On Call Ophthalmology
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
This article summarizes a practical framework for approaching overnight ophthalmology consultations in the emergency department, inpatient wards, intensive care units, and postoperative settings. It reviews preparation for call, urgency-based triage, focused bedside examination, and communication strategies for common ophthalmic presentations encountered overnight. Key vision-threatening and life-threatening conditions, including ocular trauma, acute angle-closure glaucoma, endophthalmitis, retinal detachment, orbital cellulitis, and neuro-ophthalmic emergencies, are highlighted with emphasis on timely recognition and escalation. The goal is to support efficient and clinically sound on-call decision-making while recognizing that local resources, institutional workflows, and clinical judgment should guide management.
Introduction
Overnight ophthalmology call requires rapid triage of vision-threatening and occasionally life-threatening conditions encountered in the emergency department, inpatient wards, intensive care units, and postoperative settings. The on-call ophthalmology resident or attending physician is frequently consulted for acute vision loss, ocular pain, trauma, postoperative complications, and neurologic or systemic conditions with ocular manifestations. '
Common overnight consults include open globe injuries, orbital fractures, acute angle-closure glaucoma, retinal detachment, posterior vitreous detachment, central retinal artery occlusion, endophthalmitis, orbital cellulitis, and corneal ulcers and perforations. The role of the on-call resident or attending physician is to identify conditions requiring immediate intervention, distinguish urgent from non-urgent pathology, perform a focused bedside examination, and communicate findings clearly with the primary team and supervising physician, with prompt recognition of high-risk findings being critical to prevent permanent vision loss. This article provides a structured framework for ophthalmology trainees covering overnight consults, including preparation, triage, focused examination, and communication.
Preparing for Call
Overnight ophthalmology consultations frequently occur in the emergency department, inpatient wards, intensive care units, and operating room settings, often without access to a full ophthalmic clinic. Prior to starting call, the resident should confirm availability of essential examination equipment, commonly used medications, and a clear escalation pathway to the senior resident, fellow, or attending physician.
Because many overnight evaluations must be performed at the bedside with limited resources, familiarity with handheld examination tools, safe dilation practices, and indications for urgent intervention is critical. Preparation should emphasize efficiency, portability, and readiness to evaluate vision-threatening conditions.
Essential Equipment Checklist
The following items are commonly required for inpatient and emergency department ophthalmology evaluations. Availability may vary by institution; residents should verify the location of equipment before starting call.
| Item | Purpose | Notes |
|---|---|---|
| Penlight / transilluminator | Pupillary exam, anterior segment screening | Always carry |
| Near card / Rosenbaum card | Visual acuity testing | Always document visual acuity and method used |
| Pinhole occluder | Assess refractive component of decreased vision | Useful in bedside visual acuity exams |
| Slit lamp | Detailed anterior segment exam | Confirm availability and location of portable slit lamp before starting call |
| Direct ophthalmoscope | Basic fundus evaluation | Limited view but helpful when dilation is not possible |
| Indirect ophthalmoscope | Retinal evaluation, trauma, peripheral fundus exam | Preferred over direct for most on-call fundus evaluation |
| 20D / 28D condensing lens | Used with indirect ophthalmoscope | Carry both if possible |
| Gonioscopy lens | Angle evaluation in suspected angle-closure | Requires slit lamp; may not be feasible in emergent settings like the ED |
| Dilating drops | Fundus examination | Do not dilate in suspected head injury or iris trauma, use caution in narrow angles |
| B-scan | Posterior segment evaluation | Useful in trauma, vitreous hemorrhage, endophthalmitis |
| Fluorescein strips | Detect epithelial defects, Seidel test, corneal ulcers | Requires cobalt blue light |
| Cobalt blue light / wood lamp | Fluorescein examination | Often available in ED |
| Tonopen / handheld tonometer | Measure IOP | Avoid in open globe injury |
| Tonopen covers / wipes | Infection control | Carry extras |
| Topical anesthetic | Improve comfort during exams | Avoid repeated outpatient use |
| Cotton-tip applicators | Lid eversion, foreign body removal | Useful in many exams |
| Eyelid speculum | Trauma or foreign body evaluation | Optional but helpful |
| Eye shield | Protect suspected open globe | Do not apply pressure; do not patch |
| pH paper | Chemical injury evaluation | Check before and after irrigation |
| Morgan lens | Ocular irrigation for chemical injury | Often available in ED |
| 30 Gauge needle/ Corneal spud | Remove corneal foreign bodies | |
| Laceration repair kit | Repair eyelid lacerations | Needle driver, forceps, scissors, sutures, lidocaine w/ epinephrine, needle, syringe, |
Commonly Used Medications
| Medication | Typical Use | Contraindications |
|---|---|---|
| Proparacaine/tetracaine | Topical anesthesia | Avoid prescription for home use |
| Fluorescein | Corneal exam, Seidel test | Avoid in obvious open globe rupture |
| Tropicamide | Short-acting dilation | Use caution in narrow/occludable angles |
| Phenylephrine | Dilation | Avoid in severe hypertension, cardiac disease, infants |
| Cyclopentolate | Dilation; cycloplegia | Use caution in narrow / occludable angles |
| Atropine | Long cycloplegia | Use caution in narrow / occludable angles |
| Pilocarpine | Acute angle-closure glaucoma | Defer until IOP <40 mmHg; avoid if non-pupillary block mechanism suspected (plateau iris, lens-related); use caution in uveitic glaucoma |
| Timolol | Lower IOP | Avoid in asthma, COPD, heart block, bradycardia |
| Brimonidine | Lower IOP | Contraindicated in infants (<2 yrs) |
| Dorzolamide | Lower IOP | Sulfa-related reactions possible |
| Acetazolamide | Systemic IOP reduction | Avoid in sulfa allergy, renal failure, liver disease |
| Mannitol | Severe IOP elevation | Avoid in heart failure, pulmonary edema; requires medical clearance |
| Fluoroquinolone drops | Corneal ulcers, abrasion, infection | Avoid contact lenses |
| Erythromycin ointment | Surface protection | Avoid contact lenses |
| Prednisolone acetate | inflammation | Avoid in active infection |
| Dexamethasone | Inflammation, inpatient setting | Avoid in active infection |
| Povidone-iodine | Pre-intravitreal injection, severe corneal ulcer protocols | Use diluted formulation; avoid in iodine allergy |
| Vancomycin / ceftazidime drops | Severe bacterial keratitis, endophthalmitis | Compounded; availability varies by institution |
Note: Availability and institutional protocols may vary. Clinicians should be familiar with indications, contraindications, and appropriate escalation.
Situations Requiring Immediate Escalation
The on-call resident should notify the senior resident, fellow, or attending physician promptly in the following situations:
- Suspected open globe injury
- Orbital compartment syndrome
- Acute angle-closure glaucoma
- Central retinal artery occlusion or acute vision loss of unclear cause
- Suspected endophthalmitis
- Orbital cellulitis with vision changes or afferent pupillary defect
- Retinal detachment
- Severe ocular trauma or penetrating injury
- Postoperative patient with pain and decreased vision
- Inability to complete examination due to patient condition
- Any situation in which urgent surgical intervention may be required
Early communication is recommended whenever uncertainty exists.
General Tips for Overnight Consults
- Always document visual acuity when possible
- Prepare basic portable equipment (vision card, dilating drops, tonopen, etc.) in a readily accessible call kit
- Confirm the availability and location of essential equipment (slit lamp, B-scan, etc.)
- Consider globe rupture before performing tonometry or applying pressure
- Dilate when safe and not contraindicated
- Provide clear instructions to patients in writing and their native language, without abbreviations.
- Ensure a qualified interpreter is used when needed.
- Escalate to the senior resident, fellow, or attending physician promptly when the diagnosis or management is uncertain.
Simplified Algorithm in Determining Urgency of Evaluation
While the more specific, pertinent questions to ask patients during the history gathering process would vary depending on the differential diagnoses that clinicians may already have in mind, there are general questions that may help guide the timing for ophthalmology evaluation. (Figure 1).
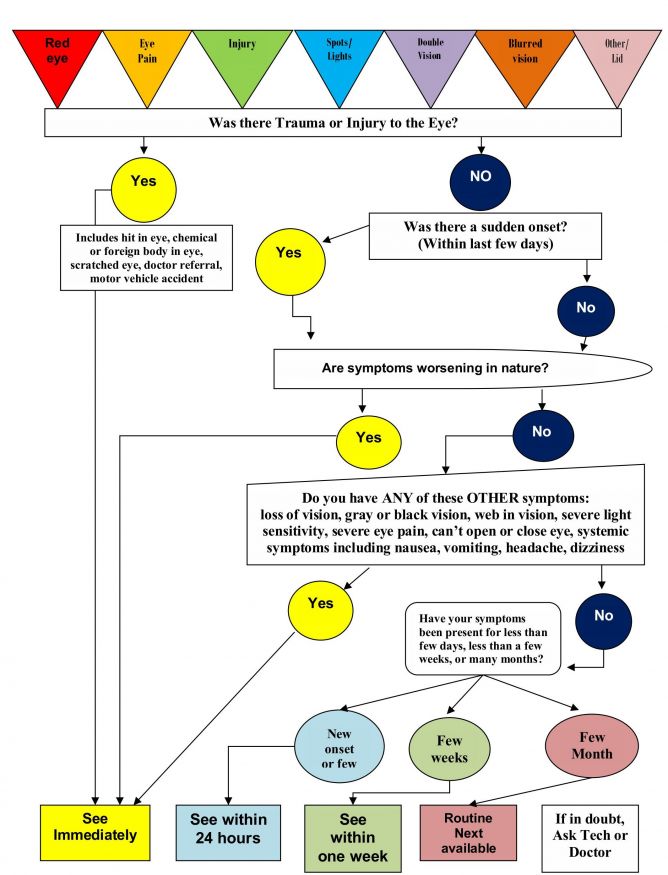
Urgency-Based Diagnosis Table
The tables below categorize common emergent ophthalmic presentations by urgency level to guide on-call triage decision-making.
In clinical practice, not all listed conditions require on-call evaluation or same-day management. Many may be appropriately managed in the outpatient setting or at the next available clinic visit. Non-urgent conditions generally do not require on-call assessment, and some semi-urgent conditions may also be deferred depending on clinical context. Furthermore, the acuity of a given condition may vary considerably between patients; for example, a patient with a small traumatic hyphema and normal intraocular pressure requires a different level of urgency than one with a total hyphema and elevated pressure, even though both fall under the same diagnosis.
This classification system is intended as a practical framework to help on-call ophthalmologists prioritize and triage patient calls and presentations, rather than as a strict protocol mandating a specific time or setting of care. Clinical judgment should always supersede any triage classification system.
Anterior Segment
| Condition | Priority |
|---|---|
| Chemical injury (alkali or acid) | Urgent |
| Acute angle-closure glaucoma | Urgent |
| Endophthalmitis (post-operative or endogenous) | Urgent |
| Intraocular foreign body | Urgent |
| Bacterial keratitis / corneal ulcer | Urgent |
| Herpes simplex keratitis | Urgent |
| Herpes zoster ophthalmicus | Urgent |
| Scleritis | Urgent |
| Anterior uveitis (acute) | Urgent |
| Corneal Ulcer | Urgent |
| Photokeratitis | Semi-urgent |
| Marginal keratitis | Semi-urgent |
| Pterygium | Non-urgent |
| Subconjunctival hemorrhage | Non-urgent |
| Viral conjunctivitis | Non-urgent |
| Allergic conjunctivitis | Non-urgent |
| Bacterial conjunctivitis | Non-urgent |
| Dry eyes | Non-urgent |
Posterior Segment
| Condition | Priority |
|---|---|
| Central retinal artery occlusion (CRAO) | Urgent |
| Endophthalmitis (vitreous involvement) | Urgent |
| Rhegmatogenous retinal detachment (macula-on) | Urgent |
| Rhegmatogenous retinal detachment (macula-off) | Urgent |
| Central retinal vein occlusion (CRVO) | Urgent |
| Branch retinal artery occlusion (BRAO) | Urgent |
| Vitreous hemorrhage | Urgent |
| Posterior vitreous detachment (symptomatic, no detachment) | Semi-urgent |
| Wet age-related macular degeneration (new/acute) | Semi-urgent |
Orbit and Adnexa
| Condition | Priority |
|---|---|
| Orbital cellulitis (postseptal) | Urgent |
| Cavernous sinus thrombosis | Urgent |
| Eyelid laceration involving canaliculus or lid margin | Urgent |
| Eyelid laceration (simple, not involving margin) | Urgent |
| Preseptal (periorbital) cellulitis | Semi-urgent |
| Orbital floor fracture | Semi-urgent |
| Orbital medial wall fracture | Semi-urgent |
| Dacryocystitis (acute) | Semi-urgent |
| Chalazion / hordeolum | Non-urgent |
| Blepharitis | Non-urgent |
| Ectropion | Non-urgent |
| Entropion | Non-urgent |
| Trichiasis | Non-urgent |
Neuro-Ophthalmology
| Condition | Priority | Notes |
|---|---|---|
| Cavernous sinus thrombosis | Urgent | Risk of intracranial extension; urgent neuroimaging + anticoagulation |
| Pituitary apoplexy | Urgent | Adrenal crisis risk; sudden vision loss + ophthalmoplegia + severe headache |
| CN III palsy (pupil-involving, new) | Urgent | Posterior communicating artery aneurysm until proven otherwise; urgent CTA/MRA |
| Amaurosis fugax | Urgent | TIA equivalent; urgent stroke workup |
| Arteritic ischemic optic neuropathy — GCA | Urgent | Immediate IV methylprednisolone; fellow eye at risk within hours |
| Acute papilledema with threatened vision | Urgent | Urgent LP ± neuroimaging to exclude mass |
| Orbital apex syndrome | Urgent | CN II/III/IV/V1/VI involvement; urgent neuroimaging |
| Non-arteritic AION | Urgent | Distinguish from arteritic; vascular risk factor modification |
| Optic neuritis (acute) | Urgent | Rule out NMO (anti-AQP4/MOG); MRI brain and orbits |
| Acute homonymous hemianopia | Urgent | Posterior cortical stroke or mass until proven otherwise |
| Internuclear ophthalmoplegia (INO), new onset | Urgent | Brainstem lesion; bilateral INO = MS until proven otherwise |
| Acute diplopia (new CN IV or VI palsy) | Urgent | MRI if atypical, painful, or young patient |
| Horner syndrome, new onset | Urgent | Exclude carotid dissection; urgent CTA and/or MRI/MRA head and neck |
| Ocular myasthenia / myasthenic crisis | Urgent | Risk of bulbar/respiratory involvement; CT chest for thymoma |
| Chronic papilledema / IIH without acute visual threat | Semi-urgent | Serial perimetry; acetazolamide; surgical options if progressive |
| Thyroid eye disease with compressive optic neuropathy | Semi-urgent | Orbital decompression if acuity or color vision deteriorating |
| Acquired nystagmus, new onset | Semi-urgent | Brainstem/cerebellar etiology until proven otherwise; MRI |
Trauma
| Condition | Priority |
|---|---|
| Ruptured globe / open globe injury | Urgent |
| Sharp / penetrating ocular trauma | Urgent |
| Traumatic hyphema with elevated IOP or total hyphema | Urgent |
| Closed globe injury (significant blunt trauma) | Urgent |
| Traumatic hyphema (small, IOP normal) | Semi-urgent |
| Corneal abrasion | Semi-urgent |
| Conjunctival laceration | Semi-urgent |
Focused Bedside Exam Pearls
Visual Acuity
- Use a Snellen chart to measure visual acuity.
- If unavailable, use a near card, newspaper, or magazine and record the smallest text the patient can read and the distance.
- Patients should wear their usual distance glasses (if any) during testing.
- Position the patient 20 feet from the chart and cover the eye that’s not being tested.
- If vision is 20/40 or worse, repeat the test using a pinhole occluder (can be used over glasses).
In many cases of serious injury, the patient may be unable to read even the largest letter on an eye chart. If this is the case:
- Record the distance at which the patient can count fingers with the affected eye.
- If the patient cannot count fingers, determine the distance at which hand movement can be detected.
- If the patient is unable to detect hand movement, use a penlight to determine whether he or she can perceive light.[1]
Occasionally, clinicians will encounter a patient who is unwilling or unable to cooperate with standard visual acuity testing or who may be suspected of faking blindness. Because the typical visual acuity test will not work for such a patient, clinicians will need to be alert to other signs. Withdrawal or a change in facial expression in response to light or sudden movement indicates the presence of vision.
Lid Examination
- Foreign bodies may be lodged on the palpebral conjunctiva of the upper lid. Clinicians may evaluate this by having the patient look down while the clinician raises the upper lid.
- To evert the upper lid:
- Ask patient to look down
- Place the stick portion of a cotton swab approximately 10 mm above the upper lash margin.
- Grasp the eyelashes with the other hand and gently pull straight out from the globe.
- Pull the lashes up toward the forehead and flip the eyelid over, using the applicator stick as a fulcrum. Hold the eyelashes against the orbital rim with your thumb and withdraw the applicator. To return the lid to its normal position, the examiner releases the lid margin, and the patient is instructed to look up.[1]
Fluorescein Staining
- Fluorescein is applied in the form of a sterile filter-paper strip, which is moistened with a drop of sterile water or saline and then touched to the palpebral conjunctiva.
- Clinicians should ask patients to blink their eyes a few times to spread the fluorescein over the cornea.
- Areas of bright-green staining under cobalt blue light denote absent or diseased epithelium.
- Precautions to keep in mind when using fluorescein are:
- Have the patient remove soft contact lenses prior to application to avoid discoloration of the lenses.
- If the formulation includes an ester anesthetic, as is often the case, hypersensitivity to such agents is also a contraindication. Other contraindications include sensitivity to para-aminobenzoic acid.[2]
Pupillary Testing
- In any case of trauma or decreased vision, check the eye for a relative afferent pupillary defect.
- Pupils should be inspected while the patient is looking at an object at a distance to avoid the pupillary constriction that occurs with a near target.
- A bright light source should be held directly in front of one eye before moving rapidly across the bridge of the nose to the front of the other eye and then shifted back to the first eye.
- Poor pupillary dilation in dim light may indicate dysfunction of the sympathetic nervous system, and poor pupillary constriction to bright light may indicate parasympathetic dysfunction.[1]
Direct Ophthalmoscopy
To perform direct ophthalmoscopy, follow these steps:
- Have the patient comfortably seated. Instruct the patient to look at a point on the wall straight ahead, trying not to move the eyes.
- Set the focusing wheel at about +8. Set the aperture wheel to select the large, round, white light.
- Begin to look at the right eye about 1 foot from the patient. Use your right eye with the ophthalmoscope in your right hand. When you look straight down the patient's line of sight at the pupil, you should see the red reflex.
- Place your free hand on the patient's forehead or shoulder to aid your proprioception and to keep yourself steady.
- Slowly come close to the patient at an angle of about 15 degrees temporal to the patient's line of sight. Try to keep the pupil in view. Turn the focusing wheel to bring the patient's retina into focus.
- When a retinal vessel comes into view, follow it as it widens to the optic disc, which lies nasal to the center of the retina.[3]
Intraocular Pressure Measurement with Tono-Pen
- Confirm that tonometry is safe. Do not measure IOP if an open globe injury is suspected.
- After allowing the Tono-Pen to calibrate, apply a sterile probe cover over the tip.
- Instill topical anesthetic to the patient’s eyes and ask the patient to blink to distribute the medication.
- Ask patient to look straight ahead at a distant target. The examiner should keep the patient’s eyelids open without pressing on the globe. Stabilize your hand by resting your fingers on the patient’s forehead for stability.
- Position the Tono-Pen perpendicular to the cornea and make multiple, rapid, and light taps to the central cornea.
- Always measure both eyes for comparison.
- If measurements vary widely, repeat the test.
- Ask patients to avoid squeezing eyelids, which falsely elevates IOP.
Confrontation Field Testing
The examiner takes a position in front of the patient. The patient is asked to cover the left eye with the palm of the left hand; the examiner closes the right eye. Thus, the field of the examiner's left eye is used as a reference to assess the field of the patient's right eye. The patient is asked to fixate on the examiner's left eye and then count the fingers of the examiner in each of the four quadrants of the visual field. The examiner should repeat the process for the other eye.[1]
Ocular Trauma
Open Globe Injury
Definition: Full-thickness wound of the eyewall (cornea/sclera). Includes penetrating, perforating injuries and intraocular foreign bodies.
Key Symptoms & Signs
| Category | Findings |
|---|---|
| Symptoms | Pain, decreased vision |
| IOP | Normal or decreased |
| Pupil | Peaked pupil (pathognomonic), RAPD |
| Other | Hyphema, uveal prolapse, shallow anterior chamber |
Management
| Category | Action |
|---|---|
| Protection | Eye shield |
| Medications | Broad spectrum IV antibiotics (vancomycin, ceftriaxone, cefotaxime, ceftazidime, ciprofloxacin), antiemetics, pain control |
| Other | Tetanus prophylaxis, NPO, surgical removal of foreign object, surgical repair within 24 hours |
Exam Considerations
- Use CT (NOT MRI if metallic FB suspected)
- Perform Seidel test for aqueous leak
- Calculate the Ocular Trauma Score (OTS) to determine prognosis. Category 1 is associated with poor prognosis and lack of light perception, while Category 5 is associated with good prognosis and has the highest probability of visual acuity >20/200.[6]
Orbital Compartment Syndrome
Definition: Compression and ischemia of the retina and optic nerve occur when intraorbital pressure exceeds ophthalmic artery pressure.[7]
Key Symptoms & Signs
| Category | Findings |
|---|---|
| Symptoms | Orbital pain, swelling, vision loss, diplopia, nausea, vomiting |
| External signs | Proptosis, periorbital edema, eyelid ecchymosis, resistance to retropulsion |
| Motility | Restricted extraocular movement, visual field defects |
| Conjunctiva | Chemosis, hemorrhage, injection |
| Pupil | Relative afferent pupillary defect (RAPD), internal ophthalmoplegia |
| IOP | Elevated; globe feels firm |
Management
| Category | Action |
|---|---|
| Emergency | Immediate lateral canthotomy/cantholysis or orbital decompression |
| Surgical | Orbitotomy ± needle decompression (if abscess or emphysema present) |
| Medications | Antiemetics, decongestants, stool softeners, pain control, antihypertensives |
| Other | Anticoagulation if thrombosis is suspected |
Exam Considerations
- Identify cause of increased orbital volume (e.g., hemorrhage, emphysema, swelling).
- Imaging (CT with contrast or venography) obtained after decompression.[7][8]
- Vision-threatening emergency requiring treatment ideally within 90 minutes.[7]
Chemical Injury
Definition: Ocular chemical injury can be due to acidic or alkaline substances.[4][9][10]
Key Symptoms & Signs
| Category | Findings |
|---|---|
| External signs | Particulate matter, eyelid malposition |
| Cornea | Epithelial defects, ground-glass appearance (acid), liquefactive necrosis (alkali) |
| Conjunctiva | Limbal ischemia, scarring, symblepharon |
| IOP | Elevated due to trabecular meshwork damage |
| Other | Corneal opacity, forniceal shortening, entropion/ectropion |
Management
| Category | Action |
|---|---|
| Immediate | Copious irrigation ≥15 minutes until pH 7.0–7.2 |
| Technique | Irrigate nasal → lateral; evert eyelids |
| Medications | Based on severity (antibiotics, steroids, cycloplegics, vitamin C) |
| Other | Avoid eye patching |
Exam Considerations
- Perform exam only after pH stabilization
- Use fluorescein to assess epithelial damage
- Grade severity using Hughes classification.[9][10]
- Do not delay irrigation for history or exam..[9][10]
Orbital Fractures
Definition: Fractured or broken bones surrounding the orbit, which include orbital rim fractures, blowout fractures, and orbital floor fractures.[11]
Key Symptoms & Signs
| Category | Findings |
|---|---|
| Symptoms | Diplopia, blurry vision or vision loss, pain, swelling, numbness |
| External signs | Bruising, eyelid swelling, enophthalmos, trismus |
| Motility | Restricted movement (especially upward gaze) |
| Neuro | Possible intracranial injury |
| Eye | Hyphema, corneal abrasion, RAPD |
| Other | Oculocardiac reflex (bradycardia, syncope) |
Management
| Category | Action |
|---|---|
| IOP >40 mmHg | Immediate canthotomy/cantholysis |
| Mild | Ice packs, observation |
| Severe | Surgical repair (implant fixation, decompression) |
| Other | Avoid nose blowing |
Exam Considerations
- Perform full neurological assessment.
- Obtain CT scan or orbital X-rays.
Eyelid Lacerations
Definition: Blunt or lacerating trauma to the eyelids. These injuries can be simple or complex.[14]
Key Symptoms and Signs
| Category | Findings |
|---|---|
| Symptoms | Pain, tearing, bleeding, swelling, numbness |
| External | Eyelid margin involvement, fat prolapse, tissue loss |
| Vision | Assess visual acuity prior to intervention |
| Pupils | Evaluate pupillary response and red reflex |
Management
| Category | Action |
|---|---|
| Initial | Keep wound moist with topical erythromycin and avoid premature tissue removal (including necrotic tissue) |
| Surgical | Urgent repair by an oculoplastic surgeon. Consult with ENT surgeons for sinus involvement and neurosurgeons for intracranial involvement. |
| Other | Ensure sutures do not contact the cornea |
Exam Considerations
- Assess for canalicular/lacrimal system involvement.
- Obtain CT imaging if indicated.
- Evaluate for associated intracranial injury.[15]
- Urgency escalates with canalicular involvement, associated orbital injury, or intracranial extension.[14][15]
High-Yield Non-Traumatic Emergencies
Acute Angle-Closure Glaucoma
Definition: Increased intraocular pressure due to mechanical occlusion of the trabecular meshwork that impairs aqueous outflow.[16]
Key Symptoms and Signs
| Category | Findings |
|---|---|
| Symptoms | Acute vision loss, blurred vision, headache, nausea/vomiting |
| Vision | Markedly reduced visual acuity |
| IOP | Elevated (typically 40–80 mmHg); globe feels firm |
| Pupil | Mid-dilated, fixed, non-reactive pupil |
| Cornea | Hazy/edematous |
| Other | Conjunctival injection, shallow anterior chamber |
Management
| Category | Action |
|---|---|
| Initial | Topical timolol, topical apraclonidine, IV/PO acetazolamide |
| Additional | Pilocarpine (once IOP <40 mmHg) |
| Refractory | IV mannitol |
| Supportive | Antiemetics to reduce Valsalva |
| Definitive | Laser peripheral iridotomy (LPI) |
Exam Considerations
- A gonioscopy confirms diagnosis (≥180° closure).
- Evaluate the unaffected eye as there is a higher risk for occurrence from baseline in the opposite eye.
- Avoid misdiagnosis as neurologic or abdominal pathology, which is how it may initially present.[12][16]
- Irreversible optic nerve damage can occur within hours and requires immediate IOP-lowering therapy and urgent ophthalmology consultation.[16][17]
Central Retinal Artery Occlusion
Definition: An acute occlusion of the central retinal artery (also known as an ocular stroke), usually from thromboembolism, resulting in retinal ischemia and sudden vision loss.[18]
Key Symptoms and Signs
| Category | Findings |
|---|---|
| Symptoms | Sudden, painless, severe monocular vision loss |
| Vision | Counting fingers, hand motion, or light perception |
| Pupil | RAPD |
| Fundus | Retinal whitening, cherry-red spot, attenuated arterioles |
| Visual Field | Near-complete loss (may spare small area) |
Management
| Category | Action |
|---|---|
| Immediate | Activate stroke protocol |
| <4.5 hrs | Consider IV tPA (in consult with the stroke team) |
| >4.5 hrs | Antiplatelet therapy, stroke workup |
| Arteritic | Immediate IV corticosteroids (suspected giant cell arteritis (GCA), which can lead to vision loss) |
| Other | Avoid delaying care with ineffective therapies |
Exam Considerations
- Labs: ESR/CRP (to rule out GCA)
- Obtain a full stroke workup (ECG, carotid imaging, echo).
- Retinal damage begins within 90-100 minutes. Treat as stroke equivalent ("eye stroke").[19]
Giant Cell Arteritis (GCA)
Definition: A granulomatous vasculitis of medium and large vessels, most commonly affecting the branches of the external carotid artery. It is the most common cause of arteritic ischemic optic neuropathy (AION) and represents one of the most vision-threatening emergencies in ophthalmology, with the fellow eye at significant risk within hours to days if untreated.
Key Symptoms and Signs
| Category | Findings |
|---|---|
| Symptoms | Sudden vision loss, scalp tenderness, jaw claudication, temporal headache, fatigue, fever, weight loss |
| Vision | Sudden, severe, often painless monocular vision loss |
| Pupil | RAPD |
| Fundus | Pale, swollen optic disc (chalky white edema characteristic of arteritic AION) |
| Other | Tender, nodular, or pulseless temporal artery on palpation |
Management
| Category | Action |
|---|---|
| Immediate | High-dose IV methylprednisolone 1g daily for 3 days |
| Subsequent | Transition to oral prednisone 1mg/kg/day |
| Labs | ESR, CRP, CBC, platelet count (thrombocytosis supportive of diagnosis) |
| Definitive | Temporal artery biopsy within 2 weeks of starting steroids |
| Other | Do not delay steroids pending biopsy; aspirin 81mg if no contraindication |
Exam Considerations
- Biopsy should not delay initiation of corticosteroids
- Contralateral eye is at risk; fellow eye involvement can occur within hours to days without treatment
- ESR and CRP are sensitive but not specific; a normal ESR does not exclude GCA
- Consider rheumatology consultation for long-term management
- Do not delay corticosteroid therapy pending confirmatory testing. The fellow eye is at imminent risk and vision loss is typically irreversible once it occurs.
Endophthalmitis
Definition: A purulent intraocular infection involving the vitreous and aqueous humor, most commonly following surgery, trauma, or hematogenous spread. The types are defined by endogenous and exogenous routes of infection entry.[20]
Key Symptoms and Signs
| Category | Findings |
|---|---|
| Symptoms | Eye pain, redness, decreased vision |
| Vision | Rapidly worsening (can be hand motion or light motion) |
| External signs | Lid swelling |
| Anterior | Hypopyon, anterior chamber inflammation |
| Posterior | Vitritis, vitreous haze |
| Other | Absent or diminished red reflex |
Management
| Category | Action |
|---|---|
| Initial | Intravitreal antibiotics (vancomycin + ceftazidime) |
| Mild (+ hand motion) | Tap and inject |
| Severe (light perception or worse) | Pars plana vitrectomy |
| Endogenous | Add systemic antibiotics ± antifungals |
| Fungal | Add intravitreal antifungal |
Exam Considerations
- Obtain vitreous/aqueous cultures to control for infection.
- Monitor for high suspicion post-surgery or trauma.
- Vision outcomes depend on time to treatment and requires immediate ophthalmology involvement.
Orbital Cellulitis
Definition: Infection posterior to the orbital septum involving orbital tissues, most commonly from sinus spread. This diagnosis must be distinguished from preseptal cellulitis.[22]
Key Symptoms and Signs
| Category | Findings |
|---|---|
| Vision | Decreased |
| Pain | Pain with eye movement |
| Motility | Restricted (ophthalmoplegia) |
| External | Proptosis, eyelid edema |
| Pupil | RAPD (optic nerve involvement) |
| Other | Fever, leukocytosis, chemosis |
Management
| Category | Action |
|---|---|
| Preseptal | Oral antibiotics with MRSA coverage if indicated (trimethoprim-sulfamethoxazole or clindamycin) |
| Orbital | Admit patient for intervention; IV vancomycin + broad-spectrum coverage |
| Surgical | Drain abscess or if no improvement in 24-48 hrs |
| Emergency | Canthotomy if orbital compartment syndrome develops |
Exam Considerations
- Obtain an ENT consult if there is a sinus source.
- Monitor for intracranial complications and consult with neurosurgery if symptoms worsen.
- Urgency escalates in the setting of optic neuropathy, orbital compartment syndrome, or abscess formation.
Retinal Detachment
Definition: Separation of the neurosensory retina from the underlying retinal pigment epithelium (RPE). The most common type is rhegmatogenous retinal detachment (RRD), which occurs due to a full-thickness retinal break allowing liquefied vitreous to accumulate in the subretinal space. Other types include tractional and exudative retinal detachments.
Key Symptoms and Signs
| Category | Findings |
|---|---|
| Symptoms | Sudden onset floaters, flashes of light (photopsia), peripheral visual field loss ("curtain" or "shadow"), painless |
| Vision | Variable; reduced acuity if macula involved |
| Pupil | RAPD if extensive detachment |
| Fundus | Elevated, billowing retina; retinal break or tear; tobacco dust (Shafer sign) in vitreous |
| Other | Reduced IOP compared to fellow eye |
Management
| Category | Action |
|---|---|
| Macula-on | Urgent surgical repair; same-day or next morning to preserve central vision |
| Macula-off (recent, <1 week) | Urgent surgical repair; timing less critical but prompt intervention improves outcomes |
| Macula-off (chronic, >1 week) | Semi-urgent; schedule elective repair |
| Surgical options | Pneumatic retinopexy, scleral buckle, pars plana vitrectomy (PPV) |
| NPO | If surgery anticipated |
Exam Considerations
- Dilated fundus exam with indirect ophthalmoscopy is essential
- Scleral depression to identify peripheral breaks
- B-scan ultrasound if media opacity prevents fundus visualization
- Examine the fellow eye for lattice degeneration or peripheral breaks
- Macula-on detachments should be treated as emergencies to prevent macular involvement and preserve central vision. Macula-off detachments require prompt but not necessarily immediate intervention, with urgency guided by duration of macular involvement.
Documentation and Communication
General Useful Information to Gather for Ophthalmology Consultation
Other services consulting ophthalmology may use the general guide below when presenting information to ophthalmology residents or attendings for consultation:
- Date and time that the patient presented
- Requesting service and reason for consultation
- Patient’s chief complaint
- History of presenting illness
- Onset
- Duration and progression
- Triggers (trauma/chemical exposure)
- Laterality (OS/OD/OU)
- Pain (severity, with eye movement?)
- Associative symptoms (erythema, floaters, diplopia, discharge, etc.)
- Prior episodes if any, types of treatment received, and outcomes
- Past ocular history
- Diagnoses
- Surgeries
- History of trauma
- Use of glasses or contact lenses
- Other relevant past medical history
- Hypertension
- Diabetes
- Thyroid eye disease
- Rheumatoid arthritis
- Systemic lupus erythematosus
- Other systemic or autoimmune conditions
- Medications and allergies
Sample Ophthalmology Consult Note Template
Below is an example of an ophthalmology consult note template commonly used in common EMR platforms (e.g. Epic).
CC/HPI
[Patient Name] is a [age]-year-old [male/female] with a history of [PMH], presenting with [chief complaint]. Ophthalmology was consulted for further evaluation.
The patient reports [symptoms].
The patient denies ocular pain, redness, foreign body sensation, itching, burning, tearing, discharge, flashes, floaters, diplopia, or photophobia.
No prior ocular history. No history of ocular surgery. Not using ocular medications. No known family history of ocular disease.
PMH:
PSH:
FamHx:
SocHx:
Current Meds & Allergies
Relevant medications patients is taking for both systemic conditions and/or ophthalmic condition. Document any known allergies.
Ophthalmic Exam
Vital Signs
| OD | OS | |
| Visual Acuity
(near) |
20/ [ ] | 20/ [ ] |
| Pupils | RR, no RAPD | RR, no RAPD |
| IOP (Tonopen) | [ ] mmHg | [ ] mmHg |
| Visual Fields (confrontation) | Full | Full |
| Color Vision (Ishihara) | 11/11 | 11/11 |
| EOM | Full, Ortho | Full, Ortho |
| OD | OS | |
| External | WNL | WNL |
| Lids/Lashes | WNL | WNL |
| Conj/Sclera | White and quiet | White and quiet |
| Cornea | Clear | Clear |
| Anterior Chamber | Deep and Quiet | Deep and Quiet |
| Iris | WNL | WNL |
| Lens | Clear | Clear |
Dilated Fundus Exam: Patient dilated with 2.5% phenylephrine and 1% tropicamide
| OD | OS | |
| Vitreous | Clear | Clear |
| Disc | Sharp and pink | Sharp and pink |
| C/D ratio | 0. [ ] | 0. [ ] |
| Macula | Flat, + FLR | Flat, + FLR |
| Vessels | WNL | WNL |
| Periphery | WNL, no tears, holes or detachments | WNL, no tears, holes or detachments |
Imaging
| OD | OS | |
| B-scan ultrasound | Retina flat, no vitritis | Retina flat, no vitritis |
Lab Data
Other Imaging
Assessment/Plan
[Patient Name] is a [age]-year-old [male/female] with [summary diagnosis].
# [Problem]
- [Assessment sentence — what you think it is]
- [Key supporting findings]
- [Plan: meds / imaging / follow-up]
Regardless of the consult template used, below are detailed points to include and consider in every new patient consult performed:
- Subjective
- Chief Complaint: [briefly describe the main reason for the visit]
- History of Present Illness: [details about the onset, duration, severity, and character of the visual complaint]
- Past Ocular History: [history of previous eye diseases, surgeries, treatments, and outcomes]
- Medical History: [relevant systemic conditions affecting ocular health]
- Medication History: [current ocular and systemic medications]
- Allergies: [medication and substance allergies]
- Family Ocular History: [family history of eye diseases]
- Social History: [tobacco use, alcohol use, occupational hazards]
- Objective
- Extraocular Movements: [full/restricted, presence/absence of pain with movement]
- Visual Acuity: [findings for visual acuity without correction and with correction, for each eye (OD, OS)]
- Pupils: [size, symmetry/asymmetry, presence/absence of RAPD]
- External Exam: [findings from lids and lashes such as proptosis and ptosis]
- Intraocular Pressure: [measurement method and values for each eye (OD, OS)]
- Anterior Segment: [findings from slit-lamp examination]
- Posterior Segment: [findings from dilated fundus examination]
- Additional Tests: [results of additional tests such as OCT and fluorescein angiography]
- Assessment
- Diagnosis [ICD-10 code]
- Plan
- Treatments: [planned treatments such as medications, laser therapy, or surgical interventions]
- Workup: [further labs and imaging]
- Follow-Up: [specified interval until next visit]
- Patient Education: [information provided about diagnosis, treatment, and prognosis]
- Referrals: [referrals to other specialists if any]
References
- ↑ 1.0 1.1 1.2 1.3 Pg D, Sftfswfe MS. &ZF 5SBVNB BOE &NFSHFODJFT.
- ↑ Pothen AG, Parmar M. Fluorescein. In: StatPearls. StatPearls Publishing; 2026. Accessed March 28, 2026. http://www.ncbi.nlm.nih.gov/books/NBK555957/
- ↑ Fundoscopic Exam (Ophthalmoscopy). Stanford Medicine 25. Accessed March 29, 2026. https://med.stanford.edu/stanfordmedicine25/the25/fundoscopic.html
- ↑ 4.0 4.1 Heath Jeffery RC, Dobes J, Chen FK. Eye injuries: Understanding ocular trauma. Aust J Gen Pract. 2022;51(7):476-482. doi:10.31128/AJGP-03-21-5921
- ↑ Open Globe Injury: Assessment and Preoperative Management. American Academy of Ophthalmology. August 1, 2020. Accessed March 17, 2026. https://www.aao.org/eyenet/article/open-globe-injury
- ↑ Tan SI, Hoskin AK, Khatri A, et al. Prognostic factors of open-globe injuries: A review. Indian J Ophthalmol. 2023;71(12):3587-3594. doi:10.4103/IJO.IJO_1496_23
- ↑ 7.0 7.1 7.2 Orbital Compartment Syndrome. American Academy of Ophthalmology. March 1, 2023. Accessed March 17, 2026. https://www.aao.org/eyenet/article/orbital-compartment-syndrome-2
- ↑ Zhao Z, Malik A, Bhat N, et al. Orbital Compartment Syndrome After High-speed Air-Gasoline Blast Injury. Ophthal Plast Reconstr Surg. 2021;37(3):e97-e100. doi:10.1097/IOP.0000000000001845
- ↑ 9.0 9.1 9.2 Chemical (Alkali and Acid) Injury of the Conjunctiva and Cornea - EyeWiki. Accessed March 17, 2026. https://eyewiki.org/Chemical_(Alkali_and_Acid)_Injury_of_the_Conjunctiva_and_Cornea
- ↑ 10.0 10.1 10.2 Treating Acute Chemical Injuries of the Cornea. American Academy of Ophthalmology. October 1, 2012. Accessed March 17, 2026. https://www.aao.org/eyenet/article/treating-acute-chemical-injuries-of-cornea
- ↑ What Is an Orbital Fracture? American Academy of Ophthalmology. September 28, 2017. Accessed March 18, 2026. https://www.aao.org/eye-health/diseases/what-is-orbital-fracture
- ↑ 12.0 12.1 Boyette J, Pemberton J, Bonilla-Velez J. Management of orbital fractures: challenges and solutions. Clin Ophthalmol. Published online November 2015:2127. doi:10.2147/OPTH.S80463
- ↑ Orbital Fracture Diagnosis and Treatment. American Academy of Ophthalmology. September 28, 2017. Accessed March 18, 2026. https://www.aao.org/eye-health/diseases/orbital-fracture-diagnosis-treatment
- ↑ 14.0 14.1 Awidi A, Zhao J, Li X, et al. Etiology and Characteristics of Patients Presenting with Eyelid Lacerations at a Level 1 Trauma Center. Clin Ophthalmol. 2024;Volume 18:929-935. doi:10.2147/OPTH.S447452
- ↑ 15.0 15.1 Stec LA. Trauma of Periocular Structures: Eyelid Laceration, Orbital Fracture & Retrobulbar Hematoma.
- ↑ 16.0 16.1 16.2 Primary vs. Secondary Angle Closure Glaucoma - EyeWiki. Accessed March 29, 2026. https://eyewiki.org/Primary_vs._Secondary_Angle_Closure_Glaucoma
- ↑ Murray D. Emergency management: angle-closure glaucoma. Community Eye Health. 2018;31(103):64.
- ↑ 18.0 18.1 CRAO: Promising Results From Emergency Protocols. American Academy of Ophthalmology. July 1, 2024. Accessed March 29, 2026. https://www.aao.org/eyenet/article/crao-emergency-protocols-may-preserve-vision
- ↑ 19.0 19.1 Madike R, Cugati S, Chen C. A review of the management of central retinal artery occlusion. Taiwan J Ophthalmol. 2022;12(3):273-281. doi:10.4103/2211-5056.353126
- ↑ 20.0 20.1 Endogenous Endophthalmitis: Diagnosis and Treatment. American Academy of Ophthalmology. June 1, 2016. Accessed March 29, 2026. https://www.aao.org/eyenet/article/endogenous-endophthalmitis-diagnosis-treatment
- ↑ Shao EH, Yates WB, Ho IV, Chang AA, Simunovic MP. Endophthalmitis: Changes in Presentation, Management and the Role of Early Vitrectomy. Ophthalmol Ther. 2021;10(4):877-890. doi:10.1007/s40123-021-00406-6
- ↑ 22.0 22.1 Moran CORE | Preseptal vs Orbital Cellulitis. Accessed March 29, 2026. https://morancore.utah.edu/basic-ophthalmology-review/preseptal-vs-orbital-cellulitis/
- ↑ Danishyar A, Sergent SR. Orbital Cellulitis. In: StatPearls. StatPearls Publishing; 2026. Accessed March 29, 2026. http://www.ncbi.nlm.nih.gov/books/NBK507901/

