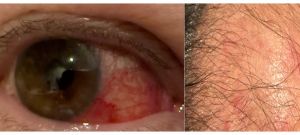
Sweet Syndrome (Acute Febrile Neutrophilic Dermatosis)
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Sweet syndrome (SS), also known as acute febrile neutrophilic dermatosis, is a primarily dermatologic, auto-inflammatory disorder with accompanying features of systemic inflammation, including inflammation of the eye.[1] [2]
Ocular manifestations of SS include periorbital and orbital inflammation, dacryoadenitis, conjunctivitis, episcleritis, scleritis, limbal nodules, peripheral ulcerative keratitis, iritis, glaucoma, choroiditis, retinal vasculitis, and optic nerve involvement although it is most commonly associated with conjunctivitis.[1][3] [4]
Etiology
There are three etiologies associated with SS. The classic/idiopathic type is, per its name, of unclear etiology, although it can be seen in association with upper respiratory tract or gastrointestinal infection, inflammatory bowel disease, or pregnancy.[1][5]
The malignancy-associated type can precede, follow, or appear concurrently with a patient’s diagnosis of neoplasm.[6] Approximately 85% of malignancy-associated cases are linked to hematological cancers, most commonly to acute myelogenous leukemia (AML).[2][7]
Lastly, a drug-induced type can occur, most commonly seen in those receiving granulocyte colony-stimulating factor.[7] Case reports have also associated sulfamethoxazole and trimethoprim and several anticancer agents, including all trans-retinoic acid proteasome inhibitors, hypomethylating agents, tyrosine kinase inhibitors, and lenalidomide, with SS.[7]
Epidemiology
Sweet syndrome is more commonly found in women with an estimated female-to-male ratio of 2-3:1.[5] The disease tends to affect women aged 30-50 years and men aged 50-90 years, although all age-groups can be affected.[1] [5]
An estimated 38-53% of SS cases are considered classical/idiopathic.[8] Recurrence rates are high and can occur in up to one-third of classical SS patients.[5] The malignancy-associated form occurs with the onset or recurrence of cancer, accounting for 25-44% of cases.[8] Medication-induced cases are responsible for 4-24% of cases.[8]
Sweet syndrome manifests with extra-cutaneous features in up to 50% of cases.[5] However, the precise prevalence of ocular involvement amongst SS patients remains uncertain. A review of 138 patients with SS reported eye involvement in only 3% of cases.[2] However, a 2008 evaluation of case reports in the literature suggests ocular infiltration occurs in about one-third of patients.[1] Ocular lesions are reported to be uncommon, although not impossible, in malignancy-associated and drug-induced forms of SS.[5] Other sites of extra-cutaneous involvement can include the musculoskeletal system, liver, brain, kidneys, lungs, and spleen.[2][5]
Pathophysiology
The exact pathophysiology of SS has yet to be elucidated, however it is strongly believed that the disease is due to hypersensitivity mediated by cytokines and neutrophils activated by interleukin-1.[7] Circulating autoantibodies, cytokines, dermal dendrocytes, HLA serotypes, immune complexes, leukotactic mechanisms, and type 1 T helper cells have all been suggested as factors contributing to the pathogenesis of SS.[7] Notably, inflammatory cell markers such as CD3, CD163, myeloperoxidase, metalloproteinases, and vascular endothelial growth factors, are found at higher values in the lesioned skin of SS patients compared to non-SS individuals or those with another neutrophilic dermatoses.[9]
There is no consistent evidence of a genetic predisposition for SS, however there are documented associations between HLA-B54 typing and SS, particularly amongst Japanese patients.[3] Analysis of HLA antigens in a Caucasian population, however, showed no association between SS and specific HLA-ABC antigens.[10]
Currently, as of 2022, there is no available literature specifying a distinct pathophysiology describing ocular involvement in SS, however it can be assumed that auto-inflammatory mechanisms are involved.
Diagnosis
Systemic Findings
Clinical Presentation
Sweet syndrome classically presents with an abrupt onset of violaceous or erythematous appearing papules, plaques, or nodules typically spanning several millimeters or centimeters.[11] Cutaneous lesions are tender to touch but rarely pruritic with an asymmetrical distribution that favors the upper extremities.[11][12] Headache, myalgias, arthralgias and malaise most commonly accompany the onset of dermatologic disease.[11] Fever is frequently seen but spares some patients and is not required for diagnosis.[11] Neutrophilic infiltration of other organ systems is highly variable with ocular and musculoskeletal involvement reported most.[5][11]
Ocular Manifestations
Ocular complaints may affect up to one-third of patients with SS.[1] Ophthalmologic findings of SS are highly varied and span nearly all aspects of the eye and surrounding structures. Case reports now recognize a spectrum of disease that includes pathology of the orbit, eyelids, anterior and posterior segments.[1] Other presentations including panuveitis with optic nerve involvement and inflammatory glaucoma have been described.[3][13] Roughly half of ocular pathology seen in SS presents bilaterally.[1] Generally, ophthalmologic manifestations present concurrently or within a few days of dermatologic findings.[1] An extensive list of ophthalmologic presentations is outlined in Table 1.
| Orbit | Periorbital vesicular eruption |
| Eyelids | Vesicular eyelid lesions, dacryoadenitis |
| Anterior Segment
Cornea: Episclera/Sclera: Iris/Ciliary body |
Iritis, Episcleritis, Scleritis, Conjunctivitis, Peripheral ulcerative keratitis, Limbal nodules |
| Posterior Segment
Retina: Choroid: |
Choroiditis, Retinal vasculitis, Vitritis |
| Neuro-ophthalmological/Other | Inflammatory Glaucoma, Panuveitis with optic nerve involvement |
Periorbital and Eyelid Involvement
An erythematous vesicular eruption of the periorbital skin and eyelids is most common.[1][14][15] [16] [17] Vesicular eruptions may be associated with painful eyelid swelling, limited ocular movement and an elevated leukocyte count.[17] Hence, SS of the periorbital space may be confused for orbital cellulitis on presentation.[17] A single case of dacryoadenitis associated with SS demonstrated orbital fat and lacrimal gland infiltration on computed tomography.[18] While not routinely indicated, periorbital skin biopsy reveals similar pathologic changes, notably mature neutrophilic infiltrates, to those seen in other dermal lesions.[16] Periorbital and eyelid eruptions readily respond to systemic corticosteroids.[1] As such, topical corticosteroids are rarely indicated.[1]
Anterior Segment
Conjunctivitis is the most common ocular manifestation of SS, yet a spectrum of anterior segment pathologies exist.[1] Iritis, episcleritis, scleritis, and peripheral ulcerative keratitis are all documented in patients presenting with SS.[1] Additionally, limbal nodules with similar histopathologic changes to those seen in other SS dermal lesions can arise.[19] Most commonly, patients with anterior pathology endorse hyperemia with irritation and eye watering.[1] Blurred vision may also be seen in patients with ocular pathology limited to the anterior segment.[20] Slit lamp examination should be utilized to evaluate anterior segment inflammation.[1] A robust response to systemic corticosteroids is commonly seen with anterior segment pathologies.[1]
Posterior Segment
While anterior segment involvement is more common, pathology involving posterior structures is also possible in SS.[4] Choroiditis, retinal vasculitis, and vitritis have all been described in SS patients.[4] [8][21] Sudden decreased vision is common among those with retinal vasculitis.[4] Patients may also endorse more mild blurred vision or other visual defects like floaters or scotomas.[4] Slit lamp exam should be used to reveal vitreous inflammation if it exists.[4] Retinal examination may uncover exudation along vessels and intraretinal hemorrhages.[4] Fluorescence angiography may reveal ischemic changes and compensatory corkscrew vessels consistent with retinal vasculitis.[4] In addition to systemic corticosteroids, more invasive therapeutic measures including intravitreal bevacizumab and retinal photocoagulation may be warranted when vision is threatened.[4][8]
Neuro-Ophthalmologic & Other Manifestations
Rarely, SS may present with involvement of the optic nerve. A single case of idiopathic panuveitis presenting with decreased vision and optic disc edema demonstrated enhancement of the optic nerve on brain MRI.[22] Another case of SS associated with microscopic polyangiitis presented similarly yet brain MRI was less revealing.[23] Panuveitis and papilledema quickly resolved in both patients with the initiation of either steroids or immunomodulators.[22] [23] Interestingly, a single case of inflammatory glaucoma associated with SS has also been documented.[13]
Diagnostic Criteria
Diagnostic criteria for SS was originally proposed by Su and Liu in 1986 and revised by Von Den Driesch in 1994.[5][24] [25] A summary of these criteria are listed in Table 2.
|
|
Drug-induced SS | |
| Major Criteria | 1 Abrupt onset of painful erythematous plaques or nodules | An Abrupt onset of painful erythematous plaques or nodules |
| 2 histopathologic evidence of a dense neutrophilic infiltrate without evidence of leukocytoclastic vasculitis | B Histopathologic evidence of a dense neutrophilic infiltrate without evidence of leukocytoclastic vasculitis | |
| Minor Criteria | 3 Pyrexia >38 C | C Pyrexia >38 C |
| 4 Association with an underlying hematologic or visceral malignancy, inflammatory disease, or pregnancy, OR preceded by an upper respiratory or gastrointestinal infection or vaccination | D Temporal relationship between drug ingestion and clinical presentation, OR temporally related recurrence after oral challenge | |
| 5 Excellent response to treatment with systemic corticosteroids or potassium iodide | E Temporally related resolution of lesions after drug withdrawal or treatment with systemic corticosteroids | |
| 6 Abnormal laboratory values at presentation (three of four): erythrocyte sedimentation rate >20 mm/hr; positive C-reactive protein; >8,000 leukocytes; >70% neutrophils | ||
The presence of both major criteria and two of the four minor criteria is required to establish the diagnosis of classical SS or malignancy-associated SS.[5][25]
All five criteria (A-E) are required to establish the diagnosis of drug-induced SS.[5][25]
Malignancy-associated SS initially was considered as a subtype of classical SS, however some may choose to distinguish between classical and malignancy-associated SS.[5]
Diagnostic Testing and Supportive Lab Values
Laboratory evaluation should include a complete blood cell count with leukocyte differential and platelet count, acute phase reactants (i.e., erythrocyte sedimentation rate, C-reactive protein), serum chemistries, and a urinalysis. Laboratory values demonstrating peripheral leukocytosis with neutrophilia and an elevated erythrocyte sedimentation rate are the most consistent abnormalities found in SS patients, but are not always observed in confirmed cases.[5] [6][26] Malignancy-associated SS patients may also be found with either anemia, neutropenia, and/or abnormal platelet counts.[5] Abnormalities in serum chemistries, urinalysis, and acute phase reactants may signal extracutaneous involvement.[5] Additional viral, bacterial, fungal, mycobacterial, and/or autoimmune workup may be reasonable to rule out other probable causes.[5][27]
Lesional skin biopsy for routine histopathologic evaluation is a useful procedure to confirm a diagnosis of SS.[5] Additionally, extracutaneous manifestations of SS may be found on brain single photon emission computed tomography (SPECT), computerized axial tomography (CT), magnetic resonance imaging (MRI), and cerebrospinal fluid analysis.[5]
Ocular manifestations of SS are highly variable and diagnostic evaluation should be a tailored choice depending on the patient’s presenting symptoms. Slit lamp and fundoscopic examination should be utilized to evaluate possible anterior and posterior pathology in every patient.[1] Suspected posterior infiltration warrants further examination. Enhanced-depth imaging optical coherence tomography (EDI-OCT) imaging, B-scan ultrasonography, and fluorescein angiography may be helpful in identifying the effusion, choroidal infiltration, diffuse scleritis, retinal vasculitis, and/or inflammation seen in SS.[4] [8] Additionally, brain magnetic resonance imaging may be warranted when involvement of the optic nerve is suspected.[22]
Differential Diagnosis
The differential diagnosis of SS is extensive but notably includes erythema multiforme (EM), erythema nodosum (EN), and Behçet disease.[5][10][28] Patients with EM may have a history of herpes simplex infection, recurrence of SS symptoms, and drug intolerance with normal-moderately abnormal inflammatory marker levels.[29] Patients with EN will have similar history and laboratory results to SS patients but may have skin lesions confined to their lower extremities with different histologic features on biopsy.[5][30] Behçet patients present similarly to SS patients, however skin lesions may be more pustular in quality with vasculitis and positive immunofluorescence on histology.[25][31] Additionally, while SS patients may be HLA-B54 positive, Behçet patients are more likely to be HLA-B51 positive.[31] Ocular manifestations are common among systemic inflammatory disorders and ultimately diagnostic criteria should be utilized to differentiate between overlapping findings.[4]
Management
Treatment
The management of SS varies according to the etiology of disease – idiopathic, malignancy-associated, or drug-induced.[12] Malignancy-associated SS has been shown to resolve with control of the underlying cancer.[32] Similarly, drug-induced SS often improves within weeks of withdrawal of the offending medication.[33] However, resolution of SS is not guaranteed, and pharmacologic therapy should be initiated to accelerate clinical improvement, regardless of etiology.[33] Systemic corticosteroid therapy is considered first-line treatment for SS independent of disease presentation.[33] An individualized approach for recalcitrant and extensive disease may be warranted consisting of intralesional corticosteroid therapy or alternative glucocorticoid-sparing agents.[33] Ocular manifestations of SS quickly respond to systemic corticosteroid use however intra-ocular steroids may improve outcomes for severe disease.[1] [4] [8] Sight threatening retinal vasculitis associated with SS may require more invasive therapeutic measures including intravitreal bevacizumab and retinal photocoagulation.[4]
Prognosis
While the initiation of therapy typically provides an early and robust response to SS, the rate of recurrence following tapering, or discontinuation of systemic steroids remains high regardless of etiology.[33] However, recalcitrant and relapsing disease remains extremely rare for ocular manifestations of SS.[1][4][8] Significant and lasting visual impairment is unlikely with permanent vision changes limited only to cases of severe retinal vasculitis.[4] Idiopathic cases of SS require monitoring of underlying hematologic malignancies that may present up to 16 months following dermatologic and ocular manifestations.[2]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 Gottlieb CC, Mishra A, Belliveau D, Green P, Heathcote JG. Ocular involvement in acute febrile neutrophilic dermatosis (Sweet syndrome): new cases and review of the literature. Surv Ophthalmol. 2008;53(3):219-226. doi:10.1016/j.survophthal.2008.02.006
- ↑ 2.0 2.1 2.2 2.3 2.4 Marcoval J, Martín-Callizo C, Valentí-Medina F, Bonfill-Ortí M, Martínez-Molina L. Sweet syndrome: long-term follow-up of 138 patients. Clinical and Experimental Dermatology. 2016;41(7):741-746. doi:10.1111/ced.12899
- ↑ 3.0 3.1 3.2 3.3 Hisanaga K, Iwasaki Y, Itoyama Y, Neuro-Sweet Disease Study Group. Neuro-Sweet disease: clinical manifestations and criteria for diagnosis. Neurology. 2005;64(10):1756-1761. doi:10.1212/01.WNL.0000161848.34159.B5
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 Baartman B, Kosari P, Warren CC, et al. Sight-threatening ocular manifestations of acute febrile neutrophilic dermatosis (Sweet’s syndrome). Dermatology. 2014;228(3):193-197. doi:10.1159/000357729
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 5.12 5.13 5.14 5.15 5.16 5.17 5.18 5.19 5.20 Cohen PR. Sweet’s syndrome – a comprehensive review of an acute febrile neutrophilic dermatosis. Orphanet J Rare Dis. 2007;2:34. doi:10.1186/1750-1172-2-34
- ↑ 6.0 6.1 Cohen PR, Talpaz M, Kurzrock R. Malignancy-associated Sweet’s syndrome: review of the world literature. J Clin Oncol. 1988;6(12):1887-1897. doi:10.1200/JCO.1988.6.12.1887
- ↑ 7.0 7.1 7.2 7.3 7.4 Villarreal-Villarreal CD, Ocampo-Candiani J, Villarreal-Martínez A. Sweet Syndrome: A Review and Update. Actas Dermosifiliogr. 2016;107(5):369-378. doi:10.1016/j.ad.2015.12.001
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 8.7 Mishra AV, Fung AT, Pollmann AS, Henderson R, Shields C, Gupta RR. Relentlessly Progressive Sweet Syndrome of the Eye with Scleritis and Choroidal Infiltration. Ocular Immunology and Inflammation. 2022;30(1):90-94. doi:10.1080/09273948.2020.1788611
- ↑ Marzano AV, Cugno M, Trevisan V, et al. Inflammatory Cells, Cytokines and Matrix Metalloproteinases in Amicrobial Pustulosis of the Folds and other Neutrophilic Dermatoses. Int J Immunopathol Pharmacol. 2011;24(2):451-460. doi:10.1177/039463201102400218
- ↑ 10.0 10.1 von den Driesch P, Simon M, Djawari D, Wassmuth R. Analysis of HLA antigens in Caucasian patients with acute febrile neutrophilic dermatosis (Sweet’s syndrome). Journal of the American Academy of Dermatology. 1997;37(2, Part 1):276-278. doi:10.1016/S0190-9622(97)80142-9
- ↑ 11.0 11.1 11.2 11.3 11.4 Alavi A, Sajic D, Cerci FB, Ghazarian D, Rosenbach M, Jorizzo J. Neutrophilic dermatoses: an update. Am J Clin Dermatol. 2014;15(5):413-423. doi:10.1007/s40257-014-0092-6
- ↑ 12.0 12.1 Rochet NM, Chavan RN, Cappel MA, Wada DA, Gibson LE. Sweet syndrome: clinical presentation, associations, and response to treatment in 77 patients. J Am Acad Dermatol. 2013;69(4):557-564. doi:10.1016/j.jaad.2013.06.023
- ↑ 13.0 13.1 Fourman S. Inflammatory Glaucoma Associated With Sweet’s Syndrome. American journal of ophthalmology. 1988;105(6):691-692. doi:10.1016/0002-9394(88)90072-4
- ↑ Bulengo-Ransby SM, Brown MD, Dubin HV, Rasmussen JE, Nickoloff BJ. Sweet’s syndrome presenting as an unusual periorbital eruption. J Am Acad Dermatol. 1991;24(1):140-141. doi:10.1016/s0190-9622(08)80050-3
- ↑ Anwar S, Hassan S, Fern AI, Douglas WS, Mann B. Bilateral periocular swelling in Sweet’s syndrome. Eye. 2004;18(2):214-216. doi:10.1038/sj.eye.6700588
- ↑ 16.0 16.1 Morgan KW, Callen JP. Sweet’s syndrome in acute myelogenous leukemia presenting as periorbital cellulitis with an infiltrate of leukemic cells. J Am Acad Dermatol. 2001;45(4):590-595. doi:10.1067/mjd.2001.119032
- ↑ 17.0 17.1 17.2 Oshitari K, Hida T, Takahashi M, Okada AA, Shiobara T. [Sweet syndrome presenting as orbital cellulitis]. Nippon Ganka Gakkai Zasshi. 2004;108(3):162-165.
- ↑ Maalouf T, Angioi K, Ssi-Yan-Kai I, Vernerey F, Witz B, George J. Dacryoadenitis associated with subcutaneous Sweet’s syndrome in a patient with acute myeloid leukemia. Orbit. 2005;24(1):55-57. doi:10.1080/01676830590903562
- ↑ Davies R. Limbal nodules in Sweet’s syndrome. Aust N Z J Ophthalmol. 1992;20(3):263-265. doi:10.1111/j.1442-9071.1992.tb00951.x
- ↑ Wang W, Wang X, Zhao H, Cui Y. A Case Report of Sweet’s Syndrome with Panuveitis and Rhegmatogenous Retinal Detachment. Ocul Immunol Inflamm. 2021;29(7-8):1345-1347. doi:10.1080/09273948.2020.1746357
- ↑ Salvador-Osuna C, Fernandez-Mosteirin N, Mayayo P, Delgado P, Giralt M. Choroiditis as systemic manifestation of a Sweet’s syndrome associated to myelodysplasia: a case report. Haematologica (Roma). 2002;87(1):ECR07-.
- ↑ 22.0 22.1 22.2 Lobo AM, Stacy R, Cestari D, Stone JH, Jakobiec FA, Sobrin L. Optic nerve involvement with panuveitis in Sweet syndrome. Ocul Immunol Inflamm. 2011;19(3):167-170. doi:10.3109/09273948.2011.560411
- ↑ 23.0 23.1 Sudhakar P, Tobin S, O Connor W, Kedar S. Neuro-Ophthalmic Presentation of Neuro-Sweet Disease. Neuroophthalmology. 2017;41(4):202-206. doi:10.1080/01658107.2017.1291687
- ↑ 24.0 24.1 Su WP, Liu HN. Diagnostic criteria for Sweet’s syndrome. Cutis. 1986;37(3):167-174.
- ↑ 25.0 25.1 25.2 25.3 25.4 von den Driesch P. Sweet’s syndrome (acute febrile neutrophilic dermatosis). J Am Acad Dermatol. 1994;31(4):535-556; quiz 557-560. doi:10.1016/s0190-9622(94)70215-2
- ↑ Cohen PR, Kurzrock R. Sweet’s syndrome: a neutrophilic dermatosis classically associated with acute onset and fever. Clin Dermatol. 2000;18(3):265-282. doi:10.1016/s0738-081x(99)00129-7
- ↑ Cohen PR, Kurzrock R. Sweet’s syndrome revisited: a review of disease concepts. Int J Dermatol. 2003;42(10):761-778. doi:10.1046/j.1365-4362.2003.01891.x
- ↑ Cohen PR, Kurzrock R. Sweet’s syndrome and cancer. Clin Dermatol. 1993;11(1):149-157. doi:10.1016/0738-081x(93)90112-p
- ↑ Trayes KP, Love G, Studdiford JS. Erythema Multiforme: Recognition and Management. Am Fam Physician. 2019;100(2):82-88.
- ↑ Suzuki Y, Kuroda K, Kojima T, Fujita M, Iseki T, Shinkai H. Unusual cutaneous manifestations of myelodysplastic syndrome. Br J Dermatol. 1995;133(3):483-486. doi:10.1111/j.1365-2133.1995.tb02684.x
- ↑ 31.0 31.1 Karadoğan SK, Başkan EB, Alkan G, Saricaoğlu H, Tunali S. Generalized Sweet syndrome lesions associated with Behçet disease: a true association or simply co-morbidity? Am J Clin Dermatol. 2009;10(5):331-335. doi:10.2165/11310790-000000000-00000
- ↑ O’Connor Reina C, Garcia Iriarte MT, Rodriguez Diaz A, Gomez Angel D, Garcia Monge E, Sanchez Conejo-Mir J. Tonsil cancer and Sweet’s syndrome. Otolaryngol Head Neck Surg. 1998;119(6):709-710. doi:10.1016/S0194-5998(98)70042-7
- ↑ 33.0 33.1 33.2 33.3 33.4 Cohen PR, Kurzrock R. Sweet’s syndrome: a review of current treatment options. Am J Clin Dermatol. 2002;3(2):117-131. doi:10.2165/00128071-200203020-00005