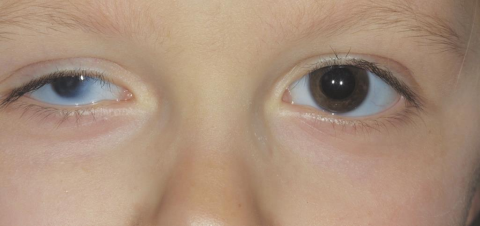
Microphthalmos
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Microphthalmos (also called microphthalmia), is a rare developmental disorder of the eye in which one or both eyes are abnormally small. It may occur as an isolated condition or in approximately one-third of cases as a part of a syndrome.[1][2] Microphthalmos itself refers to an eye with an axial length two standard deviations below that of the population age-adjusted mean, however, there is a wide phenotypic range of presentations related to the anatomical formation of the eye. [2] These presentations can range from simple microphthalmos (used interchangeably with nanophthalmos) in which the eye is small but lacks anatomical malformations, to posterior/anterior microphthalmos, to complex microphthalmos in which the eye has associated ocular disorders such as retinal dysplasias.[2] Microphthalmos, anophthalmia, coloboma are often seen in the same affected individual and are more often being referred to as MAC spectrum of disorders. The phenotype expressed is often dependent on the mutated genes and can vary among patients.[3][4]
Epidemiology
Given the rarity of microphthalmia, few population studies exist. Its estimated birth prevalence varies widely, based chiefly on national congenital anomaly registry studies.[5][6][7][8][9][10][11] Some studies consider its prevalence with conditions like anophthalmia and coloboma due to their phenotypic spectrum. Reported prevalence ranges from as high as 1.5–19/10,000 suggesting geographic and environmental differences.[2][11][12] CDC data from 2024 reported a prevalence of both microphthalmia/anopthalmia at 1 in 4,762 births or 2.1/10,000 in the United States. [13] Recent studies confirm that microphthalmos and anophthalmos have varying prevalence rates, influenced by geographic and demographic factors. Research indicates these conditions might exhibit higher prevalence in regions with certain substance-related patterns such as heavy cannabis use. [14][15]
Microphthalmia may be unilateral but is more commonly bilateral. Patients with bilateral disease are more likely to have systemic involvement.[12] It does not present differently according to sex and race and affects 3-12% of blind children.[2][5] [6][7][11] Epidemiological studies suggest microcornea or microphthalmos with coloboma are associated with worse visual outcomes.[16] About 1/5th of children with anophthalmia, microphthalmia and/or coloboma have intellectual disabilities.[2]
Etiology
The precise pathogenesis of microphthalmia remains incompletely understood. There are several hypotheses for the mechanism of microphthalmia during embryogenesis including: abnormal induction of the primitive neural tube, failure of the optic pit to enlarge and form the optic vesicle, secondary regression of an ocular structure, failure of lens induction, failure of closure of the optic fissure, failure of closure of the embryonic fissure during early gestation.[2] [17] [18]Another theory looks at post natal growth of the posterior segment and hypothesizes that reduced optic cup size, altered vitreous proteoglycan composition, low intraocular pressure, abnormal growth factor signaling, and inadequate secondary vitreous development may also contribute to both simple and complex microphthalmia.[2] [19] [20]
The etiology of microphthalmia can be attributed to genetic mutations, chromosomal abnormalities, genetic mutations, and environmental expsoures. Recent development of next generation sequencing and gene editing/knockout techniques have significantly aided in the discovery of the function of genes in eye development and the mutations that lead to microphthalmia.[21] [4] [22] Microphthalmos can be an isolated event or occur with systemic anomalies as well as both nonsyndromic and syndromic depending on the genes/chromosomes involved. They can also be inherited in an autosomal dominant or recessive pattern. There have been hundreds of genes identified in eye development and about thirty of these genes have been consistently implicated in the non syndromic form of anophthalmia/microphthalmia (A/M). One study suggests over eighty genes of significance in the MAC spectrum. [4] The major gene involved in both syndromic and nonsyndromic A/M is SOX2 accounting for about 15% of all cases.[22] SOX2 is a transcription factor that is highly expressed in the development of the eye. One study found 40% of all bilateral microphthalmia cases had heterozygous loss of function mutations in SOX2.[23] Other associated genes include OTX2, RAX, FOXE3, PAX6, BCOR, ALD1HA3, TFAP2A, Retinoic acid, BMP signaling molecules, SHH. [22][2][6][11][24][21] In only about 30% of cases a genetic cause can be determined with a mutation found in only about 10% of unilateral microphthalmia cases.[22] As our genetic sequencing techniques continue to improve genetic mutations and their accompanying syndromes are becoming easier to identify. Slavotinek et al. summarize the clinical findings associated with syndromic microphthalmia associated with the most common genes involved in mentioned above. [25] Microphthalmia is also seen in common chromosomal disorders including trisomy 13, trisomy 18, and CHARGE.[11][26][27].
Environmental risk factors include: maternal age over 40, elevated maternal pre-pregnancy body mass index (BMI), maternal smoking, maternal vitamin A deficiency, multiple births, infants of low birth weight, low gestational age, gestational-acquired infections (rubella, toxoplasmosis, varicella, cytomegalovirus, parvovirus B19, influenza virus, and coxsackie A9), maternal vitamin A deficiency, fever, hyperthermia, exposure to X-rays, solvent misuse and exposure to drugs like thalidomide, warfarin, cannabis, and alcohol.[8][19][20][27][28][29][30][31][14]
Clinical Diagnosis and Evaluation
Diagnosis of Microphthalmia is based upon clinical and imaging criteria, medical history, physical exam, family history, genetic testing, screening for malformations, and audiology. These patients often need a multidisciplinary team of healthcare providers from ophthalmologists, pediatricians, geneticist and genetic counselors, etc.[32]
Ocular Evaluation
Microphthalmia is marked by small eyes with anatomical malformation, typically an axial length two standard deviations below the mean for age, or below 21 mm in adults.[32] Diagnosis involves clinical inspection and palpation with consideration of corneal diameter measurements.
Despite the rarity of this condition, if present, it causes substantial visual impairment. Ocular disorders may affect the anterior segment and/or the posterior segment. These abnormalities include microcornea, corneal opacification, corectopia, ectopia lentis, aniridia, cataract, persistent fetal vasculature and/or retinal dysplasia persistent hyperplastic primary vitreous and retinal dysplasia[2] It’s also commonly associated with uveal colobomas. Microphthalmia may also be associated with an orbital cyst, typically located inferiorly. These cysts often communicate with the subarachnoid space and may enlarge over time.
Visual acuity depends on the extent and location of structural abnormalities. Good visual acuity may be preserved in cases with small iris or choroidal colobomas. Involvement of the macula or optic nerve head is associated with poor visual prognosis. Posterior microphthalmos is often associated with significant visual impairment. [32]
Refractive error is typically high hyperopia, though high myopia may occur in cases with posterior staphyloma.
Systemic Evaluation
Microphthalmia can be associated with intellectual disability, craniofacial malformations (as cleft lip/palate or microcephaly) and malformations of hands and feet (polydactyly). This ocular disorder can occur in isolation or be syndromic (33-50%). [9] Syndromes associated to Microphthalmia are CHARGE syndrome, Aicardi syndrome, Duker syndrome, Lenz microphthalmia syndrome, Oculo-Dento-Osseous Dysplasia, Fraser Syndrome, Cryptophthalmos syndrome, Cerebro-Oculo-Facial Syndrome, Goltz syndrome, Lowe syndrome, Meckel-Gruber syndrome, Basal cell nevus syndrome of Gorlin-Goltz, Cross syndrome, and Microphthalmia with linear skin defects.[33][34]
Since Microphthalmia can be associated to these non-ocular anomalies, physical examination (including dysmorphology examination) is mandatory to determine the presence of distinguishing clinical features. If no syndrome is identified in childhood, further examination after three or four years should be performed as many syndromes become more apparent at this age. [2]
Family history
A detailed three-generation family history should be obtained, with attention to microphthalmia, coloboma, or other ocular anomalies. Both parents should undergo a complete ophthalmic examination.
Differential Diagnosis
Includes anophthalmia, cryptophthalmos, cyclopia, and synophthalmia
Imaging/Genetic Testing
Fetal orbits are detectable by 11–12 weeks of gestation. Prenatally, ultrasound is used to assess globe size and orbital anatomy. If microphthalmia is suspected, genetic testing via amniocentesis or chorionic villus sampling with chromosomal microarray should be offered.[32][34] If clinical suspicion genetic evaluation through amniocentesis or chorionic villus sampling with chromosomal microarray analysis should be offered.
Post natally, Genetic testing using targeted gene panels or whole-exome sequencing should be offered to both unilateral and bilateral cases, as molecular diagnostic rates reach approximately 33% for each group.[35]
MRI is particularly useful due to superior soft tissue resolution and absence of radiation. It can identify residual ocular tissue, optic nerve presence, and extraocular muscles, helping distinguish severe microphthalmia from anophthalmia.[26] If there is an orbital cyst, it produces a homogeneous signal that varies from isointense to hypointense on MRI T1-weighted image, while on T2-weighted image the cyst appears hyperintense and there is no enhancement with gadolinium. [32]
Electrophysiological tests are critical for assessing the severity of visual impairment and help to determine at which level the abnormality is. In cases of severe microphthalmia, a flash visual evoked potential (VEP) will establish if any visual function is present. A pattern VEP will determine the severity of the disease and detect any optic nerve dysfunction while an electroretinogram will identify if there is retinal dysfunction.[32]
Management
Early identification is essential. A multidisciplinary approach is recommended.[2] Prevention of hemifacial asymmetry secondary to the reduced eyeball size is the goal of treatment. This is performed with socket expansion. Early identification of even minor vision is important and can guide socket expansion treatment. [32]
Medical therapy
If retinal function is detectable, refraction and treatment of any underlying amblyopia is critical.
After initial socket expansion (see below), patients must still be followed to monitor for angle closure glaucoma, retinal detachment (if chorioretinal coloboma), and need for correction of refractive error.
Surgery
The reduction of ocular volume caused by microphthalmia affects normal facial and orbital development. Therefore, early socket expansion, usually started within weeks of life, is imperative to minimize facial deformity, particularly in cases of severe microphthalmia. Therapeutic strategies aim simultaneous management of both soft tissue hypoplasia and asymmetric bone growth. [36][37][38]
Management and timing of initiating socket expansion therapy can be guided by the axial length. If the axial length of the eye is over 16 mm, orbital growth is more likely to be normal and the timing of expansion therapy is variable depending on social/aesthetic needs. However, if the axial length is less than 16 mm, it is unlikely to promote normal orbital growth alone and it is necessary to increase the socket volume early on to prevent pronouncing asymmetry as the child grows.[32]
Mild/moderate microphthalmia is generally managed conservatively with the insertion of progressively enlarging conformers. The length of time between changing conformers is not uniform and averages between a week to month.[32][39]
In severe mircophthalmia, socket expansion through conformers is often not enough and these patients require additional interventions including endo-orbital volume replacement (implants, expanders, dermis fat grafting). Orbital osteotomies are indicated in more severe cases or older children with insufficient orbital volume.[39] One study even described an expanding bony orbitotomy with the implantation of an inflatable balloon device to expand the soft tissues.[39]
If an orbital cyst is present, depending on the size and location, it may be retained or removed. In some cases, large cysts may provide natural expansion of the socket, therefore surgery is postponed until it reaches 90% of the orbital volume, allowing removal for cosmetic reasons at about the time the child starts school.[2][32][40]
Prognosis
The potential for visual development depends on the ocular structures affected and the severity of the malformations. The treatment aims to maximize the existing vision, prevent deformities and provide improvement at the aesthetic level. The lack of treatment can cause significant psychosocial issues in patients throughout life.
References
- ↑ American Academy of Ophthalmology. Microphthalmos. https://www.aao.org/image/microphthalmos Accessed July 15, 2019
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 Verma AS, Fitzpatrick DR. Anophthalmia and microphthalmia. Orphanet J Rare Dis. 2007;2:47. Published 2007 Nov 26. doi:10.1186/1750-1172-2-47
- ↑ Bardakjian T, Weiss A, Schneider A. Microphthalmia/anophthalmia/coloboma spectrum. In: Adam MP, Feldman J, Mirzaa GM, et al., eds. GeneReviews®. University of Washington, Seattle; 2015. Updated February 25, 2021. www.ncbi.nlm.nih.gov
- ↑ 4.0 4.1 4.2 Reis LM, Semina EV. Conserved genetic pathways associated with microphthalmia, anophthalmia, and coloboma. Birth Defects Res C Embryo Today. 2015;105(2):96-113. doi:10.1002/bdrc.21097
- ↑ 5.0 5.1 Dharmasena, Aruna; Keenan, Tiarnan; Goldacre, Raph; Hall, Nick; Goldacre, Michael J (2017). "Trends over time in the incidence of congenital anophthalmia, microphthalmia and orbital malformation in England: Database study". British Journal of Ophthalmology. 101 (6): 735–739.
- ↑ 6.0 6.1 6.2 Morrison D, FitzPatrick D, Hanson I, Williamson K, van Heyningen V, Fleck B, Jones I, Chalmers J, Campbell H. National study of microphthalmia, anophthalmia, and coloboma (MAC) in Scotland: investigation of genetic aetiology. J Med Genet. 2002;39:16–22.
- ↑ 7.0 7.1 Campbell H, Holmes E, MacDonald S, Morrison D, Jones I. A capture-recapture model to estimate prevalence of children born in Scotland with developmental eye defects. J Cancer Epidemiol Prev. 2002;7:21–28.
- ↑ 8.0 8.1 Shaw GM, Carmichael SL, Yang W, Harris JA, Finnell RH, Lammer EJ. Epidemiologic characteristics of anophthalmia and bilateral microphthalmia among 2.5 million births in California, 1989–1997. Am J Med Genet A. 2005;137:36–40.
- ↑ 9.0 9.1 Kallen B, Robert E, Harris J. The descriptive epidemiology of anophthalmia and microphthalmia. Int J Epidemiol. 1996;25:1009–1016.
- ↑ Forrester MB, Merz RD. Descriptive epidemiology of anophthalmia and microphthalmia, Hawaii, 1986–2001. Birth Defects Res A Clin Mol Teratol. 2006;76:187–92.
- ↑ 11.0 11.1 11.2 11.3 11.4 PH, Danysh HE, Weber KA, Shaw GM, Mitchell LE, Lupo PJ. Epidemiology of anophthalmia and microphthalmia: Prevalence and patterns in Texas, 1999-2009. Am J Med Genet A. 2018 Sep;176(9):1810-1818.
- ↑ 12.0 12.1 Galindo-Ferreiro A, Elkhamary SM, Alhammad F, AlGhafri L, AlWehaib M, Alessa D, Aldossari S, Akaishi P, Khadekar R, AlShaikh O, Schellini SA. Characteristics and management of congenital anophthalmos and microphthalmos at a tertiary eye hospital. Orbit. 2019 Jun;38(3):192-198.
- ↑ Stallings EB, Isenburg JL, Rutkowski RE, et al. National population-based estimates for major birth defects, 2016-2020. Birth Defects Res. 2024;116(1):e2301. doi:10.1002/bdr2.2301
- ↑ 14.0 14.1 Reece AS, Hulse GK. European Epidemiological Patterns of Cannabis- and Substance-Related Congenital Neurological Anomalies: Geospatiotemporal and Causal Inferential Study. International Journal of Environmental Research and Public Health. 2023; 20(1):441. https://doi.org/10.3390/ijerph20010441
- ↑ Reece AS, Hulse GK. Geotemporospatial and causal inference epidemiological analysis of US survey and overview of cannabis, cannabidiol and cannabinoid genotoxicity in relation to congenital anomalies 2001-2015. BMC Pediatr. 2022;22(1):47. Published 2022 Jan 19. doi:10.1186/s12887-021-02996-3
- ↑ Tibrewal S, Subhedar K, Sen P, et al Clinical spectrum of non-syndromic microphthalmos, anophthalmos and coloboma in the paediatric population: a multicentric study from North India. British Journal of Ophthalmology 2021;105:897-903.
- ↑ Mann I. Developmental Abnormalities of the Eye. 2nd ed. Philadelphia, PA: JB Lippincott Co; 1953.
- ↑ Guthoff R, Klein R, Lieb WE. Congenital cystic eye. Graefes Arch Clin Exp Ophthalmol. 2004;242(3):268-271. doi:10.1007/s00417-003-0820-8
- ↑ 19.0 19.1 Weiss AH, Kousseff BG, Ross EA, Longbottom J. Simple microphthalmos. Arch Ophthalmol. 1989;107:1625–1630
- ↑ 20.0 20.1 Weiss AH, Kousseff BG, Ross EA, Longbottom J. Complex microphthalmos. Arch Ophthalmol. 1989;107:1619–1624.
- ↑ 21.0 21.1 Ohuchi H, Sato K, Habuta M, Fujita H, Bando T. Congenital eye anomalies: More mosaic than thought? Congenit Anom. 2019; 59: 56–73. https://doi-org.libproxy.uams.edu/10.1111/cga.12304
- ↑ 22.0 22.1 22.2 22.3 Plaisancié J, Ceroni F, Holt R, et al. Genetics of anophthalmia and microphthalmia. Part 1: Non-syndromic anophthalmia/microphthalmia. Hum Genet. 2019;138(8-9):799-830. doi:10.1007/s00439-019-01977-y
- ↑ Blackburn PR, Chacon-Camacho OF, Ortiz-González XR, et al. Extension of the mutational and clinical spectrum of SOX2 related disorders: Description of six new cases and a novel association with suprasellar teratoma. Am J Med Genet Part A. 2018; 176A: 2710–2719. https://doi-org.libproxy.uams.edu/10.1002/ajmg.a.40644
- ↑ Taha Najim R, Topa A, Jugård Y, Casslén B, Odersjö M, Andersson Grönlund M. Children and young adults with anophthalmia and microphthalmia: Diagnosis and Management. Acta Ophthalmol. 2020 Dec;98(8):848-858.
- ↑ Slavotinek A. Genetics of anophthalmia and microphthalmia. Part 2: Syndromes associated with anophthalmia-microphthalmia. Hum Genet. 2019;138(8-9):831-846. doi:10.1007/s00439-018-1949-1
- ↑ 26.0 26.1 Bardakjian T, Weiss A, Schneider A. Microphthalmia/Anophthalmia/Coloboma Spectrum. 2004 Jan 29 [Updated 2015 Jul 9]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK1378/
- ↑ 27.0 27.1 Warburg M. An update on microphthalmos and coloboma. A brief survey of genetic disorders with microphthalmos and coloboma. Ophthalmic Paediatr Genet. 1991;12:57–63. doi: 10.3109/13816819109023675.
- ↑ Dolk H, Busby A, Armstrong BG, Walls PH. Geographical variation in anophthalmia and microphthalmia in England, 1988–94. BMJ. 1998;317:905–909.
- ↑ Weiland HT, Vermey-Keers C, Salimans MM, Fleuren GJ, Verwey RA, Anderson MJ. Parvovirus B19 associated with fetal abnormality. Lancet. 1987;1:682–683. doi: 10.1016/S0140-6736(87)90442-9.
- ↑ Knox EG, Lancashire RJ. Epidemiology of congenital malformations. London: HMSO; 1991.
- ↑ O'Keefe M, Webb M, Pashby RC, Wagman RD. Clinical anophthalmos. Br J Ophthalmol. 1987;71:635–638.
- ↑ 32.0 32.1 32.2 32.3 32.4 32.5 32.6 32.7 32.8 32.9 N K Ragge, I D Subak-Sharpe, J R O Collin, A practical guide to the management of anophthalmia and microphthalmia. Eye. 2007 21:1290–1300
- ↑ Traboulsi EI. Compendium of Inherited Disorders and the Eye. New York: Oxford University Press; 2005
- ↑ 34.0 34.1 Society for Maternal-Fetal Medicine, Benacerraf BR, Bromley B, Jelin AC. Anophthalmia and Microphthalmia. Am J Obstet Gynecol. 2019 Nov;221(5):B20-B21.
- ↑ Harding P, Gore S, Malka S, Rajkumar J, Oluonye N, Moosajee M. Real-world clinical and molecular management of 50 prospective patients with microphthalmia, anophthalmia and/or ocular coloboma. Br J Ophthalmol. 2023;107(12):1925-1935. Published 2023 Nov 22. doi:10.1136/bjo-2022-321991
- ↑ Kennedy RE. Growth retardation and volume determinations of the anophthalmic orbit. Trans Am Ophthalmol Soc. 1972;70:277–297.
- ↑ Kennedy RE. The Effect of Early Enucleation on the Orbit in Animals and Humans. Trans Am Ophthalmol Soc. 1964;62:459–510.
- ↑ Hintschich C, Zonneveld F, Baldeschi L, Bunce C, Koornneef L. Bony orbital development after early enucleation in humans. Br J Ophthalmol. 2001;85:205–208.
- ↑ 39.0 39.1 39.2 Wavreille O, François Fiquet C, Abdelwahab O, Laumonier E, Wolber A, Guerreschi P, Pellerin P. Surgical and prosthetic treatment for microphthalmia syndromes. Br J Oral Maxillofac Surg. 2013 Mar;51(2):e17-21.
- ↑ Cui Y, Li Y, Hou Z, Wang Y, Chang Q, Xian J, Li D. Management of congenital microphthalmos and anophthalmos with orbital cyst. J AAPOS. 2019 Apr;23(2):92.e1-92.e6. doi: 10.1016/j.jaapos.2018.10.015. Epub 2019 Mar 27.