Wu C-H, Tsao Y-P. The Use of Autologous Serum to Reverse Severe Contact Lens-induced Limbal Stem Cell Deficiency. Cornea. 2020;39(6):736-741. doi:10.1097/ICO.0000000000002264
- ↑ 34.0 34.1 D’Aversa G, Luchs JL, Fox MJ, Rosenbaum PS, Udell IJ. Advancing wave-like epitheliopathy. Clinical features and treatment. Ophthalmology. 1997;104(6):962-969. doi:10.1016/s0161-6420(97)30199-7
- ↑ 35.0 35.1 35.2 35.3 35.4 35.5 Tseng SC, Prabhasawat P, Barton K, Gray T, Meller D. Amniotic membrane transplantation with or without limbal allografts for corneal surface reconstruction in patients with limbal stem cell deficiency. Arch Ophthalmol Chic Ill 1960. 1998;116(4):431-441. doi:10.1001/archopht.116.4.431
- ↑ 36.0 36.1 36.2 36.3 Anderson DF, Ellies P, Pires RT, Tseng SC. Amniotic membrane transplantation for partial limbal stem cell deficiency. Br J Ophthalmol. 2001;85(5):567-575. doi:10.1136/bjo.85.5.567
- ↑ 37.0 37.1 37.2 Jenkins C, Tuft S, Liu C, Buckley R. Limbal transplantation in the management of chronic contact-lens-associated epitheliopathy. Eye Lond Engl. 1993;7 ( Pt 5):629-633. doi:10.1038/eye.1993.145
- ↑ 38.0 38.1 38.2 38.3 Tan DT, Ficker LA, Buckley RJ. Limbal transplantation. Ophthalmology. 1996;103(1):29-36. doi:10.1016/s0161-6420(96)30737-9
- ↑ 39.0 39.1 Utheim TP. Limbal epithelial cell therapy: past, present, and future. Methods Mol Biol Clifton NJ. 2013;1014:3-43. doi:10.1007/978-1-62703-432-6_1
- ↑ Holland EJ, Mogilishetty G, Skeens HM, et al. Systemic immunosuppression in ocular surface stem cell transplantation: results of a 10-year experience. Cornea. 2012;31(6):655-661. doi:10.1097/ICO.0b013e31823f8b0c
- ↑ 41.0 41.1 Solomon A, Ellies P, Anderson DF, et al. Long-term outcome of keratolimbal allograft with or without penetrating keratoplasty for total limbal stem cell deficiency. Ophthalmology. 2002;109(6):1159-1166. doi:10.1016/s0161-6420(02)00960-0
- ↑ Stasi K, Chuck RS. Update on phototherapeutic keratectomy. Curr Opin Ophthalmol. 2009;20(4):272-275. doi:10.1097/ICU.0b013e32832b4f44