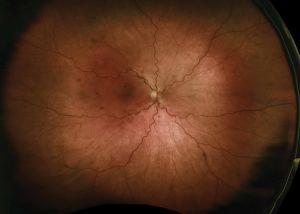
Papillophlebitis
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Disease
Papillophlebitis (PP) is a rare condition that may present clinically like an incomplete central retinal vein occlusion (CRVO). Unlike CRVO which is often associated with vasculopathic risk factors (e.g., hypertension), PP typically occurs in young, healthy females with acute, painless unilateral visual loss, optic disc edema, retinal vein engorgement, and varying amounts of intraretinal hemorrhage[1]. The disease on its own has been previously questioned in terminology and origin[2].
Pathophysiology
The pathophysiology of PP remains ill-defined and some authors have suggested that the condition stems from idiopathic “inflammation of the optic disc” which then compresses the central retinal vein and causes secondary mechanical fundus findings of venous insufficiency and intraretinal hemorrhage[3]. Studies have shown that the potential etiology/pathophysiology may be frequently confused with other pathologies like incipient nonarteritic anterior ischemic neuropathy, unilateral isolated paucisymptomatic optic disc Edema(UIODE), optic nerve edema secondary to vitreopapillary traction, peripapillary choroidal neovascular membrane[2].
Epidemiology
PP tends to occur more commonly in women and in those between the ages of 20 and 35[1].
Risk Factors
The etiology of PP remains controversial and is presumed to be idiopathic. PP however has also been reported in hematologic disorders (hypercoagulable state)[4] and systemic vascular diseases (e.g., diabetes (3-9%) and hypertension) (23-42%)[1][5]. Other associated risk factors that have been suggested include inflammatory bowel syndrome, psoriasis, pregnancy, oral contraceptives, psoriasis, high altitudes, and dehydration[1]. Recently, associated factors included COVID-19, further suggesting a connection with a hypercoagulable state[3][6].
Diagnosis
Presentation
PP commonly presents with acute, painless and mild monocular visual loss. In contrast to ischemic CRVO, the visual acuity is typically normal or near normal[7]. There may or may not be a relative afferent pupillary defect (RAPD) in PP but the absence of an RAPD is more consistent with PP than ischemic CRVO[1]. Enlargement of the blind spot on visual field testing is another classic finding associated with PP but this perimetric finding can be seen in other cases of optic disc edema (e.g., papilledema). Other nerve fiber layer type visual field defects may be seen in PP. Ophthalmoscopy shows optic disc edema, variable retinal venous dilation and tortuousity, vitreous cell, and intraretinal hemorrhages.
Diagnostic Procedures
Optical coherence tomography (OCT) may show a normal macula as opposed to the macular edema of CRVO. OCT of the optic nerve in PP may show retinal nerve fiber layer edema without traction over the optic disc. Macular edema has however been reported in PP and therefore cannot be used alone as a differentiating feature between PP and CRVO. Paracentral acute middle maculopathy (PAMM), a hyperreflective retina on OCT may be seen with the deepp capilary layer showing fernlike ischemic patterns.[8] Fluorescein angiography (FA) may show variable degrees of blockage from intraretinal hemorrhage, leakage if macular edema is present, or staining and leakage of the optic disc and retinal veins in PP.
Imaging of the brain and orbits can be used the exclude other causes of optic disc edema but both neuroimaging and laboratory testing is usually normal in PP.
Laboratory testing
Since some reports have found and underlying hypercoagulability disorder[4][5] it is recommended to further investigate the following:
- CBC
- Serum electrolytes
- PT/INR, PTT
- Protein C and S
- Homocysteine levels
- Factor V Leiden and prothrombin II mutation(G20210A)
- Antithrombin III leveles (to rule out deficiency)
- Serology for autoimmunity including: anti-DNA, perinuclear (p) and cytoplasmic (c) anti-neutrophil cytoplasmic antibody (ANCA), antinuclear antibody (ANA), anti-SM, anti- Sm/RNP, anti-ss-A, anti-ss-B, anti-scl70, and anti-mitochondrial antibodies[9]
- Other: COVID (In the appropriate scenario)
Differential Diagnosis
The differential for PP includes CRVO, retinal vein prethrombosis, impending nonarteritic ischemic optic neuropathy, hypertensive retinopathy, diabetic papillopathy, infectious papillitis, unilateral papilledema secondary to idiopathic intracranial hypertension , optic nerve sheath meningioma compression, optic nerve edema related to vitreopapillary traction, peripapillary choroidal neovascular membrane and orbital compressive lesions[2]. It is important to differentiate PP from papilledema or optic neuritis, which are more common in the affected age group[3] and some authors consider PP to be a diagnosis of exclusion.
Management
Treatment
Even though it presents similarly to CRVO, the mainstay of medical treatment for PP is corticosteroids. Anti-platelet therapy and anticoagulation have also been proposed in PP but are unproven. There remains no evidence based and universally accepted treatment modality for PP[10]. In cases of profound vision loss or not resolving macular edema, intravitreal anti-VEGF treatment can be considered, but is not FDA approved[9].
Prognosis
Because PP has a different pathophysiology and presents with much better visual acuity than ischemic CRVO, the prognosis for PP is typically much more favorable. However, if not treated immediately, PP can progress to ischemic CRVO and cause permanent retinal damage and up to 30% of patients develop ischemic venous occlusion[10].
Summary
PP is a rare ocular condition that typically affects young (20-35 years old), previously healthy women. PP is often misdiagnosed as papillitis or papilledema. The presence of retinal venous dilation and tortuosity, vitreopapillary traction, and scattered intraretinal hemorrhages should suggest secondary rather than primary optic disc edema. Ancillary testing with OCT or FA may help in differentiating PP from CRVO. Many authors believe PP to be a form of inflammatory CRVO and although the prognosis is generally favorable, PP can lead to ischemic CRVO with resulting macular edema and poor visual outcome. Although corticosteroids are the mainstay of treatment for PP, the precise etiology and pathogenesis for PP is ill-defined and an evidence-based recommendation for therapy is lacking and the use of steroids with or without adjuvant anti-platelet or anticoagulation therapy for PP remains unproven.
Additional Resources
- Porter D, Vemulakonda GA. Blood Pressure. American Academy of Ophthalmology. EyeSmart/Eye health. https://www.aao.org/eye-health/anatomy/blood-pressure-list. Accessed January 06, 2023.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 Grosso A, Calzada J, Randolph J, Sigler E. Papillophlebitis: A closer look. Retina Today. https://retinatoday.com/articles/2017-july-aug/papillophlebitis-a-closer-look.
- ↑ 2.0 2.1 2.2 Hawy, Eman MD; Sharma, Rahul A. MD, MPH; Peragallo, Jason H. MD; Dattilo, Michael MD, PhD; Newman, Nancy J. MD; Biousse, Valérie MD. Unilateral Isolated Paucisymptomatic Optic Disc Edema. Journal of Neuro-Ophthalmology 41(4):p e523-e534, December 2021. | DOI: 10.1097/WNO.0000000000001136
- ↑ 3.0 3.1 3.2 Insausti-García A, Reche-Sainz JA, Ruiz-Arranz C, López Vázquez Á, Ferro-Osuna M. Papillophlebitis in a COVID-19 patient: Inflammation and hypercoagulable state. European Journal of Ophthalmology. July 2020. doi:10.1177/1120672120947591
- ↑ 4.0 4.1 Abdel Jalil, S., & Amer, R. (2024). The Spectrum of Papillophlebitis. Ocular Immunology and Inflammation, 32(10), 2515–2520. https://doi.org/10.1080/09273948.2024.2359622
- ↑ 5.0 5.1 Güzel H, Turgut Öztürk B, Gedik Ş, Bakbak B, Beyoğlu A, Koçak N. Bilateral Papillophlebitis in a Patient with Mutation of Metilenetetrahydrofolate Reductase Enzyme. Turk J Ophthalmol. 2016;46(4):182-185. doi:10.4274/tjo.77785
- ↑ Insausti-García A, Reche-Sainz JA, Ruiz-Arranz C, López Vázquez Á, Ferro-Osuna M. Papillophlebitis in a COVID-19 patient: Inflammation and hypercoagulable state. Eur J Ophthalmol. 2022;32(1):NP168-NP172. doi:10.1177/1120672120947591
- ↑ Ferris DG, Bode D. Papillophlebitis, optic disc vasculitis. J Fam Pract. 1991;33(2):198-200.
- ↑ Arias JD. Retinal Ischemic Cascade in Multiple Conditions With PAMM. AAO 2025 Video Program. Jan 2026. Accessed April 15, 2026.https://www.aao.org/education/annual-meeting-video/retinal-ischemic-cascade-conditions-with-pamm
- ↑ 9.0 9.1 Güngör İ, Konuk GE, Süllü Y, Arıtürk N. Papillophlebitis: Treatment of Vision Loss Due To Subretinal Fluid with Intravitreal Ranibizumab. Neuroophthalmology. 2014 Oct 9;38(6):336-339. doi: 10.3109/01658107.2014.954293. PMID: 27928322; PMCID: PMC5123187.
- ↑ 10.0 10.1 Güngör İ, Konuk GE, Süllü Y, Arıtürk N. Papillophlebitis: Treatment of Vision Loss Due To Subretinal Fluid with Intravitreal Ranibizumab. Neuroophthalmology. 2014;38(6):336-339. Published 2014 Oct 9. doi:10.3109/01658107.2014.954293