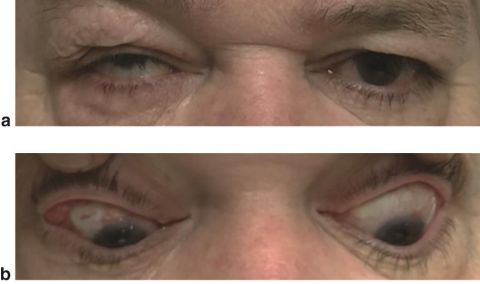
Hypertropia
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Definition
Vertical strabismus describes a vertical misalignment of the eyes. By convention, the misalignment is typically labelled by the higher, or hypertropic, eye. The vertical misalignment can also be labelled by the lower, or hypotropic eye.[2] Some advocate labelling vertical misalignments based on if the deviated eye manifests as a hypertropia or hypotropia. Depending on which eye is fixing, a hypertropia of one eye is the same as a hypotropia of the fellow eye. If the degree of deviation in all fields of gaze is the same, it is classified as comitant; if it behaves differently in different fields of gaze, it is classified as incomitant.
Etiology
Vertical misalignments of the eyes typically result from dysfunction of the vertical recti muscles (inferior and superior rectus) or of the oblique muscles (the inferior oblique and superior oblique). More rarely, they are caused by abnormal positioning of the horizontal rectus muscles. Muscle dysfunction may result from paresis, restriction, over-action, muscle malpositioning, and dysinnervation. Most forms of vertical strabismus have notable incomitance, with variable degree of deviation in different positions of gaze.
Signs and Symptoms
Suppression
Is not perceived by the patient, but rather by the observer. Suppression typically happens when the deviation starts in the early years of life (before 6 years of age), when the neuroplasticity of the visual system is still capable of suppressing the image coming from the deviated eye. The amount of suppression, which can vary from small suppression scotomas in binocular fusion to large suppression areas on the affected side and amblyopia, depends on various factors such as the size of the strabismus and age of onset.
Diplopia
Occurs when the deviation is acquired after a significant maturation of the visual system (7 to 8 years of age), when suppressive mechanisms are usually no longer initiated. Younger children may also have transitory diplopia in acquired forms of strabismus, before suppression kicks in. In the case of a hypertropia, the diplopia is vertical.
Visual Confusion
Two images are perceived in the same location, due to a misalignment of retinal correspondence points on the fovea. This symptom is rare, when compared to diplopia and the same rules apply for age of patients affected. It has been observed in glaucoma patients with an acquired strabismus (see strabismus following glaucoma surgery), due to tunnel vision and forced use of the fovea.
Diagnosis
Sensorimotor Testing
The degree of misalignment should be determined for at least primary, horizontal, and vertical gazes and in head tilts. The results can be used to perform a Three Step Test for Cyclovertical Muscle Palsy. Torsion can be tested with the double maddox rod test. Haplosopic testing can be performed to evaluate for the ability to fuse in the setting of torsion. Worth 4 dot and Bagolini lenses can be used to evaluate for suppression. Specific methods for testing are detailed in the highlighted links above as well as the article on Sensory and Motor Testing.
Categories of Vertical Strabismus
Vertical Strabismus with Horizontal Comitance
While there is frequently still some level of horizontal incomitance, some forms of vertical strabismus typically have less than 10 PD of incomitance in horizontal gazes.
Monocular Elevation Deficit Syndrome (MEDS)
Limitation of elevation with contralateral hypertropia, previously called double elevator palsy.
Other features: Chin elevation[2]and ipsilateral true or pseudo-ptosis.[3]
Cause: It can have various causes, such as orbital restrictive or neurological causes (supranuclear, nuclear or infranuclear). [4]Sometimes it can be associated with congenital inferior rectus restriction, superior rectus palsy [5] or both. [4]
- If vertical deviation in primary position of gaze, attributable to a restriction of the IR on forced ductions: Inferior rectus recession. In the case of a large angle strabismus, a contralateral superior rectus recession may be indicated.
- If superior rectus palsy: Superior transposition of half tendon lengths of medial and lateral recti or Knapp procedure. In the case of forced duction limitation, add an inferior rectus recession to the former.
Incomitant Vertical Strabismus
Incomitant vertical deviations have different degrees of deviation depending on the position of gaze. This occurs commonly when the oblique muscles are involved but may also result from other etiologies.
Etiologies of Incomitant Vertical Strabismus
| Cause | Deviation and Motility | Pattern | Torsion | Deviation with head tilt | Forced Duction Testing | Other |
| Over-depression in Adduction (ODAd)
Note: Apparent ODAd may be caused by over-depression/ under-elevation in adduction or under-depression/ over-elevation in abduction of the fellow eye | ||||||
| Superior oblique Overaction | Over-depression in adduction. VS often limited to adduction | A or lambda pattern exotropia | Typically only objective Intorsion | No | Negative | |
| Brown Syndrome | Elevation deficit and VS worst in adduction, occasional over-depression in adduction | None, Y, or V | None | No | Limited elevation in adduction | Insignificant superior oblique overaction |
| Inferior oblique palsy | Elevation deficit and VS worst in adduction | A, may be an esodeviation in upgaze and exodeviation in downgaze | Intorsion | Worse with contra-lateral tilt | Negative | Associated superior oblique over-action |
| Contralateral Superior rectus restriction | Depression deficit and VS worst in abduction of the affected eye | May have mild intorsion | Limited depression | |||
| Contralateral Inferior rectus under-action | Depression deficit and VS worst in abduction of the affected eye | May have mild intorsion | Worse with contra-lateral tilt | Decreased force generation and saccadic velocity | ||
| Contralateral Superiorly displaced lateral rectus muscle/ muscle pulley | Over-elevation of the affected eye when abducted | A | May have mild intorsion | |||
| Over-elevation in Adduction (OEAd)
Note: Apparent OEAd may be caused by over-elevation/ under-depression in adduction or under-elevation/ over-depression in abduction of the fellow eye | ||||||
| Superior oblique palsy | Depression deficit and VS worst in adduction | Possible V pattern esotropia if unilateral; larger V pattern if bilateral | Extorsion, typically >10 degrees if bilateral | Worse with ipsilateral tilt, alternates if bilateral | Laxity of the SO | If unilateral, tilt away from affected side; If bilateral, chin down position |
| Inferior oblique Overaction | Over-elevation in adduction. VS often limited to adduction | Y or V | Typically only objective Extorsion | No | Y pattern in primary; V pattern in secondary | |
| Contralateral Superior rectus under-action | Elevation deficit and VS worst in abduction of the affected eye | May have mild extorsion | Worse with ipsilateral tilt | Decreased force generation and saccadic velocity | ||
| Contralateral Inferior rectus restriction | Elevation deficit and VS worst in abduction of the affected eye | May have mild extorsion | Limited elevation | Poor or absent Bell phenomenon | ||
| Contralateral Anti-elevation syndrome following inferior oblique anterior-ization | Elevation deficit and VS in abduction of the affected eye | Typically none | Limited elevation in abduction | |||
| Contralateral Inferiorly displaced lateral rectus muscle/ muscle pulley | Over-depression of the affected eye when abducted | V | ||||
Over-depression in adduction
Superior Oblique Overaction
Vertical deviation, that increases on adduction of the affected eye. Ex.: A left superior oblique overaction causes a right hypertropia on right gaze.
Other features: Intorsion and abduction in downgaze. If congenital, the intorsion is frequently only objective and not subjective, since there is sensory adaptation. It frequently coexists with an under-action of the contralateral IR and intermittent exotropia. Sometimes it can give rise to an acquired Brown’s syndrome, due to SO contracture (for the differential diagnosis between SO overaction and Brown’s syndrome, see the differential diagnosis section).[4] A vertical deviation in primary position is more frequently associated with a unilateral or asymmetric SO paresis.[2] When bilateral, it frequently gives rise to lambda-pattern, with accentuated exotropia in downgaze.[4]
It is more frequently bilateral. It often coexists with an intermittent exotropia or other forms of horizontal strabismus.
Causes:
- Primary
- Secondary to a contralateral inferior rectus paresis
SO weakening procedures: SO expander, tenotomy, tenectomy or recession.
If the patient has binocular fusion, weakening the superior oblique may give rise to extorsional diplopia. In this particular case, horizontal muscle surgery or an expander may be more indicated, as suggested by Wright et al.[4]
In the case of a coexisting DVD, particular care has to be taken since SO weakening procedures may worsen this entity.
Brown Syndrome
Poor movement of the superior oblique tendon through the trochlea leads to limited elevation of the eye in adduction, frequently with an associated exotropia in upgaze.
Cause:[4][8][9][10][11][12][13][14]
- Congenital (Ex.: Inelasticity of the SO muscle-tendon complex; pseudo-Brown's syndrome due to inferior orbital adhesions; inferior displacement of the lateral rectus). A spontaneous resolution of congenital Brown’s syndrome has been reported.[15][16]
- Iatrogenic (Ex.: Following glaucoma, oculoplastics, strabismus, or ENT surgery)
- Inflammation of the trochlea (Ex.: Rheumatoid arthritis; systemic lupus erythematosus)
- Traumatic
- Nasal sinus infection
- Tight superior oblique muscle (Ex.: Thyroid ophthalmopathy; secondary to superior oblique overaction)
- Neoplastic
- Hurler-Scheie syndrome
- Idiopathic
Treatment:[4]
- If inflammatory: systemic nonsteroidal anti-inflammatory agents, local steroid injection to the trochlea.
- If congenital: There is an indication for surgery if there is a vertical deviation in primary position with an important face turn. SO lengthening procedures are indicated such as: SO expander, tenotomy, tenectomy. With tenotomy and tenectomy, care should be taken for overcorrections.
Unilateral Inferior Oblique Paresis
Leads to an elevation deficit in adduction and greater vertical deviation with tilt to the contralateral side. It frequently leads to a contralateral hypertropia due to overaction of the yoke muscle (SR). The increase of vertical deviation in adduction and upgaze to the contralateral side. Hypertropia, that increases on head tilt to the contralateral side. Ex.: Left inferior oblique paresis causes a right hypertropia on right and up gaze and head tilt to the right.
It is a rare and a bilateral involvement is very uncommon.
- Most frequently idiopathic or iatrogenic (following inferior oblique surgery or retrobulbar block).
- Congenital
- Traumatic
- Vascular
- Neurological
- If a vertical deviation in primary position, abnormal head posture or diplopia:
- If vertical deviation <10DP: Ipsilateral SO weakening (see superior oblique overaction)
- If vertical deviation of >10DP: Ipsilateral SO weakening + contralateral SR weakening.
Inferior Rectus Under-action of the Contralateral Eye
Leads to a depression deficit/ vertical misalignment that is worst when the affected eye is abducted and with contralateral head tilt.
- Iatrogenic (ex.: Overcorrections following inferior rectus weakening procedures as in thyroid ophthalmopathy )
- Traumatic
- Innervational anomaly of the inferior division of the III cranial nerve
- Muscle aplasia (The inferior rectus is most frequently affected, it can be associated with craniofacial disorders)
- Neoplastic
- Neurological (ex.: Myasthenia gravis)
Over-elevation in adduction
Superior Oblique Under-action
Unilateral Superior Oblique Under-action
Hypertropia that increases on adduction and and with ipsilateral head tilt. Ex.: Left superior oblique paresis causes a left hypertropia on right gaze and head tilt to the left.
It is the most common cause of an isolated vertical deviation.[4][23]
Other features: Mild extorsion (<10º); compensatory head tilt to the contralateral side and face turn towards the contralateral shoulder, sometimes associated with a facial asymmetry; contralateral inferior rectus overaction (“fallen eye’’)[4]; large vertical fusional amplitudes when congenital.[4][2] Patients who fix with the palsied eye may appear to have decreased function of the contralateral superior rectus muscle when adducting the eye with the superior oblique palsy, called an inhibitional palsy of the contralateral antagonist.
- Congenital and traumatic causes are the most frequent (Congenital causes are frequently due to absent trochlear nerves, muscle hypoplasias or tendon laxity but muscle/tendon agenesis has also been described. Symptoms sometimes arise in late childhood or middle age. If traumatic, it is bilateral until proven otherwise.)
- Vascular
- Neurologic (ex.: Myasthenia gravis)
- Iatrogenic (ex.: Slipped muscle; following tenotomy or tenectomy procedures)
- Diabetic mononeuropathy
- Neoplastic
- Viral (ex.: Herpes zoster)
- Nasal sinus affections (ex.: Mucocele)
Bilateral Superior Oblique Underaction
Left hypertropia in right gaze and left tilt, right hypertropia in left gaze and right tilt, the hypertropia is less evident than in unilateral superior oblique paresis.
Other features: Larger extorsion than in unilateral paresis (>10º); esotropia increasing in down gaze (>10º) – V pattern of the ''arrow subtype''.[4] Sometimes bilateral involvement can be masked due to an asymmetrical involvement. Some signs that can be suggestive of bilateral involvement are the reversal of hypertropia on ipsilateral side gaze and contralateral head tilt[28], objective fundus extorsion [2] and a slight IO oblique overaction of the other eye,[4]as sometimes it becomes evident only after a surgical correction.[29]
Causes:[24]
- Trauma (The IV cranial nerves exit the midbrain very closely so that strong head traumas, or sometimes even small ones, frequently cause bilateral rather than unilateral palsies)
- Neoplastic
- Vascular
- Craniosynostosis
- Congenital (uncommon)
Treatment:
- For an acquired CN IV palsy, such as from microvascular disease or trauma, spontaneous resolution may occur over weeks to months.
- For smaller deviations, prism glasses may be adequate to manage symptoms.
- In children, patching may be used to help maintain attention to the palsied eye and treat/ prevent amblyopia.
- For cases that are not amenable to more conservative measures, such as those with a large deviation, significant incomitance, or a large degree of torsion, strabismus surgery can be consider. For an issue predominantly with torsion, a Harada Ito procedure, weakening only the anterior fibers of the superior oblique can be performed. Depending on the degree of deviation, degree of torsion, and gazes in which the deviation is most symptomatic, one or more cyclovertical muscles may be addressed surgically. Treatment of the oblique muscles can address a large degree of horizontal incomitance (>15 PD) or a large degree of torsion. For deviations that are greater in upgaze, ipsilateral inferior oblique weakening is frequently used while for deviations greater in downgaze, superior oblique strenthening is often used. For deviations with less than 15 PD of horizontal incomitance surgery on the vertical recti muscles and address the deviation. It is important to consider the impact of vertical rectus surgery on torsion. If a significant degree of extorsion is present, weakening of the ipsilateral superior rectus or strengthening of the ipsilateral inferior rectus my worsen the degree of torsion. Weakening of the contralateral inferior rectus can improve alignment, especially if worse in downgaze, and extorsion. Large angle deviations may require surgery on more than one cyclovertical muscle, simultaneously or sequetially.
Inferior Oblique Overaction
Over-elevation of the eye in adduction
Other features: It may be primary or secondary, due to paresis of the ipsilateral superior oblique. Limited elevation of the contralateral eye in abduction may also be interpreted as inferior oblique overaction. It may result in Y or V pattern strabismus. When it is primary, the head tilt- test is negative (the superior rectus and oblique muscles are ‘’working’’).[4]
It is frequently bilateral and associated with a horizontal strabismus, especially if present since infancy, although it may be isolated.
Causes:
- Primary
- Secondary to an ipsilateral superior oblique paresis or apparent inferior oblique overaction due to contralateral superior rectus paresis or contralateral inferior rectus restriction
Treatment: [4]
- If binocular fusion is compromised or for cosmetic reasons: A graded anteriorization of the IO is frequently sufficient. In this procedure it is important to keep the anterior IO fibers posterior to the IR insertion in order to avoid a hypercorrection and consequent hypodeviation.
- If bilateral, even if asymmetric, consider a bilateral IO weakening procedures (myectomy, recession, anteriorization), except if amblyopia is present (surgery on the good eye is discouraged).
- In the presence of a significant Y pattern in upgaze, even if there is no significant deviation in primary position or sidegaze: Bilateral IO weakening procedures
Superior Rectus Under-action of the Contralateral Eye
Leads to an elevation deficit/ vertical misalignment that is worst when the affected eye is abducted and with ipsilateral head tilt.
- Iatrogenic (ex.: Following superior rectus weakening procedures, glaucoma surgery, oculoplastic surgery, scleral buckle insertion.)
- Traumatic
- Innervational anomaly of the superior division of the III cranial nerve
- Muscle aplasia
- Neoplastic (ex.: Pineocytoma, orbital tumor)
Treatment of Superior Oblique Under-action
Unilateral:[4][2][34]
- If <10DP hypertropia in primary position, IO overaction more significant than SO underaction (deviation greater in upgaze): Ipsilateral graded inferior oblique anteriorization (weakening procedure)
- If >15DP hypertropia in primary position (or deviation bigger in downgaze): Ipsilateral graded inferior oblique anteriorization + contralateral inferior rectus recession (yoke muscle).
Superior oblique tightening procedures - "tucks"- are indicated in congenital SO palsy with tendon laxity tested through forced duction or when there is minimal IO overaction with the vertical deviation being greatest in downgaze. This procedure may cause iatrogenic Brown syndrome.
- If the deviation has become comitant due to superior and inferior rectus contractures, respective recessions should be performed
Bilateral:[4]
In the case of a traumatic cause, it is advised to wait for 6 months and reevaluate for a potential recovery.
- If main problem is extorsional diplopia (as in partially recovered post-traumatic paresis), with minimal hypertropia and V-pattern: Harada-Ito procedure.
- If a big V-pattern, with >15DP esotropia in downgaze and >10º extorsion in primary position is present; reversing hypertropias in sidegaze: Bilateral Harada-Ito + bilateral medial rectus recessions with half-tendon width inferior transpositions or superior oblique tendon tuck + bilateral medial rectus recessions with half-tendon width inferior transpositions.
- If masked bilateral involvement or asymmetric involvement is suspected: Bilateral IO graded anteriorization + contralateral IR recession or bilateral graded IO anteriorization + Harada-Ito procedure on the more affected side.
Over depression and over-elevation in adduction
Large Angle Exotropia
Hypertropia or hypotropia in in adduction. – X- pattern
It is caused by a tight, contracted lateral rectus. As the eye tries to adduct, it slips below or above the eyeball, causing an upward or downward vertical deviation[4][2]
Displaced Horizontal Recti or their Pulleys
If horizontal recti are displaced superiorly or inferiorly, they act as additional elevators or depressors. V and A patterns may result, simulating oblique muscle paresis/overactions.
- Congenital (ex.: Craniosynostosis; extorted orbit)
- Iatrogenic (ex.: Following strabismus surgery)
- High myopia, where a posterior staphyloma misplaces the lateral rectus inferiorly
- Relocate horizontal rectus muscle. Hereby, lateral recti are moved towards the open end of the pattern (up in V, down in A), while medial recti are transposed to the closed end of the pattern (down in V, up in A). Any easy mneumonic to remember this is MALE- medials toward the apex, laterals toward the empty space.
It is very important to correctly diagnose the cause of A and V patterns, because one may have the false impression of oblique muscle affection. If the A or V pattern is caused by a horizontal muscle displacement, it responds poorly to oblique muscle surgery.
Duane Syndrome
Sometimes associated with a upshoots and downshoots in adduction, due to aberrant innervation of vertical muscles or a restrictive lateral muscle causing a leash effect.
Treatment:[4]
It may be addressed surgically with a Y-splitting procedure of the ipsilateral lateral rectus muscle.
Other Forms of Vertical Strabismus
Thyroid Eye Disease
Thyroid eye disease leads to enlargement of the extraocular muscles and restrictive strabismus. Although any extra-ocular muscle can be involved, the inferior rectus is the most frequently affected, followed by the medial rectus muscle .[2][36] While thyroid eye disease can certainly lead to incomitant strabismus due to the involvement of multiple muscles, horizontal incomitance due to vertical muscle restriction is frequently not as marked as in other forms of vertical strabismus.
Associated findings include: Intraocular pressure may increase when looking away from the restriction, [4][2] proptosis, lid retraction, compressive optic nerve dysfunction, conjunctival hyperemia, chemosis, and corneal affections due to exposure[37][38][39]
Treatment:
- Medical: Teprotumumab is now frequently used for management and can lead to improvement in alignment and motility in a majority of patients, with a greater impact on vertical alignment.[40] Use of teprotumumab does not appear to significant impact success of strabismus surgery performed following teprotumumab therapy.[41] Systemic steroids and external beam radiation may be indicated to control inflammation. [4][2][42]
- Surgical: Strabismus surgery has to be postponed until after orbital decompression procedures have been performed and orbital inflammation is controlled. A waiting period of 6 to 12 month following thyroid function test stabilization is recommended. The procedure of choice is the recession of affected muscles. In the case of IR involvement with a vertical deviation >18-20DP, a bilateral recession is advised. Late overcorrections are frequent. Wright et al. advise the use of non-reabsorbable (ex.:6-0 Mersilene) sutures in order to avoid this complication. The use of adjustable sutures has also been advised by Lueder.[43][44]
Myasthenia Gravis
Variable hyperdeviations may be noted. A very rare form of isolated IR affection has been described.[45]
Orbital Causes of Vertical Restriction
Orbital wall fracture with entrapment, orbital mass, and orbital or extraocular muscle inflammation can lead to vertical strabismus
Canine Tooth Syndrome
In addition to the restrictive elevation, there is also a SO paresis. It is frequently traumatic.[4]
Pseudoinferior Rectus Palsy
Slight hypertropia in primary position as muscular function is preserved from upgaze to primary position, and a large hypertropia from primary position to downgaze. It can be caused by an adherence of the inferior rectus to the orbital floor following a traumatic fracture, giving rise to a muscle slack in front of the adherence. [4] Treatment:[4][2]
- If due to restriction and minimal hypertropia in primary gaze: resection of the ipsilateral IR.
- If a large hypertropia is present in primary gaze position: Ipsilateral IR resection + contralateral IR recession or SR surgery or either eye. An inverse Knapp procedure may be necessary.
- In the case of orbital floor fracture with hypotropia of the affected eye:
- Orbital floor repair, if indicated.
- If 8-15PD in primary position: Unilateral IR recession.
- If >15PD in primary position: Ipsilateral IR recession plus contralateral SR recession.
- In pseudo-inferior rectus palsy with hypertropia in primary position: Ipsilateral muscle slack reduction through a plication + contralateral IR recession.
Iatrogenic Strabismus
Frequently due to peri-orbital fat adhesions to the globe, leading to a restrictive syndrome (Ex.: pseudo-Brown's syndrome), or following retinal surgery:
- Scleral buckle with posterior slippage, entrapment or splitting of extraocular muscles and anterior displacement of an oblique muscle.[4][31]
- Following ocular surgery (Ex.: Strabismus surgery; glaucoma surgery, especially with the Baerveldt device or due to a mass effect caused by the bubble[32]; oculoplastic surgery)[33]
Congenital Fibrosis of the Extraocular Muscles:
May affect any extraocular muscle, but sometimes affects solely the inferior rectus. It is thought to be related to innervational and structural abnormalities of the extraocular muscles.[2][46][47]
Dissociated Vertical Deviation
A dissociated vertical deviation is an upward drift of one eye when binocular fusion is interrupted (such as with alternate cover testing) that is not associated with a compensatory downward shift of the fellow eye when attention is focused on the drifting eye. For example, on alternate cover testing, the right eye would drift upward when covered and be seen to come down when the left eye is covered. When the cover is switched back to the right eye again, there is NO upward refixation movement of the left eye. With a bilateral dissociated vertical deviation, both eyes are seen to drift up when covered and re-fixate with a downward movement when uncovered. It manifests when binocular fusion is interrupted either by occlusion or by spontaneous dissociation.[4]
Other features: Abduction and extorsion. Increased vertical deviation on head tilt to the ipsilateral side.[4]
Most frequently both eyes are affected, although it may be asymmetrical . When bilateral, the vertical deviation of each eye is not related to the other, as in true hypertropia (no yoke muscle overaction is present).[4][48]
Cause: Any cause leading to a disruption of normal binocular development can be at its origin. Rarely primary.
- If cosmetically intolerable or if noticeable:
- If associated with an IO overaction: Sole IO graded anteriorization
- If associated with an SO overaction: Treat the A pattern with horizontal muscle transpositions, or an undercorrected SO weakening procedure, since the latter may aggravate the symptoms of DVD
- If both eyes can fixate: Bilateral SR recessions, with asymmetric recessions if asymmetric
- If overcorrected: Associate an IR plication or resection
Additional surgical management of vertical deviations is available: Strabismus Surgery, Cyclovertical
Skew Deviation:
An acquired vertical strabismus due to central or peripheral asymmetric disruption of supranuclear input from the otolith organs. A skew deviation may appear as comitant or incomitant and may not localize on a three step test. The etiology includes stroke or the brainstem or cerebellum, trauma, demyelinating disease, inflammation, tumor, abscess, iatrogenic from surgery, Arnold-Chiari malformation, and Creutzfelt-Jakob diseae. The physciain should attempt to determine the underlying etiology and address if possible, which may lead to resolution of the skew deviaiton in some cases.
Diagnostic Challenges in Vertical Strabismus
Differentiating between a Paresis and a Restriction of the Antagonist
Forced Duction Test: Forced duction testing can evaluate for evidence of restriction and possibly of laxity in the setting of a muscle palsy
Saccadic Eye Movements: In the case of a restriction, normal saccadic eye movements can be observed until the full restrictive amplitude is achieved, where it stops abruptly. In the case of a palsy, saccadic velocity and force generation are decreased
Intraocular Pressure: Restrictions may lead to increase IOPs when the eye is moving against the restriction.
Lid fissure: Restrictions may cause lid fissure narrowing, while a paresis causes lid fissure widening.[4]
Differentiating between Brown’s Syndrome, Superior Oblique Overaction and Inferior Oblique Paresis
Patients with Brown’s syndrome will have a positive forced-duction test especially evident on the Guyton’s exaggerated forced-duction test[49]. In Brown’s syndrome there is a Y-pattern, whereas a lambda pattern is present in SO overaction and an A pattern in IO paresis. To distinguish between a IO paresis and a SO overaction see head-tilt-test above. A Y pattern can also be present when there is an aberrant innervation of the lateral recti, in upgaze,[50] or in the case of a bilateral inferior oblique overaction (see above).[51]
Differential Diagnosis between DVD and Inferior Oblique Overaction
In inferior oblique overaction there is an increase of ipsilateral hypertropia in adduction to the contralateral side with a contralateral hypotropia. In a DVD when binocular fusion is interrupted, there is a hypertropia in adduction as well as in abduction without a true contralateral hypotropia (the eye with the DVD will be seen to shift downward without a compensatory upward movement of the fellow eye on alternate cover testing). In order to evaluate this, the physician needs to check for a vertical deviation of the occluded eye, while the patient looks to either side.[4] Translucent occluders of Spielman are particularly helpful.[52]
References
- ↑ American Academy of Ophthalmology. Strabismus. https://www.aao.org/image/strabismus-5 Accessed January 29, 2020.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 American Academy of Ophthalmol. Pediatric Ophthalmology and Strabismus. BCSC, 2014-2015.
- ↑ 3.0 3.1 Garg, A, Alio JL. Surgical Techniques in Ophthalmology: Oculoplasty and Reconstructive Surgery. Jitendar P Vij, NDheli, 2010
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 4.16 4.17 4.18 4.19 4.20 4.21 4.22 4.23 4.24 4.25 4.26 4.27 4.28 4.29 4.30 4.31 4.32 4.33 4.34 4.35 4.36 4.37 4.38 Wright K, Spiegel P, Thompson L. Handbook of Pediatric Strabismus and Amblyopia. Springer, 2006. Print.
- ↑ Metz HS. Double elevator palsy. Arch Ophthalmol 1979; 97:901– 909.
- ↑ Romano P, Roholt P. Measured graduated recession of the superior oblique muscle. J AAPOS 1983;20:134–140.
- ↑ Berke RN. Tenotomy of the superior oblique for hypertropia. Trans Am Ophthalmol Soc 1946;44:304–342.
- ↑ Ventura MP, Vianna R , Souza J, Solari HP and Curi RLN. Acquired Brown's syndrome secondary to Ahmed valve implant for neovascular glaucoma. Eye. 2005; 19:230–232.
- ↑ Prata JA, Minckler DS, Green RL. Pseudo-Brown's syndrome as a complication of glaucoma drainage implant surgery. Ophthalmic Surgery. 1993, 24:608-611
- ↑ Neely KA, Ernest JT, Mottier M, Combined Superior Oblique Paresis and Brown's Syndrome After Blepharoplasty. M.Journal of Clinical Neuro-Ophthalmology. 1990, 10:293
- ↑ Leibovitch I, Wormald P, Iatrogenic Brown's Syndrome During Endoscopic Sinus Surgery With Powered Instruments. Otolaryngology-- Head and Neck Surgery. 2005, 133:300-301.
- ↑ Cooper C, Kirwan JR, McGill NW, Dieppe PA. Brown's syndrome: an unusual ocular complication of rheumatoid arthritis. Ann Rheum Dis 1990;49:188-189
- ↑ Alonso-Valdivielso JL, Lario BA, López JA, Tous MJS, Gómez AB. Acquired Brown's syndrome in a patient with systemic lupus erythematosus. Ann Rheum Dis 1993;52:63.
- ↑ Thacker NM, Velez FG, Demer JL, Rosenbaum AL. Superior Oblique Muscle Involvement in Thyroid Ophthalmopathy J AAPOS 2005;9:174–178.
- ↑ Gregersen E, Rindziunski E. Brown's syndrome. A longitudinal long-term study of spontaneous course. Acta Ophthal. 1993,71:371–376.
- ↑ Dawson E, Barry J, Lee J. Spontaneous resolution in patients with congenital Brown syndrome. J AAPOS 2009,13:116–118
- ↑ Brown H. Isolated Inferior Oblique Paralysis: An Analysis of 97 Cases. Trans Am Ophthalmol Soc. 1957;55:415-454
- ↑ Castro O, Johnson LD, Mamourian AC. Isolated Inferior Oblique Paresis from Brain-Stem Infarction: Perspective on Oculomotor Fascicular Organization in the Ventral Midbrain Tegmentum Arch Neurol. 1990;47:235-237
- ↑ Pusateri TJ, Sedwick LA, Margo CE. Isolated Inferior Rectus Muscle Palsy From a Solitary Metastasis to the Oculomotor Nucleus. Arch Ophthalmol 1987;105:675-7.
- ↑ Spoor TC, Shippman S. Myasthenia Gravis Presenting as an Isolated Inferior Rectus Paresis. Ophthalmol.1979; 86:2158–2160.
- ↑ Walker JPS, Congenital absence of inferior rectus and external rectus muscles. Brit. J. Ophthal.1954;38:631.
- ↑ Sergott RC, Glaser JS. Graves' ophthalmopathy. A clinical and immunologic review. Surv Ophthalmol. 1981; 26:1-21.
- ↑ Megha M, Tollefson, Mohney BG, Diehl N, Burke JP. Incidence and Types of Childhood Hypertropia A Population-Based Study.Ophthalmol. 2006;113:1142-1145.
- ↑ 24.0 24.1 Mollan SP, Edwards JH,Price A, Abbott J, BurdonA. Etiology and outcomes of adult superior oblique palsies: a modern series Eye. 2009; 23, 640–644
- ↑ Gunther K. Superior oblique paralysis. Aust J Ophthalmol 2007;7:44-48
- ↑ Yang HK, Kim JH, Hwang JM. Congenital superior oblique palsy and trochlear nerve absence: a clinical and radiological study. Ophthalmol. 2012;119:170- 177.
- ↑ Pineles SL, Velez FG, Elliot RL, Rosenbaum AL. Superior oblique muscle paresis and restriction secondary to orbital mucocele. J AAPOS 2007;11:60–61
- ↑ Souza-Dias, C. Asymmetrical bilateral paresis of the superior oblique muscle. J AAPOS 2007; 11: 12–16
- ↑ Esmail F, Flanders M. Masked bilateral superior oblique palsy. Can J Ophthalmol. 2003;38:476–481.
- ↑ Munoz M, Page LK. Acquired double elevator palsy in a child with pineacytoma. Am J Ophthalmol 1994; 118:810-1.
- ↑ 31.0 31.1 Farr AK, Guyton DL. Strabismus after retinal detachment surgery Curr Op Ophthalmol. 2000; 11:207-210.
- ↑ 32.0 32.1 Munoz M, Parrish Rk. Strabismus Following Implantation of Baerveldt Drainage Devices. Arch Ophthalmol. 1993;111:1096-1099
- ↑ 33.0 33.1 Mazow ML, Avilla CW. Restrictive Horizontal Strabismus Following Blepharoplasty. Am J Ophthalmol. 2006; 141:773-774.
- ↑ Plager A, Buckley EG. Strabismus Surgery: Basic and Advanced Strategies. Oxford UP, NY. 2004. Print.
- ↑ Rosenberg JB, Tepper OM, Medow NB. Strabismus in craniosynostosis.J AAPOS 201350: 140-148.
- ↑ Prendiville P, Chopra M, Gauderman WJ, Feldon SE. The role of restricted motility in determining outcomes for vertical strabismus surgery in Graves’ ophthalmology. Ophthalmol. 2000;107:545– 549.
- ↑ Bartley GB, Gorman CA. Diagnostic Criteria for Graves' Ophthalmopathy. Ophthalmol 1995; 119:792–795.
- ↑ Mourits M, Koornneef L, Wiersinga M,Prummel. Clinical criteria for the assessment of disease activity in Graves' ophthalmopathy: a novel approach. Br J Ophthalmol. 1989; 73:639-644
- ↑ Mario Salvi, Davide Dazzi, Isabella Pellistri Classification and prediction of the progression of thyroid-associated ophthalmopathy by an artificial neural network. Ophthalmol. 2002; 109:1703–1708
- ↑ Dallalzadeh LO, Villatoro GA, Chen L, Sim MS, Movaghar M, Robbins SL, Karlin JN, Khitri MR, Velez FG, Korn BS, Demer JL, Rootman DB, Granet DB, Kikkawa DO. Teprotumumab for Thyroid Eye Disease-related Strabismus. Ophthalmic Plast Reconstr Surg. 2024 Jul-Aug 01;40(4):434-439. doi: 10.1097/IOP.0000000000002611. Epub 2024 Feb 2. PMID: 38319994.
- ↑ Hilliard G, Pruett J, Donahue SP, Velez FG, Peragallo JH, Ditta LC, Tavakoli M, Hoehn ME, Kuo AF, Indaram M, Kerr NC. Outcomes of Strabismus Surgery Following Teprotumumab Therapy. Am J Ophthalmol. 2024 Jun;262:186-191. doi: 10.1016/j.ajo.2024.01.005. Epub 2024 Jan 6. PMID: 38191066.
- ↑ Cockerham KP, Kennerdell JS. Does radiotherapy have a role in the management of thyroid orbitopathy? Br J Ophthalmol 2002;86:102-107
- ↑ Harrad R. Management of strabismus in thyroid eye disease. Eye 2015;29:234-237
- ↑ Lueder GT, Scott WE, Kutschke PJ, Keech RV. Long-term Results of Adjustable Suture Surgery for Strabismus Secondary to Thyroid Ophthalmopathy. Ophthalmology. 1992;99:993–997
- ↑ Spoor TC, Shipmann S. Myasthenia Gravis Presenting as an Isolated Inferior Rectus Paresis Ophthalmol. 1979; 86: 2158-2160
- ↑ Heidary G, Engle EC, Hunter DG. Congenital fibrosis of the extraocular muscles. Ophthalmol. 2008;23(1):3-8.
- ↑ Yazdani A, Traboulsi EI. Classification and surgical management of patients with familial and sporadic forms of congenital fibrosis of the extraocular muscles. Ophthamol. 2004;111:1035-1042.
- ↑ Guyton DL. Dissociated vertical deviation: Etiology, mechanism, and associated phenomena.J AAPOS. 2000,4: 131–144.
- ↑ Guyton DL. Exaggerated traction test for the oblique muscles. Ophthalmology. 1981;88(10):1035-1040. doi:10.1016/s0161-6420(81)80033-4
- ↑ Kushner BJ. Errors in the Three-step Test in the Diagnosis of Vertical Strabismus. Ophthalmol. 1989; 96: 127-132
- ↑ Kushner BJ. Pseudo inferior oblique overaction associated with Y and V patterns. Ophthalmol.1991; 98:1500-1505.
- ↑ Spielmann A. A translucent occluder for study of eye position under unilateral or bilateral cover test. Am Orthoptics J1986;36:65.