Dengue Virus
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Disease
Dengue virus is a positive sense RNA virus of the flavivirus family with at least four distinct serotypes. It is the cause of dengue fever which is associated with headache, retro-orbital pain, joint and bone pain (hence "breakbone fever"), fever and rash. The most serious form of dengue infection is known as dengue hemorrhagic fever which is characterized by thrombocytopenia and potentially multi-system organ failure. Dengue is a mosquito-borne viral illness that is spreading rapidly to become endemic in tropical and subtropical regions of the world. Infection with one serotype results in long-term immunity only to that specific serotype, and not to the others therefore a person can be infected many times with the virus. Dengue often is difficult to diagnose, and a presumptive diagnosis is established initially based on clinical signs and symptoms, while waiting for laboratory confirmation.
Etiology
The spread of Dengue fever occurs through a bite from an infected Aedes species (Ae. aegypti or Ae. albopictus) mosquito. These same mosquitoes also transmit Zika and chikungunya. Dengue can be transmitted during pregnancy to an unborn child or to a child in the perinatal period. There is one case of the virus spreading through the breast milk. Rarely it is transmitted through the blood.
Risk Factors
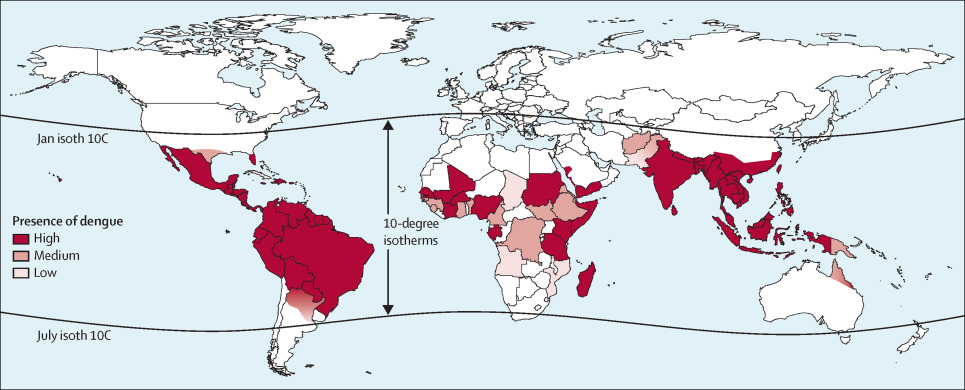
Dengue is present in over 100 countries with the most common being the Americas, Caribbean, Western Pacific Islands, Australia, Asia, Africa, and the Middle East. Each year 400 million people are infected with Dengue with 100 million symptomatic individuals and 22,000 deaths. Recent outbreaks in the United States were in Hawaii, Florida, and Texas. Travel to endemic areas and exposure to infected Aedes mosquitoes are risk factors for disease.
Pathophysiology
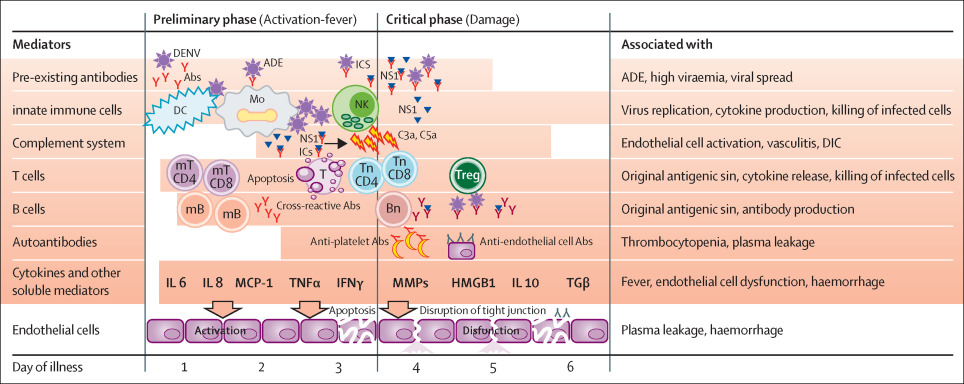
Dengue virus employs many mechanisms to utilize host cell machinery in order to facilitate viral replication. Dengue virus translation and replication occur in the endoplasmic reticulum of host cells, which experiences rearrangement and expansion during infection. Although the initial rearrangement is independent of the unfolded protein response (UPR), dengue virus alters the UPR in order to cope with endoplasmic reticulum stress throughout infection. Particular non-structural proteins (NS4A, NS2B/3) induce the UPR to slow host cell death during viral replication. In addition, dengue virus leads to autophagy and regulates lipid metabolism to enhance replication, and a functional autophagy pathway is essential to virus maturation and the production of infectious virions.
Primary Prevention
The best way to prevent a Dengue infection is to avoid mosquito bites. These mosquitos will infect individuals during the daytime and night so wearing insect repellant at all times in at risk countries is advised. Other precautions that can be taken are wearing long sleeved shirts and pants and mosquito nets at night.
Dengvaxia ® is the vaccine that is available in select countries for 9-45 year-olds, in patients that have had a prior infection. Recently, in May of 2019, the vaccine was approved in the United States for persons ages 9-16 living in a Dengue endemic area with a previous laboratory confirmed Dengue infection. If given the vaccine without prior infection, one might have a more severe systemic illness then if had not had prior exposure to the vaccine.
Diagnosis
History
Dengue fever manifests with symptomatic illness in approximately 25% of patients with mild to severe disease. Dengue is self limiting and can last from 2-7 days with the most common symptoms of arthralgias, myalgias, nausea, vomiting, rash, and fever, with 1 out of 20 patients developing the severe form which can lead to shock and bleeding. The average case fatality rate is 2.5%. Ocular symptoms include redness, photophobia, floaters, decreased vision, and scotoma.
Physical Examination
Dengue virus can manifest clinically in the eye as either ocular inflammation or as hemorrhagic complications. Uveitis from anterior to panuveitis can occur in this disease. Subconjunctival hemorrhage is a very common findings during acute illness. Anterior uveitis has been noted during both the acute illness and up to 5 months after disease remission and can occur in asymptomatic individuals. More severe vision threatening complications include serous retinal detachments and choroidal effusions. Dengue associated maculopathy is one of the most common posterior segment findings that include both retinal hemorrhages, cotton wool spots, and macular edema. In one retrospective review of 13 patients, 22 eyes were affected with a variety of manifestations including anterior uveitis, maculopathy, serous retinal detachments, and vasculitis. Notably patients’ symptoms occurred at the nadir of platelet count suggesting possible mechanism for ophthalmic complications. Ophthalmic complications related to Dengue associated eye disease include optic atrophy, retinal scarring, and retinal ischemia.
The Eye Institute Dengue-Related Ophthalmic Complications Workgroup described optical coherence tomography (OCT) findings and reported 3 patterns of disease: Type 1: diffuse retinal thickening, Type 2: cystoid macular edema, Type 3: foveolitis.[1] Agarwal et al. reported the multimodality imaging in Dengue associated foveolitis and maculopathy.[2] In their retrospective review of 16 patients (32 eyes), they reported foveolitis (disruption of outer retina) in 75% of eyes and observed flow voids in the superficial and deep capillary plexus on optical coherence tomography that persisted after treatment. They suggested that the pathogenesis of the ocular findings include both inflammation and ischemia.
Diagnostic Procedures
- Serologic testing with enzyme-linked immunosorbent assay (ELISA) or hemagglutinin inhibition
- Viral antigen (NS1) detection
- Viral isolation and identification using cell culture
- Detection of viral RNA by polymerase chain reaction (PCR)
Differential Diagnosis
- Chikungunya virus
- Zika virus infection
- Ebola virus
- Hemorrhagic fever viruses
- River Virus
- Orbivirus
- West Nile encephalitis
- Roseola infantum
- Scarlet fever
- Idiopathic thrombocytopenic purpura
- Influenza
- Leptospirosis
- Malaria
- Meningitis
- Rickettsial Infection
- Rocky Mountain Spotted Fever (RMSF)
- Typhus
- Viral Hepatitis
Management
General Treatment
For acute systemic infection with Dengue virus, supportive care with fluid replacement is the mainstay therapy. The US Food and Drug Administration (FDA) has not approved any drugs against dengue, but substantial efforts are underway to develop antiviral compounds that target viral or host factors. Advances in acute-phase diagnostic assays make early diagnosis and treatment a more realistic scenario. Prompt initiation of rehydration therapy with intravenous crystalloid and colloid infusions is the mainstay of treatment in patients with more severe dengue.
Management of the ophthalmic disease is dependent on ophthalmic manifestations and degree of inflammation. For patients with anterior uveitis topical corticosteroids and cycloplegic agents have been used with success in resolution of symptoms and disease. For posterior segment disease oral prednisone 0.5-1.0 mg/kg has been used to treat more severe disease.
Prognosis
Overall, final visual acuity and outcome is dependent on initial ocular manifestations. Patients with anterior uveitis tend to do better. In one report of 65 eyes in patients with various ocular manifestations from anterior uveitis, optic neuritis, to maculopathy (50 eyes), 83% had a final visual acuity of better than 6/12 at 1 year. In patients with vasculitis the outcomes may not be as good. In one review of retinal vasculitis patients 7/13 patients had a final visual acuity ranging from 6/12- 6/60. Other reports have also found patients with foveolitis at initial diagnosis do not recover vision as rapidly.
Additional Resources
References
- ↑ Teoh SC, Chee CK, Laude A, Goh KY, Barkham T, Ang BS; Eye Institute Dengue-related Ophthalmic Complications Workgroup. Optical coherence tomography patterns as predictors of visual outcome in dengue-related maculopathy. Retina. 2010 Mar;30(3):390-8. doi: 10.1097/IAE.0b013e3181bd2fc6. PubMed PMID: 20094013.
- ↑ Agarwal A, Aggarwal K, Dogra M, Kumar A, Akella M, Katoch D, Bansal R, Singh R, Gupta V; OCTA Study Group. Dengue-Induced Inflammatory, Ischemic Foveolitis and Outer Maculopathy: A Swept-Source Imaging Evaluation. Ophthalmol Retina. 2019 Feb;3(2):170-177. doi: 10.1016/j.oret.2018.09.008. Epub 2018 Sep 20. PubMed PMID: 31014768.
- ↑ Dengue. Centers for Disease Control and Prevention. https://www.cdc.gov/dengue/ Accessed June 4, 2024.
- Carrillo-Soto MA. Case series of ocular involvement due to dengue. First reported cases in Guatemala. Arch Soc Esp Oftalmol. 2018 Jul;93(7):329-335. doi: 10.1016/j.oftal.2018.02.005. Epub 2018 Mar 23. English, Spanish. PubMed PMID:29580756
- Koundanya VV, Chowdhary N, Agarwal M, Katre P. Secondary dengue retinitis with associated occlusive retinal vasculitis. J Ophthalmic Inflamm Infect. 2019 May 16;9(1):7. doi: 10.1186/s12348-019-0175-x. PubMed PMID: 31098778.
- Bawankar P, Lahane T, Parekh R, Lahane S, Lahane S, Pathak P, Sonawane S. An unusual occurrence of stromal keratitis in dengue fever. Indian J Ophthalmol. 2018 Nov;66(11):1631-1633. doi: 10.4103/ijo.IJO_387_18. PubMed PMID: 30355887; PubMed Central PMCID: PMC6213663.
- Oliver GF, Carr JM, Smith JR. Emerging infectious uveitis: Chikungunya, dengue, Zika and Ebola: A review. Clin Exp Ophthalmol. 2019 Apr;47(3):372-380. doi: 10.1111/ceo.13450. Epub 2019 Jan 2. Review. PubMed PMID: 30474222.